 Your new post is loading...
 Your new post is loading...
Traumatic brain injury (TBI) is one of the most common causes of disability and death in people. About 1.6 million individuals suffer traumatic brain injuries in the United States every year. TBI can cause a process of injury which may ultimately cause a variety of neurodegenerative diseases and other health issues. Many of the neurodegenerative diseases following TBI include health issues such as Alzheimer’s disease (AD), Parkinson’s disease (PD), and amyotrophic lateral sclerosis (ALS). The mechanisms underlying the pathogenesis which result in these type of neurodegenerative diseases, however, are still completely misunderstood. Where many of the health issues following TBI have a high incidence, there are currently only several treatment approaches which can help prevent the pathological development of chronic neurological diseases. A better understanding of the mechanisms underlying TBI and neurodegenerative diseases is ultimately fundamental to determine the possible connection between these health issues to allow safe and effective diagnosis and treatment. In part 1 of the following article, we will discuss the pathological mechanisms of traumatic brain injury (TBI) and how it’s associated with the development of a variety of neurological diseases and other health issues, including Alzheimer’s disease (AD).
Microglial cells make up about 10 to 15 percent of all the glial cells in the human body, which can be found in the central nervous system (CNS) and play a fundamental role in the human brain. Microglial cells are responsible for maintaining and regulating changes in the physiological and pathological condition of the CNS by changing their morphology, phenotype and function. In an average physiological state, the microglial cells are continuously in charge of controlling their environment. However, when the homeostasis of the brain is interrupted, the microglia change into an amoeba-like shape and become a phagocyte where they can actively reveal a variety of antigens. If the homeostasis interruption in the CNS continues, the microglial cells will then trigger at a much stronger state, which is known as microglial priming. Microglia are the “Bruce Banner” of the CNS. However, once they go into protective “Hulk” mode, primed microglia become much more sensitive to stimulation and they have a much stronger possibility of reacting to stimulation, even reacting towards normal cells. Microglial priming can become a double-edged sword. As a matter of fact, primed microglia are created from different phenotypes of microglia and the phenotypes are context-dependent, which means they are associated to the sequence and duration of their exposure to different varieties of stimulation in a variety of pathologies. In the article below, we will demonstrate the effect of microglial priming on the central nervous system (CNS), especially in neurological diseases.
About 6 million people in the United States have Alzheimer’s disease (AD) and about 50 million people worldwide have dementia. There aren’t many treatments to treat these neurological diseases. Scientists in a 2018 research study on red light therapy and mice described that “treatment for Alzheimer’s disease and dementia has not been effective for more than 100 years.” Another research study described that there is currently “no treatment to prevent brain health issues. However, research studies on red light therapy as a treatment for Alzheimer’s disease and dementia have been positive over the last few years in laboratory settings with rodent models. Based on this lab data, researchers recommend red light therapy and near-infrared light therapy in human patients with AD and dementia. In this article, we will look at what the initial human research studies on red light therapy and Alzheimer’s disease/dementia have shown over the last few years.
According to research studies, transcranial infrared laser stimulation, as well as other types of transcranial lasers, utilized on frontal cortex functions can improve sustained attention and working memory, among other brain functions. Transcranial laser stimulation with low-power density (mW/cm2) and high-energy density (J/cm2) monochromatic light in the near-infrared wavelengths regulates and maintains brain functions and may promote neurotherapeutic effects in a non-destructive and non-thermal manner. Researchers determined through the first controlled research study that transcranial laser stimulation improves human cognitive and emotional brain functions. In the field of low-level light/laser therapy or LLLT, developing a model to demonstrate how luminous energy from red-to-near-infrared wavelengths improves bioenergetics has been in development for the last 40 years. Previous LLLT research studies have demonstrated historical a variety of developments, principles and applications on the subject matter. The purpose of the following article is to demonstrate an update on LLLT’s neurochemical mechanisms supporting transcranial laser stimulation for cognitive-enhancing functions. We will describe the effect of LLLT on brain bioenergetics, briefly discussing its bioavailability and dose-response, and its effects on cognitive brain function. Although our focus is on prefrontal-related cognitive functions, LLLT should be able to improve other brain functions. By way of instance, stimulating different brain regions affect different functions associated with sensory and motor systems.
