 Your new post is loading...
 Your new post is loading...
Gender transitioning is the process of affirming and expressing an individual's internal sense of gender rather than the one assigned at birth. How can learning the aspects of gender and gender transitioning help support the LGBTQ+ community? Gender Transitioning Gender transitioning or gender affirmation is a process through which transgender and gender-nonconforming individuals align their internal gender identity with their external gender expression. It can be described as a binary - male or female - but can also be non-binary, meaning an individual is neither exclusively male nor female. - The process can involve aesthetic appearances, changes in social roles, legal recognitions, and/or physical aspects of the body.
- Social affirmation - dressing differently or coming out to friends and family.
- Legal affirmation - changing name and gender on legal documents.
- Medical affirmation - using hormones and/or surgery to change certain physical aspects of their body.
- Transgender individuals can pursue some or all of these.
Barriers Gender transitioning can be obstructed by various barriers that can include: - Cost
- Lack of insurance
- Lack of family, friends, or partner support.
- Discrimination
- Stigma
Addressing All Aspects The process does not have a specific timeline and is not always linear. - Many transgender and gender-nonconforming individuals prefer gender affirmation to gender transitioning because transitioning is often taken to mean the process of medically transforming the body.
- An individual does not have to undergo medical treatment to affirm their identity, and some transgender people avoid hormones or gender-affirming surgery.
- Transitioning is a holistic process that addresses all aspects of who a person is inwardly and outwardly.
- Certain aspects of transitioning may be more important than others, like changing one's name and gender on their birth certificate.
- Reevaluation and revision of gender identity can be continual rather than a step-by-step, one-way process.
Exploring Gender Identity Gender transitioning often starts in response to gender dysphoria which describes the constant sense of uneasiness that occurs when the gender an individual was assigned at birth does not match how they experience or express their gender internally. - Some individuals have experienced symptoms of gender dysphoria as early as 3 or 4 years of age. (Selin Gülgöz, et al., 2019)
- Gender dysphoria can be largely informed by the culture that surrounds the individual, specifically in cultures where strict codes determine what is masculine/male and feminine/female.
Unease Expressed in Different Ways - Dislike of one’s sexual anatomy.
- A preference for clothes typically worn by the other gender.
- Not wanting to wear clothes typically worn by their own gender.
- A preference for cross-gender roles in fantasy play.
- A strong preference for engaging in activities that are typically done by the other gender.
Dysphoria - Gender dysphoria can fully emerge during puberty when awareness about how an individual's body defines them creates internal distress.
- Feelings may be amplified when an individual is described as a tomboy, or a sissy, or is criticized and attacked for acting like a girl or acting like a boy.
- During puberty, the physical changes can cause long-standing feelings of not fitting in and may evolve into feelings of not fitting in their own body.
- This is when individuals can undergo a process referred to as internal transitioning and begin to change how they see themselves.
Gender transitioning/affirmation becomes the next step. Transitioning is not about changing or recreating oneself but about expressing their authentic self and asserting who they are socially, legally, and/or medically. Social Social transitioning involves how a person publicly expresses their gender. The transition can include: - Changing pronouns.
- Using chosen name.
- Coming out to friends, family, coworkers, etc.
- Wearing new clothes.
- Cutting or styling hair differently.
- Changing mannerisms like moving, sitting, etc.
- Changing voice.
- Binding - strapping the chest to hide breasts.
- Wearing breast and hip prosthetics to accentuate feminine curvature.
- Packing - wearing a penile prosthesis to create a penile bulge.
- Tucking - tucking the penis to conceal a bulge.
- Playing certain sports
- Pursuing different lines of work.
- Participating in activities that might typically be seen as male or female.
Legal Legal transitioning involves changing legal documents to reflect the individual's chosen name, gender, and pronouns. This includes governmental and non-government documents that can include: - Birth certificates
- Social Security ID
- Driver's license
- Passport
- Bank records
- Medical and dental records
- Voter registration
- School ID
- Provisions allowing for changes can vary by state.
- Some states only allow changes if bottom surgery - genital reconstruction is performed.
- Others will allow the changes without any form of gender-affirming surgery.
- Other states have begun to offer an X-gender option for non-binary individuals. (Wesley M King, Kristi E Gamarel. 2021)
Medical Medical transitioning typically involves hormone therapy to develop some of the male or female sex characteristics. It can also involve surgery to change certain physical aspects combined with hormone therapy. - Hormone therapy assists individuals to physically look more like the gender they identify as.
- They can be used on their own and can also be used before gender-affirming surgery.
Hormone therapy takes two forms: Transgender Men Transgender Women Surgery Gender affirmation surgery aligns an individual's physical appearance to their gender identity. Many hospitals provide gender-affirming surgery through a transgender medicine department. Medical procedures include: - Facial surgery - Facial feminization surgery.
- Breast augmentation - Increases breast size with implants.
- Chest masculinization - Removes contours of breast tissues.
- Tracheal shaving - Reduces Adam's apple.
- Phalloplasty - Construction of a penis.
- Orchiectomy - Removal of the testicles.
- Scrotoplasty - Construction of a scrotum.
- Vaginoplasty - Construction of a vaginal canal.
- Vulvoplasty - Construction of the outer female genitalia.
