 Your new post is loading...
 Your new post is loading...
Knee meniscus injuries are common in athletes, workers, and active adults. The meniscus is a C-shaped piece of fibrocartilage that helps absorb shock, distribute forces across the knee, improve stability, support lubrication, and enhance joint awareness during movement. Because the meniscus does so much work, even a small tear can lead to pain, swelling, catching, stiffness, and trouble walking, squatting, or turning. Protecting and preserving the meniscus matters because loss of meniscal function can increase joint stress and may raise the risk of later knee degeneration and osteoarthritis (Patil et al., 2017; Razi et al., 2020). Why Meniscus Tears Can Be Hard to Heal One reason meniscus injuries are challenging is that not every part of the meniscus gets the same blood supply. The outer zone has better circulation and usually has a stronger healing potential. The inner zone has poor blood flow, which slows and makes natural repair less reliable. That is why treatment decisions often depend on the tear's location, size, pattern, severity, and the patient's age and activity level. In simple terms, a tear near the outer rim may heal more easily than one deeper in the low-blood-flow inner portion (Shahid et al., 2017). What PRP Is Platelet-Rich Plasma, or PRP, is made from a sample of the patient's own blood. The blood is processed so the platelets become more concentrated in the plasma. Platelets contain signaling proteins and growth factors that help the body respond to injury. In musculoskeletal care, PRP is used as a minimally invasive treatment to support healing, reduce inflammation, alleviate pain, and improve function in certain joint and soft-tissue conditions (Johns Hopkins Medicine, 2026a; Johns Hopkins Medicine, 2026b). How PRP May Help a Torn Meniscus The main idea behind PRP for meniscus injuries is not that it magically rebuilds every tear, but that it may create a better healing environment. Growth factors in PRP are thought to support cell signaling, collagen activity, tissue remodeling, angiogenesis, and control of inflammation. For a meniscus tear, especially one in a poorly vascularized area, this may help calm irritation and encourage repair processes that would otherwise be weak or slow. This is why PRP has drawn attention as both a non-surgical option and an add-on to repair procedures in some patients (El Zouhbi et al., 2024; Liang et al., 2025). What the Research Shows So Far A 2024 narrative review on PRP for meniscus injuries reported that short-term results are promising. Across the reviewed studies, PRP was associated with improvements in pain, symptoms, daily function, and sports activity in many patients, particularly in studies with follow-up of less than 1 year. Some imaging findings also suggested that meniscal conditions were stable after treatment. At the same time, the review made an important point: long-term effectiveness remains unsettled, and study methods vary widely across papers. That means PRP looks encouraging, but it should be presented honestly as a treatment with promise, not as a guaranteed cure (El Zouhbi et al., 2024). Other research reaches a similar middle ground. Some clinical studies and reviews suggest PRP may help symptom relief, support healing, and lower failure rates when used with meniscal repair in selected cases. However, results are not perfectly consistent across all studies, partly because researchers use different PRP preparation methods, injection techniques, tear types, and follow-up periods. A 2025 study on grade II meniscal tears showed a trend toward improved healing with precise PRP treatment, but the difference was not statistically significant compared with controls at all follow-up points. This supports a balanced conclusion: PRP may help some patients, but good patient selection is critical (Yang et al., 2021; Shayan et al., 2025). Who May Benefit Most PRP tends to make the most sense for carefully selected patients rather than everyone with knee pain. It may be considered for people with stable meniscal injuries, mild-to-moderate symptoms, or tears in which a clinician believes tissue preservation is still realistic. It may also appeal to patients who want to delay or avoid surgery when appropriate. People with major mechanical locking, severe displaced tears, or advanced structural damage may still need surgical evaluation. In other words, the best outcomes usually occur when the tear type, knee mechanics, and overall patient goals align with the treatment (El Zouhbi et al., 2024; Patil et al., 2017). Why Success Depends on Tear Location, Severity, and Age The statement that success depends on tear location, severity, and patient age is well supported by meniscus science. Location matters because the outer meniscus heals better than the inner avascular region. Severity matters because small stable tears behave differently from complex, degenerative, or displaced tears. Age matters because tissue quality, healing speed, and the presence of arthritis often change over time. This does not mean older adults cannot improve with PRP, but it does mean expectations should be individualized. A younger patient with a smaller peripheral tear may have a very different response than an older patient with a degenerative tear and joint wear (Shahid et al., 2017; El Zouhbi et al., 2024). PRP as Part of a Non-Surgical Knee Preservation Plan One of the most important ideas in modern knee care is preservation. Because the meniscus plays such a major role in distributing force and protecting cartilage, clinicians increasingly try to preserve meniscal tissue whenever possible. PRP fits into this goal because it may reduce symptoms and support healing without removing tissue. In some cases, that can delay surgery, reduce irritation enough for better rehabilitation progress, or serve as an adjunct after repair. Even when PRP does not fully "heal" a tear on imaging, it may still help the patient move with less pain and better function, which is clinically meaningful (Razi et al., 2020; Weber et al., 2018). Where Integrative Chiropractic Care Fits In Integrative chiropractic care does not replace orthopedic evaluation or regenerative procedures, but it can support the overall recovery plan. When the knee hurts, people often change the way they walk, stand, squat, and climb stairs. Over time, that may affect the ankle, hip, pelvis, and lower back. Chiropractic and movement-based care may help improve joint mechanics, reduce compensations, ease surrounding soft-tissue tension, and restore movement patterns. The goal is not to "push a torn meniscus back into place" but to improve how the body loads and protects the injured knee during healing (Cognetti et al., 2024). Supportive care around the knee often includes: - Gait and posture assessment
- Hip, ankle, and pelvic mobility work
- Soft tissue treatment for tight surrounding muscles
- Progressive strengthening of the quadriceps, hamstrings, glutes, and calf muscles
- Balance and proprioception training
- Activity modification to reduce overload without complete deconditioning
These strategies matter because stronger surrounding muscles and better movement control can improve joint stability and function while reducing unnecessary stress on the healing meniscus (Cognetti et al., 2024; Hammami et al., 2023). Clinical Observations from Dr. Alexander Jimenez Dr. Alexander Jimenez, DC, APRN, FNP-BC, publicly describes a dual-scope model that combines chiropractic care with nurse practitioner medical insight, functional medicine, rehabilitation planning, and integrative support. On his website and LinkedIn, he emphasizes integrating patient history, physical examination, imaging, movement mechanics, and personalized rehabilitation to develop practical recovery plans. In knee and sports-related cases, this kind of model may be useful because meniscus pain is rarely limited to a single structure; it often involves inflammation, altered biomechanics, strength deficits, and lifestyle factors that affect healing (Jimenez, n.d.-a, n.d.-b, n.d.-c). From a clinical observation standpoint, Dr. Jimenez's public materials repeatedly stress several themes that fit meniscus recovery well: - Preserve function when possible
- Use non-invasive care before more invasive options when appropriate
- Improve alignment and mechanics across the whole lower body
- Pair treatment with rehabilitation and lifestyle support
- Track symptoms, function, and response over time rather than relying on one intervention alone
Those observations are consistent with a comprehensive, non-surgical knee strategy, although the strength of the evidence should still be based on published research rather than clinic marketing materials alone (Jimenez, n.d.-a; Jimenez, n.d.-c). What Patients Should Expect PRP is usually done in an outpatient setting. Blood is drawn, processed, and then the PRP is injected into the target area. Results are not usually instant. Johns Hopkins notes that for joint injections, benefits are often noticed over several weeks, and some patients may need additional injections based on clinical response. The treatment is generally considered minimally invasive because it uses the patient's own blood products, but it still needs proper diagnosis, sterile technique, and realistic expectations (Johns Hopkins Medicine, 2026a). Recovery usually works best when PRP is combined with a smart rehab plan rather than treated like a stand-alone shortcut. Early care may focus on reducing overload and irritation. As symptoms improve, the emphasis usually shifts toward restoring range of motion, muscle strength, knee stability, and functional movement. This step matters because even if biologic healing improves, the knee still needs coordinated muscle support to handle walking, work, exercise, and sport safely (Symmetry Physical Therapy, n.d.; Monson et al., 2025). A Realistic Bottom Line Regenerative medicine, especially PRP therapy, offers a promising non-surgical option for some knee meniscus injuries. It may reduce inflammation, lessen pain, and support healing in tissue that often struggles to repair on its own. For the right patient, PRP may delay surgery or help avoid it altogether. Still, outcomes depend on the tear's location, severity, tissue quality, age, biomechanics, and the quality of the rehabilitation plan. The best approach is usually not PRP alone, and not chiropractic alone, but a coordinated plan that protects the meniscus, improves joint mechanics, restores strength, and follows the patient's symptoms and function over time (El Zouhbi et al., 2024; Johns Hopkins Medicine, 2026a; Cognetti et al., 2024). Knee Pain Rehabilitation | El Paso, Tx References El Zouhbi, A., Yammine, J., Hemdanieh, M., Korbani, E. T., & Nassereddine, M. (2024). Utility of Platelet-Rich Plasma Therapy in the Management of Meniscus Injuries: A narrative review Orthopedic Reviews, 16. https://doi.org/10.52965/001c.94240 Hammami, N., Rebai, H., Sahli, S., et al. (2023). Concentric isokinetic strengthening program's impact on physical and functional outcomes in women with chronic meniscal lesions Healthcare. Jimenez, A. (n.d.-a). El Paso, TX Doctor Of Chiropractic | Dr. Alex Jimenez, DC, APRN, FNP-BC Jimenez, A. (n.d.-b). Dr. Alexander Jimenez, DC, APRN, FNP-BC, IFMCP, CFMP Jimenez, A. (n.d.-c). Chiropractic Care Methods for Ligament Injuries & Knee Pain Johns Hopkins Medicine. (2026a). Platelet-Rich Plasma (PRP) Injections Johns Hopkins Medicine. (2026b). Musculoskeletal Platelet-Rich Plasma Injections Johns Hopkins Medicine. (2025). Knee Injections for Pain Relief Liang, J., et al. (2025). Efficacy and Safety of Platelet-Rich Plasma for Patients With Meniscal Injuries Cureus. Monson, J. K., et al. (2025). Current Rehabilitation Principles Following Meniscus Repairs Current Reviews in Musculoskeletal Medicine. Patil, S. S., Kumar, H., & Varghese, M. (2017). Meniscal Preservation is Important for the Knee Joint Indian Journal of Orthopaedics. Razi, M., et al. (2020). Save the Meniscus, A Good Strategy to Preserve the Knee EFORT Open Reviews. Shahid, M., Kundra, R., & Malhotra, R. (2017). Platelet-rich plasma (PRP) for knee disorders EFORT Open Reviews. Shayan, R., et al. (2025). Evaluating the efficacy of precise platelet-rich plasma injections in grade II meniscal tears International Journal of Burns and Trauma. Weber, J., Koch, M., Angele, P., & Zellner, J. (2018). The role of meniscal repair for prevention of early onset of osteoarthritis Journal of Experimental Orthopaedics. Yang, C. P., et al. (2021). Clinical Outcomes of Meniscus Repair with or without Multiple Intra-Articular Platelet-Rich Plasma Injections Journal of Clinical Medicine. The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and facilitate clinical collaboration with specialists across disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and identify relevant research studies for our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We are here to help you and your family. Blessings Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182 Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-State Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
New York APRN License #: N25929, Verified: APRN-N25929*
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States* Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Building a weekly workout routine is not about going “all out” every day. It’s about training with a plan so your body can adapt, get stronger, and stay healthy. In a place like El Paso—where heat, sun, and dry air can change how you feel during exercise—your routine should balance: -
Strength training (to build muscle and protect joints) -
Cardio (to support heart and lung fitness) -
Mobility and movement quality (to keep you moving well) -
Recovery (so your body can rebuild) A practical target for many adults is to complete at least 150 minutes of moderate-intensity activity per week, plus 2 days of strength training, then build up based on goals and recovery (Centers for Disease Control and Prevention [CDC], 2025). Just as important, most workouts should include a 5–10-minute warm-up and a 5–10-minute cooldown. A warm-up gradually increases your heart rate and prepares muscles and joints. A cooldown helps your body return to baseline more smoothly and supports flexibility work after training (Mayo Clinic, 2023; Mayo Clinic Press, 2025). Why routine structure matters (especially if you’re busy) A good weekly plan helps you: -
Train each major muscle group enough times to improve -
Avoid repeating the same stress on the same joints every day -
Reduce “random workouts” that feel hard but don’t build consistency -
Recover better, so you can show up next session A common beginner-to-intermediate sweet spot is 3–5 training days per week, with at least 1–2 recovery-focused days (EōS Fitness, 2024; SELF, 2026). Warm-up and cooldown basics (simple, safe, and repeatable) The 5–10 minute warm-up (dynamic) A warm-up is usually light movement + dynamic motion that matches what you’re about to do. Examples that work for most workouts: -
2–3 minutes easy walk, bike, or row -
3–5 minutes dynamic mobility (hips, ankles, thoracic spine, shoulders) -
1–2 “practice sets” of your first lift (lighter weight) Mayo Clinic describes warming up by starting the activity at a slow pace and gradually building intensity, then cooling down by doing the activity at a lower intensity for ~5 minutes (Mayo Clinic, 2023).
ISSA also notes that warm-ups typically range from 5–15 minutes, depending on workout length and intensity (ISSA, 2022). Quick dynamic warm-up flow (5–8 minutes): -
30–60 seconds brisk walk or march in place -
8–10 bodyweight squats (slow and controlled) -
8–10 hip hinges (hands on hips, practice the pattern) -
6–8 alternating lunges (short range if stiff) -
8–12 band pull-aparts or wall slides (upper back/shoulders) -
20–30 seconds plank or dead bug (core activation) The 5–10 minute cooldown (downshift + stretch) Cooldowns often look like: Mayo Clinic Press emphasizes using slow movement and stretching to gradually reduce heart rate after exercise (Mayo Clinic Press, 2025).
Some fitness education sources recommend allocating 5–10 minutes for warm-ups and cooldowns as a practical rule (Westwood Fitness, 2025).
Research discussions also note that cool-down practices vary, and the strongest evidence depends on the outcome you care about (like performance vs. soreness), but a short downshift is still widely used for safe transitions and flexibility work (Van Hooren & Peake, 2018).
Simple cooldown (8 minutes): -
3 minutes easy walk -
30 seconds calf stretch (each side) -
30 seconds hip flexor stretch (each side) -
30 seconds hamstring stretch (each side) -
30 seconds chest/pec stretch (each side) -
60–90 seconds slow nasal breathing (hands on ribs) The El Paso factor: heat, dryness, and smart scheduling El Paso workouts can feel harder when it’s hot and dry. Two practical strategies: -
Train earlier or later when temps are lower -
Hydrate more intentionally, especially if you sweat a lot One heat-safety resource recommends adjusting intensity in the heat, staying hydrated, and considering electrolytes for longer/hotter sessions (One Medical, 2023).
(If you have blood pressure, kidney, or heart conditions—or you’re unsure—check with your clinician before adding electrolyte supplements.) Hot-weather training checklist: -
Bring water every session (even short ones) -
Use a “talk test”: you should be able to speak in short sentences for most cardio -
Reduce intensity on extreme-heat days rather than skipping the week entirely -
Choose indoor options (gym, track, treadmill, rower) when needed How to choose the right weekly routine (3-day, 4-day, or 5-day) Think of your plan like a menu. Your “best” routine is the one you can repeat weekly without burning out. Option A: 3 days/week (full-body strength + light cardio) This is a strong starting point for many people, especially if you want joint-friendly progress. Weekly layout (example): -
Mon: Full-body strength + short cardio finish -
Wed: Full-body strength + mobility -
Fri: Full-body strength + easy cardio -
2 optional days: walking, easy biking, yoga, or recovery work Some programs schedule strength sessions (e.g., Mon/Wed/Fri) to allow recovery between sessions (EōS Fitness, 2025). Option B: 4 days/week (upper/lower split) Good if you want more volume without making each workout too long. Weekly layout (example): Split routines are commonly used because they organize training stress and recovery across the week (EōS Fitness, 2024). Option C: 5 days/week (strength + cardio + mobility) Best for people who recover well and enjoy training most days. A common fitness guideline for weekly planning is a mix of strength, cardio, and recovery, rather than doing hard sessions daily (Health.com, 2025; SELF, 2026). A practical 7-day template you can copy (beginner-to-intermediate) This sample structure aligns with many mainstream weekly plans: cardio, strength, and recovery days (Health.com, 2025). Monday — Cardio + Core (35–50 min) -
Warm-up 5–10 min (walk + dynamic hips/ankles) -
Cardio 20–30 min (zone 2 pace: steady, can talk) -
Core 8–10 min (dead bug, side plank, carry) -
Cooldown 5–10 min (walk + stretch) Tuesday — Lower Body Strength (45–60 min) -
Warm-up + movement prep -
Squat pattern (goblet squat or back squat): 3–4 sets -
Hinge pattern (RDL or hip hinge): 3–4 sets -
Split squat or step-up: 2–3 sets -
Calves + short mobility finish -
Cooldown Wednesday — Upper Body + Core (45–60 min) -
Warm-up (shoulders + upper back) -
Push (incline press or push-ups): 3–4 sets -
Pull (row variation): 3–4 sets -
Overhead press (light/moderate): 2–3 sets -
Lat pull-down or band pulls: 2–3 sets -
Cooldown Thursday — Active recovery (20–45 min) -
Easy walk, gentle bike, yoga, or mobility session -
Keep it light. This is a “feel better” day. Friday — Full Body Strength (45–60 min) -
Warm-up -
Deadlift pattern (trap bar or hinge focus): 3 sets -
Lunge pattern: 2–3 sets -
Push + pull superset: 3 rounds -
Farmer carry or sled work (if available): 4–6 short rounds -
Cooldown Saturday — Choice cardio or class (30–60 min) -
Choose something enjoyable: steady cardio, intervals, hiking, or a group class -
If it’s hot: go early, shorten it, or go indoors (One Medical, 2023). Sunday — Rest What “balanced” really means (so you don’t burn out) A balanced routine usually includes: -
2–4 days of strength training -
2–3 days cardio (some easy, some harder) -
1–2 mobility/recovery days -
At least 1 true rest day when needed If you’re unsure how hard to go, use this simple guide: -
Easy days: you could do them again tomorrow -
Hard days: you’ll need recovery time -
Most weeks should have more easy/moderate training than all-out training Integrative chiropractic: how it can support training (and help prevent injuries) Many people wait until pain forces them to stop training. A smarter approach is to treat movement quality like a skill. Integrative chiropractic care is often used alongside training to support: -
Posture and spinal alignment -
Joint mobility where you’re stiff -
Neuromuscular control (how well muscles “turn on” during movement) -
Recovery strategies when training load increases Clinical writing from Dr. Alexander Jimenez frequently emphasizes combining chiropractic care with whole-person planning—mobility, neuromuscular balance, and movement strategies—so workouts feel smoother and more stable (Jimenez, 2025a).
He also describes using integrative strategies to reduce injury risk by addressing imbalances before they become pain problems (Jimenez, 2025b). A research review on chiropractic in sports contexts discusses how addressing musculoskeletal imbalances and biomechanical factors can support athletic recovery and performance (Lin et al., 2023). Where chiropractic fits best in a weekly routine: -
Before a training block (2–6 weeks): improve mobility and movement patterns -
During a training block: support recovery and reduce flare-ups -
When increasing load: help manage joint stress and technique breakdown -
After minor strains: guide safer return-to-training progressions Simple example (weekly “stack”): -
Strength days: warm-up + lift + cooldown -
Recovery day: mobility + easy cardio -
Chiropractic check-ins: support alignment/mobility + movement coaching when needed Using local El Paso options to keep your routine consistent Consistency is easier when you have options for different days (especially during extreme heat). Examples of local-style choices mentioned in El Paso fitness spot roundups include yoga studios and group fitness environments (Fox Lexus of El Paso, 2020).
A structured boot camp class format can also help people who do better with coaching and a set schedule (Fit Body Boot Camp, n.d.).