The central nervous system plays a fundamental role in the pathogenesis of infection. The CNS is regulated by the blood-brain barrier or BBB, however, it can be exposed to a microbial invasion from a contiguous focus, hematogenous dissemination, or intraneural passage of organisms. Various environmental or commensal bacteria, viruses, fungi, protozoa, or parasites can enter the CNS and cause infections and health issues. Central nervous system infections can cause headache, stiff neck, vomiting, fever, photophobia, and focal neurological symptoms.
Mitochondria are the “energy factory” of the human body. Several thousand mitochondria can be found in nearly every cell. Mitochondria also play several fundamental roles in the body, such as converting chemicals from the foods we eat into energy as well as to process oxygen. Mitochondria produce 90 percent of the energy the human body requires to function accordingly. The purpose of the following article is to describe an overview of mitochondrial disease and well-being. What are Mitochondrial Diseases? Mitochondrial diseases are characterized as chronic, genetic, and often inherited health issues which ultimately occur when mitochondria fail to produce enough energy for the human body to function properly. Mitochondrial diseases may develop from birth however they can frequently develop at any age. Mitochondrial disease can affect any region of the human body, including the cells of the brain, muscles, heart, liver, kidneys, pancreas, eyes, ears, and nerves, among other structures. When the mitochondria don’t function as well as they should because of another health issue, mitochondrial dysfunction occurs. Furthermore, many health issues can cause secondary dysfunction and result in other neurological diseases, such as Alzheimer’s disease, Lou Gehrig’s disease, and muscular dystrophy. People with secondary dysfunction don’t have genetic mitochondrial disease and do not need to be concerned about the ongoing development or worsening of symptoms.
Cerebral perfusion pressure, or CPP, is the net pressure gradient which carries oxygen to brain tissue. It is measured by the difference between the mean arterial pressure, or MAP, and the Intracranial Pressure, or ICP, which is measured in millimeters of mercury (mm Hg). Regulating CPP is fundamental in the treatment of patients with intracranial pathology, including shock, hemodynamic distress, and traumatic brain injury. Although the average CPP is generally between 60 and 80 mm Hg, these values may change to the left or to the right depending on individual physiology. MAP and ICP has to be measured together because CPP is a calculated measure. Regulating CPP at hemodynamically unstable conditions with abnormal ICP or in cases of intracranial pathology will reduce the chance of ischemic brain injury.
You have probably heard about the “gray matter” of the brain which is made up of cells known as neurons, however, a lesser-known type of brain cell is ultimately what makes up the “white matter” of the brain. These are well-known as glial cells as well as glia. Glial cells, also known as glia or neuroglia, were only considered to simply offer structural support. The term “glia” literally translates to “neural adhesive.” However, relatively recent research studies have demonstrated that they play a variety of roles in the brain and the nerves which run throughout the entire human body. However, there is more information still left to determine and find out.
The human brain is the human body’s control center. It is a fundamental structure in the nervous system, which also includes the spinal cord and a system of nerves and neurons. The nervous system controls every structure and function in the human body. When the brain is damaged, it can ultimately affect the function of the nervous system, including memory, sensation, and even personality. Brain disorders include any health issues which affect the brain. This includes health issues due to: - genetics
- illness
- trauma or injury
What are the Different Types of Brain Disorders? There is a wide array of different brain disorders which can vary tremendously in symptoms and grade of severity. In the following article, we will demonstrate the different types of brain disorders and discuss several of the most common types of brain disorders.
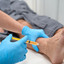
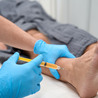
Leg Length Discrepancy (LLD) has profound effects on the body's biomechanics, which can result in back pain and a number of other debilitating conditions. Overview Also known as Leg length inequality leg length discrepancy affects as many as 60 to 90% of the population. It is categorized as functional or structural, but both have profound effects on the body's biomechanics and result in back pain. Other conditions include: - Arthritis of the knee
- Psoasitis
- Arthritis of the hip
- Patellar tendinitis
- Patellofemoral pain syndrome
- Plantar fasciitis
- Medial tibial stress syndrome
- Iliotibial band syndrome
- Lateral knee pain
- Trochanteric bursitis
- Sacroiliac discomfort
- Achilles tendinitis
- Cuboid syndrome
Functional Short Leg: Alignment difference of the supporting structures between the ground and the top of the femur or thigh bone. This is caused by excessive pronation or the natural rolling in of the foot as someone walks. Anatomical Short Leg: A difference in the size or length of the thigh bone (femur). This is most often caused by growth asymmetry that can be inherited/genetic condition but can sometimes come from a fracture or surgery. - Our body can work with leg inequality for short a period but over time, biomechanical problems throughout the body can begin to happen.