Roadblocks If you know someone who is transgender or is considering transitioning, learning about gender and gender transitioning and how to be supportive is a great way to be an ally. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Gülgöz, S., Glazier, J. J., Enright, E. A., Alonso, D. J., Durwood, L. J., Fast, A. A., Lowe, R., Ji, C., Heer, J., Martin, C. L., & Olson, K. R. (2019). Similarity in transgender and cisgender children's gender development. Proceedings of the National Academy of Sciences of the United States of America, 116(49), 24480–24485. https://doi.org/10.1073/pnas.1909367116 Irwig, M. S., Childs, K., & Hancock, A. B. (2017). Effects of testosterone on the transgender male voice. Andrology, 5(1), 107–112. https://doi.org/10.1111/andr.12278 Tangpricha, V., & den Heijer, M. (2017). Estrogen and anti-androgen therapy for transgender women. The Lancet. Diabetes & endocrinology, 5(4), 291–300. https://doi.org/10.1016/S2213-8587(16)30319-9 National Center for Transgender Equality. Know Your Rights in Health Care. Kaiser Family Foundation. Update on Medicaid coverage of gender-affirming health services. Center of Medicare and Medicaid Services. Gender dysphoria and gender reassignment surgery. Transgender Legal Defense and Education Fund. Health insurance medical policies. National Center for Transgender Equality and National Gay and Lesbian Task Force. Injustice at Every Turn: A Report of the National Transgender Discrimination Survey. Turban, J. L., Loo, S. S., Almazan, A. N., & Keuroghlian, A. S. (2021). Factors Leading to "Detransition" Among Transgender and Gender Diverse People in the United States: A Mixed-Methods Analysis. LGBT health, 8(4), 273–280. https://doi.org/10.1089/lgbt.2020.0437
For athletes, the vertical jump is a skill that can be increased and improved with proper training. To improve jumping abilities for sports like basketball, tennis, volleyball, or track and field events such as the high jump it is necessary to do both strength and power training. Research has found certain key components can help athletes become better at jumping. There are different ways to improve an individual's vertical jump. Here we go over some of the most effective exercises including plyometrics, and exercises that build strength and power. Vertical Jump Increase and Improvement Jumping is an explosive movement. - To jump well, an individual needs a consistent powerful spring.
- This is achieved by training the explosive/fast-twitch muscle fibers with the ability to shorten and stretch dynamically.
- Upper body strength is important for creating upward momentum.
- Strength exercises involve slow, controlled movements like squats, lunges, and step-ups with weights.
- Power exercises involve explosive, quick movements.
- Plyometrics involve explosive hopping, bounding, and jumping drills that combine strength and speed.
Exercises Plyometrics - Common plyometric exercises include hops, jumps, and bounding movements.
- A popular exercise is jumping off a box and rebounding off the floor then jumping onto another, higher box.
- Box jumps provide practice for jumping.
Single-Leg Squats - Single-leg squats can be done almost anywhere, without equipment.
- They work the hips, hamstrings, quadriceps, gluteus maximus, and calves.
- They strengthen the core and increase flexibility.
Full Squats - This is a barbell exercise to build strength and power.
- It is considered one of the best total body exercises.
Weighted Step-Ups - The step-up is a recommended all-around exercise that can be done almost anywhere.
- Not only will it build strength in your quadriceps, but you can also use it as part of a cardio workout.
- It has a low risk of injury.
Overhead Walking Lunges - All that is needed is a weight and room to walk.
- This exercise builds power, strength, and speed in the legs.
- Improves core strength.
Stair Running - This is a high-intensity workout that builds speed, power, and cardiovascular fitness.
- It targets the glutes, quads, and calves.
Agility Drills - Agility drills can include jumping to improve coordination, speed, power, and specific skills.
Sprints - Sprints are quick intense exercises to build muscle and increase performance.
- Sprints use more muscle groups.
Practice - Build strength by performing basic weight training exercises using slow, controlled movements.
- Build power with faster dynamic movements.
- Improve movement speed to create power with explosive, quick exercises.
- Work on form, by incorporating the lead-up to the jump, arm motion, and safe landing technique.
- Include time to practice maximum jumping and bring it all together.
- Always warm up before jumping or performing drills to keep the joints and body safe.
- Athletes jump rope to get the blood circulating and warm up their muscles.
- Do several slow, controlled toe raises to prepare the feet and ankles for jumping and landing.
- Gradually work up to a full vertical jump, by doing box and squat jumps.
Jumping - When finally working on the vertical jump, start with the feet hips-distance apart.
- If measuring jump height, stand about a foot away from the measuring tape or measuring bar on the side.
- Start with arms overhead.
- As you drop into a squat position swing the arms behind the hips.
- Swing back up to the starting position before going for the full jump.
- The pre-swing helps build momentum.
- Land with the knees bent to minimize the impact.
