Your new post is loading...
 Your new post is loading...
Researchers from Karolinska Institutet have published a study in Alzheimer's Research & Therapy that addresses possible associations between chronic stress, mild cognitive impairment and Alzheimer's disease. The study shows how people aged between 18 and 65 with a previous diagnosis of chronic stress and depression were more likely than other people to be diagnosed with mild cognitive impairment or Alzheimer's disease.
Via LGA
So top healthcare digital transformation trends in 2023 are as follows: Internet of Medical Things (IoMT) Cybersecurity and Data Privacy Remote Patient Monitoring (RPM) Improved Big Data & Analytics Cloud Migration Robotic Process Automation (RPA) Cognitive Automation (CA) FinTech Integration Interoperability and Connectivity Telehealth Data Breach Prevention Network Strategies Tailored Patient Experience 1. Internet of Medical Things (IoMT) According to Precedence Research, the global internet of things (IoT) in healthcare market size was valued at $180.5 billion in 2021 and it is expected to reach around $960.2 billion by 2030 with a compound annual growth rate (CAGR) of 20.41% during the forecast period 2022 to 2030. Wearables and trackers are a huge part of healthcare information technology development. Their key benefit is providing real-time and detailed data on the patients’ health states, which is precious for doctors’ observation. 2. Cybersecurity and Data Privacy Data security is still a key industrial concern, and cybersecurity will appear relevant among trends in the health information technology industry for a long time. All future technological enhancements will stick to the requirement to possess a significant security layer. The ultimate goal is to protect sensitive patient data delivered online. At the end of 2021, the number of weekly attacks on healthcare reached an average of 626 per organization and is constantly growing. The US Federal Bureau of Investigation stated that over 40 million patients’ healthcare records were compromised in 2021, as half of the internet-connected hospital devices are vulnerable to cyberattacks. 3. Remote Patient Monitoring (RPM) Of the latest trends in the healthcare industry, RPM occupies a special place. COVID-19 also contributed to turning remote patient monitoring into the current tendency in the medical field. The rise of virtual healthcare takes many forms, including online appointments, remote care, and video conferencing. And the wide range of IoMT devices empowers RPM with even more opportunities. According to Research and Markets, the global RPM systems market is projected to be worth over $175.2 billion by 2027, compared to $53.6 billion in 2022. 4. Improved Big Data & Analytics According to Frost & Sullivan’s forecast, introducing AI technology in healthcare data analytics can save the industry at least $150 million by 2025. Such an achievement is possible thanks to real-time and long-distance analysis and measurement of patient data. Given such striking cost-effectiveness, the AI trend will hit its stride in the next few years. For medical providers and researchers, the COVID-19 pandemic spotlighted data analytics, along with the immense challenge of real-time decision-making under rapidly changing conditions. Healthcare providers can get lost in dozens of spreadsheets and meetings if processed manually. That’s why the digital future inevitably includes technology capable of processing Big Data instead of humans and providing real-time analytics for decision-makers. 5. Cloud Migration Cloud migration in healthcare is now in full swing and will see significant growth in the future. MarketsandMarkets states that the global healthcare cloud computing market is projected to reach $89.4 billion by 2027, from an estimated $39.4 billion in 2022 at a CAGR of 17.8% during the forecast period. It solves many major challenges in service delivery, including record management, remote care, and reaching low-income patients. Providers worldwide use the cloud to efficiently manage emails and electronic medical records (EMRs) and make real-time data available to healthcare professionals. 