- Our body's ability to adapt to abnormal stress eventually takes its toll and the surrounding soft tissues can't take it anymore.
- Even the simplest movements begin to require much more muscular effort and energy, which reduces endurance.
Excessive stress gets transmitted to the ligaments, which then creates: - Misalignment
- Muscle fatigue
- Ligamentous stress
Treatment A Chiropractor will use a combination of techniques to help your condition, but treatment is dependent on the cause and symptoms. The first goal of treatment is to improve alignment and restore symmetry. This can be accomplished with: - Spinal adjustments focus on providing better spinal column alignment
- Exercises to help the affected muscles
- Proper orthotics with a pronation wedge under the heel for long-term correction
Sometimes LLI causes a profound gait (walk) disfunction, which means physical therapy might be necessary. Prevention - Keep your bones and tissues strong and healthy with exercise and diet can help.
- Avoid tobacco and excessive alcohol use, which weaken bones and can cause problems with the blood supply in the legs.
- Reduce your risk of injury by adhering to safety measures (like wearing a seatbelt).
- Custom orthotics provide support, stability, and shock absorption.
Recovery The body’s foundation can be made level with custom orthotics, but it does take some time to adjust to proper and healthier alignment/posture. Talk to your doctor or chiropractor to learn more. Symptoms: - Back pain
- Leg pain
- Pelvic obliquity
- Scoliotic deviations of the lumbar spine
- Increased risk of injury, especially in athletes
Chiropractic care does wonders for helping individuals regain their spinal alignment and loosen the joints and muscles affected by leg length inequality, and the orthotic heel lifts balance out the legs, which balances the hips and pelvis. Foot pronation is the natural movement which occurs during foot landing while walking or running. Foot pronation also occurs while standing, and in this instance, it is the amount in which the foot rolls inward toward the arch. Foot pronation is normal, however, excessive foot pronation can cause a variety of health issues, including bad posture. The following video describes the 5 red flags of excessive foot pronation, which can ultimately affect a person's overall health and wellness. Dr. Alex Jimenez can help diagnose and treat excessive foot pronation. Patients recommend Dr. Jimenez and his staff as the non-surgical choice for excessive foot pronation health issues.
Glutamate is the main excitatory neurotransmitter in the central nervous system, or CNS, of mammals and it primarily interacts with both metabotropic and ionotropic receptors to activate and regulate postsynaptic responses. Both AMPA and NMDA receptors are fundamental mediators of synaptic plasticity, the ability of synapses to strengthen or weaken, where dysregulation of those receptors leads to neurodegeneration in a variety of disorders, including Alzheimer’s disease. The main difference between AMPA and NMDA receptors is that sodium and potassium increases in AMPA receptors where calcium increases along with sodium and potassium influx in NMDA receptors. Moreover, AMPA receptors do not have a magnesium ion block while NMDA receptors do have a calcium ion block. AMPA and NMDA are two types of ionotropic, glutamate receptors. They are non-selective, ligand-gated ion channels, which mainly enable the passage of sodium and potassium ions. Furthermore, glutamate is a neurotransmitter which creates excitatory postsynaptic signals in the CNS.
For many years, most neuroscientists believed we were born with all the neurons we were ever going to carry in our brains. As children, we may develop new neurons to help create the pathways, known as neural circuits, which function as information highways between different regions of the brain. However, scientists believed that after a neural circuit was created, developing any new neurons could interrupt the flow of information and disable the brain’s communication system.