Jumping is a high-impact activity that can take a toll on the knees, hips, ankles, and feet. Be sure to rest the body between hard workouts so the muscles have time to recover, repair, and build up. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Barnes, Jacque L et al. “Relationship of jumping and agility performance in female volleyball athletes.” Journal of Strength and conditioning research vol. 21,4 (2007): 1192-6. doi:10.1519/R-22416.1 Bezerra, Ewertton DE S et al. “Influence of Trunk Position during Three Lunge Exercises on Muscular Activation in Trained Women.” International journal of exercise science vol. 14,1 202-210. 1 Apr. 2021 Hedlund, Sofia, et al. “Effect of chiropractic manipulation on vertical jump height in young female athletes with talocrural joint dysfunction: a single-blind randomized clinical pilot trial.” Journal of Manipulative and physiological therapeutics vol. 37,2 (2014): 116-23. doi:10.1016/j.jmpt.2013.11.004 Hernández, Sebastian, et al. “Effects of Plyometric Training on Neuromuscular Performance in Youth Basketball Players: A Pilot Study on the Influence of Drill Randomization.” Journal of sports science & medicine vol. 17,3 372-378. 14 Aug. 2018 Karatrantou, Konstantina, et al. “Can sport-specific training affect vertical jumping ability during puberty?.” Biology of sport vol. 36,3 (2019): 217-224. doi:10.5114/biolsport.2019.85455 Markovic, Goran. “Does plyometric training improve vertical jump height? A meta-analytical review.” British Journal of sports medicine vol. 41,6 (2007): 349-55; discussion 355. doi:10.1136/bjsm.2007.035113 McLellan, Christopher P et al. “The role of rate of force development on vertical jump performance.” Journal of Strength and conditioning research vol. 25,2 (2011): 379-85. doi:10.1519/JSC.0b013e3181be305c Rodríguez-Rosell, David, et al. “Traditional vs. Sport-Specific Vertical Jump Tests: Reliability, Validity, and Relationship With the Legs Strength and Sprint Performance in Adult and Teen Soccer and Basketball Players.” Journal of Strength and conditioning research vol. 31,1 (2017): 196-206. doi:10.1519/JSC.0000000000001476 Vanezis, Athanasios, and Adrian Lees. “A biomechanical analysis of good and poor performers of the vertical jump.” Ergonomics vol. 48,11-14 (2005): 1594-603. doi:10.1080/00140130500101262
Regular exercise and physical activity help with cardiovascular health, improved mood, better management of chronic conditions, and can help digestion. For individuals with any GI distress or inflammatory bowel disease that has caused digestive enzyme deficiencies, exercise, and physical movement have been found to provide digestive aid. Here we look at activities to help digestion. Exercises To Help Digestion When exercising the body, the cardiac output/volume of blood the heart pumps every minute increases as the demand for oxygenated blood throughout the body increases, particularly in the working muscles. During exercise, the same increase in blood circulation happens within the digestive system's muscle groups. The blood flow to digestive organs causes peristalsis, which is involuntary constriction and relaxation of the muscles in the digestive tract. This process helps move food efficiently through the gastrointestinal tract. Exercise supports the growth of beneficial gut bacteria to maintain a healthy digestive system. - Exercise helps relieves stress which means lower amounts of cortisol.
- Research has found that elevated cortisol levels are associated with compromised digestive function.
- Chronic cortisol production can cause:
- Increased intestinal permeability.
- Impaired absorption of micronutrients.
- Abdominal pain or discomfort.
Types of Exercise - Sticking to moderate-intensity workouts supports a healthy gut microbiome and reduces inflammation.
- Whereas high-intensity exercise sends blood away from the core and toward the extremities to power the muscles, which does not help digestion.
- High-intensity exercise may trigger an inflammatory response, leading to abdominal pain or discomfort, diarrhea, and cramps.
Moderate-intensity exercise activities to try include: Yoga - Yoga is a great stress reduction tool, helping to reduce inflammation that can lead to various gut issues, including constipation and stomach pain.
- Left untreated, chronic inflammation can cause inflammatory bowel disease symptoms to flare.
- Yoga places mild pressure on the digestive organs in certain positions, which can help digestion.
Walking - Walking 30 to 40 minutes three to four times a week can make a digestive difference.
- Walking stimulates blood flow to the intestinal muscles, which helps activate the lymphatic system.
- The gut's lymphatic system helps to absorb and transport lipids and other nutrients throughout the body during digestion.
- The system activates through walking or manual lymphatic massage can improve constipation.
Tai Chi - Tai chi has been shown to improve immune function and inflammation of the gut and is a helpful tool for maintaining homeostasis/gut balance.
- This is a form of moderate-intensity exercise and meditative practice.
- The emphasis is on slow controlled movements and deep breathing.
- This makes it recommended for individuals looking to improve digestion and those with gastrointestinal conditions.
Pilates - Pilates is the practice that targets abdominal muscles and utilizes diaphragmatic breathing to help individuals perform a series of movements to strengthen and elongate the body’s muscles.
- Individuals who perform this exercise often report relief from bloating and gas.
- Exercises like rolling like a ball or the swan dive are great for the digestive organs.
Digestion Goals Whether new to exercise or returning, a plan can help you get there. Meeting with a fitness trainer or sports chiropractor is a great place to begin if you have limited knowledge about what works best for your body and schedule. - A certified trainer can help guide you toward an achievable program that focuses on gut health.
- Individuals with a GI disorder should talk with their doctors before starting a new exercise plan.
- This does not mean you can’t do intense exercises like running; you’ll want to work with a doctor to set up a program that doesn’t cause flare-ups.
- Aim for roughly three hours of moderate-intensity weekly exercise to support a healthy digestive system.
- Sit less and move more.
- Do at least two or more muscle-strengthening activities of moderate intensity every week.