You don’t need the “perfect” gym. You need a plan you’ll actually follow. Pick 1–2 “default” workouts for busy weeks: That way, if your week gets chaotic, you still have a minimum routine that protects progress. Common mistakes (and quick fixes) Mistake: skipping warm-ups Mistake: training hard every day Mistake: doing random exercises without progression Mistake: ignoring heat and hydration -
Fix: adjust timing, lower intensity, and hydrate more effectively in hot conditions (One Medical, 2023). Key takeaways you can use today -
Aim for 3–5 training days/week depending on recovery and schedule (EōS Fitness, 2024; SELF, 2026). -
Use a 5–10-minute warm-up and a 5–10-minute cooldown for most workouts (Mayo Clinic, 2023; Westwood Fitness, 2025). -
Build your week around strength + cardio + mobility + recovery -
In the El Paso heat, adjust intensity and timing rather than quitting for the whole week (One Medical, 2023). -
Integrative chiropractic can support mobility, posture, and movement quality, helping you train with fewer setbacks (Jimenez, 2025a; Lin et al., 2023). References -
Adding Physical Activity as an Adult (CDC, 2025). -
Adult Activity: An Overview (CDC, 2023). -
Aerobic exercise: How to warm up and cool down (Mayo Clinic, 2023). -
How to warm up and cool down for exercise (Mayo Clinic Press, 2025). -
Weekly Workout Plan: Your Simple 7-Day Fitness Routine (Health.com, 2025). -
Successful 7-Day Gym Workout Plan: How to Create Your Weekly Gym Routine (EōS Fitness, 2024). -
Here’s What a Perfect Week of Working Out Looks Like (SELF, 2026). -
How to Structure a Gym Workout for Optimal Results (ISSA, 2022). -
The Ultimate Guide to Warm-Ups and Cool-Downs (Westwood Fitness, 2025). -
6 Tips for Safe Summer Workouts in the Heat (One Medical, 2023). -
Physical Activities to Improve Posture with Chiropractic Support (Jimenez, 2025a). -
Integrative Therapies to Prevent Common Sports Injuries (Jimenez, 2025b). -
The Integration of Chiropractic Care into the Sports Industry: A Review (Lin et al., 2023). -
Sweat it Out at These El Paso Workout Spots (Fox Lexus of El Paso, 2020). -
Fit Body Boot Camp Gym in El Paso, TX (Fit Body Boot Camp, n.d.). -
Do We Need a Cool-Down After Exercise? A Narrative Review of the Psychophysiological Effects and the Effects on Performance, Injuries and the Long-Term Adaptive Response (Van Hooren & Peake, 2018). The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and identify relevant research studies for our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We are here to help you and your family. Blessings Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182 Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-State Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
New York APRN License #: N25929, Verified: APRN-N25929*
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States* Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master’s in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
A Practical, Integrative Guide for Strength, Stability, and Pain Prevention Lower back and hip pain are extremely common. Many people experience discomfort from muscle strains, poor posture, weak core muscles, tight hips, or spinal instability. These issues can affect daily movement, exercise, work, and sleep. When the muscles that support the spine and hips are weak or tight, the body often compensates in unhealthy ways, leading to pain and reduced mobility. Squats and core exercises are powerful tools when used correctly. They strengthen the muscles that stabilize the spine, improve hip mobility, and help the body move as a connected system instead of placing stress on one area. When combined with professional care, such as chiropractic treatment and nurse practitioner oversight, these exercises become part of a safe and effective plan for both short-term and long-term recovery. Why the Lower Back and Hips Are So Closely Connected The lower back and hips work together during almost every movement, including standing, walking, bending, lifting, and sitting. When one area is not functioning well, the other is forced to compensate. Common contributors to lower back and hip pain include: -
Tight hip flexors or glute muscles -
Weak abdominal and deep core stabilizers -
Poor posture during sitting, standing, or lifting -
Limited hip mobility -
Lumbar spine instability -
Muscle imbalances between the front and back of the body Research shows that poor movement patterns during squatting and bending can place excessive strain on the lower back, especially when the hips are stiff or the core is weak (Healthline, 2020; Carter PT, n.d.). How Squats Help the Lower Back and Hips Squats are a full-body movement that trains the hips, legs, and core to work together. When performed properly, squats help shift stress away from the lower back and onto the stronger muscles of the hips and legs. Benefits of Squats for Back and Hip Health -
Strengthen the glute muscles, which support the pelvis -
Improve hip mobility and joint control -
Reduce excessive spinal movement during bending -
Promote proper posture and alignment -
Improve balance and coordination When the hips move well during a squat, the lower back does not have to overwork. Studies and clinical observations show that many people with lower back pain experience relief once hip mobility and strength improve (Redefine Your Pain, n.d.; HSS, n.d.). The Role of Core Exercises in Spinal Stability The “core” is more than just the abdominal muscles. It includes deep stabilizing muscles that surround the spine and pelvis. These muscles help control movement and protect the spine during daily activities and exercise. Key core muscles include: -
Transverse abdominis -
Multifidus -
Pelvic floor muscles -
Diaphragm -
Obliques Core stability exercises help the spine stay neutral and controlled during movement. This reduces strain on spinal discs, joints, and ligaments (Cary Orthopaedics, n.d.; PMC, 2022). How Core Strength Reduces Lower Back Pain Core exercises help with lower back pain by: -
Improving spinal control during movement -
Reducing excessive bending or arching -
Supporting proper posture -
Distributing forces evenly through the body -
Preventing muscle fatigue and overload Clinical research supports core stabilization exercises as an effective approach for non-specific low back pain by improving the body’s ability to control spinal movement during functional tasks (PMC, 2022). Squats, Core Training, and Common Conditions When performed correctly and matched to the individual, squats and core exercises can help with several common conditions. Conditions That May Benefit -
Chronic low back pain -
Muscle strains -
Poor posture-related discomfort -
Lumbar instability -
Mild sciatica caused by muscular compression -
Hip stiffness and glute weakness For sciatica, strengthening the core and hips can reduce pressure on the sciatic nerve when symptoms are mild and related to muscular imbalance rather than severe nerve damage (Pecan Country Chiropractic, n.d.). Why Proper Form Matters So Much Squats and core exercises are only helpful when performed with good technique. Poor form can increase pain rather than reduce it. Key Form Principles for Squats -
Maintain a neutral spine -
Keep the core gently engaged -
Sit back through the hips, not the lower back -
Keep weight evenly distributed through the feet -
Avoid collapsing forward or rounding the spine Lower back pain during or after squats is often a sign that form, mobility, or strength needs to be addressed before continuing (Hinge Health, n.d.; One Peloton, n.d.). Warning Signs That Require Medical Evaluation Exercise should not cause sharp or worsening pain. Some symptoms require immediate professional evaluation. Seek medical care if you experience: -
Numbness or tingling in the legs -
Muscle weakness -
Pain that worsens with activity -
Loss of bladder or bowel control -
Pain following trauma or an accident These symptoms may indicate nerve compression or structural issues that require medical imaging and professional assessment. The Value of an Integrative Care Approach An integrative approach combines exercise with hands-on care and medical oversight. This model addresses both the mechanical and physiological causes of pain. Components of Integrative Management -
Chiropractic care to restore joint alignment and mobility -
Nurse practitioner evaluation for medical screening and diagnostics -
Guided exercise programming -
Movement education and posture correction -
Inflammation and pain management strategies This approach is commonly used for both acute injuries and chronic conditions, especially when muscle imbalance and joint dysfunction are present (Dr. Mauger, n.d.; Duke Health, n.d.). Clinical Observations from Dr. Alexander Jimenez Based on decades of clinical practice, Dr. Alexander Jimenez, DC, APRN, FNP-BC, observes that many patients with chronic back and hip pain improve significantly when movement training is paired with professional care. According to his clinical insights: -
Weak core muscles often limit the effectiveness of chiropractic adjustments -
Hip stiffness frequently contributes to recurring lower back pain -
Exercise alone is not enough if spinal alignment and joint mechanics are ignored -
Nurse practitioner involvement improves safety by identifying underlying medical conditions Dr. Jimenez emphasizes that restoring movement quality is just as important as building strength, especially for long-term pain relief and injury prevention (Jimenez, n.d.). Why Professional Guidance Is Essential Before starting a squat or core exercise routine, especially if you have existing pain or injury, professional guidance is critical. Healthcare professionals can: -
Assess movement patterns -
Identify mobility restrictions -
Modify exercises safely -
Rule out serious conditions -
Ensure proper progression Consulting a chiropractor, physical therapist, or medical provider helps ensure that exercises support healing rather than aggravate the problem (Harvard Health, 2011; Orthopedic Institute SF, n.d.). Practical Takeaways -
Squats and core exercises support lower back and hip health by improving strength, stability, and mobility. -
Proper form is essential to prevent injury -
Mild back and hip issues often respond well to guided strengthening -
Severe pain or neurological symptoms require medical evaluation -
An integrative approach provides the most comprehensive care When exercise is combined with chiropractic and nurse practitioner care, patients often experience better outcomes, fewer flare-ups, and improved quality of movement. Transform your Body! | El Paso, Tx References Healthline. (2020). Lower back pain when squatting.
https://www.healthline.com/health/back-pain/lower-back-pain-when-squatting Redefine Your Pain. (n.d.). Does squatting help or hurt lower back pain?
https://redefineyourpain.com/does-squatting-help-or-hurt-lower-back-pain/ Orthopedic Institute of San Francisco. (n.d.). Preventing back pain during exercise.
https://orthopedicinstitutesf.com/5-ways-to-prevent-back-pain-during-exercise-or-everyday-activities-according-to-experts/ Carter Physical Therapy. (n.d.). Lower back pain when squatting.
https://carterpt.com/blog/lower-back-pain-when-squatting Hinge Health. (n.d.). Hip pain when squatting.
https://www.hingehealth.com/resources/articles/hip-pain-when-squatting/ Cary Orthopaedics. (n.d.). Reducing low back pain through core strength.
https://caryortho.com/reduce-low-back-pain/ Hospital for Special Surgery. (n.d.). Back pain after squats.
https://www.hss.edu/health-library/move-better/back-pain-after-squats One Peloton. (n.d.). Lower back pain after squats.
https://www.onepeloton.com/blog/lower-back-pain-after-squats National Center for Biotechnology Information. (2022). Core stabilization exercise and low back pain.
https://pmc.ncbi.nlm.nih.gov/articles/PMC9340836/ Dr. Mauger. (n.d.). A combined approach to back pain treatment.
https://www.drmauger.com/blog/posts/a-combined-approach-to-back-pain-treatment Harvard Health Publishing. (2011). Strengthening your core the right way.
https://www.health.harvard.edu/blog/strengthening-your-core-right-and-wrong-ways-to-do-lunges-squats-and-planks-201106292810 Jimenez, A. (n.d.). Clinical insights on integrative musculoskeletal care.
https://dralexjimenez.com/
https://www.linkedin.com/in/dralexjimenez/ The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and to identify relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Martial arts offer discipline, strength, and confidence—but they also bring a real risk of head injuries. Even when a fighter doesn’t get knocked out, repeated blows to the head can quietly damage the brain and nerves over time. That hidden damage can show up years later as memory problems, mood changes, or even degenerative brain disease like chronic traumatic encephalopathy (CTE).PMC+1 At the same time, recovery is not hopeless. Integrative chiropractic care—especially when it combines spinal adjustments, neurological rehab, and functional medicine—may help fighters improve balance, reduce symptoms, and support the brain’s ability to rewire itself after injury.Synergy Chiropractic+1 This article explains, in clear language: -
What happens to a martial artist’s brain and nerves after head trauma -
Why sub-concussive hits still matter, even without a diagnosed concussion -
The short- and long-term symptoms to watch for -
How integrative chiropractic care can support healing and neuroplasticity Why Martial Artists Face Unique Brain and Nerve Risks Martial arts like boxing, kickboxing, Muay Thai, MMA, taekwondo, and karate often involve repeated strikes to the head. Even when rules and referees try to protect fighters, the basic goal is still to land powerful blows or submit an opponent. Studies on combat sports show: -
CTE was first recognized in boxers (“punch-drunk” syndrome) and has now been linked to other fighters, including mixed martial artists.PMC+1 -
In the Professional Fighters’ Brain Health Study, active professional fighters with more bouts and more head trauma had smaller brain volumes and slower processing speed.British Journal of Sports Medicine -
Research in MMA athletes shows that repeated mild traumatic brain injuries (mTBIs) and head impacts are tied to worse cognitive function over time.PMC+1 MMA and other striking arts combine punches, kicks, elbows, knees, and sometimes ground-and-pound. That means more angles and more chances for both big concussive blows and smaller, repeated hits that add up.e-Journal of Education+1 What Happens in the Brain During a Head Impact When a fighter takes a hard shot to the head, the brain rapidly moves and twists inside the skull. This can: -
Stretch and damage long nerve fibers (axons) -
Disrupt blood vessels and the blood–brain barrier -
Trigger chemical changes and inflammation Even blows that do not cause a full loss of consciousness can still cause microscopic tearing of nerve tissue and metabolic stress.PMC+1 After a knockout (KO) or technical knockout (TKO), the damage can be greater. Studies of KO events in combat sports show the brain experiences high rotational forces that can disturb nerve signaling and set the stage for long-term problems.PMC Over time, if these injuries keep happening, the brain may struggle to repair itself, especially if there is not enough rest between fights or sparring sessions. Sub-Concussive Blows: Hidden Damage Without a Classic Concussion Many martial artists worry about “big” concussions—but sub-concussive hits may be just as important. These are impacts that: -
Don’t cause obvious concussion symptoms -
Don’t lead to a fight being stopped -
Still transfer force to the brain Large studies in contact sports show that repeated head impacts, even without diagnosed concussions, are linked with brain changes and may increase the risk of CTE.Live Science+3CDC+3Boston University+3 For fighters, this means that years of hard sparring, drilling, and competition can: -
Slowly lower brain volume in key regions -
Alter white matter (the wiring that connects different brain areas) -
Reduce processing speed and reaction timeBritish Journal of Sports Medicine+1 The danger is that the damage is “silent” at first. A fighter may feel fine but be losing a little function year after year. Short-Term Symptoms After a Head Injury After a hard head shot or a series of blows, martial artists can experience symptoms right away or within hours to days. Common short-term signs of mild TBI or concussion include: -
Headache or pressure in the head -
Confusion or feeling “foggy” -
Dizziness or balance problems -
Blurred or double vision -
Nausea or vomiting -
Sensitivity to light or sound -
Trouble concentrating or remembering what happenedMayo Clinic+3NICHD+3Mayo Clinic+3 Sometimes, symptoms show up later, after training or once the adrenaline wears off. Even a fighter who “shakes it off” may still have an injury that needs rest and medical supervision. Long-Term Brain Changes: Cognitive Decline and CTE When head trauma continues over years, especially in professional fighters, the risk of long-term problems increases. Research shows: -
In professional fighters, more cumulative head trauma is linked to lower brain volumes and slower processing speed, even while they are still active.British Journal of Sports Medicine+1 -
Retired fighters may show brain shrinkage patterns similar to degenerative diseases like Alzheimer’s or CTE.Practical Neurology+1 -
MMA and boxing both carry risks, but at least one study reported that brain injury risk per event may be higher in MMA than in boxing, due to the way fights end and where strikes land.espn.com+1 CTE is a progressive condition linked with repeated head impacts. It is associated with abnormal tau protein buildup, nerve loss, and inflammation in the brain.Cleveland Clinic+2Mayo Clinic+2 Over time, CTE and other trauma-related brain changes can show up as: -
Memory loss -
Trouble with planning and decision-making -
Slowed thinking and reaction time -
Difficulty with attention and focus -
Parkinsonism-like symptoms in some athletesPMC+2ScienceDirect+2 Emotional, Behavioral, and Physical Symptoms That Worsen Over Time CTE and repeated brain trauma do not only affect thinking. They also impact how fighters feel and behave. Studies and reports of former combat athletes describe: -
Depression, anxiety, and mood swings -
Irritability, anger, or aggressive behavior -
Apathy or loss of motivation -
Impulsivity and poor judgment -
Sleep problems and chronic fatiguePMC+2Mayo Clinic+2 Many fighters also experience ongoing physical symptoms: This combination of emotional, cognitive, and physical changes can slowly erode quality of life—often while the person still looks “healthy” on the outside. Why Some Fighters Seem Fine—Until They Don’t One of the most troubling parts of trauma-related brain disease is how long it can stay hidden. Several factors play a role: -
Brain reserve: Some people have more cognitive reserve and can compensate longer before symptoms show. -
Culture of toughness: Fighters are used to ignoring pain and may under-report symptoms. -
Delayed onset: CTE symptoms may appear years or decades after a fighter retires.Mayo Clinic+1 -
Sub-concussive load: No single hit causes a dramatic change, but the total number of hits adds up.PMC+1 This is why a martial artist can compete for years with few obvious issues, then suddenly experience rapid decline in mood, memory, or behavior later in life. Because these changes are gradual, early screening and multidisciplinary care—neurology, neuropsychology, physical medicine, and chiropractic—are extremely important.Mayo Clinic Health System+2Synergy Chiropractic+2 Hidden Nerve Damage: What “Lower Brain Volume” Really Means When studies talk about lower brain volumes, they are describing measurable shrinkage in parts of the brain on MRI. In fighters, volume loss has been seen in areas responsible for: This shrinkage often reflects nerve-cell loss or damage to the supporting structures around those neurons. At the microscopic level, repeated trauma can cause: -
Axonal injury (damage to the long “wires” of nerve cells) -
Disconnection between brain regions -
Chronic inflammation and abnormal protein buildupScienceDirect+2PMC+2 Functionally, that hidden nerve damage may look like: -
Slower reaction time in sparring -
Trouble multitasking or remembering combinations -
Feeling “off” or uncoordinated, especially when tired -
Greater risk of injury because timing and balance are slightly off These changes are real, even when routine scans or quick exams look “normal.” Integrative Chiropractic Care: A Whole-Person Approach for Injured Fighters Integrative chiropractic care combines traditional chiropractic adjustments with neurological rehab, exercise therapy, and sometimes nutritional or functional medicine support. For martial artists with a history of head trauma, this type of care focuses on: -
Spinal alignment, especially the upper neck -
Nervous system regulation -
Balance, eye, and movement training -
Support for brain neuroplasticity and overall healingSynergy Chiropractic+2Mayo Clinic+2 Rather than replacing medical care, integrative chiropractic is usually part of a team approach that includes neurologists, primary care providers, and sometimes neuropsychologists and physical therapists.Mayo Clinic Health System+1 How Correcting Spinal Misalignment May Help the Brain The upper cervical spine (especially the atlas and axis—C1 and C2) sits right under the brainstem. If these vertebrae are misaligned after repeated whiplash, chokes, takedowns, or head kicks, they can affect: -
Blood flow through the vertebral arteries -
Cerebrospinal fluid (CSF) drainage -
Mechanical stress on the brainstem and cranial nervesSynergy Chiropractic Integrative chiropractors, including Dr. Alexander Jimenez in El Paso, use gentle, image-guided adjustments to: -
Restore normal joint motion and alignment -
Reduce abnormal tension around the brainstem and upper spinal cord -
Improve proprioceptive input from neck joints (the “position sense” that feeds the balance centers of the brain)Synergy Chiropractic+1 By improving neck mechanics and nerve signaling, adjustments may help reduce: This does not “cure” CTE or erase all damage, but it may relieve mechanical stress and improve the way the nervous system functions day to day.Synergy Chiropractic Balance, Eye, and Movement Training to Support Neuroplasticity Many fighters with head injuries report: -
Feeling unsteady on their feet -
Trouble tracking moving targets -
Motion sensitivity or feeling “spaced out” in crowds or bright gyms These issues often come from dysfunction in the vestibular system, eye movement control, and cervical proprioception.Mayo Clinic+2BrainFacts+2 Integrative chiropractic care often includes: -
Vestibular rehab: Head and eye movement drills to recalibrate balance systems -
Oculomotor exercises: Smooth-pursuit and saccade training to improve eye tracking -
Proprioceptive work: Controlled neck and body movements to retrain how joints send information to the brain -
Gait and posture work: Training to normalize walking patterns and stance Research suggests that repeated, targeted movement sends sensory input to the cerebellum and cortex, stimulating neuroplasticity—the brain’s ability to adapt and build new connections after injury.Synergy Chiropractic+1 Dr. Jimenez’s clinical model emphasizes movement-based therapy, spinal decompression, flexion–distraction, and soft-tissue treatment (such as Graston or Gua Sha) to reduce pain and improve spinal mechanics, which in turn supports more normal neural signaling.Synergy Chiropractic+1 Supporting the Whole Fighter: Functional and Integrative Care Brain and nerve health are not only about joints and muscles. Integrative chiropractic clinics, like those led by Dr. Jimenez, often combine:El Paso, TX Doctor Of Chiropractic+1 -
Nutritional guidance to lower inflammation and support brain recovery (for example, omega-3 fats, colorful fruits and vegetables, and adequate protein) -
Sleep and stress support, since poor sleep can prolong post-concussion symptoms -
Strength and conditioning plans that avoid excessive head trauma while maintaining fitness -
Coordination with neurologists and imaging centers for advanced diagnostics (MRI, DTI, functional neuro testing, and biomarkers in some cases) This team-based integrative approach is especially important for martial artists who want to keep training safely, adjust their style if needed, and protect long-term brain health.Synergy Chiropractic+1 Practical Steps for Martial Artists After a Head Injury If you are a martial artist or coach, consider these practical steps: -
Take every head impact seriously.
If there is confusion, memory loss, vomiting, severe headache, or difficulty standing, treat it as an emergency and seek urgent care.Mayo Clinic+1 -
Do not return to sparring or competition too soon.
Guidelines strongly advise against going back into a fight or hard practice the same day after a suspected concussion.Mayo Clinic+1 -
Get a full evaluation.
This may include: -
Consider integrative chiropractic and rehab.
A clinician experienced in TBI and combat sports—such as Dr. Jimenez and his team—can assess neck alignment, movement patterns, and nervous system function and build a customized rehab plan.Synergy Chiropractic+2Synergy Chiropractic+2 -
Monitor for delayed symptoms.