Neurogenic inflammation, or NI, is the physiological process where mediators are discharged directly from the cutaneous nerves to commence an inflammatory response. This results in the creation of local inflammatory reactions including, erythema, swelling, temperature increase, tenderness, and pain. Fine unmyelinated afferent somatic C-fibers, which respond to low intensity mechanical and chemical stimulations, are largely responsible for the release of these inflammatory mediators. When stimulated, these nerve pathways in the cutaneous nerves release energetic neuropeptides, or substance P and calcitonin gene related peptide (CGRP), rapidly into the microenvironment, triggering a series of inflammatory responses. There is a significant distinction in immunogenic inflammation, that’s the very first protective and reparative response made by the immune system when a pathogen enters the body, whereas neurogenic inflammation involves a direct connection between the nervous system and the inflammatory responses. Even though neurogenic inflammation and immunologic inflammation can exist concurrently, the two are not clinically indistinguishable. The purpose of the article below is to discuss the mechanism of neurogenic inflammation and the peripheral nervous system’s role in host defense and immunopathology.
|
Alzheimer’s disease (AD) is one of the most common types of dementia among older adults. Research studies have demonstrated that pathological changes in the human brain, whether directly or indirectly, can ultimately cause loss of synaptic function, mitochondrial damage, microglial cell activation, and neuronal cell death. However, the pathogenesis of AD is not yet fully understood and there is currently no definitive treatment for the neurological disease. Research studies have demonstrated that the activation and priming of microglial cells may contribute to the pathogenesis of AD. A proinflammatory status of the central nervous system (CNS) can also cause changes in the function of the microglial cells or microglia. Neuroinflammation is closely associated with the activation of microglia and astrocytes which are connected to a variety of neurological diseases by the synthesis and secretion of inflammatory mediators such as iNOS, ROS, and proinflammatory cytokines. According to research studies, microglial priming is also caused by the inflammation of the CNS. Therefore, whether microglial priming is the result or the cause of neuroinflammation is still controversial. Microglial cell activation commonly causes an increase of Aβ and tau proteins as well as a decrease of neurotrophic factors, ultimately leading to the loss of healthy brain cells or neurons and the development of neuritic plaques and neurofibrillary tangles which are closely associated with AD. With the progression of Alzheimer’s disease, changes from neuronal dysfunctions which may have no obvious symptoms to memory loss and cognitive impairment may become more noticeable.
Low-level laser therapy (LLLT), also known as photobiomodulation, is the use of low-power lasers or light-emitting diodes (LEDs) for treatment purposes. When LLLT is used on the brain, it is known as transcranial LLLT or transcranial photobiomodulation. Many research studies have shown that LLLT can help treat a variety of brain health issues. Different from high-intensity surgical lasers, low-powered lasers do not cut or burn tissue. Instead, these lasers stimulate a biological reaction and promote cells to function properly. Moreover, it’s also easy to use LLLT utilizing red and near-infrared light on your own home. In the article below, we will discuss the brain health benefits of low-level laser therapy (LLLT).
The human brain is made up of approximately billions of small cells which utilize electrical impulses and chemical signals to communicate with one another and other parts of the human body. These are known as neurons. When neurons stop functioning properly, it can cause a variety of brain disorders, such as Alzheimer’s disease, epilepsy, and even depression. Researchers developed several treatment methods and techniques of brain stimulation which allow them to control neural activity to better understand and regulate these type of health issues. In conventional treatment methods and techniques of deep brain stimulation, electrical neurostimulators, also known as “brain pacemakers,” are surgically implanted in the brain. Researchers also developed non-invasive treatment approaches to stimulate cells found deep within the brain. While several researchers utilize magnetic pulses or sound waves to stimulate neurons, researchers in the optogenetics utilize light therapy. Shuo Chen, Ph.D., winner of Science and PINS Prize for Neuromodulation, was recognized for his work in this area. “Dr. Chen demonstrated that near-infrared light, when utilized with certain nanoparticles, allowed the stimulation of neurons deep within the brain,” stated Dr. Karl Deisseroth, professor of bioengineering, psychiatry and behavioral sciences at Stanford University. “More research studies are needed to make this a useful process,” he said, “but Dr. Chen took a key step.”
Central nervous system, or CNS, infections can be life-threatening if they are not diagnosed and treated early. Because CNS infections are non-specific, determining an accurate diagnosis can be challenging. The nucleic acid in vitro amplification-based molecular methods are starting to be utilized for routine microbial diagnosis. These molecular methods have improved beyond conventional diagnostic techniques with increased sensitivity and specificity. Moreover, molecular methods utilized on cerebrospinal fluid samples are considered the new standard for diagnosis of CNS infections caused by pathogens. Molecular methods for the diagnosis of CNS infections offers a variety of monoplex and multiplex PCR assays to diagnose several types of health issues. Pan-omic molecular platforms can also help diagnose CNS infections. Although molecular methods are utilized for the diagnosis of CNS infections, the outcome measures for these diagnostic techniques must be carefully identified by healthcare professionals. The following article discusses conventional diagnostic techniques and molecular methods utilized for the diagnosis of central nervous system infections, their application, and future approaches.