6. Robotic Process Automation (RPA) The World Healthcare Organization (WHO) predicted that the global healthcare worker shortage could reach 12.9 million professionals by 2035, making in-person medical appointments a luxury few patients can afford. And the COVID-19 pandemic has only aggravated things. Wide-scale adoption of robotic process automation (RPA) solutions in healthcare may cure medical system inefficiencies. RPA-empowered bots are a significant milestone in healthcare information technology development. Health providers can experience accurate automation, cost reduction, staff optimization, and even introduce transformational changes with the know-how. On the patient side, AI algorithms can guide people to the needed doctor by scanning their symptoms more accurately than traditional search engines. 7. Cognitive Automation (CA) Among the emerging healthcare technology trends, it is worth highlighting CA. Cognitive Automation is the next-level tendency for true digital transformation. These days, it’s among emerging IT market trends in healthcare, but the tech package and applicability are about to change the state of managing an industry to the core. It takes the achievements of RPA but applies the mimicking of human behavior beyond the repetitive tasks. In short, it serves as the digital brain of the healthcare organization. In essence, CA takes the automation capabilities of current software providers and applies ML algorithms to introduce decision velocity in the industry. It becomes possible to process zettabytes of data within seconds and provide decision-makers with ready-to-accept recommendations backed up by real-time data. The ultimate goal is to establish a self-driving enterprise where all the operational processes are automated. 8. FinTech Integration Healthcare spending is likely to reach $6 trillion by 2027. Until recently, the healthcare system tended to be an old-school bureaucratic system. But now, many hospitals and medical institutions have turned to the tech industry to improve their filing and billing processes, and tech has begun delivering. The financial technology covers insurance, management services, digital payments, settlement services, capital-raising, deposits, and credit services. Thus it facilitates and streamlines healthcare processes by lowering the cost of financial services. Through robotic investment advice, P2P lending, mobile payments, artificial intelligence, machine learning, and blockchain technologies, fintech boosts the healthcare sector by mitigating inefficiencies in its payment plans. 9. Interoperability and Connectivity It is another healthcare tech trend that popped up during the global pandemic due to the lack of data interoperability. It has slowed caregivers down for years and impacted their ability to provide the best possible care. The interoperability and connectivity of medical devices are widely recognized as important factors in helping hospitals achieve better patient data flow, synchronization, quicker and more accurate identification of high-risk patients, and improving the overall outcome. 10. Telehealth Throughout the COVID-19 pandemic, telemedicine has seen the wildest growth and has become one of the hottest trends in the healthcare industry. 82% of customers experienced telemedicine for the first time since the start of COVID-19. According to Precedence Research, the telemedicine market is poised to grow from about $60.8 billion in 2022 to $225 billion in 2030. It has become an integral part of the whole healthcare industry. 11. Data Breach Prevention Over the years, the data breach issue has become more critical. According to the HIPAA Journal, today, the number of healthcare data breaches exceeds two times daily, which was a concern only once a day in 2017. 12. Network Strategies The healthcare digital transformation market is growing at over 14% annually. In conditions where doctors actively use telemedicine and patients track their progress through wearables and mHealth apps, a network strategy is necessary. Therefore, the implementation of network solutions for effective communication and data exchange between doctors, patients, and healthcare organizations is another trend in the medical field. 13. Tailored Patient Experience Another prominent trend in healthcare is the provision of a tailored patient experience. It’s especially noticeable considering the global precision medicine market growth, which will reach $146.6 billion by 2028, in contrast to $65.9 billion in 2021. In the coming years, implementing any new technology in the medical field will be carried out by putting the patient at the center of this process. Studying the specifics of each patient’s condition will help draw up more effective treatment plans and get better treatment outcomes.
Via Dr. Russ Conrath