Watch for changes in mood, memory, sleep, or behavior in the weeks and months after an injury. Early support is better than waiting until symptoms become severe.CDC+2Mayo Clinic+2 When to Seek Emergency Care Call emergency services or go to the ER right away after a head injury if you notice: -
Worsening or severe headache -
Repeated vomiting -
Seizures -
Unequal pupils -
Weakness or numbness in arms or legs -
Slurred speech, confusion, or behavior that is very unusual -
Trouble waking up or loss of consciousnessBrainFacts+2Mayo Clinic+2 Chiropractic and rehab care are not substitutes for emergency evaluation. They are part of recovery after life-threatening problems have been ruled out and the person is medically stable. Conclusion: Protecting the Brain While Protecting the Passion for Martial Arts Martial arts will always involve risk. But understanding how head trauma affects the brain and nerves helps fighters make smarter choices about training volume, protective gear, and recovery. The evidence is clear: Integrative chiropractic care—like the approach used by Dr. Alexander Jimenez, DC, APRN, FNP-BC—works to: -
Realign the spine, especially the upper cervical region -
Improve brain–body communication -
Enhance balance, eye movements, and coordination -
Stimulate neuroplasticity through targeted movement and rehabilitation -
Support overall recovery with nutrition, lifestyle, and collaborative medical careSynergy Chiropractic+2Synergy Chiropractic+2 For martial artists, the goal is not just to fight well today, but to think clearly, move confidently, and live fully decades from now. Protecting the brain—and partnering with an integrative, neuroscience-informed chiropractor when injuries happen—can help make that possible. B.C. Martial Artists Creating Awareness About Concussion References Bernick, C., Banks, S. J., & others. (2013). What boxing tells us about repetitive head trauma and the brain. Cleveland Clinic Journal of Medicine, 80(3), 185–190. PMC Bernick, C., Zetterberg, H., & others. (2015). The Professional Fighters’ Brain Health Study: Cognitive function, brain structure and exposure to repetitive head trauma. British Journal of Sports Medicine, 49(15), 1007–1011. British Journal of Sports Medicine Centers for Disease Control and Prevention. (2024). About repeated head impacts. CDC Cleveland Clinic. (n.d.). Effects in football and professional combat sports: Repetitive head trauma and brain health. Cleveland Clinic Lim, L. J. H., Ho, C. S. H., & Ho, R. C. M. (2019). Dangers of mixed martial arts in the development of chronic traumatic encephalopathy. International Journal of Environmental Research and Public Health, 16(2), 254. PMC Mańka-Malara, K., & others. (2022). Head trauma exposure in mixed martial arts: A narrative review. Journal of Clinical Medicine, 11(21), 6293. PMC Mayo Clinic. (2024). Concussion – Symptoms and causes. Mayo Clinic Mayo Clinic. (2025). Chronic traumatic encephalopathy – Symptoms and causes. Mayo Clinic National Institute of Neurological Disorders and Stroke. (2025). Traumatic brain injury (TBI). NINDS National Institute of Child Health and Human Development. (2020). What are common symptoms of traumatic brain injury (TBI)?. NICHD Reis, H. (2020). Chiropractic and traumatic brain injuries: Consider all your holistic options. Stern, R. A., & others. (2011). Long-term consequences of repetitive brain trauma. PM&R, 3(10 Suppl 2), S460–S467. ScienceDirect U.S. Centers for Disease Control and Prevention. (2025). Symptoms of mild TBI and concussion. CDC Verywell Health. (2024). How long do concussion symptoms last? Key signs to watch for. Verywell Health World Federation of Neurology / BrainFacts.org. (n.d.). Traumatic brain injury. BrainFacts Dr. Alexander Jimenez and Integrative Chiropractic Sources El Paso Chiropractic / Synergy Chiropractic. (n.d.). Traumatic brain injury: Integrated chiropractic–neurological recovery. Synergy Chiropractic Jimenez, A. (n.d.). Sports head injuries: Chiropractic’s role (articles section). El Paso, TX Doctor Of Chiropractic Turnersville Chiropractic. (n.d.). Consider chiropractic care for mixed martial arts injuries. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and to identify relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Explore the benefits of body strengthening combined with Pilates for improving strength and flexibility in your daily routine. Introduction Hello, health warriors! Think of your body as a busy city where inflammation shows up like an unexpected traffic jam. It’s important for signaling trouble, but it can be a real pain when it gets in the way. Now, picture Pilates, the graceful exercise system that came from a dancer’s dream, swooping in like a city planner to clean up the mess and keep things running smoothly. With some body-strengthening exercises and chiropractic care, you have a powerful trio that can help you with musculoskeletal problems and get you on the road to better health. In this long guide, we’ll talk about how Pilates and strength training can help with inflammation, stress from the environment, and working with chiropractic professionals to get you moving without pain. We’ll include some exercises that can be done at home or at the gym, add some humor for fun, and get some advice from Dr. Alexander Jimenez, DC, APRN, FNP-BC, a top doctor in El Paso. This is your guide to feeling great, whether you’re trying to avoid back pain or recover from an injury. You don’t need a gym membership, but it helps! We’ll keep it simple and full of useful tips and facts backed by science. If you’re stuck because of inflammation, Pilates and chiropractic care might be the way to get out. Let’s go! What Is Inflammation and Why Does It Matter? Let’s start with the basics. Inflammation is like a fire truck racing to a fire; it’s your body’s built-in alarm system. When you twist your ankle or get a cold, your immune system sends white blood cells, chemicals, and fluids to the area, which can make it red, swollen, hot, or painful (Cleveland Clinic, n.d.). This is a heroic move in a healthy body: it traps germs, clears away damaged tissue, and starts the healing process while keeping everything in balance, a state known as homeostasis (Yale Medicine, 2020). Think about this: You hurt yourself lifting groceries. Inflammation sends blood to the area, which brings oxygen and nutrients to help heal the damage. If you don’t get it, that strain might never heal, and you could end up walking like a pirate with a peg leg. It also controls your immune system, which helps you fight off germs every day. It also helps your muscles heal after a workout, which is your body’s way of saying, “Let’s rebuild stronger!” (Vanderbilt Medicine, 2015). But when inflammation sticks around too long, it can lead to serious problems like arthritis, heart disease, or chronic pain (Yale Medicine, 2022). So, inflammation is like a bouncer for your body. It keeps troublemakers out, but if it starts a fight, it’s a problem. Funny question: Why does inflammation make you swell? Your body is throwing a “block the baddies” party with balloons, but someone needs to pop them before it gets too crazy! References Acute vs. Chronic Inflammation: What’s the Difference? Let’s break the scene down into two parts: acute and chronic inflammation. Acute inflammation is the quick responder, like a superhero coming in for a short mission that lasts hours or days before leaving (Harvard Health, 2020). Think of a stubbed toe: it hurts, turns red, and then goes back to normal. It’s how your body sends blood and immune cells quickly to help you heal faster. Chronic inflammation, on the other hand, is the bad guy that sticks around for months or years and can hurt tissues (Cleveland Clinic, n.d.). Autoimmune problems, long-lasting irritants, or unresolved acute injuries can all make conditions like chronic back pain or joint stiffness worse (NCBI, 2023). The main differences are that acute conditions are short, sweet, and healing, while chronic conditions are long, draining, and bothersome. Acute improves repair by increasing blood flow and cleaning up (Physiopedia, n.d.). Chronic conditions drain energy, lead to persistent pain, and increase the risk of illness (Encompass Health, 2021). Warning: Laughter Acute inflammation is like a quick cameo in an action movie; it only lasts for one scene. Long-term? It’s the sequel that no one wanted, and it drags on with no plot twists! Knowing this helps you customize your recovery: use ice for sudden flare-ups and holistic methods like Pilates for long-term problems. References Environmental Factors Fueling Inflammation and Musculoskeletal Issues Your surroundings aren’t just the background; they play a big role in inflammation and problems with your bones and muscles. Pollution, diet, stress, and even your daily routine can all make you feel hotter (Nature Medicine, 2019). Air pollution introduces harmful chemicals into your lungs, which can cause oxidative stress and inflammation, potentially making your muscles tight or your joints hurt (The University of Queensland, n.d.). It’s like your body is fighting a smoggy enemy. Diet is a big deal: Processed foods, sugars, and unhealthy fats can worsen inflammation, which can make your back stiff or exacerbate sciatica. Foods high in antioxidants, like berries or greens, can help calm it down (PMC, 2019). Pesticides and heavy metals can harm gut health, leading to systemic inflammation that puts stress on musculoskeletal tissues (ScienceDirect, 2013). Stress raises cortisol levels, which not only worsens inflammation but can also intensify neck or back pain by making muscles tense (Northwestern University, 2017). Other causes of chronic pain include smoking, which irritates tissues; being overweight, which puts pressure on joints and sends inflammatory signals; and bad posture from desk jobs or repetitive tasks, which strains your spine (PMC, 2019). Poor nutrition and other things that happen early in life can even lead to musculoskeletal problems in adults (Northwestern University, 2017). In conditions like fibromyalgia, things in the environment can make pain and inflammation worse (CGH Journal, 2024). Sitting at a desk all day? Ha ha! Your spine is begging you to take a break from that office chair that makes your back hurt! To fight these, make smart choices like eating better, finding ways to relax, or doing Pilates or other movement-based exercises. More on that next. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
As people age or face health challenges that limit movement, staying active becomes both more important and more difficult. For seniors or individuals with limited abilities, exercise is not just about fitness—it is about preserving independence, reducing pain, and preventing falls. In integrative chiropractic settings, where spinal health is supported with adjustments, soft-tissue care, and therapeutic modalities, exercise takes on an even more important role. Chiropractors often prescribe adaptive movements that are low-impact, safe, and tailored to each person’s needs. Dr. Alexander Jimenez, DC, APRN, FNP-BC, a dual-scope chiropractor and nurse practitioner in El Paso, emphasizes that targeted exercise is essential for older adults. His clinic integrates chiropractic adjustments with exercise therapy, massage, acupuncture, and advanced neuromusculoskeletal imaging to create personalized plans for patients recovering from injuries, chronic pain, or motor vehicle accidents (MVAs). According to Dr. Jimenez, “Movement is medicine. When exercise supports adjustments, the body not only heals but adapts to prevent further damage.” This article explores the best low-impact exercises for seniors and those with mobility limitations in integrative chiropractic care. Each section will highlight safe movements, clinical insights, and practical strategies to maintain flexibility, balance, and strength. Why Exercise Matters for Seniors With Limited Abilities Preventing Decline in Mobility Without regular movement, muscles weaken, joints stiffen, and balance declines, making daily tasks more difficult. Seniors with limited abilities may already face reduced mobility from arthritis, injuries, or neurological conditions, and inactivity can speed up functional decline (Comfort Keepers, n.d.). Supporting Chiropractic Adjustments Exercise complements chiropractic care by strengthening the muscles around the spine, improving circulation, and maintaining alignment. This reduces the risk of tension, pain flare-ups, and misalignments between appointments (Erie Chiropractic, n.d.). Reducing Fall Risks Falls are one of the leading causes of injury in older adults. Balance exercises and gentle strength training can significantly reduce this risk by improving coordination and stabilizing joints (McCarthy & Stone, n.d.). Dr. Jimenez often sees seniors who have fallen or been in car accidents in his El Paso clinic. Using advanced imaging, he diagnoses hidden joint instability or ligament damage and creates dual treatment plans that include chiropractic adjustments to restore alignment and guided exercises to restore balance and coordination. The Role of Chiropractors in Adaptive Exercise Chiropractors are uniquely positioned to design exercise programs that respect the patient’s limitations while still challenging the body safely. According to Rush Chiropractic (n.d.), these programs often include: -
Range-of-motion stretches to maintain flexibility. -
Core strengthening to support the spine. -
Balance drills to prevent falls. -
Modified strength training to preserve muscle mass without strain. Dr. Jimenez highlights that chiropractors can bridge both the medical and rehabilitative aspects of care. For example, in MVA cases, he not only documents injuries for legal purposes but also prescribes exercise therapy that complements chiropractic adjustments, reducing inflammation and promoting natural healing. Best Low-Impact and Adaptive Exercises 1. Chair Exercises For seniors who struggle with standing, chair exercises are safe and accessible. These include seated marches, arm raises, and gentle torso twists. They build muscle endurance while preventing dizziness or falls (Comfort Keepers, n.d.). 2. Cat-Cow Stretch This yoga-inspired movement improves spinal flexibility and relieves tension. Performed slowly, it aligns well with chiropractic adjustments, keeping the spine mobile and pain-free (Elevate to Life, n.d.). 3. Heel-to-Toe Walking A simple but effective balance drill, heel-to-toe walking, strengthens stabilizer muscles and improves gait. Chiropractors often recommend it for fall prevention (Village Green Retirement, n.d.). 4. Water Aerobics Exercising in water reduces joint stress while allowing a greater range of motion. Aquatic therapy is excellent for those with arthritis, hip pain, or post-surgical recovery (Live2BHealthy, n.d.). 5. Gentle Strength Training Chair squats, resistance bands, or light hand weights help maintain muscle mass and bone density. Chiropractors may adapt these exercises to prevent overloading joints (Peregrine Crossgate, n.d.). 6. Balance and Stability Drills Standing leg lifts, supported side steps, or one-leg holds near a wall improve coordination. These movements are critical for seniors who fear losing stability at home (McCarthy & Stone, n.d.). 7. Core Stability Work Bridges, modified planks, and seated abdominal contractions build spinal support. Core strength helps keep adjustments effective for longer and reduces the risk of misalignment (Best Grand Rapids Chiropractor, n.d.). Dr. Jimenez stresses that “simple movements performed consistently are more powerful than advanced routines abandoned after two weeks.” His clinic tailors each exercise to match injury recovery timelines, ensuring patients progress safely. Clinical Applications in Injury and Recovery Motor Vehicle Accidents (MVAs) After car accidents, seniors may face whiplash, spinal misalignment, or nerve injuries. Dr. Jimenez uses imaging tools to pinpoint damage and then prescribes gentle stretches and strengthening exercises that protect healing tissues while restoring function. Work and Sports Injuries Older adults working in physically demanding jobs or participating in sports often suffer from sprains or joint strains. Chiropractic adjustments combined with adaptive exercise help restore the full range of motion and reduce reinjury risks. Chronic Pain and Arthritis For patients with arthritis or degenerative joint disease, low-impact exercise reduces stiffness, enhances circulation, and promotes natural anti-inflammatory effects (Atlas Senior Living, 2024). Legal and Medical Documentation In El Paso, Dr. Jimenez’s clinic also plays a role in personal injury cases. Detailed treatment records, including prescribed exercises, support patients’ legal claims and document recovery progress, ensuring care is both medical and protective of patient rights. Integrative Care: Beyond Exercise While exercise is central, integrative chiropractic care also includes: -
Massage therapy to reduce muscle tension. -
Acupuncture for pain relief and circulation. -
Nutritional counseling to support joint health and reduce inflammation. -
Lifestyle coaching to encourage safe habits and fall prevention. Dr. Jimenez explains that combining these approaches with tailored exercise ensures patients receive “a full-spectrum path to healing, not just symptom management.” Practical Tips for Seniors Starting an Exercise Program -
Begin slowly—even 5 minutes a day can create benefits. -
Use support tools such as chairs, railings, or water for balance. -
Prioritize consistency over intensity. -
Stay hydrated and rest as needed. -
Consult with a chiropractor to create a safe and personalized plan. Conclusion Low-impact, adaptive exercises are a cornerstone of integrative chiropractic care for seniors and those with limited abilities. These movements enhance spinal health, improve balance, and reduce pain, making daily life safer and more fulfilling. With the guidance of experts like Dr. Alexander Jimenez, exercise becomes more than physical activity—it becomes a form of preventive medicine, injury rehabilitation, and empowerment. In El Paso and beyond, chiropractors integrating exercise, imaging, and holistic therapies are reshaping how older adults maintain mobility and independence. Movement, when guided and supported, allows seniors not just to live longer but to live better. How Chiropractic Helped Me Recover References General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Athletes, whether professionals or weekend enthusiasts, rely on more than physical training to achieve peak performance. Nutrition, recovery, and body alignment all play vital roles. A chiropractic and integrative sports diet focuses on nutrient-dense, whole foods to reduce inflammation, accelerate healing, and support both short-term performance and long-term health. Unlike generic sports nutrition plans, this approach is highly individualized. It examines the root causes of fatigue, injury, or poor recovery, rather than just treating symptoms. El Paso nurse practitioner and chiropractor Dr. Alexander Jimenez, DC, APRN, FNP-BC, applies this dual-scope strategy in his clinical practice. By combining chiropractic care, advanced imaging, functional medicine, and nutrition, he addresses musculoskeletal issues at their source. His integrative care model is not just about faster return to play—it’s about preventing long-term damage while enhancing strength, resilience, and mental focus【chiropractorinoviedo.com†source】. Why Athletes Need an Integrative Approach Traditional sports diets often emphasize carbohydrates and protein, but may overlook the importance of nutrient density and inflammation control. Intense training and competition lead to microscopic muscle damage, oxidative stress, and immune strain. Without proper nutrition and musculoskeletal care, these small injuries accumulate, increasing the risk of chronic pain and decreased performance【evolvedhealthchiropractic.com†source】. An integrative chiropractic nutrition plan helps athletes: -
Reduce inflammation by incorporating anti-inflammatory foods, such as omega-3 fatty acids, leafy greens, and berries. -
Repair tissues by optimizing protein intake and balancing amino acids. -
Improve joint function through micronutrients like magnesium, vitamin D, and collagen-supporting foods. -
Support energy metabolism with complex carbohydrates and phytonutrients. This holistic care model ensures athletes not only recover but also improve their body’s resilience against repetitive strain【redeeminglifenutrition.com†source】. Nutrient-Dense Foods for Inflammation Control Inflammation is the body’s natural response to stress and injury, but chronic inflammation delays healing and increases pain. Integrative chiropractic sports diets prioritize anti-inflammatory foods: -
Fatty fish (salmon, sardines, tuna) provide omega-3 fatty acids that decrease inflammatory markers. -
Leafy greens and cruciferous vegetables (spinach, kale, broccoli) support detoxification and joint health. -
Berries, cherries, and citrus fruits deliver antioxidants that reduce oxidative stress. -
Nuts, seeds, and olive oil support heart and musculoskeletal health. Dr. Jimenez often explains that inflammation after injuries, especially those resulting from motor vehicle accidents or repetitive sports strains, can linger long after the initial pain has faded. Correcting diet is as essential as chiropractic adjustments or physical therapy in reducing long-term joint stress【bbcgoodfood.com†source】【atlanticchirofl.com†source】. The Role of Protein in Recovery Protein is critical for muscle repair, joint stabilization, and tissue regeneration. Athletes undergoing intense training or recovering from injury require a consistent intake of protein throughout the day. Key protein sources include: -
Lean meats like chicken and turkey. -
Plant proteins such as lentils, tofu, and quinoa. -
Low-fat dairy products, such as Greek yogurt and cottage cheese. -
Protein-rich snacks such as nuts and seeds. Research shows that balanced protein intake helps reduce soreness, supports collagen synthesis, and accelerates muscle recovery【revistanutricion.org†source】【childrensmercy.org†source】. In his El Paso clinic, Dr. Jimenez has observed that patients with ligament or tendon injuries heal faster when combining protein-rich diets with chiropractic care, massage therapy, and rehabilitative exercise. This dual-scope strategy reduces scar tissue buildup and improves the range of motion. Carbohydrates and Energy for Peak Performance Carbohydrates are not the enemy—they’re essential for fueling muscles during high-intensity activity. The focus should be on complex carbohydrates that release energy steadily. Recommended sources include: -
Whole grains (quinoa, oats, brown rice). -
Vegetables and legumes for fiber and micronutrients. -
Fruit for quick recovery glycogen replenishment. Balanced carbohydrate intake prevents energy crashes and reduces the risk of overtraining injuries【betterhealth.vic.gov.au†source】【stanford.edu†source】. Healthy Fats for Hormone and Joint Support Healthy fats support hormone balance, reduce inflammation, and cushion joints. Athletes who cut too much fat from their diet risk delayed healing and hormone imbalance. Beneficial sources include: -
Avocados and olives. -
Fatty fish (salmon, sardines, mackerel). -
Nuts and seeds (chia, flax, walnuts). Studies show athletes who follow a Mediterranean-style diet rich in healthy fats recover faster and experience fewer musculoskeletal injuries【nuffieldhealth.com†source】【longevity.stanford.edu†source】. Micronutrients for Strength and Stability While macronutrients get most of the attention, micronutrients are equally important: -
Vitamin D and calcium: support bone density. -
Magnesium: supports muscle relaxation and nerve conduction. -
Vitamin C and zinc: aid tissue repair. Chiropractic care identifies when joint or bone weakness contributes to injury. Integrative nutrition ensures athletes rebuild these systems with the right vitamins and minerals【parcofontario.com†source】【cityviewchiropractor.com†source】. Chiropractic Nutrition and Injury Recovery Athletes recovering from injuries—whether from work, sports, or motor vehicle accidents—need specialized care. Chiropractic adjustments restore spinal alignment, which improves circulation and nutrient absorption. At the same time, integrative nutrition reduces inflammation and accelerates tissue repair【sportsrd.org†source】【essendonsportsmedicine.com.au†source】. Dr. Jimenez frequently combines: -
Advanced imaging (X-rays, MRIs, DMX studies) to assess tissue and joint damage. -
Targeted exercise therapy to restore mobility. -
Massage and acupuncture to improve circulation and reduce scar tissue. -
Nutritional counseling to optimize healing from the inside out. This dual-scope approach ensures patients recover not just structurally but metabolically. Legal and Clinical Integration in Personal Injury Cases In El Paso, Dr. Jimenez works with patients who suffer from motor vehicle and workplace injuries. Beyond medical treatment, he provides legal documentation critical for personal injury claims. This includes: -
Detailed medical records. -
Imaging reports. -
Chiropractic assessments. -
Nutrition and lifestyle recommendations that support recovery timelines. This integration of medical and legal care allows patients to navigate lawsuits with objective evidence of their injuries and recovery progress. For patients, this means their care is both comprehensive and defensible in court【dralexjimenez.com†source】. Holistic Therapies in Integrative Care Chiropractic care goes beyond spinal adjustments. Dr. Jimenez integrates multiple therapies for neuromusculoskeletal issues: -
Massage therapy: reduces tension and improves circulation. -
Acupuncture: balances energy flow and reduces inflammation. -
Rehabilitative exercise: builds strength and prevents re-injury. -
Nutritional therapy: ensures adequate fueling for tissue regeneration. This integrative model helps patients recover faster, perform better, and prevent long-term complications【americansportandfitness.com†source】【holisticwholenessinstitute.com†source】. Conclusion A chiropractic and integrative sports diet is more than a meal plan—it’s a philosophy of care that connects nutrition, spinal alignment, recovery, and performance. Athletes who adopt this approach benefit from reduced inflammation, faster recovery, and improved long-term health and wellness. Dr. Alexander Jimenez’s dual role as chiropractor and nurse practitioner highlights the strength of integrated medicine. By treating underlying causes rather than symptoms, his patients achieve better recovery outcomes, enhanced performance, and protection from chronic injuries. This whole-body, individualized strategy demonstrates that optimal health is not built on a single therapy alone, but rather through the integration of nutrition, chiropractic care, and holistic healing. Spondylolysis: The Hidden Challenge for Athletes | El Paso, TX References General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction: The Silent Toll on Passengers When a motor vehicle accident (MVA) happens, most people think of the driver first. But passengers are just as likely—if not more likely—to suffer serious injuries. Sitting in the front or back seat doesn’t guarantee safety. Whether the crash is minor or severe, passengers can suffer injuries that require immediate care, ongoing treatment, and long-term support. These injuries range from minor bruises and whiplash to traumatic brain injuries, broken bones, and even psychological conditions like post-traumatic stress disorder (PTSD)【Lowman Law Firm, n.d.】. Dr. Alexander Jimenez, a dual-licensed chiropractor and nurse practitioner in El Paso, has seen the full range of passenger injuries in his clinical practice. His dual-scope expertise allows him to assess, diagnose, and treat both the physical and legal aspects of injury recovery, using advanced imaging and comprehensive integrative protocols that support long-term health. “Passengers often suffer injuries without fully realizing the extent until days or even weeks later,” explains Dr. Jimenez. “That’s why early diagnostic imaging, clinical correlation, and integrated treatment are essential for recovery.” Whiplash: A Common and Painful Injury Whiplash is one of the most common injuries passengers suffer, especially in rear-end collisions. It happens when the neck jerks suddenly forward and backward, stretching and damaging the muscles, ligaments, and tendons in the cervical spine【Kirshenbaum, n.d.】. Symptoms might include neck pain, stiffness, headaches, dizziness, or even difficulty concentrating【Pi Attorney Law Firm, n.d.】. A ccording to Dr. Jimenez, “Whiplash injuries are often underestimated. With digital motion X-rays, we can detect soft tissue injuries and vertebral misalignment that aren’t visible on standard films. Early intervention reduces the risk of chronic pain and permanent damage.” Chiropractic care is particularly helpful for whiplash. Gentle spinal adjustments, manual therapies, and posture correction help reduce inflammation and restore mobility without medication or surgery. 🔗 Kirshenbaum