- An anti-inflammatory diet may aid digestion.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Cherpak, Christine E. “Mindful Eating: A Review Of How The Stress-Digestion-Mindfulness Triad May Modulate And Improve Gastrointestinal And Digestive Function.” Integrative medicine (Encinitas, Calif.) vol. 18,4 (2019): 48-53. Drouin, Jacqueline S et al. “Comparisons between Manual Lymph Drainage, Abdominal Massage, and Electrical Stimulation on Functional Constipation Outcomes: A Randomized, Controlled Trial.” International Journal of environmental research and public health vol. 17,11 3924. June 1. 2020, doi:10.3390/ijerph17113924 Hamasaki, Hidetaka. “Exercise and gut microbiota: clinical implications for the feasibility of Tai Chi.” Journal of integrative medicine vol. 15,4 (2017): 270-281. doi:10.1016/S2095-4964(17)60342-X Joyner, Michael J, and Darren P Casey. “Regulation of increased blood flow (hyperemia) to muscles during exercise: a hierarchy of competing physiological needs.” Physiological Reviews vol. 95,2 (2015): 549-601. doi:10.1152/physrev.00035.2013 LeBouef T, Yaker Z, Whited L. Physiology, Autonomic Nervous System. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538516/ Singhal, Rashi, and Yatrik M Shah. “Oxygen battle in the gut: Hypoxia and hypoxia-inducible factors in metabolic and inflammatory responses in the intestine.” The Journal of biological chemistry vol. 295,30 (2020): 10493-10505. doi:10.1074/jbc.REV120.011188 van Wijck, Kim, et al. “Physiology and pathophysiology of splanchnic hypoperfusion and intestinal injury during exercise: strategies for evaluation and prevention.” American Journal of Physiology. Gastrointestinal and liver physiology vol. 303,2 (2012): G155-68. doi:10.1152/ajpgi.00066.2012
Introduction Everyone, at some point, has some form of physical activity that helps them release the stresses of everyday factors. Whether for athletic training or to keep a healthy lifestyle, exercising for at least 30 minutes to an hour can help promote muscle growth and toning, reducing stress and high blood pressure. However, many individuals would often not be able to find time to exercise, which can lead to many problems in their bodies. When many individuals are physically inactive, it can lead to musculoskeletal pain, weak muscles, and other chronic conditions. To that point, it can make the person miserable and cause disability. Luckily numerous therapies can help reduce the effects of pain-like symptoms associated with physical inactivity and can help restore the body. Today’s article focuses on how MET (muscle energy techniques) therapy uses a chair and abdominal exercises to help promote spinal flexibility, reduce abdominal weakness, and strengthen low back and pelvic muscles. We utilize and incorporate valuable information about our patients to certified medical providers using the chair and abdominal exercises in MET therapy. We encourage and refer patients to associated medical providers based on their findings while supporting that education is a remarkable and fantastic way to ask our providers the essential questions at the patient’s acknowledgment. Dr. Alex Jimenez, D.C., comprises this information as an educational service. Disclaimer Chair Exercises In MET Therapy Are you experiencing muscle pain in specific areas of your body? Do your legs feel tired after a long day at work or when you bend down to pick something up? These musculoskeletal pain symptoms are often caused by physical inactivity, which can cause muscles to become weak and short. This can lead to various health issues related to musculoskeletal pain if not addressed. However, you can help reduce these effects by incorporating everyday objects like a chair into your exercise routine. Research studies have revealed that chair-based exercises can provide cognitive and psychological benefits while reducing the risk of injury. Additionally, using a chair for exercise can improve spinal flexibility. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
The biceps curl is an exercise to build strength in the upper arm. Curls are a common exercise used in upper-body strength training. Specifically, the curl works the muscles in the front of the upper arm. It's recommended for achieving strength and definition and provides core and stability challenges. Injury Medical Chiropractic and Functional Medicine Clinic can educate individuals on fitness, strength training, nutrition, and injury prevention. Bicep Curls Located at the upper arm, the biceps comprise a short and long head that operates as a single muscle. - The bicep heads begin at different places around the shoulder/scapula region,
- They have a common insertion point on the elbow tendon.
- Together allow the bending of the arm at the elbow joint to curl and pull weight.
- Curls work the muscles at the front of the upper arm and the lower arm. The brachialis and brachioradialis.
Dumbbells Different equipment and grips can be used, including dumbbell weights, kettlebells, barbells, resistance bands, or cable machines. Select equipment with enough weight that can be lifted ten times using proper form, ensuring the last three repetitions are challenging to the point of being unable to raise another. From there, use this same weight to perform eight repetitions or slightly lower the weight and perform ten repetitions. - Begin by standing with the feet about hip-width apart.
- Keep the abdominal/core muscles engaged.
- Hold one dumbbell in each hand.
- Relax the arms down at the sides with palms facing forward.
- Keep the upper arms stable and shoulders relaxed.
- Bend at the elbow and lift the weights so the dumbbells approach the shoulders.
- Raise the dumbbells to eye or forehead level for a full range of motion.
- Tension will be felt in the muscles in the front of the upper arm.
- Keep movements smooth and controlled.
- The elbows should stay tucked in close to the body.
- Be careful to keep the wrist straight and rigid.
- Flexing the wrist while bending the elbow won't target the biceps effectively and can result in a wrist or elbow injury.
- Exhale while lifting.
- Lower the weights to the starting position.
- For most, one set of 12 to 15 repetitions is adequate.
- Train to failure performing the desired reps, staying within 3 to 5 repetitions of total failure.
- When able, slightly increase weight and/or reps over time to increase muscle and strength.
- Both biceps can be worked out by alternating arms.
- It can be done standing or sitting.
Avoid Errors Get the most out of the workout by avoiding these errors. Rushing Through - Focus on proper form and avoid rushing through the workout.