|
Rescooped by
Dennis Swender
from HMHS History
April 26, 2022 12:02 PM
|
In this fiery and funny talk, New York Times food writer Mark Bittman weighs in on what's wrong with the way we eat now (too much meat, too few plants; too much fast food, too little home cooking), and why it's putting the entire planet at risk.
Via Michael Miller

|
Scooped by
Dennis Swender
June 24, 2021 3:11 PM
|
The information blocking provisions of the 21st Century Cures Act officially went into effect this week, putting into focus the Department of Health and Human Services’ regulatory and compliance effort around HIPAA-required data sharing between applicable healthcare entities. Enacted by the 21st Century Cures Act in 2017 and implemented by a final rule in 2020, Congress defined information blocking and established penalties for providers that engage in practices that interfere with the access, exchange, and use of electronic health information. The long-awaited info blocking provision established rules and penalties for non-compliance. The law carves out exclusions for providers if they meet an exception established by the HHS Secretary, or for other applicable reasons. Starting April 5, relevant covered entities and business associates must comply. The Office for the National Coordinator recently released insights on just what the law’s enactment means for those relevant providers, as well as the areas HHS will focus on in the next 18 months. For now, a smaller subset of electronic health data is in scope. “Specifically, the electronic health information that cannot be blocked is limited to the data elements represented in the US Core Data for Interoperability,” ONC officials explained. “This initial 18-month period and limited scope gives the regulated community time to grow more experienced with the information blocking regulation, including when and how to meet an exception, before the full scope of the regulation’s EHI definition comes into effect.” “Of course, those who are able to share more EHI than is represented by the USCDI need not wait to begin doing so,” they added. “Similarly, as a way to prepare for October 2022, we strongly encourage the regulated community to make all EHI available as if the scope of EHI were not currently limited.” As the US surpasses its one-year milestone of the COVID-19 national emergency and subsequent Department of Health and Human Services’ HIPAA liability waivers, it’s the ideal time for providers to assess the health of their privacy governance and compliance programs. INFORMATION BLOCKING PROVISIONS To Sean Sullivan, a senior associate attorney with the Health Care Group of Alston & Bird, the industry should consider this period as breathing room: the enforcement arm of the rule hasn’t been fully enacted and the HHS liability waivers put into place for COVID-19 remain intact -- for now. The info blocking provisions signal a sea of change for the industry, he explained. Providers had the last year to prepare for these drastic changes, and now ONC has stressed it will be focusing on this compliance area moving forward. While the rules won’t immediately change things, it does provide new rights to accessing data between providers and other covered entities through authorized requests. Sullivan stressed that it overlays HIPAA’s information sharing requirements that merely suggested providers may share data with other covered entities. The new provisions make data sharing a requirement, or those efforts could be considered info blocking and a direct violation of the provisions. The timeline for data sharing has also changed from the previous 30-day requirement to “on a timely basis and without necessary delay.” There’s no strict deadline, rather an expectation that the data be immediately available, he explained. The idea is to allow other healthcare providers to use their EHR or the platform of the connected covered entity to download the needed information. “The expectation is that now data should be instantaneously available as long as it’s electronic,” Sullivan said. “And a lot of providers who miss those new timeframes are going to continue to fall back on that 30-day timeline. It’s a mistake.” Instead, providers need to review their policies and procedures for all electronic data within their possession and determine whether the tech in place is capable of adhering to the provisions. They will also need to assess how to provide electronic data on a timely basis, via the EHR or even a patient portal. “Frankly, the government has been struggling with [data sharing and info blocking] for some time,” Sullivan said. “But the financial services industry figured it out years ago.” Sullivan also mused that providers, insurers, and specialists are operating within similar environments, but still the data sharing process has remained stagnant -- with the healthcare industry, as a whole, reluctant to change. Previous arguments have stressed the sensitive nature of the data, while others have pointed to a lack of resources to invest in needed tech. There’s also an anti-competitive factor, where some providers worry that its patients may shop around at a competitor’s care site.

|
Rescooped by
Dennis Swender
from Revalued
May 28, 2021 11:53 AM
|
Both the first and second numbers in a person's blood pressure reading are important for predicting the risk of cardiovascular disease.
Via Peter Mellow, Susan Myburgh