🔗 Pi Attorney Law Firm Neck and Back Injuries: Invisible but Dangerous Neck and back injuries go beyond whiplash. Herniated discs, strained muscles, spinal misalignment, and nerve impingement are all possible outcomes of sudden impact. Passengers may feel pain that radiates down their arms or legs, experience numbness, or find it hard to move【Lowman Law Firm, n.d.】. Dr. Jimenez uses advanced diagnostic tools—such as MRIs and motion studies—to locate the source of these symptoms. As a chiropractor and nurse practitioner, he can design customized care plans that combine chiropractic adjustments with therapeutic exercises, regenerative therapies, and medical referrals when needed. 🔗 Lowman Law Firm Brain and Head Injuries: Concussions and Beyond A concussion can occur even without hitting your head. The brain moves rapidly inside the skull during a crash, causing trauma. Symptoms can include confusion, headaches, memory loss, mood changes, and fatigue. In more serious cases, traumatic brain injury (TBI) may result, requiring long-term care【NCBI, 2023】. “Concussions are tricky,” Dr. Jimenez explains. “They don’t always show up on scans. That’s why we combine neurological exams, balance testing, and cognitive assessments to catch signs early.” Early diagnosis is key to preventing long-term complications like chronic headaches, mood disorders, or neuroinflammation. 🔗 NCBI Facial Injuries and Airbag-Related Trauma Airbags are lifesaving but powerful. If a passenger is seated too close or not wearing a seatbelt properly, airbag deployment can cause facial fractures, eye injuries, burns, or even chest trauma【Lawyers 24-7, n.d.】. The force of the airbag can also cause abrasions to the arms, hands, or upper body【Traub Law, n.d.】. Dr. Jimenez emphasizes safety education: “Understanding how to position the seat and wear the seatbelt properly can reduce these types of injuries. Clinically, we also look at soft tissue damage from airbag deployment, which often goes unnoticed but can cause chronic pain.” 🔗 Lawyers 24-7
🔗 Traub Law Broken Bones and Fractures Broken bones and fractures are common in passengers—especially the ribs, collarbone, arms, legs, and pelvis. These injuries may occur from the seatbelt, airbag, dashboard, or being thrown around in the car during the crash【Rands Injury Law, n.d.】. While many fractures heal with immobilization, some require surgery and months of rehab. Dr. Jimenez points out that chiropractic care helps manage pain during healing and speeds up recovery by promoting circulation and reducing muscle guarding. He also provides medical documentation required for insurance or legal claims. 🔗 Rands Injury Law Soft Tissue Injuries: Hidden but Harmful Passengers often suffer muscle strains, tendon sprains, or ligament injuries. These soft tissue injuries don’t show up on X-rays but can cause significant pain, swelling, and limited mobility【Miller Weisbrod, n.d.】. Without treatment, soft tissue damage can lead to chronic pain syndromes. Dr. Jimenez relies on orthopedic testing and motion palpation to identify the exact location of the injury. His dual-scope care model uses both chiropractic and rehabilitative techniques—like myofascial release, cold laser therapy, and medical-grade bracing—to accelerate healing. 🔗 Miller Weisbrod Internal Injuries: Life-Threatening but Delayed Internal injuries like organ damage, internal bleeding, or abdominal trauma may not show symptoms right away. Seatbelt trauma, blunt force impact, or even airbag deployment can damage the liver, kidneys, or intestines【Attorney Guss, n.d.】. These injuries can be fatal if not diagnosed and treated quickly. “Internal injuries require immediate imaging and emergency care,” warns Dr. Jimenez. “As a nurse practitioner, I can refer patients for CT scans and coordinate with surgeons if necessary. It’s part of our integrated approach to safety.” 🔗 Attorney Guss Psychological Injuries: The Silent Wounds Being a passenger in a car crash can be emotionally traumatic. Many people experience anxiety, depression, or PTSD. These symptoms can disrupt sleep, cause panic attacks, or lead to avoidance of driving altogether【Lowman Law Firm, n.d.】. Dr. Jimenez uses trauma-informed care to support emotional health after an MVA. He also partners with mental health providers when necessary. Integrative medicine techniques like breathing therapy, guided visualization, and functional nutrition can help balance the nervous system and support mental recovery. 🔗 Lowman Law Firm Passengers vs. Drivers: Who Is at Greater Risk? According to several studies, passengers are often more seriously injured than drivers—especially in side collisions or if seated in the rear without proper restraints【Poisson Law, n.d.】【Joye Law Firm, n.d.】. Rear-seat passengers are less protected by airbags and may not always wear seatbelts. Dr. Jimenez uses this data to help educate patients, insurance adjusters, and attorneys. His clinical reports include detailed assessments of seating position, biomechanics, and injury probability, assisting patients to receive proper compensation and care. 🔗 Poisson Law
🔗 Joye Law Firm How Dr. Alexander Jimenez Supports Passenger Injury Recovery Dr. Alexander Jimenez is a unique provider because he’s both a licensed chiropractor and a certified nurse practitioner. This dual scope allows him to manage not only spinal and musculoskeletal injuries but also internal, neurological, and psychological conditions. His clinic in El Paso specializes in: -
Advanced diagnostics like digital motion imaging, MRIs, and functional neurological exams -
Comprehensive treatment including chiropractic adjustments, rehab exercises, soft tissue therapies, and nutritional support -
Legal-medical integration, offering clear documentation for attorneys and insurers -
Holistic recovery protocols to prevent long-term complications His clinical insights are available through platforms like Dr. Jimenez’s Website, LinkedIn, Instagram, and Facebook, where he regularly educates the public about injury recovery, functional medicine, and personal injury law. “It’s not just about fixing the body,” Dr. Jimenez states. “It’s about restoring function, confidence, and control over your life after trauma.” Conclusion: Recovery Requires the Right Team Passenger injuries after a motor vehicle accident can range from soft tissue strains to life-threatening conditions. They often involve hidden complications—like emotional trauma or delayed symptoms—that require expert evaluation. Dr. Alexander Jimenez’s dual expertise allows him to support both medical and legal recovery. Through chiropractic care, integrative medicine, and comprehensive diagnostics, he helps passengers heal naturally and completely. Knee Pain Rehabilitation (Chiropractic Care) | El Paso, Tx References Attorney Guss. (n.d.). How much money can a passenger in a car accident get? https://attorneyguss.com/blog/how-much-money-can-a-passenger-in-a-car-accident-get/#:~:text=Abdominal%20Injuries Dean Waite & Associates, LLC. (n.d.). Airbag injuries: Risks every driver should know. https://www.deanwaite.com/articles/airbag-injuries-risks-every-driver-should-know#:~:text=Common%20airbag%20injuries Joye Law Firm. (n.d.). Are passengers or drivers more likely to be injured in car crashes? https://www.joyelawfirm.com/blog/south-carolina-car-accident-lawyer-passengers-or-drivers-more-likely-injured-in-crashes/ Kirshenbaum & Kirshenbaum. (n.d.). Common injuries from car accidents. https://www.kirshenbaumri.com/library/injuries-from-car-accidents.cfm#:~:text=Whiplash%20can%20occur Lawyers24-7.com. (n.d.). Airbag injuries: What NY passengers need to know. https://www.lawyers24-7.com/airbag-injuries-what-ny-passengers-need-to-know/#:~:text=The%20forceful%20deployment%20of%20an%20airbag Lowman Law Firm. (n.d.). The most common passenger injuries sustained in a car crash. https://www.lowmanlawfirm.com/blog/the-most-common-passenger-injuries-sustained-in-a-car-crash#:~:text=Neck%20and%20Back%20Injuries Miller Weisbrod Olesky LLP. (n.d.). Passenger injuries in car accidents. https://www.millerweisbrod.com/passenger-injuries-in-car-accidents#:~:text=One%20common%20type%20of%20injury National Center for Biotechnology Information. (2023). Concussion. In StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK441955/ Pi Attorney Law Firm. (n.d.). Rear-end collisions. https://www.piattorneylawfirm.com/practice-areas/car-accident/rear-end-collisions#:~:text=Whiplash%20is%20a%20common%20injury Plaza Injury Law. (2023, July). Understanding car accident injuries. https://plazainjurylaw.com/2023/07/understanding-car-accident-injuries/#:~:text=Airbag%20Injuries Poisson, Poisson & Bower, PLLC. (n.d.). Passengers vs. drivers in crash injuries. https://poissonlaw.com/blog/passengers-vs-drivers-in-crash-injuries/#:~:text=Factors%20Affecting%20Passenger%20Injury%20Rates Rands Injury Law. (n.d.). Common passenger injuries in car accidents. https://www.randsinjurylaw.com/common-passenger-injuries-in-car-accidents/#:~:text=Broken%20Bones%20and%20Fractures Traub Law. (n.d.). How serious does a motor vehicle accident have to be for airbags to deploy? https://www.traublaw.com/blogs/7767/how-serious-does-a-motor-vehicle-accident-have-to-be-for-airbags-to-be-deployed/#:~:text=Additionally%2C%20airbags%20can%20cause%20more%20serious%20injuries General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Find out how physical therapy can alleviate pain from auto injuries, focusing on whiplash recovery strategies and tips. Introduction Motor vehicle accidents (MVAs) are a major global health concern, contributing to millions of injuries annually. The World Health Organization notes that road traffic injuries are the eighth leading cause of death across all age groups, particularly affecting younger individuals (Global Road Safety). Among the injuries sustained, whiplash is one of the most prevalent, especially in rear-end collisions. This injury, caused by rapid neck movement, can lead to a range of symptoms that disrupt daily life. Physical therapy has emerged as a cornerstone of recovery, offering evidence-based solutions to manage pain and restore function. In El Paso, Texas, Dr. Alexander Jimenez, a board-certified chiropractor and nurse practitioner, is a prominent figure in treating injuries related to motor vehicle accidents (MVAs). His expertise in combining physical therapy, chiropractic care, and advanced diagnostics makes him a vital resource for personal injury victims. This article examines the clinical rationale for physical therapy following a motor vehicle accident (MVA), the role of whiplash, and Dr. Jimenez’s contributions to recovery and legal support. What is Whiplash? Whiplash, or cervical acceleration-deceleration (CAD) syndrome, is a neck injury resulting from sudden, forceful back-and-forth neck movement. First described in 1928 by Dr. Harold Crowe, it typically occurs in motor vehicle accidents (MVAs) but can also result from sports injuries or falls (Cervical Spine Injuries). The rapid motion can strain or tear: - Neck muscles and ligaments
- Intervertebral joints
- Discs
- Nerve roots or the spinal cord in severe cases
This damage leads to a condition known as whiplash-associated disorders (WAD), which can range from mild to severe, depending on the force of impact and individual factors like pre-existing neck issues. Symptoms of Whiplash Whiplash symptoms may appear immediately or develop over days, varying in intensity. Common symptoms include: Symptom Description Neck Pain & Stiffness Pain that worsens with movement, often described as a tight or sore neck. Headaches Often starting at the skull base, sometimes radiating to the forehead. Dizziness/Vertigo Feeling unsteady or lightheaded, occasionally with nausea. Fatigue Persistent tiredness is impacting daily activities. Shoulder/Back Pain Discomfort in the upper back or shoulders, sometimes radiating to the arms. Tinnitus Ringing or buzzing in the ears. Cognitive Issues Trouble concentrating, memory lapses, or sleep disturbances. Visual Disturbances Blurred vision or sensitivity to light in some cases. These symptoms can make everyday tasks, such as driving, working, or even turning your head, feel like auditioning for a role as a rusty robot. In severe cases, whiplash may lead to complications like cervical radiculopathy or post-concussion syndrome, especially if untreated (Whiplash Overview). General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Can pace running help runners concentrate on other things, like breathing, form, or mental toughness? Pace Running Running is a sport many participate in and doesn’t require any equipment—only quality running shoes. Running in races comes with various physical and mental challenges. Some runners enjoy running in races and marathons but want to perfect their abilities and techniques, become more consistent, finish in a certain time, or pass a personal record. This is where pace running or working with a pace runner can help achieve those goals. What is a Pace Runner? A pace runner, or pacer, is an experienced runner who can run at a set pace for a long time. The pacer sets the speed so the runner can focus on running. Pacers run in races or marathons to help set the pace for a runner or runners. There are different reasons why professional and amateur runners work with a pace runner. Professional runners often use pace runners to work on techniques and help reach new levels in their running, while amateur runners can work on improving their overall running abilities. There are three typical types of pacers. Race Pacer - Pacers wear or carry signs to make it easier for the runners and can often run split times.
- A split time is the time it takes to run a certain distance.
- Typically, these pacers will run at an even pace.
- Many marathons will have pace groups that run at a specific speed or pace throughout the race.
- The pace groups will have runners running a set time so other runners can key off these runners.
- There are typically set paces for a 3-hour marathon time up to a 6-hour marathon time.
- Runners can use pacers to help them reach their goals without relying on technology, such as a smartwatch or GPS, to determine if they maintain the correct speed throughout the race.
Distance Pacer - Professional and non-professional runners who run long distances or ultramarathons may also use a pace runner to set a specific tempo.
- Ultramarathons are any race with a distance longer than the standard marathon of 26.2 miles.
- Because some ultramarathons can be as long as 50 to 100 miles, runners who choose to have a pacer often have several pacers at different sections to motivate them and help set the rhythm.
Record Pacer or Rabbit - A record pacer, also known as a rabbit, is a pacer who helps a professional runner set a new record.
- A rabbit often leads the race for a predetermined distance at a predetermined pace.
- Some races have multiple pacers at various distances.
How Are Pacers Used? There are different reasons for having a pacer, but they are based on the runner's goals. - A runner being paced runs directly behind a pacer or pacers.
- A pacer can run any pace requested, but typically, the pace groups run at an even pace or with a slight negative split.
- A negative split is when a runner runs the race's second half faster than the first half.
How Do They Help? - A pacer can be helpful because it takes more energy to lead a race than to sit back and follow another runner.
- The pacer is responsible for timing and establishing the tempo so runners only have to focus on running.
- A pacer does more work setting the pace, which allows the runner being paced to relax and not stress about hitting the pace.
A study focused on elite athletes who used pacers. It found that running together at a realistic speed helped optimize and achieve finishing time goals. (Casado A. et al., 2021) However, not all elite events allow pacers to participate. Some championship events, like the Olympics and NCAA Championships, do not allow pacer runners. Benefits Benefits of running with a pacer. Prevent Running Too Fast - When a race begins, runners can take off and start too fast.
- Starting too quickly can negatively impact the runners, like losing energy and stamina.
- A pacer can help start the race with a steady pace, keeping them from going out too fast or expending too much energy.
Maintain an Even Pace - Maintaining an even pace can be difficult throughout a long race or a marathon.
- Having a pacer can relieve some stress and pressure.
- A pacer can keep the runners on an even pace or negative splits versus going out too fast and losing energy.
Focus on the Race - Pacers help the runners stay focused on the race without worrying about how they are running or maintaining the right speed.
- A pacer can help keep runners relaxed.
Motivating - Pacers can help motivate runners.
- The pace runners may encourage individuals along the way and help them stay motivated to keep working toward their goal, especially when the hard parts come.
Disadvantages Running with a pacer can sometimes be more stressful than beneficial, especially for amateur runners. A pacer or pace group can be helpful, but it also can create more stress for some amateur runners. - Sometimes, individuals realize the pacer is running too quickly for what they can handle.
- Anxiety can present as not being able to keep up.
- Other times, runners underestimate their abilities and run more slowly than their bodies can handle.
- However, runners don't have to stay with a pace group just because they started with them.
- Individuals can run ahead.
- Or if the group is too fast, the runner can slow down and join the slower-paced group behind them.
- The key is to listen to your body and do what feels right.
Becoming a Pacer An experienced runner who wants to be a pacer for a race can contact a running organization about becoming a pace runner. - Individuals need to be able to have consistent racing times.
- Be able to run at a set speed for a long duration.
- Most pacers will contact the race organization to apply for a certain pace.
- Some pacers enjoy the thrill of running in a race and helping other runners meet their goals.
- The runner's goals and the type of event also influence who the pacer is.
Injury Medical Chiropractic & Functional Medicine Clinic Individuals can talk to local running experts or a running coach. Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop an optimal health and wellness solution. We focus on what works for you to relieve pain, restore function, and prevent injury. We can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal issues. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Casado, A., Hanley, B., Jiménez-Reyes, P., & Renfree, A. (2021). Pacing profiles and tactical behaviors of elite runners. Journal of Sport and Health Science, 10(5), 537–549. https://doi.org/10.1016/j.jshs.2020.06.011
During pregnancy, is indoor cycling a safe and recommended way to maintain fitness? Pregnancy Indoor Cycling Exercising during pregnancy is highly recommended for both the parent and the baby. Staying physically active can: - Increase blood circulation
- Increase energy
- Reduce backaches
- Improve digestion and sleep
- Enhance mood
- Help manage weight
- Promote muscle tone, strength, and endurance. (Hinman, S. K. et al., 2015)
The American College of Obstetricians and Gynecologists, or ACOG, advises pregnant individuals to exercise regularly during pregnancy. (The American College of Obstetricians and Gynecologists, 2024) The guidelines indicate that individuals who regularly engage in vigorous-intensity aerobic exercise before pregnancy should continue these activities during their pregnancy. (Syed H., Slayman T., & DuChene Thoma K. 2021) According to ACOG, observational studies of pregnant individuals who exercise show benefits such as: - The reduced risk of gestational diabetes mellitus
- Cesarean birth
- Operative vaginal delivery
- Reduced postpartum recovery time
- Exercise can also help prevent postpartum depression. (Syed H., Slayman T., & DuChene Thoma K. 2021)
Stationary cycling has been extensively studied in pregnancy and found safe and beneficial (American College of Obstetricians and Gynecologists, 2024). Safety Indoor cycling is ideal because individuals won’t have to deal with balance challenges or generate a heavy impact on their joints. There are many indoor cycling workouts to try, whether spin or on-demand classes. Indoor cycling is safer during pregnancy than outdoor cycling, which is not recommended because of the risk of falls from traffic and weather conditions. Although indoor cycling is generally considered safe during pregnancy, individuals should get clearance from their OB/GYN if they have any underlying medical conditions that might limit physical activity options. Cycling Classes Taking cycling classes during pregnancy is safe if a healthcare provider has no concerns. It’s important to take precautions. - It’s recommended to continue with any exercise you were doing before pregnancy rather than start a new routine.
- Remember that this is an exercise for two, so the heart rate will elevate quickly and become overheated more easily.
- Take it easier on the bike, and don't push too hard.
Consult With the Instructor It's recommended to seek out an instructor with some prenatal exercise training. Individuals may benefit from sticking with the same instructor whenever possible to get to know them and familiarize themselves with their modifications and needs. Whether or not you’re showing, tell the instructor that you’re pregnant before the class starts. This way, they can monitor progress and will not push too hard. The instructor can also give important pointers on modifying the ride to suit your needs. Modify Bike Set-Up Individuals may need to adjust the saddle position and raise the handlebars to stay comfortable as their bodies change. Sitting more upright is recommended to relieve strain on the lower back, and increasing the handlebars and bringing them closer instead of leaning forward is another goal. Another goal is to keep the weight more evenly distributed between the hands and body. Also, avoid movable indoor bikes that mimic outdoor riding. They can lean sideways, which might cause a fall. Dial Down Intensity With indoor cycling, it’s best to exercise moderately during pregnancy. Consider wearing a heart rate monitor to ensure a safe intensity. It’s also helpful to pay attention to the Rating of Perceived Exertion scale/RPE. Even if the heart rate isn’t too high, slow down or stop exercising immediately if you’re gasping for breath or feeling lightheaded. ACOG guidelines indicate that 13-14 "somewhat hard" on the Borg RPE scale is a safe and acceptable level of exertion. The guidelines also state that RPE is a better gauge of exertion than heart rate and that the talk test (holding a conversation while exercising) can indicate safe workout intensity. Stay Cool and Properly Hydrated Wear comfortable, breathable clothing to help you stay cool and a bra with plenty of support. Drink lots of water throughout the workout, actually more than usual. Overheating and dehydration are common during pregnancy and can be dangerous for both parents and babies. Carrying an extra 20 to 30 pounds and having 40% more blood pumping through the body toward the end of pregnancy makes you likely to sweat more and can easily lead to dehydration. Using a fan for home gyms is highly recommended. Avoid Standing and Stay In a Seated Position During the early months, you may be able to ride in a standing position without any problems. But as the belly grows, it changes the body’s center of gravity, putting more pressure on the joints and making it difficult to ride standing. Joints are looser or more flexible during pregnancy, which makes standing while cycling more difficult and risky. It is still a healthy workout if you stay seated the whole time—and, most importantly, avoid overdoing it or injuring yourself. Body Signs Listen to the body while exercising. If you get winded, dizzy, or unwell while riding, take a break or reduce your effort by a few notches. If a 45-to-60-minute class is too intense, feel free to depart early; just let the instructor know you’re OK. Energy will likely ebb and flow during pregnancy, so pay attention to the body's signals and take care of them accordingly. Stop exercising if you experience any of the following (Syed H., Slayman T., & DuChene Thoma K. 2021) - Abdominal pain
- Dyspnea: shortness of breath before exertion
- Headache
- Dizziness
- Calf pain or swelling
- Muscle weakness affects balance
- Chest pain
- Amniotic fluid leakage
- Regular painful contractions
- Vaginal bleeding
Call your doctor if you experience sharp pain, contractions, a surge of fluid, a sudden severe headache, prolonged swelling, or decreased baby movement. Injury Medical Chiropractic & Functional Medicine Clinic It’s important to exercise wisely during the nine months to accommodate body changes, the extra weight, the increasingly relaxed ligaments, and the shift in the center of gravity. The stationary bike provides a personalized, low-impact workout. You get to control the intensity and the duration of the ride. Monitor your heart rate and/or RPE to avoid overdoing it. Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop an optimal health and wellness solution. We focus on what works for you to relieve pain, restore function, and prevent injury. Regarding musculoskeletal pain, specialists like chiropractors, acupuncturists, and massage therapists can help mitigate the pain through spinal adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal issues. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Hinman, S. K., Smith, K. B., Quillen, D. M., & Smith, M. S. (2015). Exercise in Pregnancy: A Clinical Review. Sports Health, 7(6), 527–531. https://doi.org/10.1177/1941738115599358 The American College of Obstetricians and Gynecologists. (2024). Exercise during pregnancy. https://www.acog.org/womens-health/faqs/exercise-during-pregnancy?utm_source=redirect&utm_medium=web&utm_campaign=int Syed, H., Slayman, T., & DuChene Thoma, K. (2021). ACOG Committee Opinion No. 804: Physical Activity and Exercise During Pregnancy and the Postpartum Period. Obstetrics and gynecology, 137(2), 375–376. https://doi.org/10.1097/AOG.0000000000004266
Can converting a bicycle into a stationary bike be a way for individuals to exercise more while still enjoying cycling? Bicycle Stationary Conversion Is your bike collecting dust in the garage? Do you miss riding, but the weather or temperatures keep you indoors? Why not quickly and painlessly turn your bike into a stationary bike? An indoor stationary bike is a great way to maintain physical activity while avoiding inclement weather and outdoor elements. Plus, bicycle stationary conversion in your home, office, or garage is quick and straightforward. A bike trainer or roller is needed to convert a bicycle into a stationary bike. The bike is mounted onto the trainer stand, and its rear axle is replaced with a special axle provided with the trainer kit to secure it and hold the wheel in place while allowing you to pedal, creating resistance for indoor cycling. Cycling Bicycle stationary conversion isn’t only for die-hard cyclists. Research shows indoor cycling is a great way to stay healthy and consistent with your workouts. One study showed that indoor cycling improves aerobic capacity, blood pressure, lipid profile, and body composition. (Chavarrias, M. et al., 2019) Stationary Bikes Types For those who don’t have the space or know that they won't regularly use a stationary bike, indoor bike trainers and rollers can provide convenient, economical, and compact options. Whether individuals want to exercise more, maintain a riding schedule, or train for an event, trainers and rollers can be highly effective tools for any cyclist. However, choosing between a bike trainer and rollers varies depending on the pros and cons. Selecting the right equipment depends on several factors, including: - Personal needs
- Space - indoor or garage.