- Lift the weights with a smooth motion.
- Take as much time to lower the weight as when lifting it.
- Lowering the weight slowly can help build more muscle, making the most of the workout.
Improper Elbow Position - The position of the elbows should remain close to the side of the body.
- Only the lower arm should move until the end of the movement when the elbows rise. This is a complete range of motion.
- If the elbows move away from the torso or swing behind the body, there is probably too much weight.
Avoid Swinging the Weights - Focus on maintaining a tall, upright spine and a tight core.
- The shoulders or torso should not swing the weights up when doing the curl.
- It can feel like swinging, twisting, or heaving movements.
- Don't let the hips hinge, or the lower body assist the movement.
- Keep the elbows at the sides until they naturally rise at the end of the motion.
- Keep the shoulders relaxed
- Make sure the shoulders don't move forward to initiate the movement.
- Use lighter weights or reduce the number of repetitions if this happens.
Safety This exercise is generally recommended for most individuals. However, getting clearance from a primary caregiver before beginning any exercise routine is recommended. - Individuals with an arm injury or who experience pain during the motion should not perform the exercise without a doctor's approval.
- Don't try to lift weights that are too heavy.
- After a few lifts, expect to feel fatigued and a burning sensation in the biceps and forearm muscles.
- This is the desired effect to get the muscles strong and growing.
- Do not force extra repetitions once proper form cannot be achieved.
- Take a thorough rest before the next set.
- Stop if pain begins to present.
Benefits - These muscles are in constant use when picking things up.
- Consistently performing the biceps curl will help build strength in the upper arm.
- Individuals learn to use their arm muscles correctly and with the core muscles.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Coratella, Giuseppe, et al. “Biceps Brachii and Brachioradialis Excitation in Biceps Curl Exercise: Different Handgrips, Different Synergy.” Sports (Basel, Switzerland) vol. 11,3 64. 9 Mar. 2023, doi:10.3390/sports11030064 Coratella, Giuseppe, et al. “Bilateral Biceps Curl Shows Distinct Biceps Brachii and Anterior Deltoid Excitation Comparing Straight vs. EZ Barbell Coupled with Arms Flexion/No-Flexion.” Journal of functional morphology and Kinesiology vol. 8,1 13. 19 Jan. 2023, doi:10.3390/jfmk8010013 Marchetti, Paulo H et al. “Seated row and biceps curl exercises present similar acute responses on muscle thickness, arm circumference, and peak force for elbow flexors after a resistance training session in recreationally-trained subjects.” The Journal of sports medicine and physical fitness vol. 60,11 (2020): 1415-1422. doi:10.23736/S0022-4707.20.10996-4 Sato, Shigeru, et al. “Elbow Joint Angles in Elbow Flexor Unilateral Resistance Exercise Training Determine Its Effects on Muscle Strength and Thickness of Trained and Non-trained Arms.” Frontiers in physiology vol. 12 734509. 16 Sep. 2021, doi:10.3389/fphys.2021.734509 Schoenfeld, Brad Jon, et al. “Differential effects of attentional focus strategies during long-term resistance training.” European Journal of sports science vol. 18,5 (2018): 705-712. doi:10.1080/17461391.2018.1447020
Introduction An exercise routine is highly important for anyone trying to get a kick start on their health and wellness journey. It could be simple as walking around the park for 30 minutes, going to the community pool to swim, or taking a group fitness class with friends. Incorporating an exercise regime can even help reduce the effects of musculoskeletal disorders and their associated symptoms from causing pain in the muscles and joints in the body. Even though many individuals have busy lives, it is important to ensure that their bodies are getting enough exercise to feel less joint and muscle pain while improving other systems that benefit from training. Today’s article looks at how to keep a constant exercise routine, how exercise can help musculoskeletal disorders, and how the MET technique is combined with physical activity. We provide and mention valuable information about our patients to certified medical providers who offer available therapy treatments like the MET technique combined with physical activities for individuals dealing with musculoskeletal pain disorders. We encourage each patient by referring them to our associated medical providers based on the patient’s diagnosis findings appropriately. We acknowledge that education is a spectacular way when asking our providers the most helpful questions at the patient’s acknowledgment. Dr. Alex Jimenez, D.C., utilizes this information as an educational service. Disclaimer Keeping A Constant Exercise Routine Have you been feeling sluggish throughout the day? Do you believe you don’t have enough time to exercise and feel stressed? Or have you been experiencing unwanted pain and stiffness in your muscles and joints? Many individuals experiencing these issues in their bodies could not be getting enough exercise to reduce these musculoskeletal disorders. When it comes to many individuals trying to keep a constant exercise routine to better their health may be difficult but not impossible. There are many ways to incorporate a daily consistent exercise routine by making small changes in your daily life routine. Walking with friends or pets, attending a group fitness class, or doing squats at home can benefit muscle growth and promote motivation to continue these small changes. However, some of the reasons that many people need to exercise more are to need more time. Studies reveal that most people often refrain from any form of exercise due to needing more time out of their busy schedules. People who do not exercise regularly are potentially at risk of developing health-related problems and disorders linked to the musculoskeletal system. Exercise For Musculoskeletal Disorders When the musculoskeletal system is linked to health-related problems due to physical inactivity, when the body is not getting enough exercise, it can cause muscle and joint pain and other associated symptoms that can affect mobility. Research studies have revealed that pain in specific areas of the body, which includes the back, neck, and shoulders, is often due to extended periods of sitting down and inactivity that cause many people to develop musculoskeletal disorders. When pain and discomfort affect the body, it can cause visceral-somatic pain in different body areas. Not only that, but the various muscles in the upper and lower extremities of the body will become shortened and weak over time, leading to disability and poor posture. Now all is not lost, as there are ways to reduce the effects of musculoskeletal disorders and incorporate exercise as part of a person’s daily routine. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction Dr. Jimenez, D.C., presents how implementing different strategies for patients to incorporate exercise in their health and wellness journey in this 2-part series. Many factors and lifestyle habits tend to take over our daily lives, leading to chronic disorders that can impact our bodies and cause many unwanted symptoms. In this presentation, we will look at different strategies and options to incorporate into our patients regarding health and wellness. Part 1 looks at how to implement exercise in a clinical setting. We mention our patients to certified medical providers that provide available therapy treatments for individuals suffering from chronic conditions associated with Lyme disease. We encourage each patient when it is appropriate by referring them to associated medical providers based on their diagnosis or needs. We understand and accept that education is a marvelous way when asking our providers’ crucial questions at the patient’s request and acknowledgment. Dr. Alex Jimenez, D.C., uses this information as an educational service. Disclaimer Different Strategies For Patients Part 1 in the last presentation mentioned what to do when examining patients. We said how to implement different strategies to incorporate exercise into a daily routine for many individuals who want to kickstart their health and wellness journey. By coming up with a plan, many doctors can help their patients develop a personalized plan to cater to the individual; it can allow both the patient and doctor to see what works and what doesn’t. Part 1 also explains how to delegate with the patients to help ease them into implementing exercise as part of their daily routine. Delegation is described as a transfer of responsibility for the performance of the patient’s care while retaining accountability for the outcomes. The main point here is you are delegating the educational process related to the exercise prescription. You can use it for the diet prescription, or you can use it for anything that tends to be educational and formatted for your patients. Based on the documentation complexity, we would ensure a face-to-face encounter with the patient to meet the legal requirement for insurance to bill it as a 99-213 or a 99-214. So what we do with our health coaches is we also want to have them do other cross-trained roles in our office because we’re a small little practice. So, our health coaches are involved with our patients and know how to assess if an interested new patient would be a good candidate for our services. They are great at using the technology we do with some of our new patients, whether it’s a BIA or if we prescribe heart math. So they are great with technology and with education around nutrition, exercise, whatever you can train your health coach to do, then you can create a way to delegate for her to do it, whether it’s through insurance or cash. Okay, now last but certainly not least, it is so important to know, and you know this if you have children or you know if you have a family member, which we know you do that what you say and what you do are two different things. So there are studies that show an association that if a provider is exercising or implementing a journey of improving their exercise and diet, it shows up more in their recommendations. And when a provider talks about it authentically during a motivational interviewing process with a patient, it’s obvious to the patient that it’s important to the provider because they’re not just talking the talk; they’re walking the walk, which is important for all of us. We are patients as well. To consider that one of the best ways to start an exercise prescription program and your office is to do one for yourself. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction When everyday factors affect how many of us function, our back muscles begin to suffer. The back muscles in the cervical, thoracic, and lumbar section surround the spine and spinal cord, which helps the body stay upright and promotes good posture. The muscles allow the upper portions of the body to bend down and twist without pain while providing stability to the lower parts of the body. However, when the body ages or everyday activities cause issues, it can develop low back pain associated with weak back muscles. There are many ways to prevent these issues from escalating with various hyperextension exercises for low back pain. This 2-part series examines how low back pain affects the body and how different hyperextension exercises can help strengthen the back. Part 1 examines how hyperextension affects the body and how it is associated with low back pain. We mention our patients to certified medical providers that provide available therapy treatments for individuals suffering from chronic low back pain. We encourage each patient when it is appropriate by referring them to associated medical providers based on their diagnosis or needs. We understand and accept that education is a marvelous way when asking our providers’ crucial questions at the patient’s request and acknowledgment. Dr. Jimenez, D.C., makes use of this information as an educational service. Disclaimer Low Back Pain Affecting The Body Have you been dealing with aches and pains when bending down? Do you feel stiffness in your torso when twisting? Or have you experienced limited mobility in your hips? Many of these symptoms correlate with low back pain. Studies reveal that back pain is one of the most common issues in the emergency room. Low back pain is associated with many factors that put pressure on the various muscles in the back and can lead to underlying conditions that can cause symptoms to make the body dysfunctional. Additional studies have revealed that chronic low back pain can have influenced overlapping risk profiles, which include: - Stress
- Dietary habits
- Lifting heavy objects
- Musculoskeletal disorders