|
Scooped by
Dennis Swender
April 24, 2021 11:09 AM
|
As of now, your HIPAA checklist for 2021 looks much the same as years prior. Although there are no confirmed changes to HIPAA, there are several proposed changes that may come into effect soon. What is the 2021 HIPAA Checklist? The 2021 HIPAA checklist consists of several questions in which an organization working in healthcare can use to assess their overall HIPAA compliance. Have you completed all of your annual self-audits? Have you identified gaps in your compliance based on findings from your self-audits? Have you created remediation plans to address these gaps? Have all employees received their annual HIPAA training? Do you have policies and procedures in accordance with HIPAA requirements? Do you have signed business associate agreements with all of your business associates? Do you have a process for identifying, tracking, and reporting breaches? How to Use the Checklist to Help with Your Compliance By utilizing the HIPAA compliance checklist 2021, you can assess your current HIPAA practices against HIPAA standards. The purpose of the 2021 HIPAA checklist is to give you a basic understanding of whether or not you are meeting HIPAA requirements. However, the checklist is not meant to confirm or verify your compliance program. To do so, you should speak with a HIPAA expert, such as Compliancy Group. We will walk you through the checklist to help you understand where your compliance program is lacking, and help you implement an effective HIPAA compliance program in accordance with the law. When working with us, you will never have to go at it alone, we will be there every step of the way to make sure that you have HIPAA compliance covered! Proposed HIPAA Changes Although there are no current changes to the HIPAA compliance checklist 2021, it is highly likely that it will change in the near future. This is because there are several proposed changes to the HIPAA Privacy Rule that may come into effect soon. These changes may include: Reducing identity verification burdens Improving information sharing Expansion of permitted PHI disclosures Reducing administrative burdens Updating Notice of Privacy Practices requirements For more information on proposed Privacy Rule changes, please click here. Cybersecurity as a Priority In addition to potential changes to the Privacy Rule, there has also been a push to update HIPAA cybersecurity requirements. As of January 2021, a bill known as HR 7898, requires the Department of Health and Human Services (HHS) to incentivize healthcare organizations to implement cybersecurity practices. In essence, if an organization is subject to a HIPAA audit, and they can prove that they had implemented a recognized cybersecurity framework, instead of being fined, they would be given technical assistance from the HHS.
Even the body works harder when running outdoors compared to on a treadmill, running outside feels easier and you’re more likely to feel more motivated to keep going.
Via Peter Mellow
Many Americans know they’ve put on weight during the pandemic, but it’s been difficult for experts to detail the scope of the problem.
Via Peter Mellow

|
Rescooped by
Dennis Swender
from Hospitals and Healthcare
March 4, 2021 7:49 PM
|
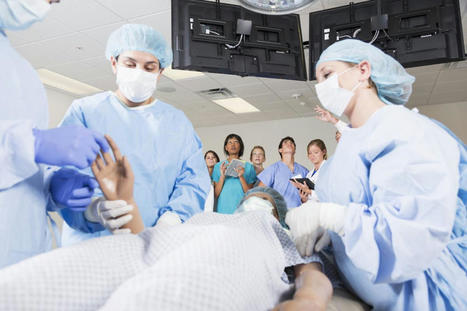
Some doctors contend that medical schools should take a closer look at race, not just in terms of whom they admit, but what they teach.
Via Peter Mellow

|
Rescooped by
Dennis Swender
from Customer service in tourism
February 27, 2021 3:04 AM
|
"Hotels, and even some cruise ships, are installing state-of-the-art filtration systems that claim to tackle the coronavirus where it is believed to be the most dangerous: in the air ..."
Via Leona Ungerer

|
Rescooped by
Dennis Swender
from Hospitals and Healthcare
February 24, 2021 2:19 AM
|
Advancing nursing leadership, investing in nursing education, and providing support and resources for nurses around the world are key to addressing disease outbreaks and improving global public hea…
Via Peter Mellow

|
Rescooped by
Dennis Swender
from Hospitals and Healthcare
February 20, 2021 1:06 PM
|
“Ineke Crezee’s book fills a vital gap in health interpreting, placing the extensive medical vocabulary needed within the context of interpreter’s practice and the issues they face in the very varied areas of health care. It is ideal for all training levels from short courses to postgraduate work.”
Uldis Ozolins, University of Western Sydney
Via Peter Mellow