- Cycling experience
Most cyclists, even hobbyists, prefer indoor cycling bikes over traditional stationary bikes because they are riding a real bicycle, including the positioning and pedaling, compared to upright, air, or recumbent bikes. Trainer A bike trainer is a stand that lets an individual ride a regular bicycle while stationary. Cyclists often use it to warm up before races, and it comes in handy when weather conditions or time constraints prevent riding outdoors. Most trainer stands can accommodate bicycles. Trainers are suitable for beginners and professional riders. There are two types of indoor bike trainers. Direct-drive - Direct-drive trainers attach to the bike’s rear dropouts, replacing the wheel and providing a direct connection to the resistance unit.
- These can cost more, but they're worth the investment because they’re more accurate and deliver the highest resistance levels.
Friction - A small roller is installed against the rear wheel with friction trainers, which use magnetic or fluid resistance.
- These are typically lighter and easier to transport than direct-drive trainers but are less accurate and provide less resistance.
Rollers Rollers are the most basic type of indoor stationary bike but may not be the best option for individuals new to indoor cycling. This is because it requires advanced cycling techniques, such as balancing and keeping the front tire straight while riding. The cycle is on rollers instead of being fixed, allowing the resistance to range from zero to the equivalent of a direct-drive trainer. Rollers help refine pedaling technique and improve cycling form because you balance and stabilize while riding. Conversion - What Is Needed The most important equipment needed to convert the cycle is a bike stand, which will be the foundation of the stationary bike setup. (Bike To Work Day, 2025) There are two-piece stands and one-piece stands. (Bike To Work Day, 2025) Tools like an Allen wrench may be needed. Various bike trainer kits contain all the parts needed for this conversion, but extra standard tools may be required to remove the back wheel and replace the axle. - Choose the right trainer: Consider your bike type, desired resistance levels, and budget.
- Install the trainer: Follow the manufacturer's instructions to position and secure the trainer properly.
- Mount the bike: Remove the rear wheel quick release, insert the trainer's axle, and tighten it securely.
- Adjust resistance: Most trainers have a knob or lever to control the difficulty level.
- If you are uncertain whether your bike stand is set up correctly or having issues with the installation, contact a professional bike mechanic. They can help get the stationary bike up and running properly.
Considerations - Tire wear: Using a dedicated trainer tire for the rear wheel can minimize wear and tear.
- Noise level: Some trainers can be noisy, especially wheel-on types.
- Stability: Ensure the bike is properly secured on the trainer and your training area is stable.
Injury Medical Chiropractic and Functional Medicine Clinic Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop optimal health and wellness solutions. For musculoskeletal pain, chiropractors, acupuncturists, and massage therapists can mitigate the pain through spinal adjustments that help the body realign itself. The clinic can also integrate a treatment plan to resolve musculoskeletal problems with other medical professionals. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies that are available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Chavarrias, M., Carlos-Vivas, J., Collado-Mateo, D., & Pérez-Gómez, J. (2019). Health Benefits of Indoor Cycling: A Systematic Review. Medicina (Kaunas, Lithuania), 55(8), 452. https://doi.org/10.3390/medicina55080452 Bike To Work Day. (2025). How to turn a bike into a stationary bike: Things to know. https://biketoworkday.us/turn-a-bike-into-a-stationary-bike/#Setting_up_Your_Stationary_Bike
Can individuals incorporate these simple but effective exercise routines to reduce pain and discomfort in their spine and back? Why It’s Important To Keep The Back Mobile When many individuals are dealing with back pain from their upper, middle, and lower portions, it can put a halt to a person’s routine. When back pain becomes present, it causes the person to find a comfortable place like a couch or a bed and lie down. However, this can cause more issues than the original one, affecting the individual. Back pain is a common worldwide problem and is the leading issue of disability associated with a high socio-economic cost. (Chou, 2021) Additionally, when a person is dealing with back pain, they are also dealing with degenerative issues that are also affecting their spines, thus causing problems to their joints, discs, and bones. (Hauser et al., 2022) This is because back pain is a multifactorial musculoskeletal disorder that can cause referred pain to different body locations. So when a person dealing with back pain rests, it can become an issue as inflammation builds up and swelling in the affected areas. Hence, many doctors, chiropractors, physical therapists, and spine specialists recommend keeping mobile to allow blood flow and the body’s natural healing response to reduce pain and speed up recovery. Since back pain relief is challenging through visceral-somatic disturbances, it is important to find various treatment options to aid the person’s specific condition. As a person goes to get treatment for their back pain, it is important to note that the causes of their back pain can help determine which exercises can be most effective within their treatment plan. We associate with certified medical providers who inform our patients of the benefits of incorporating simple but effective exercises for their back pain. While asking important questions to our associated medical providers, we advise patients to integrate an exercise routine to reduce the chances of environmental factors causing back pain to return. Dr. Alex Jimenez, D.C., envisions this information as an academic service. Disclaimer. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
|
Starting a weight-loss exercise routine is not usually a motivation problem. Most people feel motivated at the beginning. The real challenge is staying consistent when life gets busy, energy dips, or progress feels slow. The good news is that motivation is not something you either have or do not have. Motivation is something you can build with simple systems: clear goals, tiny daily actions, tracking, support, and a plan for hard days. When you combine that with low-impact movement you actually enjoy, your routine becomes much easier to stick with over time. (Cleveland Clinic, 2024; HelpGuide, n.d.; Planet Fitness, n.d.) Below is a practical, beginner-friendly approach that focuses on consistency first, intensity later. Start With SMART Goals That Are Small Enough to Win A common mistake is setting a goal that is too big, too vague, or too fast. "Lose weight" is not a plan. "Walk 20 minutes, 4 days a week" is a plan you can actually follow. SMART goals help because they turn hope into steps. SMART stands for: -
Specific: What exactly will you do? -
Measurable: How will you track it? -
Achievable: Can you realistically do it right now? -
Relevant: Does it fit your "why" and your life? -
Time-bound: When will you do it and for how long? Examples of beginner SMART goals: -
"Walk for 15 minutes after dinner, 5 days a week, for the next 2 weeks." (Hey Life Training, n.d.; Modern Image Aesthetics, 2024) -
"Do a 10-minute yoga video on Monday, Wednesday, and Friday for 30 days." (HelpGuide, n.d.) -
"Dance for 3 songs every day at 6 p.m. for the next 14 days." (Medical Beauty & Weight Loss, 2025) Why this works: your brain stays motivated when it can see clear wins. Small wins build confidence, and confidence builds consistency. (Cleveland Clinic, 2024) Start Small and Build Consistency Before You Build Intensity When you are a beginner, the goal is not to "go hard." The goal is to show up. Ten minutes done consistently beats one intense workout followed by two weeks off. A simple beginner progression can look like this: -
Week 1–2: 10–15 minutes per day, most days -
Week 3–4: 15–25 minutes per day, most days -
Month 2: Add light strength training 2 days per week -
Month 3: Add time, resistance, or variety as your body adapts HelpGuide also highlights that "something is always better than nothing," and that you can build toward the general public health goal of about 150 minutes per week by starting small and stacking minutes over time. Beginner-friendly low-impact options that are easier to recover from: -
Walking (outside, treadmill, mall walking) -
Gentle cycling -
Swimming or water exercise -
Beginner yoga or chair yoga -
Light resistance bands -
Bodyweight strength (sit-to-stand, wall pushups) Picking low-impact movement reduces soreness and injury risk, helping you stay consistent. (Cleveland Clinic, 2024; HelpGuide, n.d.) Track Progress in More Than One Way (So You Do Not Quit Too Early) If you only track the scale, motivation can drop fast. Weight can fluctuate due to sleep, stress, salt, hormones, and muscle soreness. Instead, track multiple "wins," so your progress is obvious. Helpful things to track: -
Minutes exercised per week -
Step count (daily or weekly average) -
How many days you moved this week -
Waist measurement (every 2–4 weeks) -
How your clothes fit -
Energy, mood, sleep quality -
Strength progress (more reps, easier stairs, better balance) Planet Fitness encourages tracking progress and celebrating milestones because visible progress supports motivation and consistency. Zen Habits also emphasizes noticing how good you feel after exercising, which can become its own motivation over time. Simple tracking tools that work: Tracking is not about being perfect. It is about seeing proof that your effort is working. Make It Enjoyable (Because Fun Beats Willpower) If you hate your workout, you will eventually stop doing it. Enjoyment is not a bonus. For beginners, enjoyment is a strategy. Ways to make exercise more enjoyable: -
Pick music, podcasts, or audiobooks you love -
Walk a new route once a week -
Try dancing, swimming, or cycling instead of forcing the gym -
Use “exergames” (movement-based video games) to make it feel like play -
Join a beginner class where you feel comfortable HelpGuide recommends making exercise feel more like a game, which can reduce boredom and increase follow-through. Planet Fitness also encourages finding your “why,” building a plan that fits your lifestyle, and using tracking to keep motivation steady. A practical rule: choose the version of movement you can repeat. That is the one that works. Use Rewards the Right Way (Non-Food Wins That Reinforce the Habit) Rewards help because they teach your brain: “When I do this, something good happens.” The key is to use rewards that support your goal and do not turn into a setback. Good non-food rewards: -
New workout socks or a comfortable shirt -
A movie night -
A new water bottle -
A massage or sauna session -
Extra time for a hobby -
A relaxing bath or early bedtime Zen Habits lists rewards and positive feelings after exercise as real motivators that can keep you returning. Modern Image Aesthetics also highlights tracking and celebrating small victories as a way to maintain motivation. Example milestone plan: -
5 workouts = new playlist -
10 workouts = new walking shoes (if needed) -
20 workouts = new gym bag or massage Keep rewards tied to your effort, not to the scale. Build Accountability So You Are Not Doing This Alone Accountability can be a “buddy,” a coach, a class, or a clinic check-in. The goal is simple: make it easier to show up, even when motivation is low. Accountability ideas: -
Walk with a friend twice a week -
Join a beginner class (in-person or online) -
Schedule workouts on your calendar like appointments -
Use a group chat to report “done” -
Get a dog and commit to daily walks (if that fits your life) Cleveland Clinic recommends enlisting support from a friend or professional when building a new routine. Modern Image Aesthetics also emphasizes the value of a support system for motivation and consistency. Reddit threads on consistency often echo a practical truth: routines that match your lifestyle are easier to keep long-term, and rest or lighter days can be part of the plan. Remember Your “Why” (And Make It Real) Your “why” is the deeper reason you want change. A strong “why” helps you keep going when motivation drops. Examples of strong “why” statements: -
“I want better energy in the afternoon.” -
“I want to sleep better and wake up less stiff.” -
“I want to feel confident in my clothes.” -
“I want to keep up with my kids or grandkids.” -
“I want less pain and better mobility.” Planet Fitness specifically encourages identifying your “why” as a foundation for staying motivated during a weight-loss journey. Try this quick exercise: write your “why” in one sentence and place it where you will see it (phone lock screen, bathroom mirror, fridge). Plan for Low-Energy Days (So You Do Not Break the Habit) A big reason people quit is this belief: "If I cannot do the full workout, I might as well do nothing." That mindset kills consistency. Instead, create a backup plan. Your backup plan is the smallest action that keeps the habit alive. Backup plan ideas (10 minutes or less): -
Gentle yoga flow -
Slow walk around the block -
Stretching + deep breathing -
5-minute bodyweight circuit (very light) -
Mobility routine for hips, ankles, and shoulders HelpGuide's "something is better than nothing" message fits perfectly here. On tough days, the goal is not fitness. The goal is identity: "I am someone who keeps my promises to myself." Beginner Weight-Loss Exercise Ideas That Actually Work Here are simple, effective workouts that build confidence without overwhelming you. Walking plan (beginner-friendly) Walking is a low-impact way to build endurance and can also support mobility and posture when done consistently. Beginner strength routine (2 days per week) Do 1–2 rounds: -
Sit-to-stand from a chair: 8–12 reps -
Wall pushups: 8–12 reps -
Hip hinge (good morning) with no weight: 8–12 reps -
Farmer carry with light weights: 30–60 seconds -
Gentle plank (countertop plank): 20–30 seconds Strength training supports fat loss by helping you maintain muscle while you lose weight. Fun cardio options Choose one: Enjoyable activities are often easier to sustain long-term. Functional training (simple "real life" movement) Functional exercises can make daily movement easier (stairs, lifting, getting up from the floor). MultiFit lists functional movements such as squat-to-press, swings, Turkish get-ups, medicine ball slams, and lateral lunges with rotation as examples of training styles for fitness and weight loss. Beginners can start with bodyweight versions and focus on control rather than speed. How an Integrative Chiropractic + Functional Medicine Clinic Can Boost Motivation Many people want to exercise, but pain, stiffness, fatigue, and slow recovery get in the way. This is where integrative care can help remove barriers, making movement feel safer and more realistic. Pain reduction and improved mobility Chiropractic care is commonly associated with improving musculoskeletal function and reducing pain, making it easier for beginners to move more consistently. When pain is lower, the mental barrier to exercise often drops too. Low-impact plans that fit your body Instead of pushing you into intense workouts too early, integrative clinics often emphasize manageable steps (walking, gentle strength, mobility work). This aligns with behavior-change guidance: start realistically and build gradually. Addressing metabolic barriers with functional medicine thinking Functional and integrative weight management programs often focus on more than calories, including sleep, stress, nutrition quality, and metabolic health. Jefferson Health describes integrative weight management through the Marcus Institute for Integrative Health as a specialized approach that includes functional medicine for weight loss and weight management. Stress, sleep, and recovery support Stress and poor sleep can worsen cravings, energy, and recovery. Dr. Alexander Jimenez's clinical writing highlights the value of a broader, “whole-person” approach when discussing weight-related challenges, including the role of lifestyle factors beyond diet and exercise alone. Built-in accountability Regular visits, re-checks, and measurable progress markers can create structure, which helps people stay consistent. Support systems and check-ins are repeatedly linked to better follow-through in real-world weight-loss efforts. Clinical Observations From Dr. Alexander Jimenez, DC, APRN, FNP-BC In integrative injury and wellness care, a common pattern is simple: people stay more motivated when movement feels doable, and symptoms are not constantly flaring. Dr. Jimenez often emphasizes practical, repeatable habits that support mobility and function, including low-impact activity like walking and lifestyle strategies that support metabolic health. From a clinical perspective, motivation improves when patients experience: -
Less pain and stiffness during basic movement -
Better confidence in posture and stability -
Clear “next steps” instead of confusing advice -
Progress that is tracked in multiple ways (not only weight) -
A plan that matches real life (time, stress, sleep, schedule) That combination often turns exercise from something scary into something safe, structured, and repeatable. A Simple Weekly Motivation Blueprint (Beginner Version) If you want a clear starting point, try this: Weekly plan (first 2 weeks): -
Walk 15 minutes, 4 days/week -
Gentle mobility or stretching, 5–10 minutes, 2 days/week -
One optional "fun movement" day (dance, swim, bike) Motivation supports: -
Write your "why" in one sentence -
Track minutes and step count -
Pick one non-food reward at the end of week 2 -
Add one accountability piece (buddy, class, check-in) This is not "too easy." This is how you build a base that lasts. Transform your Body! | El Paso, Tx References The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and facilitate clinical collaboration with specialists across disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and identify relevant research studies for our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We are here to help you and your family. Blessings Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182 Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-State Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
New York APRN License #: N25929, Verified: APRN-N25929*
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States* Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
A back extension machine—often called a hyperextension bench or Roman chair—is gym equipment that helps strengthen the “backside” of your body. This includes your lower back, glutes, and hamstrings (the muscles along the back of your thighs). When used with good form, it can improve core stability, support better posture, and help you build the strength you need for daily life and sports. (Chuze Fitness, 2022; MasterClass, 2021). This article explains: -
What the back extension machine is and what it trains -
How to set it up for your body -
Step-by-step form (without painful “over-arching”) -
Common mistakes and safety tips -
How integrative chiropractic care and nurse practitioner support can fit into a complete plan (including clinical observations consistent with Dr. Alexander Jimenez’s integrative approach) What the Back Extension Machine Does (and Why It Matters) Back extensions are a hip-hinge movement. That means the motion should come mostly from the hips, not from cranking your spine backward. Done correctly, you train the posterior chain—the muscle team that helps you stand tall, lift safely, and protect your lower back. (MasterClass, 2021). Main muscles trained -
Glutes (hip power and pelvis support) -
Hamstrings (hip hinge control) -
Erector spinae (small and medium muscles that support the spine) -
Core bracing muscles (to keep your trunk stable) Many people don’t realize how much the glutes and hamstrings should help during back extensions. When they do, the lower back often feels less “pinched” and more supported. Key Benefits (When You Use It Correctly) A back extension machine is popular because it can build strength without needing a barbell. It can also be adjusted to fit different body sizes and goals. (Verywell Fit, 2025). Common benefits include: -
Lower-back strength and endurance (Chuze Fitness, 2022). -
Better posture support (stronger backside helps you stay upright) (Chuze Fitness, 2022). -
Stronger glutes/hamstrings, which can protect your back by sharing the workload (MasterClass, 2021). -
Improved range of motion and control when you hinge at the hips (Verywell Fit, 2025). Important note: If you already have back pain, the goal is not to “push through.” The goal is to move well, build strength gradually, and stop if pain increases. Machine Types: What You Might See at the Gym You might see different setups. They all aim at a similar pattern, but your body position changes slightly. -
45-degree hyperextension bench (common in gyms) -
Roman chair (similar, often more upright) -
GHD-style back extension (often in performance gyms; can be more intense) Some equipment brands highlight adjustability to target hips/glutes/hamstrings and accommodate different body sizes. (Valor Fitness, n.d.). How to Set Up the Back Extension Machine (Quick Checklist) A good setup makes safe form much easier. Step 1: Pad placement -
The pad should sit just below your hip bones, so you can hinge at the hips. -
You should be able to bend forward without the pad jamming into your stomach. Step 2: Foot and ankle position Step 3: Start position WebMD’s basic guidance commonly includes bracing, controlled movement, and avoiding sloppy form. (WebMD, 2024). Step-by-Step: How to Do Back Extensions Safely Think: hinge, brace, squeeze glutes, return to neutral. Brace and align -
Cross your arms over your chest or keep your hands at your sides. -
Keep your neck neutral (look at the floor a few feet ahead). -
Tighten your stomach gently—like you’re “locking in” your torso. Hinge down (slowly) -
Push your hips back. -
Lower until you feel a stretch in your hamstrings or you reach a comfortable range. -
Keep the spine neutral (not rounded hard, not over-arched). Lift using glutes and hamstrings -
Squeeze your glutes to bring your torso back up. -
Stop at neutral, where your body is in a straight line again. Avoid “hyperextending” at the top This “neutral spine” focus aligns with standard safety cues in mainstream exercise education resources. (MasterClass, 2021; WebMD, 2024). Common Mistakes (and Easy Fixes) Mistake: Bending from the lower back instead of the hips Fix: Think “hips back” first. The pad is there so your hips can hinge. Mistake: Throwing yourself up fast Fix: Slow down. Use a 2–3 second lower and a controlled lift. Mistake: Over-arching at the top Fix: Stop at neutral. Squeeze glutes and brace abs. Mistake: Feeling it mostly in the lower back Fixes to try: -
Slightly tuck your pelvis at the top (gentle, not forced) -
Squeeze glutes earlier in the movement -
Reduce the range of motion for now Who Should Be Careful (or Get Guidance First) It’s smart to talk with a qualified clinician before starting, especially if you have new, severe, or spreading symptoms. Get checked first if you have: -
Pain shooting down the leg, numbness, or weakness -
Bowel/bladder changes -
Fever, unexplained weight loss, or pain at night -
Recent trauma (car accident, fall) -
Known spinal fracture, severe osteoporosis, or an unstable spine condition For many people, the back extension can still be useful—but the right version, range, and load matters. Progressions: How to Build Strength Without Flaring Pain Start easy. Your tissues adapt with time and consistency. Beginner (2–3 days/week) Intermediate Advanced options (only if form is solid) -
Pause reps (1–2 seconds at neutral) -
Single-leg variations (higher skill) -
Higher resistance (slowly) Verywell Fit’s equipment overview also emphasizes choosing a machine style that fits your space, needs, and experience level. (Verywell Fit, 2025). Integrative Care: Why Combine Strength Work + Chiropractic + Nurse Practitioner Support? Strength training can be powerful—but it’s often not the full story. Many people also need: -
Better joint mobility -
Nervous system calming strategies -
Lifestyle changes (sleep, stress, nutrition) -
A plan that matches their specific diagnosis Chiropractic care (how it can help) Chiropractic care often focuses on: -
Restoring motion in stiff spinal or pelvic joints -
Reducing mechanical irritation -
Helping patients move with better control and confidence Some chiropractic resources describe improvements such as better alignment, increased mobility, and relief of pressure/irritation around sensitive tissues. (Calhoun Spine Care, 2026). Nurse practitioner support (how it can help) Nurse practitioners can support a “whole-person” plan, including: -
Screening for red flags and medical causes of pain -
Medication guidance when appropriate -
Sleep support, nutrition coaching, and inflammation-aware habits -
Coordinating imaging or referrals when needed Why integration works better than “one thing” Some integrative care resources emphasize combining adjustments + guided exercise to improve function, reduce pain, and lower the chance of repeat flare-ups. (OptmzState, 2026). Clinical Observations Consistent With Dr. Alexander Jimenez’s Integrative Approach Dr. Alexander Jimenez, DC, APRN, FNP-BC, often presents a model that combines: -
Chiropractic care + functional/integrative strategies -
Rehab-style strengthening and movement retraining -
A multidisciplinary approach for complex cases, including injury recovery and chronic pain support In real-world practice, many people improve faster when they: -
Calm pain drivers (irritation, overload, poor mechanics) -
Restore mobility where needed -
Rebuild strength gradually (including posterior chain work like back extensions) -
Address sleep, stress, and recovery habits That “stacked” approach is often what turns short-term relief into long-term stability. A Simple Weekly Plan (Example) This is a general example for many adults with mild recurring back tightness (not severe or worsening pain). 2–3 days/week strength -
Back extension machine: 2–3 sets of 8–12 -
Glute bridge: 2–3 sets of 10–15 -
Side plank: 2–3 sets of 20–40 seconds -
Easy walking: 10–30 minutes Daily habits -
Short movement breaks every 30–60 minutes -
Gentle hip flexor and hamstring mobility -
Sleep routine (same bedtime/wake time most days) If symptoms worsen, step back and get evaluated. Quick FAQ “Should I feel it in my low back?” You may feel your low back working, but it shouldn’t feel sharp, pinchy, or like it’s doing 100% of the job. You should also feel glutes and hamstrings helping. “How far down should I go?” Go only as far as you can keep control and stay comfortable. More range is not always better early on. “Is it good for preventing back pain?” Many fitness sources suggest that stronger posterior chain support can help reduce strain and support posture. (Chuze Fitness, 2022).