We often think of proteins are nutrients found in the food we eat and the main component of muscles, however, proteins are microscopic molecules located inside of cells which actually perform a variety of fundamental roles. The function of a protein depends on its shape, and when protein formation goes awry, the resulting misshapen proteins can cause numerous health issues, such as when proteins neglect their essential roles or when they form a sticky, clumpy clutter inside of cells. Protein formation is an error-prone procedure and mistakes along the way have been associated with neurological diseases. There are approximately 20,000 to over 100,000 unique types of proteins found inside a common human cell. Why so many? Proteins are the workhorses of the human cell. By way of instance, several of these proteins are structural, lending stiffness and rigidity to thin neurons or muscle tissues. Other proteins shuttle them to new places and bind to specific molecules and others catalyze responses. A property of proteins is possible through diversity and specificity in their role when they fold.
Cerebrovascular disease is characterized as a group of diseases, conditions, and disorders which ultimately affects the blood vessels and the blood supply to the human brain. Brain damage can occur when a blockage, malformation, or hemorrhage prevents the brain cells from receiving enough oxygen. Cerebrovascular disorders can include stroke, transient ischemic attack or TIA, aneurysm, and vascular malformation. Cerebrovascular disease can develop due to a variety of health issues, such as atherosclerosis, where the arteries become narrow; thrombosis or embolic arterial blood clot, which is a blood clot in an artery of the brain; or cerebral venous thrombosis, which is a blood clot in a vein of the brain. In the United States, cerebrovascular disease is one of the most common causes of death. In 2017, it caused about 44.9 deaths per 100,000 individuals or 146,383 deaths in total. Fortunately, people can decrease their risk of developing cerebrovascular disease. In the following article, we will describe the types, the symptoms, the diagnosis, and the treatment for cerebrovascular disease and how to prevent them.
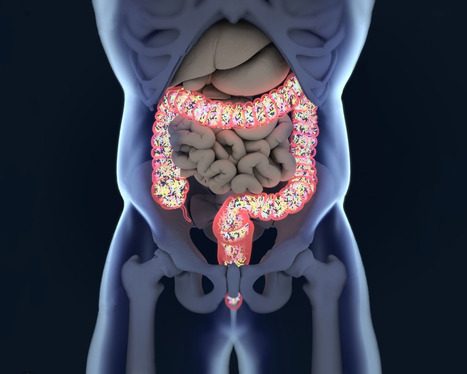
You Are What You Eat The phrase, “You are what you eat” implies that the way we are defines us as the food we all consumed. However, our gut tells us otherwise as the food we eat, may, in fact, be leading us to obesity. Our gut plays a role in our overall health, when we eat good food our gut is happy and when we eat bad food our gut will tell us by fighting off the bad food. A recent study showed us that the bacteria in our gut produce amyloid and lipopolysaccharides. These two microbiomes seem to show us that together, with proper dieting that these microbiomes can prevent Alzheimer’s Disease. As the microbiomes and the bacteria that co-exist in our gut, there are the two most predominant groups that have also played a key role in our lifestyle: gram-positive Firmicutes and gram-negative Bacteroidetes- both play a huge role in obesity. Firmicutes are bad bacteria that lead us to obesity. When we eat processed food and sugars, our body starts to crave it more, thus leading us to be overweight. Junk Food When we eat junk food, all that sugar and fat are feeding the Firmicutes. Firmicutes thrive on sugar since our bodies need it and it can be both good or bad While Bacteroidetes are the good bacteria that leads us to a healthy gut. Bacteroidetes are in the stomach regions as well as the Firmicutes. These two predominant bacteria groups tell us that the food we eat can actually affect our bodies when we eat bad foods or good foods. However, Dr. Kristen Senella mentioned that we all have a different balance of Firmicutes and Bacteroidetes since we are all different shapes and sizes. Depending on our health and food lifestyle, we can have either a low Firmicutes and a high Bacteroidetes or a high Firmicutes and a low Bacteroidetes. Plus, having either a high or low count of Firmicutes can lead to weight gain or weight loss; depending on which healthy lifestyle and exercise regime you are following. Gram-Positive Gram-positive bacteria will appear blue or violet, while gram-negative bacteria will appear red or pink under the microscope. When studying the gut and the bacteria groups that it is hosting, scientist use mice to study how their guts react to different diets they are put through so that way we, as humans, can take either pills to help our bodies maintain a healthy lifestyle or to read and do our own research. One group is fed in a healthy lifestyle and doesn’t experience diseases or ailments that we face. And the other group is fed with a bad lifestyle where they are prone to many of the diseases and fatigue as their life span is shortened very