|
Rescooped by
Dennis Swender
from Health & Fitness Teens
February 19, 2021 3:26 PM
|
Resolving to lose weight in 2021? Here are three reasons why you might want to reconsider your approach.
Via Larisa Ens
|
Martinus Evans wants to make running more inclusive. His new book beckons back-of-the-packers to lace up.
Via Peter Mellow
Hayden Kendrick is an amateur bodybuilder who’s focused on getting big and getting cut.
Via Peter Mellow

|
Rescooped by
Dennis Swender
from Creative teaching and learning
February 2, 2022 6:55 PM
|
"The pandemic has intensified many stress points for faculty and academic librarians while highlighting existing issues with how academic work is structured ..."
Via Leona Ungerer
We all believe we should exercise more. So why is it so hard to keep it up? Daniel E Lieberman, Harvard professor of evolutionary biology, explodes the most common and unhelpful workout myths
Via Peter Mellow

|
Rescooped by
Dennis Swender
from Social Media and Healthcare
April 30, 2021 2:30 PM
|
It’s time for healthcare organizations to make bigger investments in mobile patient engagement. The past year’s pandemic struck a painful blow to health organizations’ pre-COVID patient engagement efforts. There are now fewer patient visits amidst coronavirus fears and stay-at-home orders. People are simply not going into clinics to address non-COVID medical needs. The result is more serious health issues developing, such as cancers being found at later stages and chronic conditions advancing beyond easy treatment options. As patient engagement strategies ramp up, mobile communication channels are becoming more attractive for reaching those living in geographically isolated areas, far from their medical providers. While video visits have replaced many non-urgent in-person visits, those in rural areas struggle to use even telemedicine options due to lack of access or unreliable broadband connectivity. The travel is too far and the technology is not part of their daily lives making healthcare completely out of reach. Because most people own a cell phone, mobile is an ideal way to communicate and elicit collaboration for health. Healthcare systems that leverage mobile channels are finding this platform a powerful way to serve patients. Text (SMS) is an ideal channel for reaching underserved communities, as one does not need a smartphone or broadband to send or receive SMS messages. SMS also provides a quick and easy way for patients to send information back to their doctors about side effects related to the vaccines. Moving beyond one-way communication with SMS gives patients a way to ask questions or relay information on their current health status. To take things beyond basic SMS, healthcare providers can consider fleshing out a full mobile communications strategy to deliver tailored analytics. With real-time data and services, staff work-flow can be improved and resources can be allocated more efficiently, also lowering costs. It’s the next step up from SMS but patients with chronic conditions who have mobile access to medical portals showed improved self-management and an increase in regular contact with their care team. read the entire piece at https://hitconsultant.net/2021/04/29/mobile-channels-improve-patient-engagement-outcomes/#.YIt7UOvhUf0
Via nrip

|
Scooped by
Dennis Swender
April 22, 2021 2:17 PM
|
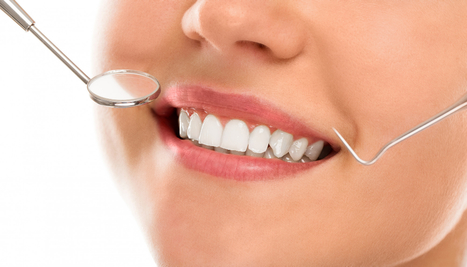
Similar to other healthcare or medical facilities, the majority of dental offices are run digitally these days. While technology makes the entire process for patients and staff easier, advanced tech also creates a more complex legal situation. Dental providers run a heightened risk of potentially violating HIPAA rules. HIPAA stands for the Health Insurance Portability and Accountability Act. HIPAA is legislation that ensures both the privacy and security of a patient’s personal and protected health information. Complying with HIPAA means safeguarding patient’s information and reducing the overall chance of a data breach in your system. As security is a top priority within a facility, here is a HIPAA compliance checklist for dental providers to follow. Know and Observe the HIPAA Security Rule There are three parts to the HIPAA security rule, which includes three different aspects of security requirements. These requirements are technical requirements, physical requirements, and administrative requirements. Technical requirements for security include the technicality of communication—how information is transmitted and communicated electronically. There should be a controlled system with standard transmittance processes set in place in order to protect patients’ information. The physical requirements under the security rule rely on the computer systems in place at a dental facility. These computer systems and their surrounding environment should be inaccessible to those who are not responsible for information imputation, meaning there should be procedures set in place to validate a person’s physical access to private information. Administrative requirements under the security rule ties into this procedure. Administrators are appointed to select a communications system that is compliant with HIPAA and are responsible as well to develop policies and protocols for compliance. Be Secure Against Cybersecurity Threats As mentioned above, healthcare and dental facilities have gone digital with recordkeeping and patient files. At the top of this HIPAA compliance checklist for dental providers lies an important task—knowing how to act under the HIPAA security rule. To best way to protect patient’s private information is to have a system of secure messaging as well as data encryption. Encryption of patient data is a requirement to appropriately protect sensitive information like SSNs, birthdates, addresses, or phone numbers. It’s also best to use passwords on computers in the office, and have secured and not open or public Wi-Fi network. Ensure Proper Staff Education and Training Having clear compliance protocols set in place is the very best way to protect patient information. Examples of such protocols would be not public broadcasting private information in the office and safely and quietly inputting private information in the computer. Employee error is a major cause of data breaches, so train staff under HIPAA’s privacy, security, and breach notification rules.