But prevention works best when strength is combined with smart movement and recovery habits.
Safety Disclaimer This article is for general education and is not medical advice. If you have severe pain, progressive weakness, numbness, or other concerning symptoms, seek evaluation from a licensed healthcare professional. References The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and to identify relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
When people say they “want to get healthy,” they often confuse fitness with wellness. The terms sound similar, but they are not the same. -
Fitness is your physical ability – your strength, endurance, flexibility, and how well your body can perform tasks like walking, lifting, or climbing stairs. (HelpGuide, 2025; MedlinePlus Magazine, 2022) HelpGuide.org+1 -
Wellness is a broader, holistic state. It includes your physical, mental, emotional, social, and sometimes spiritual health. (Long, 2024; EBSCO Research Starters, n.d.) ACE Fitness+1 Exercise is the bridge between fitness and wellness. Regular movement helps your muscles and heart, but it also boosts mood, lowers stress, and supports long-term health. As Dr. Alexander Jimenez, DC, APRN, FNP-BC, emphasizes in his integrative practice in El Paso, patients do best when spinal health, movement, and lifestyle habits are addressed together—not in isolation. El Paso, TX Doctor Of Chiropractic What Is Fitness? Fitness is about what your body can do. It describes how well your heart, lungs, muscles, and joints work together during activity. (MedlinePlus Magazine, 2022; HelpGuide, 2025) NIH MedlinePlus Magazine+1 Common components of physical fitness include: -
Cardio endurance – how long you can walk, jog, or cycle without tiring quickly. -
Muscular strength – how much force you can produce, like lifting a heavy box. -
Muscular endurance – how long your muscles can work without fatigue. -
Flexibility – how easily your joints move through a full range of motion. -
Body composition – the balance of muscle, fat, bone, and water in your body. (HelpGuide, 2025) HelpGuide.org When you train for fitness, your goals might be: -
Walking 30 minutes without getting winded -
Doing a set of pushups or squats -
Reducing joint stiffness -
Improving posture and balance Fitness focus is often performance-oriented: “How far, how fast, how strong?” What Is Wellness? Wellness goes beyond muscles and lungs. It is a whole-person state of health where different areas of your life feel in balance. (Foothills Sports Medicine PT, 2017; Long, 2024) Foothills Therapy & Sports Medicine+1 Wellness models usually include several dimensions: -
Physical wellness – movement, nutrition, sleep, and medical care -
Emotional wellness – coping with stress and managing emotions in healthy ways -
Mental/intellectual wellness – learning, problem-solving, creativity -
Social wellness – supportive relationships and a sense of belonging -
Occupational/financial wellness – meaningful work and stable finances -
Spiritual or purpose-based wellness – values, beliefs, and a sense of meaning As EBSCO’s physical wellness summary notes, physical wellness includes regular activity, a balanced diet, sleep, and wise choices about substances, and it closely connects with emotional and social health. EBSCO In simple terms: Fitness is what your body can do.
Wellness is how well you feel and function overall. How Exercise Bridges Fitness and Wellness Regular exercise is one of the strongest links between fitness and overall wellness. It builds your physical capacity while also supporting your mood, brain, and long-term health. Health organizations like the CDC and many rehab clinics recommend at least 150 minutes of moderate aerobic exercise per week (for example, brisk walking) plus strength training on 2 or more days. (Foothills Sports Medicine PT, 2017; Mayo Clinic, 2023) Foothills Therapy & Sports Medicine+1 Physical benefits -
Stronger heart and lungs -
Better muscle strength and endurance -
Improved joint mobility and flexibility -
Lower risk of heart disease, type 2 diabetes, and some cancers Foothills Therapy & Sports Medicine+1 -
Lower risk of falls and fractures in older adults Mental and emotional benefits -
Lower stress and anxiety -
Improved mood and self-esteem -
Better sleep quality -
Sharper thinking and memory (HelpGuide, 2025; EBSCO Research Starters, n.d.) HelpGuide.org+1 Social and lifestyle benefits -
More energy for work, family, and hobbies -
Greater confidence to join group activities or sports -
A sense of progress and control over your health This is why many experts say exercise is not just “training your body,” but also medicine for your brain and life. Wellness Exercise vs. Fitness Exercise Both wellness and fitness exercises use movement, but the focus and mindset can differ. Fitness-focused exercise Here, your goal is physical performance: -
Running faster or farther -
Lifting more weight -
Improving sport performance -
Hitting specific numbers (steps, reps, time, pace) You might see: Wellness-focused exercise Here, your goal is how you feel overall: Wellness exercise often includes: -
Walking for mood and energy -
Yoga, tai chi, or Pilates for body–mind balance -
Stretching and mobility work -
Gentle strength training to support daily life Many sources emphasize that wellness exercise is about consistency and enjoyment, not perfection or competition. (Chambers, n.d.; VIDA Fitness, n.d.) Kellie Chambers+1 In reality, most people benefit from a blend: -
Enough fitness work to keep your heart, muscles, and joints strong -
Enough wellness-focused movement to manage stress and support a calm, resilient nervous system Where Integrative Chiropractic Care Fits In Chiropractic care focuses on the spine, nervous system, and musculoskeletal health. Integrative chiropractic care goes further by combining spinal adjustments with exercise, lifestyle, and sometimes nutrition or functional medicine. (Newbold Chiropractic, n.d.; ShoreLife Chiropractic & Wellness, n.d.) Newbold Chiropractic+1 Chiropractic can support both fitness and wellness by: -
Aligning the spine to reduce joint stress and improve posture -
Improving nerve function, which helps muscles coordinate and recover -
Reducing pain in areas like the neck, back, hips, and shoulders -
Improving range of motion, making exercise easier and safer -
Prescribing specific exercises, like stretches, core work, and postural drills Clinics that focus on wellness and prevention often use chiropractic care to keep the spine moving well, to reduce future injuries, and to support long-term lifestyle change. Evolve Chiropractic+1 Dr. Jimenez’s clinical perspective In Dr. Alexander Jimenez’s El Paso practice, care plans often include: El Paso, TX Doctor Of Chiropractic -
Detailed assessments of posture, movement, and joint function -
Chiropractic adjustments to restore spinal and joint alignment -
Sports medicine and agility training to rebuild strength and coordination -
Functional medicine and nutrition to support energy, healing, and weight management -
Tailored home exercise programs, including mobility and strengthening From his experience with thousands of patients, he observes that those who combine spinal care with consistent movement and lifestyle changes tend to: -
Recover faster from injuries -
Maintain better mobility as they age -
Feel more energetic, focused, and resilient The Synergy: Chiropractic Care + Exercise Combining chiropractic care with exercise creates a powerful synergy. Each approach supports the other. Sports medicine and wellness-oriented chiropractors describe this combined approach as a key strategy for performance, recovery, and long-term health. Tigard Chiropractic+1 How chiropractic prepares the body for exercise -
Corrects joint restrictions that limit movement -
Reduces compensations that overload certain muscles -
Helps normalize nerve signals to muscles -
Decreases pain that might make you avoid movement How exercise supports chiropractic results -
Strengthens the core to stabilize the spine -
Builds muscle around adjusted joints to keep them in better alignment -
Improves circulation, which supports tissue healing -
Trains better movement patterns for daily life and sport Together, they can: -
Lower the risk of future injuries -
Improve balance and coordination -
Enhance athletic performance and daily function -
Support long-term fitness and wellness, not just short-term symptom relief Tigard Chiropractic+1 Many clinics note that patients do best when they: -
Get adjusted to create a healthy structural foundation -
Perform targeted exercises to reinforce that foundation -
Keep up general wellness habits like walking, stretching, and good sleep Dr. Jimenez’s integrative clinic reflects this model by combining chiropractic, rehabilitative exercise, functional medicine, and wellness coaching to support “normal body functions” and “total functional health.” El Paso, TX Doctor Of Chiropractic Building Your Own Fitness–Wellness Plan You don’t need a perfect plan to start. You just need a clear, simple path that respects both fitness and wellness—ideally with professional guidance when you have pain or past injuries. 1. Clarify your main goal Ask yourself: -
Do I want more energy for daily life? -
Do I want to move without pain? -
Do I want to improve strength, balance, or endurance? -
Do I want to feel calmer and sleep better? Your answers help decide how much of your plan is fitness-focused (performance, strength, endurance) and how much is wellness-focused (stress relief, sleep, mood). 2. Get a baseline assessment If you have pain, previous injuries, or major stiffness, start with an integrative provider such as: -
An integrative chiropractor -
A chiropractor who works with physical therapy or rehab exercises -
A clinic like Dr. Jimenez’s, that blends chiropractic, functional medicine, and movement coaching El Paso, TX Doctor Of Chiropractic+1 They can: -
Check posture and spinal alignment -
Evaluate joint mobility and muscle imbalances -
Identify red flags that need imaging or medical follow-up -
Suggest safe starting points for exercise 3. Build a weekly movement routine A balanced week might include: Example weekly pattern: -
3 days: Cardio + short strength circuit -
2 days: Strength + core + stretching -
Most days: Light walking and movement breaks 4. Layer in wellness habits To support whole-person wellness, add: -
Nutrition – more whole foods, fiber, and water to fuel activity and support body composition NIH MedlinePlus Magazine+1 -
Sleep – aim for 7–8 hours most nights -
Stress management – breathing exercises, mindfulness, or gentle stretching -
Social connection – walking with a friend, group classes, or family activity nights These habits help your nervous system recover, making your workouts more effective and your body more resilient. 5. Re-assess and adjust Wellness is not a one-time project. It changes with age, injuries, and life demands. Every few months, check: Work with your chiropractor or integrative provider to refine your exercise plan, posture habits, and lifestyle strategies so they match your current needs. Tigard Chiropractic+2ShoreLife Chiropractic & Wellness+2 The Takeaway: Fitness, Wellness, and the Power of Exercise + Chiropractic Care To pull it all together: -
Fitness = how strong, flexible, and durable your body is; what you can physically do. -
Wellness = how well you feel and function in all areas of life—body, mind, and relationships. -
Exercise = the bridge that connects fitness and wellness by strengthening your body, improving your mood, and supporting long-term health. -
Integrative chiropractic care = the foundation builder, aligning the spine, improving nerve function, easing pain, and guiding exercises that protect and enhance movement. When you combine chiropractic care and exercise, you create a structure where: Chiropractic sets the foundation.
Exercise builds the house.
Wellness is how good it feels to live in it. By respecting both fitness and wellness—and using exercise plus integrative spine care—you give yourself the best chance for long-term mobility, lower injury risk, and a healthier, more satisfying life. Aligned & Empowered: Chiropractic Conversations on Women’s Health References The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and to identify relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Summary -
Pre-workout massage (light pressure) can help you feel loose, warm, and ready—but avoid deep tissue right before training because it may temporarily reduce muscle strength or speed. (Dakić, 2023; Mine & Nakayama, 2018; Arabaci, 2008; One Peloton, 2024). Peloton+3PubMed Central+3PubMed Central+3 -
Post-workout massage is the better choice for recovery—it supports circulation, reduces soreness, and helps you relax. (Verywell Fit, 2022; PureGym, 2025; Northwich Foot Clinic, 2023; Marathon Handbook, 2023). Marathon Handbook+3Verywell Fit+3PureGym+3 -
Blending massage with chiropractic care targets both soft tissue and joint alignment. This combo can improve mobility, flexibility, and pain relief, and it often leads to longer-lasting results. (The Joint, 2025; Link Chiropractic Clinic, 2025; ChiroSports USA, 2025; Maverick Chiropractors, n.d.). Maverick Chiropractic+3The Joint Chiropractic+3Link Chiropractic Clinic+3 Why timing matters Your body needs different inputs before a workout versus after it. Before training, your goal is readiness—you want muscles warm and responsive. After training, your goal is recovery—you want to reduce soreness and restore balance. Light, brief massage strokes (think Swedish-style, rhythmic glides) can increase blood flow, ease stiffness, and support range of motion pre-workout, especially when paired with a short dynamic warm-up. (Marathon Handbook, 2023; One Peloton, 2024). Marathon Handbook+1 After exercise, massage promotes lymph and blood circulation, helps clear metabolic by-products, and can reduce delayed-onset muscle soreness (DOMS)—with some reports suggesting the sooner after training, the better. (Verywell Fit, 2022; PureGym, 2025; Northwich Foot Clinic, 2023). Verywell Fit+2PureGym+2 Pre-workout massage: what to do (and what to skip) Do this -
Keep it light and short (5–10 minutes) on the main muscles you’re about to use. -
Use sweeping, rhythmic strokes to promote circulation without “flattening” muscle tone. -
Pair with a dynamic warm-up (leg swings, A-skips, carioca drills) for an easy transition into work sets. (Marathon Handbook, 2023; One Peloton, 2024). Marathon Handbook+2Marathon Handbook+2 Skip this -
Deep tissue right before training. Evidence shows longer or deeper pre-event massage can blunt explosive performance or reduce high-velocity output—likely by over-relaxing tissue and dampening neural drive. Save deep work for recovery days. (Mine & Nakayama, 2018; Dakić, 2023; Arabaci, 2008). PubMed Central+2PubMed Central+2 Why light beats deep before you lift or sprint Pre-event massage should prime, not fatigue, your muscles. When pressure is too intense, muscle tone and stiffness drop more than you want, which can reduce force production in the short term. (One Peloton, 2024). Peloton Post-workout massage: the recovery booster What it helps -
Soreness: Less DOMS, especially when done soon after exercise. (PureGym, 2025; Verywell Fit, 2022). PureGym+1 -
Circulation & lymph flow: Supports removal of metabolic waste and brings nutrients to the tissue. (Northwich Foot Clinic, 2023; Verywell Fit, 2022). Northwich Foot Clinic+1 -
Range of motion & relaxation: Eases tightness so you move more freely later. (Marathon Handbook, 2023). Marathon Handbook Timing tips Aim for immediately to the same day after training for general workouts. Some endurance events (like marathons) may call for a 24–48 hour wait before deeper work—light recovery work is still OK sooner. (Aescape, 2025). aescape.com Choosing your focus: before vs. after -
Choose pre-workout (light) if your goal is preparation—you want to feel mobile, warm, and ready to move. (Marathon Handbook, 2023; One Peloton, 2024). Marathon Handbook+1 -
Choose post-workout if your goal is recovery—you want to limit soreness, calm the nervous system, and sleep better. (Verywell Fit, 2022; PureGym, 2025). Verywell Fit+1 -
Skip deep tissue right before training; reserve it for rest days or hours after your workout. (Mine & Nakayama, 2018; Dakić, 2023). PubMed Central+1 Massage + Chiropractic Care: a smarter, complementary pairing Massage mainly addresses muscles, fascia, and circulation. Chiropractic care targets joint alignment, spinal mechanics, and the nervous system. Together, they reinforce each other: soft tissues relax so adjustments take more easily, and alignment helps muscles hold their gains. (The Joint, 2025; Link Chiropractic Clinic, 2025; ChiroSports USA, 2025). The Joint Chiropractic+2Link Chiropractic Clinic+2 What to schedule first? It depends on the goal: -
Tight, guarded muscles? A light massage before the adjustment can reduce resistance to care. (Tucson Sports Recovery, 2025). tucsonsportsrecovery.com -
Maintaining alignment? A massage after the adjustment can help tissues adapt and hold. (Tucson Sports Recovery, 2025; The Joint, 2025). tucsonsportsrecovery.com+1 -
Injury recovery or pain management? Before and after (in the same week or split days) is often useful, with pressure tailored to your current phase. (Tucson Sports Recovery, 2025; Maverick Chiropractors, n.d.). tucsonsportsrecovery.com+1 Inside Dr. Alexander Jimenez’s integrative model (El Paso, TX) Dr. Alexander Jimenez, DC, APRN, FNP-BC, leads an El Paso clinic that blends chiropractic care, massage therapy, physical rehabilitation, and functional medicine. His dual-scope training (chiropractic + nurse practitioner) supports a holistic but evidence-driven plan for athletes and people recovering from work, sports, personal, and motor vehicle accidents (MVAs). El Paso, TX Doctor Of Chiropractic Clinical correlations, he emphasizes -
Advanced neuromusculoskeletal imaging when needed (e.g., MRI/CT for disc, ligament, or nerve involvement; EMG for radicular symptoms) to correlate injuries with exam findings. (Jimenez, 2025a; Jimenez, 2025b; Jimenez, 2025c). El Paso, TX Doctor Of Chiropractic+2El Paso, TX Doctor Of Chiropractic+2 -
Objective documentation that supports both medical recovery and legal reporting in personal-injury cases (clear mechanism of injury, imaging, progress metrics, and function). (Jimenez, 2025a; Jimenez, 2025d). El Paso, TX Doctor Of Chiropractic+1 -
Soft-tissue preparation (massage, instrument-assisted, percussive therapy) before or after adjustments, depending on the phase—light for warm-up or moderate for recovery. (Jimenez, 2023; Jimenez, 2022; Jimenez, 2025e). El Paso, TX Doctor Of Chiropractic+2El Paso, TX Doctor Of Chiropractic+2 Common injury paths seen at the clinic -
Work & posture-related strain: Neck/shoulder tightness, mid-back pain, tension headaches. Massage reduces tone; adjustments restore mechanics; targeted rehab improves endurance. (Jimenez, 2025e). El Paso, TX Doctor Of Chiropractic -
Sports injuries: Tendinopathies, muscle strains, and joint restrictions. Imaging and functional testing guide return-to-play; massage aids circulation and ROM. (Jimenez, 2021; Jimenez, 2022). El Paso, TX Doctor Of Chiropractic+1 -
MVAs: Whiplash, soft-tissue sprain/strain, nerve irritation. Chiropractic realigns; massage reduces guarding; precise documentation (imaging + exam) supports claims. (Jimenez, 2025a; Jimenez, 2025d). El Paso, TX Doctor Of Chiropractic+1 Practical playbooks If you lift weights or do HIIT -
Pre-workout (optional): 5–8 minutes of light massage on prime movers (quads, glutes, pecs, lats), then dynamic prep. -
Post-workout: 10–20 minutes of moderate pressure on worked areas. Hydrate, eat, and sleep well. (PureGym, 2025; Verywell Fit, 2022). PureGym+1 -
Avoid: Deep tissue immediately before heavy sets; schedule that on rest days or later that evening. (Mine & Nakayama, 2018). PubMed Central If you run or cycle -
Pre-workout: Brief, light massage to calves, quads, and hips + dynamic drills (A-skips, carioca). -
Post-workout: 10–15 minutes on calves, quads, glutes, and back. Longer deep work 24–48 hours after big events. (Marathon Handbook, 2023; Aescape, 2025). Marathon Handbook+1 If you’re sore from a long day or travel What type of massage when? -
Light Swedish/relaxation massage: Best before workouts (short) or after workouts (longer) to support blood flow and nervous-system calm. (Verywell Fit, 2022; One Peloton, 2024). Verywell Fit+1 -
Deep tissue/sports massage: Best after training or on rest days to address knots/adhesions without blunting performance. (Mine & Nakayama, 2018; Dakić, 2023). PubMed Central+1 -
Percussive therapy: Useful post-workout to maintain circulation and reduce soreness. (Jimenez, 2022). El Paso, TX Doctor Of Chiropractic How chiropractic enhances your results -
Alignment & joint mechanics: Adjustments reduce joint restrictions so muscles don’t have to “brace” as hard. That extends the benefit of massage. (The Joint, 2025; Link Chiropractic Clinic, 2025). The Joint Chiropractic+1 -
Nervous system regulation: Adjustments can normalize input/output signaling; massage promotes a parasympathetic “rest & digest” state. Together, you often feel less pain and more mobility. (The Joint, 2025). The Joint Chiropractic -
Program design: Clinics often alternate sessions (massage → adjustment or adjustment → massage) based on your phase: acute pain, subacute training, or maintenance. (Tucson Sports Recovery, 2025; ChiroSports USA, 2025). tucsonsportsrecovery.com+1 Safety tips & when to wait -
Avoid massage over open wounds, infection, fever, uncontrolled hypertension, active DVT, or in areas of acute trauma. -
For post-event marathons/ultras, you might delay deep tissue 24–48 hours; opt for light recovery work sooner. (Aescape, 2025). aescape.com -
If you have new numbness, weakness, or severe pain, see a licensed clinician first for evaluation—imaging may be appropriate. (Jimenez, 2025a; 2025b). El Paso, TX Doctor Of Chiropractic+1 Simple scheduling templates (mix and match) Performance day (strength or sprints) Deload or rest day (recovery focus) Chiro-massage integration (El Paso model) -
Phase 1 (acute): adjustment → light massage (to calm guarding). -
Phase 2 (subacute): massage → adjustment (to improve tissue compliance). -
Phase 3 (maintenance): alternate weekly; add percussive therapy/rehab as needed. (The Joint, 2025; Jimenez, 2022; Tucson Sports Recovery, 2025). The Joint Chiropractic+2El Paso, TX Doctor Of Chiropractic+2 Key takeaways -
Before you train, use light, short massage to prime your body; skip deep tissue right before lifting, sprinting, or power work. (Mine & Nakayama, 2018; Dakić, 2023). PubMed Central+1 -
After you train, massage is your recovery multiplier—circulation up, soreness down, relaxation up. (Verywell Fit, 2022; PureGym, 2025). Verywell Fit+1 -