quickly. In order for us to actually maintain a healthy lifestyle and importantly feel good is to make sure our Firmicutes are not too dangerously low, but we can control it with probiotics. Probiotics Probiotics can vary from yogurt, fermented vegetables, kombucha, and miso. But there are certain companies that also reign supreme in the probiotic market. Activia yogurt and Yakult are two of the most well-known companies that use the live microorganisms to help us maintain a healthy lifestyle as well as keeping our gut’s microbiome in check. When we have some sort of probiotic foods in our system, we are preventing certain ailments and diseases going out of control. Like our cholesterol, blood pressure, being lactose intolerant, or recurring abdominal pains. When we mix probiotics into our food when we are trying to maintain a healthy lifestyle, we can see a vast improvement in how we have more energy, we feel full that we don’t have to overeat or mindless snacking, and overall we feel good in our gut as we go through our daily routine. From 2007 to now, roughly 3.9 million Americans use probiotics to maintain a healthy gut, however, those probiotics are just a fraction of what the six types of foods that can help maintain a healthy gut microbiome to help support a healthy lifestyle. Healthy Lifestyle For instance, a good healthy lifestyle is eating your basic food groups; whether it be plant-based or omnivorous, as well as, exercising a couple of times out of the year. A bad healthy lifestyle is eating processed food and not exercising, which leads to obesity and cardiac arrest. Depending on the person and the efforts that they are willing to maintain a healthy lifestyle, they can achieve longevity by taking care of their gut first and foremost. Protein Let’s start with protein. Protein can vary with lean meats like chicken and beef or plant-based like beans, legumes or tofu. Any of these types of protein can help our bodies by making us make our muscles grow, but also control the bacteria in our guts. Next up is fats. Fats can vary like good and bad bacteria. There are good fats like fish, nuts, olive oil, and avocado; as well as, bad fats like butter, lard, and fatty foods. Granted that we can overindulge on the trans fats as there are many fast-food chains, but we can moderate ourselves to not eat out at fast food joints all the time. Yes, they are cheap and easy to access, however now and days, we as humans are now cooking more in our homes and meal prepping our meals to be healthier. Digestible and Non-Digestible Carbohydrates are mostly starch, sugars, and fibers. These two food groups can make our gut feel happy or upset depending on the food we consume. Sugars, starches, and fibers help our bodies by feeling full with the starches, the fibers help our bowel movements in case our gut feels bloated, and the sugars gives us microburst of energy for our fast-paced lives. Fermented & Polyphenols The last two food groups are fermented food and Polyphenols. Both of these food groups have amazing properties since we see them everywhere in the food market, hiding in plain sight. Fermented foods like yogurt and kimchi are a few examples of ways of keeping our guts happy and stopping many diseases. Polyphenols are antioxidant foods like dark chocolate, berries, dark greens, and certain fruits. These help our gut curb that sugar hunger and all in all taste really good. All in all, our gut microbiomes are important to us and our overall health as we all try to maintain and achieve a healthy lifestyle. The phrase “we are what we eat” still implies to all of us, however, it is up to us to actually put in the work and constantly try out different foods to make sure that our gut is still functioning properly. No matter which diet you choose, pick one that will work with your body and your gut since we all are made differently. But our gut should be the first thing that we should listen to. Cites: Role of gut microbiota and nutrients in amyloid formation and pathogenesis of Alzheimer disease. - PubMed – NCBI: https://www.ncbi.nlm.nih.gov/pubmed/27634977 Bacteroidetes Glossary Biome360: https://www.biome360.com/glossary/bacteroidetes/ What are Firmicutes? : https://www.biome360.com/blog/firmicutes/ Bacteria and the body – Wikiversity: https://en.wikiversity.org/wiki/Bacteria_and_the_body#Gram-positive_bacteria Nanoparticle relieved symptoms of inflammatory bowel disease in mice: https://phys.org/news/2019-08-nanoparticle-relieved-symptoms-inflammatory-bowel.html Probiotic: https://en.wikipedia.org/wiki/Probiotic Polyphenols: What They Are, and Why You Need Them: https://articles.mercola.com/sites/articles/archive/2015/12/14/polyphenols-benefits.aspx