|
Rescooped by
Dennis Swender
from Hospitals and Healthcare
April 11, 2021 12:42 PM
|
The horrors of Covid-19 may give proponents of the liberal arts an unexpected opening.
Via Peter Mellow
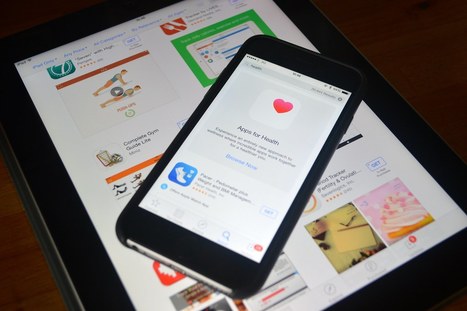
Digital health technologies involve the use of information and communication technologies (ICT) to address health problems faced by patients. Health apps are making it easier than ever to collect, manage and monitor health information These apps can help patients contact their doctors in case of an
Via Poorna Stefan
That walk to the bus stop, taking the stairs instead of the lift, using a manual lawnmower to cut the grass — how much benefit can we get from incidental exercise?
Via Peter Mellow

|
Scooped by
Dennis Swender
February 24, 2021 2:21 AM
|
A recent study concluded that many popular mobile health apps pose a risk to protected health information (PHI) security. The study analyzed the security of 30 health apps that allow healthcare providers to review patient charts and schedules and found that all of them are vulnerable to API cyberattacks. More details on the risks of mobile health apps are discussed. Risks of Mobile Health Apps: What Did the Study Find? The study into the risks of mobile health apps security was conducted by Approov, a mobile app API security company, and Knight Ink, a cybersecurity marketing firm. To determine whether or not health apps were putting PHI at risk, the companies reverse-engineered 30 mobile health apps to analyze their static code, and then conducted API penetration testing. Ok, now that you’re confused, what does that even mean? Basically, both of these things are done to determine if there are any cybersecurity vulnerabilities within the health apps’ codes or security protections. So, what did the study find? All apps were vulnerable to unauthorized access to ePHI. 77% had hard-coded API keys (an API is a unique identifier used to authenticate developers or users). Hard-coding API keys is widely regarded as a security flaw, and therefore is ill advised. 50% allowed unauthorized access to clinical results and admissions records. 7% had hard-coded user names and passwords. This practice is explicitly advised against as it allows threat actors to easily access login credentials, giving them full access to the health apps’ data. Alissa Knight, the report’s author and partner at Knight Ink stated, “There will always be vulnerabilities in code so long as humans are writing it. Humans are fallible. But I didn’t expect to find every app I tested to have hard-coded keys and tokens and all of the APIs to be vulnerable to [BOLA] vulnerabilities allowing me to access patient reports, X-rays, pathology reports, and full PHI records in their database. The problem is clearly systemic.” Risks of Mobile Health Apps: What Does This Mean? Cybersecurity in the healthcare space has long been a concern, particularly as of late with the rise in use of software applications in healthcare. The risks of mobile health apps security found in the analyzed apps point to a larger trend of vulnerable, frequently relied on, technology. For instance, the 30 analyzed apps, on average, have been downloaded 772,619 times. All of these apps allowed unauthorized access and alteration of PHI including patients’ demographics, photos, and clinical histories.