When these factors affect the back, many individuals will be in constant pain and take medication to relieve their pain. However, medicine can only go so far as it only masks the pain, but there are other ways to reduce low back pain and help strengthen the various muscles surrounding the low back. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The various muscles and ligaments that encompass the back help protect the spine’s thoracic region. The spine has three sections: cervical, thoracic, and lumbar, which assist the body with bending, turning, and twisting. For the thoracic spine, various muscles like the rhomboid, trapezoid, and other superficial muscles provide functionality to the scapula or shoulder blades to stabilize the ribcage. When the body succumbs to injuries or traumatic forces, it can develop myofascial pain syndrome associated with upper back pain. Upper back pain can lead to unwanted symptoms affecting their quality of life. Fortunately, various exercises target the upper portion of the back and can strengthen multiple muscles from injuries. Today’s article looks at the effects of upper back pain in the body and shows a few stretches and exercises that can support the various muscle groups in the upper back region. We refer our patients to certified providers that incorporate techniques and multiple therapies for many individuals suffering from upper back pain and its correlating symptoms that can affect the musculoskeletal system in the neck, shoulders, and thoracic region of the spine. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a fantastic way when asking our providers intricated questions at the patient’s request and understanding. Dr. Jimenez, D.C., only utilizes this information as an educational service. Disclaimer The Effects Of Upper Back Pain In The Body Have you been experiencing stiffness around or near your shoulder blades? Do you feel muscle strain when you are rotating your shoulders? Or does it hurt when you stretch your upper back in the morning? Many of these issues are signs and symptoms of upper back pain. Studies reveal that back pain is one of the most common complaints many individuals would go for emergency care. Back pain can affect the different regions in the back and cause unwanted symptoms in various areas in the upper back. Additional studies mentioned that persistent pain in the thoracic region could cause hyper-sensitization of the intercoastal nerves that mimic other conditions affecting the back. Some of the causes and effects that can lead to the development of upper back pain include: - Poor posture
- Improper lifting
- Traumatic events or injuries
- Chronic diseases (Osteoporosis, Scoliosis, Kyphosis)
When this happens, it can lead to overlapping conditions that mimic other issues and, if not treated right away, leave individuals with chronic disabling symptoms that correlate with upper back pain. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Agility is the ability to accelerate, decelerate, stabilize, and quickly change directions with proper form and posture. Everyone, athletes and non-athletes, use agility every day. This can be maneuvering around objects during a jog, shifting movements or positions when walking through a crowd, reaching toward the highest shelf, or carrying things upstairs. These controlled reactions require a balance of coordination, speed, stamina, and strength. Injury Medical Chiropractic and Functional Medicine Clinic can provide agility enhancement through adjustments, massage, and decompression to relax the body, strengthen the muscles, and improve circulation and nerve function. Agility Enhancement Individuals need skill and control to react to a stimulus or movement. Agility requires muscular coordination, efficiency, and cohesiveness between the upper and lower body. Agility and reaction time are two components of neuromusculoskeletal health that work together. Agility enhancement can improve cognitive ability, power production, and physical performance. Agility enhancement improves overall physical skills, including: - Balance
- Stability
- Coordination
- Body Control
- Cognition
- Recovery time
Chiropractic Care Chiropractic improves agility neurologically through improved circulation and energy flow in the nervous system. Injury Treatment and Prevention Agility enhancement can help with injury prevention, as agility training increases control, balance, and flexibility. It teaches the correct body placement while moving to protect the knees, shoulders, and lower back. It also helps to strengthen the muscles and improve the resiliency of the connective tissue allowing them to shorten and lengthen rapidly. This helps prevent injuries and relieves pain and stiffness associated with muscle overuse. - Stiffness often occurs from the overuse of muscles.
- Stiffness reduces flexibility, increasing the risk of injury and affecting movement and physical capabilities.
- Stiffness can even occur from changes in everyday routines.
- Chiropractic prevents the muscles from tensing up, reducing stiffness and increasing your range of motion.
- Chiropractic helps strengthen the musculoskeletal system, which makes it easier to maintain normal balance.
- Chiropractic can strengthen the muscles by making the muscle fibers more excitable, contributing to quicker reaction time.
We create rehabilitation and strength and conditioning treatment plans that are individualized for each individual. This program entails the following: - Chiropractic assessment.
- Therapeutic massage.
- Rehabilitation exercises.
- Strengthening of the whole body.
- Posture, mobility, and performance education for improved movement.
- Health and nutritional recommendations.
Our treatment programs are designed to improve each individual's whole body health and decrease the risk of injury. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Ali, Kamran, et al. "Comparison of Complex Versus Contrast Training on Steroid Hormones and Sports Performance in Male Soccer Players." Journal of chiropractic medicine vol. 18,2 (2019): 131-138. doi:10.1016/j.jcm.2018.12.001 Järvinen, Tero A H, et al. "Muscle injuries: optimizing recovery." Best practice & research. Clinical rheumatology vol. 21,2 (2007): 317-31. doi:10.1016/j.berh.2006.12.004 Lennemann, Lynette M et al. "The influence of agility training on physiological and cognitive performance." Journal of strength and conditioning research vol. 27,12 (2013): 3300-9. doi:10.1519/JSC.0b013e31828ddf06 Miners, Andrew L. "Chiropractic treatment and the enhancement of sports performance: a narrative literature review." The Journal of the Canadian Chiropractic Association vol. 54,4 (2010): 210-21.
Preparing for the holidays is exciting but can generate intense stress and anxiety. This can cause individuals to feel tired constantly, which can lead to other issues like sleep problems, brain fog, digestive issues, and musculoskeletal disorders. Chiropractic care can return the body to optimal function, increasing circulation, restoring spinal alignment, re-energizing the mind and body, and preventing future fatigue and exhaustion. Exhaustion and Fatigue Primary causes of fatigue and exhaustion are stress, overworking, school work, lack of sound sleep, excessive caffeine or other energy boosters, and the holidays. Stress Reduction Stress is a leading contributor to fatigue and exhaustion. - Stress causes the muscles to contract, restricting blood circulation.