Massage + chiropractic treat soft tissue + joints together, often giving faster, longer-lasting relief—especially when care is personalized and documentation is clear (vital in injury cases). (The Joint, 2025; Jimenez, 2025a; 2025d). The Joint Chiropractic+2El Paso, TX Doctor Of Chiropractic+2 Medical note & disclaimer This guide is educational and not a substitute for personalized medical care. If you have an injury, new numbness or weakness, fever, infection, blood-clot risk, or any serious condition, seek professional evaluation before massage or exercise. References Northwich Foot Clinic. (2023, October 5). Should I get a sports massage before or after a workout? https://northwichfootclinic.co.uk/sports-massage-before-after-workout/ Northwich Foot Clinic PureGym. (2025). Is it best to get a massage before or after a workout? https://www.puregym.com/us/blog/is-it-best-to-get-a-massage-before-or-after-a-workout PureGym Marathon Handbook. (2023, April 24). Should you get a massage before or after a workout? https://marathonhandbook.com/massage-before-or-after-a-workout/ Marathon Handbook One Peloton. (2024, September 6). Should you massage muscles before or after a workout? https://www.onepeloton.com/blog/massage-before-or-after-workout Peloton Verywell Fit. (2022, October 28). How to use massage for post-workout recovery. https://www.verywellfit.com/massage-after-exercise-may-speed-muscle-recovery-3436572 Verywell Fit Prime Massage Chairs. (2025, January 24). Should I workout before or after massage? https://www.primemassagechairs.com/blogs/news/should-i-workout-before-or-after-massage Prime Massage Chairs Delta Valley Health Club. (2025, January 21). Can I do strength training after a massage? https://deltavac.com/2025/01/21/can-i-do-strength-training-after-a-massage/ Delta Valley Health Club Thai Kosai Massage. (n.d.). Massage for marathon preparation. https://www.thai-kosai.com/massage-blog/massage-marathon-prep/ Thai Massage | NeuLife Chiropractic. (2024, September 24). Unlocking wellness: The role of massage therapy in chiropractic care. https://neulifechiro.com/role-of-massage-therapy-in-chiropractic-care/ Neu Life Chiropractic Maverick Chiropractors. (n.d.). Power of combining therapeutic massage with chiropractic care. https://maverickchiros.com/power-of-combining-therapeutic-massage-with-chiropractic-care/ Maverick Chiropractic Islip Chiropractic. (2024, December 30). Guide to the powerful combo of massage and chiropractic care. https://www.islipchiropractic.com/post/guide-to-the-powerful-combo-of-massage-and-chiropractic-care Islip Chiropractic Hanson Chiropractic. (n.d.). Benefits of massage and chiropractic together. https://hansonchiropractic.net/benefits-of-massage-and-chiropractic-together/ Hanson Chiropractic and Massage Clinic Yoder Chiropractic Center. (2025, August 8). How does professional chiropractic care complement massage therapy for optimal results? https://www.yoderchiropracticcenter.com/blog/how-does-professional-chiropractic-care-complement-massage-therapy-for-optimal-results/ yoderchiropracticcenter.com Tucson Sports Recovery. (2025, March 14). Should I get a massage before or after a chiropractic adjustment? https://www.tucsonsportsrecovery.com/should-i-get-a-massage-before-or-after-a-chiropractic-adjustment tucsonsportsrecovery.com The Joint Chiropractic. (2025, August 5). Is it good to combine massage therapy with chiropractic care? https://www.thejoint.com/2025/08/05/chiropractic-care-and-massage-therapy The Joint Chiropractic Link Chiropractic Clinic. (2025). Combined benefits of massage therapy and chiropractic care. https://linkchiropracticclinic.com/combined-benefits-of-massage-therapy-and-chiropractic-care/ Link Chiropractic Clinic ChiroSports USA. (2025, May 17). Can you combine massage therapy and chiropractic care? https://www.chirosportsusa.com/blog/posts/can-you-combine-massage-therapy-and-chiropractic-care chirosportsusa.com Mine, K., & Nakayama, T. (2018). Is pre-performance massage effective to improve running performance? Journal of Physical Therapy Science. https://pmc.ncbi.nlm.nih.gov/articles/PMC6159489/ PubMed Central Dakić, M., et al. (2023). The effects of massage therapy on sport and exercise performance and recovery. Sports, 11(6), 110. https://www.mdpi.com/2075-4663/11/6/110 PubMed Central Arabaci, R. (2008). Acute effects of pre-event lower limb massage on explosive and high-speed motor capacities and flexibility. Journal of Sports Science & Medicine. https://www.jssm.org/jssm-07-549.xml%3EFulltext Journal of Sports Science and Medicine Aescape. (2025, March 4). Massage before or after a marathon? https://www.aescape.com/news/massage-before-or-after-marathon aescape.com Dr. Alex Jimenez. (2025a). MVA injuries and their impact on mobility. https://dralexjimenez.com/mva-injuries-and-their-impact-on-mobility/ El Paso, TX Doctor Of Chiropractic Dr. Alex Jimenez. (2025b). Durable medical equipment solutions for MVA injuries. https://dralexjimenez.com/durable-medical-equipment-solutions-for-mva-injuries/amp/ El Paso, TX Doctor Of Chiropractic Dr. Alex Jimenez. (2025c). Physical therapy for MVAs: Overcoming injuries effectively. https://dralexjimenez.com/physical-therapy-for-mvas-overcoming-injuries-effectively/ El Paso, TX Doctor Of Chiropractic Dr. Alex Jimenez. (2025d). Post-automobile accident recovery and healing foods. https://dralexjimenez.com/post-automobile-accident-recovery-and-healing-foods/ El Paso, TX Doctor Of Chiropractic Dr. Alex Jimenez. (2023). Percussive massage therapy: Functional chiropractor. https://dralexjimenez.com/percussive-massage-therapy-functional-chiropractor/ El Paso, TX Doctor Of Chiropractic Dr. Alex Jimenez. (2022). Using a percussive massager correctly. https://dralexjimenez.com/using-a-percussive-massager-correctly-ep-chiropractic-clinic/ El Paso, TX Doctor Of Chiropractic Dr. Alex Jimenez. (2021). Chiropractic sports massage for injuries, sprains, and strains. https://dralexjimenez.com/chiropractic-sports-massage/ El Paso, TX Doctor Of Chiropractic General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Discover the advantages of chiropractic care for achieving balance, flexibility, and pain relief in your body from muscle imbalances. Introduction Muscle imbalances occur when one muscle or muscle group is stronger, weaker, or less flexible than its opposing group, leading to improper movement patterns, posture issues, and an increased risk of injury. These imbalances can affect both the upper and lower extremities, contributing to pain, reduced mobility, and chronic conditions if left unaddressed. Fortunately, nonsurgical treatments like chiropractic care, targeted exercises, massage therapy, acupuncture, and integrative medicine can effectively address muscle imbalances, promote the body’s natural healing process, and prevent long-term complications. This comprehensive guide examines the causes of muscle imbalances, their clinical implications, the role of chiropractic care in treatment, and provides practical exercises to address these issues at home or in the gym. What Are Muscle Imbalances? Muscle imbalances develop when opposing muscle groups, such as the quadriceps and hamstrings or the chest and upper back muscles, have unequal strength, flexibility, or activation. This imbalance disrupts the body’s natural alignment and movement, leading to compensatory patterns that can cause pain and injury. For example, tight hip flexors paired with weak glutes can tilt the pelvis, contributing to lower back pain. Similarly, overdeveloped chest muscles and weak upper back muscles may lead to forward shoulder posture, a hallmark of upper crossed syndrome. According to Dr. Alex Jimenez, a chiropractor and family nurse practitioner in El Paso, Texas, muscle imbalances are a common underlying factor in many musculoskeletal complaints seen in his practice. “When muscles are not working in harmony, the body compensates, which can lead to strain, joint dysfunction, and chronic pain,” Dr. Jimenez explains (Jimenez, n.d.). His integrative approach combines chiropractic adjustments, targeted exercises, and therapeutic modalities such as massage to restore balance and function. Causes of Muscle Imbalances Several factors contribute to the development of muscle imbalances, affecting both the upper and lower extremities. Understanding these causes is crucial for preventing and effectively treating the condition. 1. Improper Exercise Routines Many exercise programs focus on specific muscle groups, such as the chest or quadriceps, without balancing them with opposing muscles, like the upper back or hamstrings. For instance, overemphasizing bench presses without incorporating rows can lead to stronger chest muscles and weaker back muscles, which can contribute to forward shoulder posture (Jimenez, n.d.). A study on scapular stabilization exercises highlighted that imbalanced exercise routines can exacerbate upper crossed syndrome, characterized by forward head posture and rounded shoulders (Nitayarak et al., 2021). 2. Sedentary Lifestyle and Poor Posture Prolonged sitting, especially with poor posture, can cause certain muscles to become tight or weak. For example, sitting for long periods shortens the hip flexors and weakens the glutes, leading to pelvic tilt and lower back pain. Similarly, slouching at a desk can weaken the upper back muscles and tighten the chest, contributing to forward head posture (Jimenez, n.d.). 3. Repetitive Movements Repetitive tasks, such as typing or lifting, can overwork specific muscle groups while underutilizing others. Athletes who perform repetitive motions, such as runners or cyclists, may develop imbalances between the quadriceps and hamstrings, which increases the risk of injuries like hamstring strains (Silvers-Granelli et al., 2021). 4. Injuries and Compensation Injuries often lead to compensatory movement patterns that create imbalances. For example, a sprained ankle may cause an individual to favor one leg, weakening the muscles on the injured side and overworking the muscles on the opposite side. This compensation can persist even after the injury heals, leading to chronic imbalances (Jimenez, n.d.). 5. Anatomical and Structural Factors Structural issues, such as scoliosis or glenoid retroversion, can contribute to muscle imbalances. A study in a fetal lamb model suggested that muscle imbalances in the abdominal wall may lead to scoliosis, indicating that structural abnormalities can perpetuate uneven muscle development (Kawaguchi et al., 2021). Similarly, posterior humeral head subluxation has been linked to imbalances in the rotator cuff muscles (Mitterer et al., 2021). 6. Systemic Factors Chronic conditions like chronic obstructive pulmonary disease (COPD) can lead to muscle dysfunction due to deconditioning, inflammation, or oxidative stress. These systemic factors can weaken both respiratory and peripheral muscles, exacerbating imbalances (Gea et al., 2013). 7. Myofascial Trigger Points Myofascial trigger points (MTrPs), also known as “knots” in muscles, can contribute to imbalances by altering muscle activation patterns. A study found that MTrPs in the upper trapezius muscle were associated with increased electromyographic activity in the masticatory muscles, indicating a broader impact on the musculoskeletal system (Ginszt et al., 2022). General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Understand the benefits of exercises with chiropractic care which provides for muscle pain, enhancing both recovery and mobility. Introduction Muscle pain is like that one friend who shows up uninvited and overstays their welcome—whether it’s from sitting too long at a desk, getting rear-ended in El Paso traffic, or sleeping in a position that makes you question your life choices. For many, it’s not just a one-time annoyance but a chronic issue tied to lifestyle, environmental factors, or conditions like pain syndromes that mimic musculoskeletal issues. The good news? Combining chiropractic care with exercises like CrossFit and weight training can be a game-changer for managing muscle pain. In this guide, we’ll explore why this combo works, how it strengthens your muscles, and why Dr. Alexander Jimenez, DC, APRN, FNP-BC, a leading chiropractor in El Paso, is a go-to expert for personal injury cases and pain relief. Grab a comfy seat (preferably not that creaky office chair) and let’s dive in! Understanding Musculoskeletal Pain and Environmental Triggers Musculoskeletal pain hits your muscles, bones, joints, and connective tissues like a bad plot twist in your day. It’s not just about overexertion at the gym—environmental factors sneak in like uninvited guests at a barbecue. Poor posture from hunching over a laptop, repetitive motions at work (like typing faster than a caffeinated squirrel), or stress from navigating El Paso’s rush-hour traffic can strain your musculoskeletal system. Add a sedentary lifestyle, and you’ve got a recipe for aches that linger like a catchy jingle you can’t unhear. Environmental factors are major players. Sitting for hours in a chair that’s as supportive as a wet paper towel can lead to tight hip flexors, a cranky lower back, and neck pain that feels like you’re carrying a backpack full of bricks. Cold or damp weather—even in sunny El Paso—can make joints creak like an old wooden floor. Stress, meanwhile, tightens muscles faster than you can say “deadline.” Pain-like symptoms, such as those caused by fibromyalgia or other chronic conditions, can mimic musculoskeletal pain, making diagnosis tricky. These conditions often overlap with musculoskeletal issues, increasing pain sensitivity and reducing mobility (Jimenez, 2025a). This complexity calls for a multifaceted approach, which is where chiropractic care and exercise shine. References Why Chiropractic Care Works for Muscle Pain Chiropractic care is like giving your spine a motivational speech—it realigns joints, calms irritated nerves, and tells your muscles to chill out. Chiropractors use spinal adjustments, soft tissue therapy, and other techniques to restore alignment, which can ease pain from misaligned joints or tense muscles. It’s like hitting the reset button on your body’s framework, minus the tech support hold music. The clinical rationale for chiropractic care is rooted in addressing pain at its source, rather than merely masking it. Misaligned vertebrae can pinch nerves, causing muscle tension and pain that spreads like gossip. Adjustments enhance joint mobility, reduce inflammation, and improve blood flow, thereby facilitating faster muscle recovery (Jimenez, 2025b). Research shows that non-surgical treatments like chiropractic care are cost-effective and yield better outcomes for musculoskeletal disorders compared to physician-first approaches (Ojha et al., 2021). General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Find out how calisthenics and chiropractic care can enhance your workouts and promote better body mechanics and health. Introduction Musculoskeletal pain—whether it’s a nagging ache in your lower back, a stiff neck from too many hours hunched over a laptop, or sore joints after a long day—can feel like an unwelcome guest who overstays their welcome. If you’ve ever tried to “walk it off” only to realize your body is staging a full-blown protest, you’re not alone. Millions of people deal with musculoskeletal pain daily, and it can range from mildly annoying to downright debilitating. But here’s the good news: combining chiropractic care with calisthenics, a bodyweight exercise method rooted in ancient Greece, offers a powerful, natural way to tackle this pain and reduce overlapping risk factors. In this comprehensive guide, we’ll explore the clinical rationale behind this dynamic duo, spotlight the expertise of Dr. Alexander Jimenez, DC, APRN, FNP-BC, a leading practitioner in El Paso, Texas, and share beginner-friendly calisthenic exercises you can do at home or in the gym. Plus, we’ll sprinkle in a bit of humor to keep things light—because nobody wants to read a 5,000-word snooze-fest! Understanding Musculoskeletal Pain and Its Overlapping Risk Profiles Musculoskeletal pain affects the bones, muscles, ligaments, tendons, and nerves in the body. It is like your body’s way of saying, “Hey, something is not right here!” Common culprits include lower back pain, neck pain, sciatica, and joint discomfort from conditions like arthritis or injuries. According to research, chronic musculoskeletal pain is a major global health issue, impacting a person’s quality of life while increasing the risk of other health problems (Cimmino et al., 2011). What Are Overlapping Risk Profiles? Overlapping risk profiles refer to the interconnected factors that make musculoskeletal pain worse or more likely to persist. Think of it like a bad party where uninvited guests keep showing up. These risk factors include: - Sedentary Lifestyle: Sitting for long hours can weaken muscles and stiffen joints, making pain more likely.
- Poor Posture: Slouching at your desk or while scrolling on your phone can strain your spine and neck.
- Injuries: From car accidents to sports mishaps, injuries can disrupt musculoskeletal alignment and function.
- Stress: Psychological stress can tighten muscles, exacerbating pain.
- Obesity: Excess weight puts pressure on joints and muscles, amplifying discomfort.
- Neuroinflammatory Conditions: Inflammation from conditions like arthritis can worsen pain and limit movement.
These factors do not just add up—they multiply, creating a vicious cycle where pain leads to less movement, which leads to more pain. The good news? Chiropractic care and calisthenics can break this cycle by addressing both the symptoms and the root causes. Why Chiropractic Care and Calisthenics? Chiropractic care, led by experts like Dr. Alexander Jimenez, focuses on restoring proper alignment to the spine and joints, reducing nerve irritation, and improving overall function. Calisthenics, on the other hand, strengthens muscles, boosts flexibility, and enhances mobility using just your body weight—no fancy gym equipment required. Together, they are like peanut butter and jelly: each is great on its own, but when combined, they are a game-changer. References The Clinical Rationale: Why This Combo Works Dr. Alexander Jimenez, a dual-licensed chiropractor and board-certified Family Nurse Practitioner (FNP-BC) based in El Paso, Texas, is a trailblazer in integrative healthcare. His practice at Injury Medical & Chiropractic Clinic combines chiropractic adjustments with functional medicine to address musculoskeletal pain holistically. Let us dive into the science behind why chiropractic care and calisthenics are a match made in pain-relief heaven. Chiropractic Care: Restoring Balance Chiropractic care focuses on the musculoskeletal and nervous systems, particularly the spine. Misalignments, or subluxations, can irritate nerves, causing pain and dysfunction. Dr. Jimenez uses advanced imaging (like MRI and CT scans) and diagnostic evaluations to pinpoint these issues. His “dual-scope” approach—combining chiropractic techniques with medical diagnostics—ensures precise, customized treatment plans tailored to each patient’s needs (El Paso Back Clinic, 2025). For example, a patient with sciatica (pain radiating from the lower back down the leg) might have a herniated disc compressing a spinal nerve. Chiropractic adjustments can realign the spine from misalignment, reducing pressure on the nerve, while manual therapies like spinal decompression ease pain and promote healing. A 2020 study found that combining manual therapy with exercise significantly reduces pain and disability in patients with nonspecific neck pain (Hidalgo et al., 2020). Calisthenics: Building Strength and Resilience Calisthenics, derived from the Greek words “kallos” (which means beauty) and “sthenos” (which means strength), is a form of exercise that uses bodyweight exercises to build muscle, improve flexibility, and enhance endurance. Unlike weightlifting, which can sometimes strain joints if done improperly, calisthenics is low-impact and adaptable to all fitness levels. A 2022 study showed that calisthenics can improve neuromuscular function, reducing the negative effects of sedentary time on muscle health (Schoenfeld et al., 2022). By strengthening core muscles and improving posture, calisthenics addresses risk factors like weak muscles and poor alignment. For instance, exercises like planks strengthen the core, thus supporting the spine and reducing lower back pain. A 2021 network meta-analysis found that exercises targeting core stability, like those in calisthenics, are highly effective for chronic low back pain (Owen et al., 2021). General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Why Massage Matters After a Crash Motor vehicle accidents (MVAs) are a leading cause of musculoskeletal injuries. These collisions can result in a variety of issues, including whiplash, back pain, nerve compression, spinal misalignments, and emotional trauma. While emergency medical treatment is crucial, many individuals also benefit from ongoing therapy to achieve a full recovery. One powerful tool in this recovery journey is massage therapy. Massage therapy isn't just for relaxation. It's a medically backed method that can reduce inflammation, improve mobility, manage pain, and support mental health. When combined with chiropractic care and integrative medicine, massage therapy can help address both the physical and emotional impact of a car accident. Dr. Alexander Jimenez, a chiropractor and nurse practitioner based in El Paso, Texas, integrates massage therapy into a broader rehabilitation strategy. He specializes in dual-scope treatment—meaning he can diagnose and treat both musculoskeletal and neurological injuries, as well as manage the legal documentation required for personal injury cases. According to Dr. Jimenez, “Massage therapy is often underestimated. It’s a cornerstone in reducing soft tissue inflammation, restoring function, and promoting parasympathetic healing after traumatic injury” (Jimenez, n.d.). CureZone Physiotherapy, n.d. Common Injuries After a Motor Vehicle Accident MVAs can cause more than just bumps and bruises. Many survivors experience complex injuries, some of which may not show symptoms until days or weeks later. The most common types of post-accident injuries include: -
Whiplash: Caused by the rapid back-and-forth movement of the neck, often leading to neck pain, stiffness, and headaches. -
Muscle Strain and Spasms: Often in the shoulders, neck, and back. -
Nerve Compression: Herniated discs or spinal misalignment can put pressure on nearby nerves, leading to pain, tingling, or numbness. -
Spinal Misalignments: Displacement of spinal joints (subluxations) can contribute to chronic pain and reduced mobility. -
Post-Traumatic Stress: Accidents can cause significant emotional distress that manifests as anxiety, sleep issues, or depression. These injuries may require a combination of physical therapy, chiropractic care, and massage therapy for full recovery. MVAMVP, n.d. The Science Behind Massage Therapy Massage therapy has been studied for its benefits in treating musculoskeletal and soft tissue injuries. Research shows that massage therapy: -
Increases blood flow and oxygenation to injured tissues -
Reduces inflammation and scar tissue buildup -
Promotes lymphatic drainage to decrease swelling -
Releases muscle tension and trigger points -
Activates the parasympathetic nervous system to promote relaxation One systematic review found that massage therapy had moderate effects in managing neck pain and post-traumatic soreness, especially when combined with exercise and chiropractic care (Yuan et al., 2015). Massage also helps reduce cytokines (inflammatory chemicals) released after tissue injury, which aids in easing pain and promoting faster recovery (Crane et al., 2012). Types of Massage Used After a Car Accident Different massage techniques are recommended depending on the injury and the stage of recovery. Here's a look at the most effective types: 1. Swedish Massage This gentle form utilizes long strokes and kneading techniques to promote relaxation and enhance circulation. It’s ideal for people experiencing anxiety or emotional trauma after an accident. 2. Deep Tissue Massage Targets deeper layers of muscle and connective tissue. It's helpful for chronic muscle tension, trigger points, or whiplash pain. Rocky Mountain Accident Care, n.d. 3. Trigger Point Therapy Focuses on specific tight spots in muscle tissue that refer pain to other areas. Commonly used for whiplash and shoulder injuries. EG Healthcare, n.d. 4. Myofascial Release Gentle pressure is applied to fascia—the connective tissue around muscles—to relieve stiffness and pain. 5. Neuromuscular Massage Combines deep pressure with stretching to treat nerve compression, especially useful in cases involving pinched nerves or sciatica. Eastbridge Massage, 2021 How Massage Eases Emotional Trauma Massage doesn't just heal the body—it calms the mind. Many accident survivors experience lingering emotional effects such as: Massage activates the parasympathetic nervous system, helping lower cortisol (the stress hormone) and increase serotonin and dopamine. This hormonal shift encourages relaxation and emotional healing. In fact, trauma-informed massage therapy has shown benefits for PTSD, helping patients feel safe and grounded while processing difficult emotions (Boulder Sports Clinic, n.d.). Dr. Alexander Jimenez’s Clinical Approach Dr. Alexander Jimenez, DC, APRN, FNP-BC, practices a unique dual-discipline model in El Paso. As both a licensed chiropractor and family nurse practitioner, Dr. Jimenez combines diagnostic imaging, orthopedic evaluation, and integrative rehabilitation—including massage therapy. Here’s how his approach stands out: -
Dual Diagnosis: He evaluates both orthopedic and neurological injury patterns, including spinal misalignment, disc herniation, nerve impingement, and inflammation. -
Advanced Imaging: MRI, CT, and digital motion X-rays help track soft tissue damage and healing progress. -
Integrated Care: Combines chiropractic, massage, rehabilitative exercises, and emotional support strategies. -
Legal Support: Prepares injury documentation for personal injury lawyers, ensuring patient care aligns with case timelines and medical evidence requirements. According to Dr. Jimenez, “Massage plays a foundational role in reducing residual inflammation, breaking up adhesions, and restoring neuromuscular balance post-MVA” (Jimenez, n.d.). Combining Massage Therapy with Chiropractic and Integrative Medicine Massage therapy is especially effective when combined with other rehabilitative strategies such as chiropractic care, acupuncture, physical therapy, and nutrition counseling. This integrative approach can: -
Enhance spinal alignment by relaxing surrounding muscles -
Improve outcomes for nerve injuries like sciatica or pinched nerves -
Accelerate tissue healing through improved circulation and reduced inflammation -