|
Scooped by
Dennis Swender
February 21, 2021 3:44 PM
|
With more and more remote workers in the healthcare space, PHI security should be a top concern. A recent survey determined that 44% of employees are currently working from home, with several employers expecting workers to continue to work remotely permanently. So what does this mean for cybersecurity and HIPAA compliance? To provide healthcare organizations with guidance, remote workers and HIPAA is discussed. Remote Workers and HIPAA: Data Privacy As a requirement of HIPAA, organizations working with protected health information (PHI) must ensure the confidentiality, integrity, and availability of the data. When you suddenly have a remote workforce, this becomes more difficult to accomplish, and you therefore must adjust your business practices. Paper records. Paper records are still used frequently in the healthcare field. When working from home, healthcare workers may be printing medical records from their home office, as such they must be cognizant of who in their household has the potential to view them. Records that contain any patient information must be kept in a secure location such as locked filing cabinets or a locked office. Otherwise, if an unauthorized individual views these paper documents, even when viewed accidentally by a family member, this is considered a HIPAA violation. Access controls. There are several instances in which remote workers would require access to their organization’s network. In these cases, it is essential that the organization has policies and procedures in place for secure remote access, this may include the requirement of an employee to connect to a virtual private network (VPN) before connecting to the organization’s network, or requiring the implementation of multifactor authentication. PHI disposal. Perhaps the most challenging aspect of remote workers and HIPAA, is how to dispose of records in a secure manner. Paper records that are no longer needed must be shredded, burned, pulped, or pulverized beyond recognition, or stored in a secure location until they can properly be disposed of. The difficult aspect of proper PHI disposal is when the records are electronic. For electronic PHI disposal, organizations likely must contract a third-party for disposal, which means remote workers must have clear guidelines on how they may comply with ePHI disposal requirements when they aren’t working in the office. Security risk assessment. Security risk assessments (SRAs) must be conducted annually, however it is recommended to conduct an SRA whenever there are changes to your business practice, much like the change to a remote workforce. Having remote workers poses a significant cybersecurity risk to any organization, and as such it is important to identify risks and vulnerabilities presented by a remote workforce. By conducting an SRA, gaps in current security practices are identified so that organizations can create remediation plans to address gaps. Vendor management. Just like it is important to conduct SRAs when there are changes to your organization’s business practices, it is important to consider your vendors’ risks. Many of your vendors have likely converted to a largely remote workforce, therefore it is essential to reassess the risk that they pose to your organization’s security by sending vendor risk assessments to any vendor that has the potential to access PHI. HIPAA policies and procedures. Healthcare organizations must have HIPAA policies and procedures that relate directly to the way their business operates. So it isn’t surprising that organizations with remote workers must have policies and procedures that provide guidelines on how to comply with HIPAA with a remote workforce. To ensure that your organization is complying with HIPAA while your workforce is remote, you must either adapt your existing policies to account for the changes a remote workforce poses to your business, or create new policies and procedures for working remotely. Office reopenings. When workers begin to return to the office, they will likely be on a hybrid work schedule, working both from the office and at home. This can pose risks when employees are bringing paperwork or electronic portable devices back and forth. When reopening, organizations must consider this risk and develop policies and procedures to minimize PHI exposure.

|
Scooped by
Dennis Swender
February 20, 2021 12:59 PM
|
Here are 8 things to know about the second dose of the vaccine. Side effects may be stronger than after the first dose, and immunity isn’t immediate.
|



 Your new post is loading...
Your new post is loading...