Neural cell death can occur both during the development and throughout the pathophysiology of the nervous system. Two different types of cell death, known as necrosis and apoptosis, are involved in pathological neuronal loss, however, apoptosis is the process of programmed cell death during development. All types of cells will go through apoptosis. This mechanism controls neuronal growth where an excess of neurons is produced and only those which form connections with the target structures will receive enough survival factors. The remaining neurons will then ultimately go through death and removal. Apoptosis continues throughout life and it is the main process involved in the elimination of surplus, unwanted, damaged or aged cells. Dysregulation of apoptosis is demonstrated after damage or injury as well as in neurodegeneration and in tumorigenesis. Treatment approaches which influence the apoptotic pathway offer valuable therapeutic options in a wide variety of pathological states. The purpose of the article is to describe the significance of apoptosis in neurological diseases.
In humans, the nervous system consists of the central nervous system and the peripheral nervous system. The central nervous system, or CNS, consists of the brain and the spinal cord. It is in the CNS where the review of information occurs. The peripheral nervous system, or PNS, consists of the neurons and parts of neurons outside the CNS, including sensory neurons and motor neurons. Sensory neurons bring signals into the CNS, and motor neurons carry signals out of the CNS. The cell bodies of PNS neurons, such as the motor neurons which control skeletal muscles, are found in the CNS. These motor neurons have long extensions, known as axons, which run from the CNS all the way to the muscles with which they connect with or innervate. The cell bodies of additional PNS neurons, such as the sensory neurons which provide information on touch, pain, position, and temperature, are found outside the CNS, in which they are found in clusters known as ganglia. The axons of peripheral nerves which run through a common pathway are bundled together to form nerves.
Functional neurology primarily focuses on the fundamentals of neuron health and it is mainly based on neuroplasticity theories. It’s believed that the brain and the nervous system are capable of changing, and can become malleable, due to a reaction to certain stimulation. The brain can be shaped by sensory, motor, cognitive, or emotional experiences. The creation of synapses in the nervous system depends on the stimulation they receive. Neurons which receive too much stimulation are the ones which become stronger and those which don’t receive stimulation become weaker and eventually diminish. It is believed that it is possible to create new neurons even after there has been damage to the nervous system.
Until only several decades ago, neuroscientists believed that the brain stopped creating new neural connections, meaning that your memory starts to become irreversibly worse when the human body stopped developing, which is generally in your early 20s. Neuroscientists also understood that neurons weaken and die as we age. The loss of brain function due to neural breakdown was believed to be a normal part of aging until recent research studies demonstrated the opposite of this belief. Over the last several years, it has become evident to neuroscientists that you can, as a matter of fact, create new neurons and develop new neural connections starting in your early 20s and continuing well into your old age. As the older regions of the brain start to wear out, you can ultimately rewire your brain and improve your overall brain health. But, how can you improve brain health? In the following article, we will discuss 5 ways you can improve your brain health and promote your well-being.
Neurological diseases are characterized as health issues associated with the brain, the spine, and the nerves which connect them. Neurological disease is considered to be one of the most prevalent health issues with a high burden to the patients, their families, and society. However, there are now estimates of the burden of neurological diseases in the United States.
|

 Your new post is loading...
Your new post is loading...




























Traumatic brain injury is among one of the most prevalent causes of disability and death among the general population in the United States. According to a variety of research studies, mild, moderate, and severe traumatic brain injury has been associated with neurodegenerative diseases, such as Alzheimer’s disease, as well as a variety of other neurological diseases and health issues. It is fundamental to understand the pathophysiological mechanisms of traumatic brain injury while further research studies are still required to determine the association between TBI and neurodegenerative diseases. For more information, please feel free to ask Dr. Alex Jimenez or contact us at (915) 850-0900.