Help the body return to homeostasis, or natural balance, more quickly Dr. Jimenez often begins with diagnostic imaging to assess spinal integrity and nerve involvement, then works with licensed massage therapists to target areas of dysfunction. “Once we understand where the injury is rooted—be it a disc bulge, ligament tear, or soft tissue fibrosis—we can tailor the massage to amplify healing,” he explains (Jimenez, n.d.). Biotone, n.d. Addressing Whiplash: A Common MVA Injury Whiplash is one of the most frequent injuries from car accidents, especially rear-end collisions. It occurs when the neck is suddenly forced backward and then forward, stretching muscles, ligaments, and nerves. Common symptoms include: Massage therapy for whiplash often involves gentle strokes and deep tissue techniques to relieve tightness and pain. Techniques like trigger point therapy and myofascial release are especially helpful for chronic whiplash syndromes. Sage Bodyworks Seattle, n.d. Massage Envy, n.d. PhysioFlow, n.d. The Legal Value of Massage in Personal Injury Cases One overlooked aspect of massage therapy is its value in legal documentation for personal injury claims. Insurance companies and attorneys often seek proof of medical necessity and progress. Massage therapy can provide: -
Evidence of ongoing pain and treatment -
Documented reduction in symptoms over time -
Support for lost wages or limited mobility -
Validation of emotional and psychological impact Dr. Jimenez collaborates with legal teams to ensure that therapeutic notes, treatment plans, and outcomes are properly documented to support a patient’s case. His dual-scope licensure allows him to act as both a medical provider and a chiropractic care expert in court-related matters. East Bay Chiropractic, n.d. Emotional Healing After a Traumatic Accident Healing the body is only half the journey after a traumatic event like a car accident. Emotional recovery is just as important. Many survivors suffer from: -
Anxiety when driving -
Sleep disturbances or insomnia -
Loss of appetite or emotional numbness -
Depression or survivor’s guilt Massage helps regulate the nervous system and can provide a safe, grounding experience that allows individuals to reconnect with their bodies. This tactile form of care can restore trust, soothe trauma, and facilitate the processing of emotional pain. According to trauma specialists, combining massage with talk therapy, mindfulness, and yoga leads to improved outcomes in post-MVA recovery (Primary Rehab, n.d.). Galiny Accident Recovery, n.d. How Often Should You Receive Massage Therapy After an Accident? There is no one-size-fits-all answer. Depending on the severity of the injury, massage therapy may be recommended: -
2–3 times per week in the early stages of injury -
Once weekly for chronic conditions -
Monthly or as needed for maintenance and emotional support Treatment duration can range from a few weeks to several months. Dr. Jimenez stresses the importance of consistent follow-up, stating: “Early intervention with massage therapy can prevent long-term complications and reduce dependency on medication” (Jimenez, n.d.). MindBodyMed Seattle, n.d. Conclusion: Whole-Person Healing After a Car Accident Motor vehicle accidents can impact every aspect of a person’s life—physically, emotionally, and financially. Massage therapy is a powerful, non-invasive way to support recovery across all these areas. When integrated with chiropractic care, medical evaluation, and mental health support, massage therapy can accelerate healing, enhance outcomes, and even strengthen personal injury claims. Dr. Alexander Jimenez’s dual approach—blending physical rehabilitation with emotional insight and legal clarity—provides a roadmap for true, whole-person recovery. Whether you're suffering from whiplash, nerve pain, or anxiety, massage therapy can help restore not just your body, but your peace of mind. Denver Chiropractic, n.d. Understanding Long-Lasting Injuries - El Paso, TX References General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction Motor vehicle accidents (MVAs) are a leading cause of musculoskeletal injuries, ranging from mild whiplash to severe spinal trauma. The aftermath often includes chronic pain, reduced mobility, and impaired posture. While emergency care addresses immediate threats, the long-term effects frequently require comprehensive rehabilitation. Physical therapy plays a crucial role in restoring function, alleviating pain, and preventing further injury. According to Texas Physical Therapy Specialists, each patient’s recovery is unique, requiring personalized therapeutic programs tailored to their specific needs and injuries (Texas Physical Therapy Specialists, n.d.). The Hidden Impact of Motor Vehicle Accidents Injuries from car accidents aren’t always visible. Even without broken bones, individuals may suffer from soft tissue damage, nerve impingement, and ligament strain. These hidden injuries can lead to chronic pain if not properly treated. Whiplash, one of the most common accident-related conditions, can result in significant cervical spine dysfunction and muscular imbalances (Breakthrough Physical Therapy, n.d.). Dr. Alexander Jimenez, DC, APRN, FNP-BC, notes that seemingly minor collisions often result in postural changes, joint instability, and persistent discomfort that may not manifest for days or weeks (Jimenez, 2024). Common Injuries Requiring Physical Therapy Physical therapists address a wide range of injuries following motor vehicle accidents (MVAs). These include: -
Whiplash and cervical spine dysfunction -
Herniated or bulging discs -
Lower back pain -
Muscle sprains and ligament strains -
Joint instability and misalignment -
Nerve compression syndromes, including sciatica and thoracic outlet syndrome According to OneRehab, these injuries can reduce a patient’s ability to function and may delay their return to daily activities unless treated with a structured physical therapy plan (OneRehab, n.d.). How Physical Therapy Aids Recovery Physical therapy restores mobility and function by focusing on both healing and strengthening. It promotes blood flow to injured tissues, reduces inflammation, and improves neuromuscular coordination. For patients in El Paso, Dr. Jimenez utilizes a dual-scope approach, integrating chiropractic adjustments with rehabilitative exercises to ensure comprehensive musculoskeletal recovery (Jimenez, 2024). As noted by Bay State Physical Therapy, customized PT regimens help patients avoid long-term issues such as chronic pain and re-injury (Bay State Physical Therapy, n.d.). Stretching and Flexibility Restoration After an accident, soft tissues often become tight and inflamed. Stretching exercises are essential for improving flexibility and relieving stiffness. According to Sports Physical Therapy Centers, early gentle stretching can enhance circulation and prepare the muscles for more demanding movements (Sports PT Centers, n.d.). Dr. Jimenez recommends progressive flexibility routines, starting with static stretches and advancing to dynamic stretches, to avoid muscle guarding and further tissue damage (Jimenez, 2024). Range-of-Motion and Postural Exercises Restricted movement in the neck, back, and limbs is a common complaint following an accident. Range-of-motion (ROM) exercises help restore joint mobility. These include: Postural training is also vital, especially for patients with forward head posture or pelvic tilting. As discussed by Synergy Rehab, correcting posture through targeted exercises can reduce spinal strain and improve breathing efficiency (Synergy Rehab, n.d.). Strengthening and Core Stability Strengthening exercises rebuild muscle integrity and support injured joints. Core-focused training enhances spinal stability, especially in the lumbar and cervical areas. Functional training methods, like those used at Release Physical Therapy, incorporate multi-joint, multi-muscle movements to restore strength, coordination, and balance (Release PT, n.d.). Patients recovering from back pain benefit significantly from exercises like: -
Pelvic tilts -
Bird-dog extensions -
Resistance band rowing Dr. Jimenez emphasizes the importance of integrating core training early in recovery to prevent re-injury and facilitate spinal alignment (Jimenez, 2024). Pain Relief Techniques and Modalities To manage pain and inflammation, physical therapists use modalities such as: Rocky Mountain Physical Therapy reports that these techniques reduce nerve sensitivity and support tissue healing when used in conjunction with exercise (Rocky Mountain URPT, n.d.). Dry needling, as offered by Benchmark Physical Therapy, has also been shown to be effective in releasing myofascial trigger points and reducing pain (Benchmark PT, n.d.). Manual Therapy and Joint Mobilization Manual therapy techniques, including myofascial release and joint mobilization, target deep-seated tension and realign dysfunctional joints. Apex Orthopedic & Sports Nutrition notes that these hands-on methods enhance joint mechanics, reduce muscular adhesions, and improve circulation (Apex OSN, n.d.). Dr. Jimenez’s dual-scope license allows him to combine joint mobilization with chiropractic manipulation, optimizing outcomes for MVA victims. This integration bridges the gap between traditional physical therapy (PT) and holistic care (Jimenez, 2024). Functional and Aerobic Rehabilitation As the patient regains mobility, the next phase involves restoring endurance and functionality. Texas Physical Therapy Specialists encourage incorporating aerobic activity, such as light treadmill walking, aquatic therapy, or cycling, to promote cardiovascular health and oxygenate healing tissues (Texas Physical Therapy Specialists, n.d.). Functional tasks, such as sit-to-stand transitions, step-ups, and reaching exercises, mimic real-life movements, preparing patients to resume their daily activities with confidence. Neuromuscular and Balance Reeducation Accidents often impair balance and coordination. Neuromuscular training helps patients retrain their nervous systems. Techniques include: According to Breakthrough Physical Therapy, this reeducation helps prevent falls and enhances overall motor control (Breakthrough PT, n.d.). Dr. Jimenez regularly assesses proprioception and vestibular function to develop balanced neuromuscular rehabilitation protocols (Jimenez, 2024). El Paso Case Study: Dr. Alexander Jimenez’s Dual-Scope Approach Dr. Alexander Jimenez stands out as a dual-licensed Doctor of Chiropractic and Family Nurse Practitioner, specializing in personal injury care in El Paso. His clinic uses advanced diagnostic imaging, orthopedic assessments, and integrative physical therapy to address pain, nerve damage, joint dysfunction, and postural misalignments. His unique treatment approach integrates traditional chiropractic techniques with evidence-based PT protocols, offering a customized path to recovery for MVA victims. His experience allows him to correlate physical findings with legal documentation—an essential aspect in personal injury claims (Jimenez, 2024). Advanced Imaging, Legal Needs & Clinical Correlation In personal injury cases, establishing a clinical correlation between physical findings and imaging results is crucial. Dr. Jimenez uses digital motion X-rays, MRI, and musculoskeletal ultrasound to validate diagnoses and guide therapy. This also supports legal documentation in cases involving insurance and court claims. Through precise diagnostic assessments and dual licensure, Dr. Jimenez ensures patients receive ethical, holistic care while fulfilling the evidentiary needs of personal injury cases. His methodology is widely trusted by legal professionals and injury recovery teams across El Paso (Jimenez, 2024). Conclusion: Empowering Recovery with Personalized Care Recovery from a motor vehicle accident requires more than rest—it demands a structured, personalized rehabilitation plan. Physical therapy plays a central role in restoring function, alleviating pain, and preventing chronic musculoskeletal complications. Incorporating expert guidance from dual-licensed providers like Dr. Alexander Jimenez ensures that treatment not only addresses physical injuries but also supports legal and long-term wellness goals. Whether through stretching, strengthening, manual therapy, or functional training, PT helps MVA victims return to their lives stronger and more resilient. References General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Learn how calisthenics can enhance strength and endurance through simple yet effective bodyweight movements. Introduction Many individuals, when their schedules and routines become hectic, can lead to the development of musculoskeletal disorders. From low back pain to muscle imbalances, it can affect anyone at any age; treatment is necessary when individuals experience overlapping risk profiles. When people are dealing with musculoskeletal disorders, many start to seek treatment to reduce the musculoskeletal pain in their bodies. Depending on the severity, many would go for surgical treatment to reduce the overlapping risk profiles. In contrast, others may try non-surgical treatment to relieve the pain within the musculoskeletal system. Since musculoskeletal disorders are amongst the leading causes of disability, non-surgical treatments can provide relief to the referred pain in the body while being cost-effective and safe. Non-surgical treatments like chiropractic care can help address musculoskeletal issues through spinal alignment and stretching out the affected muscles. However, for long-term recovery, chiropractors will work on a customized treatment plan that requires active movement exercises to help rebuild muscle strength and restore mobility function, hence where calisthenics comes into play. What is Calisthenics? Also known as bodyweight training, calisthenics utilizes the person’s body to build muscle strength and increase flexibility while enhancing neuromuscular control. When people start incorporating regular physical activity into their routine, they will notice their health and quality of life improved, their fitness levels will increase, and the risk of several chronic diseases associated with the musculoskeletal body will be reduced. (Bellissimo et al., 2022) The best way to think about calisthenics is to think like push-ups, planks, squats, and dynamics stretches when working out. Additionally, calisthenics can be scalable and adaptable to any person’s fitness level without heavy gym equipment or HIIT workouts. For individuals dealing with musculoskeletal conditions like low back pain or associated pain symptoms, calisthenics is a safer and more effective option. Calisthenics can even help with cognitive decline associated with musculoskeletal disorders by reducing comorbidities correlated with the muscles and cognitive function. (Osuka et al., 2020) How It Supports Musculoskeletal Health? Musculoskeletal pain is a multi-factorial condition that involves environmental factors that cause long-term pain and disability. (Caneiro et al., 2021) Everyday motions can cause strain and fatigue to the various muscle groups and, over time, can affect the joints in the extremities. For individuals dealing with musculoskeletal disorders, calisthenics can offer numerous benefits to reduce pain-like symptoms associated with the musculoskeletal system: - Improved Core Stability: Calisthenics can help strengthen the core muscles, providing the necessary stability to reduce low back pain. (Zemkova & Zapletalova, 2022)
- Enhanced Mobility: Calisthenics can utilize gentle functional movements within the upper and lower extremities to help preserve the joint’s range of motion.
- Injury Prevention: Individuals incorporating calisthenics for muscle pain will notice that their postural muscles are getting stronger, thus improving body biomechanics and reducing compensatory movements.
- Neuromuscular Re-education: Calisthenic exercises help retrain muscles to fire appropriately, which is excellent for individuals with a sedentary lifestyle. Individuals with a sedentary lifestyle who start doing calisthenic exercises will notice a positive effect on energy expenditure, endothelial function, and muscle improvement. (Mear et al., 2022)
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
What type of exercise is recommended for individuals who want to exercise before bed? Exercising Before Bed Exercising sounds like a good way to tire the mind and body before bed. However, research shows that moderate to vigorous exercise later in the day can negatively impact sleep quality. (Alkhaldi E. H. et al., 2023) - To improve sleep, it is recommended that you exercise in the morning or earlier in the day, at least four hours before bed.
- Individuals who exercise later should aim for lighter activities, such as non-strenuous walking or gentle, restorative yoga.
- Light physical activity, like a slow walk after dinner, is OK.
Advantages Daily exercise improves sleep quality. (Johns Hopkins Medicine, 2025) Mild exercise before bed and engaging in light activities like walking or stretching can positively affect health (Hijikata Y, Yamada S. 2011). These include: - Decrease muscle tension
- Improve digestion
- Improve blood sugar regulation
- Relax the mind and body
Disadvantages The nervous system naturally switches between active and calm. It is ready to work and engage in physical activities when it is active. When it is resting, sleep occurs. Activating the nervous system before bed can affect sleep, and exercising can affect body temperature, producing sleep challenges. Typically, body temperature decreases as the body prepares for sleep. Exercising before bed can increase core temperature and disrupt the process. (Szymusiak R. 2018) Moderate or vigorous physical activity close to going to sleep can: (Alkhaldi E. H. et al., 2023) - Make it more difficult to fall asleep
- This leads to more waking up during the night.
- Decrease sleep quality
Recommended Types of Exercise Pre-bedtime activities should not be vigorous or engaging enough to make the body and mind more alert. Some exercises to calm the body and mind before bed include: (Sleep Foundation, 2023) Restorative Yoga - Yoga Nidra and other low-intensity yoga can help promote sleep.
- More intense forms of yoga, such as vinyasa/flow, should be done earlier.
Tai Chi - A Chinese practice that incorporates slow, gentle movements and focuses on breathing to promote peace and relaxation.
Slow Walking - Walking at a leisurely pace can help the body unwind and relax.
A slow heart rate and breathing indicate that the activity is calming and not stimulating. Exercises to Avoid Moderate to high-intensity workouts before bed that increase breathing and heart rate can disrupt sleep. Individuals who struggle to fall asleep or get restful sleep should try reducing the intensity of certain exercises or avoiding them one to two hours before bed. Examples of moderate to vigorous exercises include: (American Heart Association, 2024) - Gardening or heavy yard work
- Running
- Brisk walking
- Cycling
- Dancing
- Sports activities
Working Out In The Evening Sometimes, exercising later in the day or close to bedtime is the only time to get physical activity. If this is the case, late exercise is better than no exercise at all, but there are ways to lessen its impact on sleep, including: - Light physical activity, like walking, can be done up to an hour before bed.
- Do more intense exercises at the beginning of the workout.
- End the workout with a cooldown, like walking or stretching, to relax the mind and body.
- Know how your workout schedule impacts your sleep, and adjust as necessary.
How Long After Working Out to Go To Sleep? For individuals who want restful and uninterrupted sleep, experts recommend waiting one to two hours after a moderate or vigorous workout to go to bed. (Harvard Health Publishing, 2024) (Johns Hopkins Medicine, 2025) Injury Medical Chiropractic & Functional Medicine Clinic Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop an optimal health and wellness solution. We focus on what works for you to relieve pain, restore function, and prevent injury. Regarding musculoskeletal pain, specialists like chiropractors, acupuncturists, and massage therapists can help mitigate the pain through spinal adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal issues. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies that are available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Alkhaldi, E. H., Battar, S., Alsuwailem, S. I., Almutairi, K. S., Alshamari, W. K., & Alkhaldi, A. H. (2023). Effect of Nighttime Exercise on Sleep Quality Among the General Population in Riyadh, Saudi Arabia: A Cross-Sectional Study. Cureus, 15(7), e41638. https://doi.org/10.7759/cureus.41638 Johns Hopkins Medicine. (2025). Exercising for better sleep. https://www.hopkinsmedicine.org/health/wellness-and-prevention/exercising-for-better-sleep Hijikata, Y., & Yamada, S. (2011). Walking just after a meal seems to be more effective for weight loss than waiting for one hour to walk after a meal. International journal of general medicine, 4, 447–450. https://doi.org/10.2147/IJGM.S18837 Szymusiak R. (2018). Body temperature and sleep. Handbook of Clinical Neurology, 156, 341–351. https://doi.org/10.1016/B978-0-444-63912-7.00020-5 Sleep Foundation. (2023). Bedtime routines for adults. https://www.sleepfoundation.org/sleep-hygiene/bedtime-routine-for-adults American Heart Association. (2024). American Heart Association recommendations for physical activity in adults and kids. https://www.heart.org/en/healthy-living/fitness/fitness-basics/aha-recs-for-physical-activity-in-adults Harvard Health Publishing. (2024). Does exercising at night affect sleep? https://www.health.harvard.edu/staying-healthy/does-exercising-at-night-affect-sleep
Could older individuals who do not have symptoms of shoulder pain or loss of shoulder and arm function have a rotator cuff tear? Rotator Cuff Tear Physical Therapy A rotator cuff tear is a common injury to the four muscles and tendons surrounding and stabilizing the shoulder joint. Studies have shown that (Geary M. B., & Elfar J. C. 2015) - 30% of those under the age of 70
- 70% of those over age 80 have a rotator cuff tear.
Physical therapy is often recommended as a first-line initial treatment for rotator cuff pain. In most cases, a rotator cuff tear will not need surgical treatment. Determining when surgery is necessary depends on several factors a patient can discuss with their healthcare provider. Causes - Overuse and repetitive motions
- Trauma (e.g., falls, collisions)
- Age-related degeneration
Symptoms - Shoulder pain, especially with overhead or rotational movements
- Weakness and difficulty raising the arm
- Clicking or grinding sounds in the shoulder
- Limited range of motion
Treatment The goal of physical therapy for a rotator cuff tear is not necessarily to heal the torn tendon but to relieve pain and improve strength by reducing inflammation and restoring shoulder joint mechanics. This is achieved through physical therapy, ice application, anti-inflammatory treatments like medications, and cortisone injections. Physical Therapy The goal of physical therapy is to improve the function of the muscles that surround the shoulder. Physical therapy targets the smaller muscles around the shoulder that are commonly neglected. By strengthening these muscles, the treatment can help compensate for damaged tendons and improve the mechanics of the shoulder joint. A chiropractic physical therapy team will develop a personalized exercise program. Generally, rehabilitation will start with gentle range of motion exercises that can be accomplished using the arms to lift a mobility stick/wand overhead. Shoulder Pulleys - These improve shoulder range of motion and flexibility.
Isometric Exercises - These exercises are for the rotator cuff muscles and may then be started.
- This exercise can improve the contracting of the muscles around the shoulder and offer more support to the shoulder joint.
Scapular Stabilization Exercises - These can also be done to improve the muscles surrounding the shoulder blade's function.
- This can help improve how the shoulder joint, arm, and scapulae move together when using the arm.
Advanced Strengthening - Advanced exercises can be done with a dumbbell or resistance band.
Consult your healthcare provider or physical therapist before starting these or any other exercises for a rotator cuff tear. Doing exercises correctly prevents further pain, injury, or shoulder problems. Specific, focused exercises can help expedite and regain normal shoulder function. Injury Medical Chiropractic and Functional Medicine Clinic The prognosis for rotator cuff tears depends on the severity of the tear and the individual's overall health. With proper treatment, most people can regain the full function of their shoulders. However, some may experience ongoing pain or limitations in severe cases. Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to build optimal health and wellness solutions. We focus on what works for you to relieve pain, restore function, prevent injury, and help mitigate issues through adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal problems. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Geary, M. B., & Elfar, J. C. (2015). Rotator Cuff Tears in the Elderly Patients. Geriatric orthopaedic surgery & rehabilitation, 6(3), 220–224. https://doi.org/10.1177/2151458515583895
|





 Your new post is loading...
Your new post is loading...
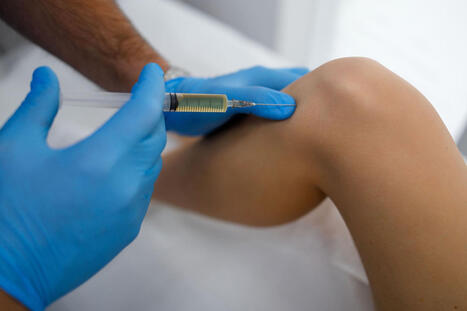




























Alex Jimenez Jr. gave it his all to become the best at wrestling, and coming to Push-as-Rx ® gave him the mental bearing he needed.