- Chronic stress causes the musculoskeletal system to be in a state of continued constriction.
- Constant muscle tension can cause injury and chronic conditions that can lead to secondary disorders like tension headaches and migraines.
Quality Sleep High-quality rest means falling asleep naturally, staying asleep through the night comfortably, and waking rested and refreshed. - Lack of enough sleep strains the nervous system.
- Not enough sleep or disruptions to the sleep-wake cycle (that can happen with shift work or traveling work) can cause physiological fatigue.
- This causes reduced motor skills, similar to having a blood alcohol content of 0.1.
Nutrition Proper nutrition is key to overall health and stress management. An unhealthy diet can be the main cause of fatigue. Just like putting the wrong gas into your car can cause major issues stalling or stopping entirely. The same is true with the body. The body is a complicated engine that requires healthy fuel to work properly. - Macronutrients (fat, carbohydrates, and protein) and Micronutrients (vitamins and minerals) are essential.
Chiropractic Care and Functional Medicine Chiropractic care can be a long-term solution for fatigue and exhaustion. Spine Realignment Spinal realignment resets the body through better posture and brain function through the improved circulation flowing through the spinal cord. - Optimal spinal realignment:
- Relieves headaches
- Alleviates discomfort symptoms
- Increases energy
- Restores range of motion
Relieve Pressure On The Nerves Chiropractic releases pressure on the nerves. - The central nervous system's response to pain, energy levels, comfort, and mobility is impacted by the health of the nerves.
- Just a minimal amount of pressure can reduce the strength of a nerve by 90%.
- Nerves that are not working correctly have difficulty transmitting messages, often causing pain.
Loosen Tense Muscles Chiropractic care and massage therapy can help relieve the tension in overworked muscles. - Fatigue and exhaustion can cause the muscles to work harder/overcompensate to try to maintain balance.
- Over time, the muscles can't keep it up and become frozen and tense.
Nervous System Regulation Chiropractic care can restore nervous system function. - When the spine is not correctly aligned, the electrical impulses are not transmitted properly.
- Common side effects include headaches, neck and back problems, and digestive issues.
Chiropractic care can restore the body to a refreshed and rejuvenated state. It can improve circulation, rebalance the body, increase oxygen levels and strengthen the immune system. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Azzolino, Domenico, et al. “Nutritional Status as a Mediator of Fatigue and Its Underlying Mechanisms in Older People.” Nutrients vol. 12,2 444. 10 Feb. 2020, doi:10.3390/nu12020444 Chaudhuri, Abhijit, and Peter O Behan. “Fatigue in neurological disorders.” Lancet (London, England) vol. 363,9413 (2004): 978-88. doi:10.1016/S0140-6736(04)15794-2 Evans, William J, and Charles P Lambert. “Physiological basis of fatigue.” American journal of physical medicine & rehabilitation vol. 86,1 Suppl (2007): S29-46. doi:10.1097/phm.0b013e31802ba53c Finsterer, Josef, and Sinda Zarrouk Mahjoub. “Fatigue in healthy and diseased individuals.” The American journal of hospice & palliative care vol. 31,5 (2014): 562-75. doi:10.1177/1049909113494748 Rosenthal, Thomas C et al. “Fatigue: an overview.” American family physician vol. 78,10 (2008): 1173-9.
Diagnosing ankylosing spondylitis usually involves multiple tests. When doctors order blood tests to diagnose ankylosing spondylitis, an individual is experiencing worsening symptoms in their back and joints. Often, a blood test diagnosis means the doctor is looking for evidence of anything else that could be causing the symptoms. However, blood tests by themselves cannot definitively diagnose ankylosing spondylitis, but when combined with imaging and assessment, they can provide important clues that point to the answers. Ankylosing Spondylitis Blood Test Diagnosis Ankylosing spondylitis is arthritis that primarily affects the spine and hips. It can be difficult to diagnose as no single test can provide thorough information for a definitive diagnosis. A combination of diagnostic tests are utilized, including a physical exam, imaging, and blood tests. Doctors are not only looking for results that will point to ankylosing spondylitis, but they are looking for any results that might point away from the spondylitis results that might provide a different explanation for symptoms. Physical Exam The diagnostic process will begin with the individual's medical history, family history, and physical exam. During the exam, the doctor will ask questions to help rule out other conditions: - How long have symptoms been presenting?
- Do symptoms get better with rest or exercise?
- Are the symptoms getting worse or staying the same?
- Are the symptoms worse at a particular time of day?
The doctor will check for limitations in mobility and palpate tender areas. Many conditions can cause similar symptoms, so the doctor will check to see if the pain or lack of mobility is consistent with ankylosing spondylitis. The feature sign of ankylosing spondylitis is pain and stiffness in the sacroiliac joints. The sacroiliac joints are located in the lower back, where the base of the spine and pelvis meet. The doctor will look at other spinal conditions and symptoms: - Back pain symptoms caused by - injuries, posture patterns, and/or sleeping positions.
- Lumbar spinal stenosis
- Rheumatoid arthritis
- Psoriatic arthritis
- Diffuse idiopathic skeletal hyperostosis
Family History - Family history plays a part in diagnosis because of the genetic element of ankylosing spondylitis.
- The HLA-B27 gene corresponds with ankylosing spondylitis; if an individual has it, one of their parents has it.
Imaging - X-rays often serve as the first step to a diagnosis.
- As the disease progresses, new small bones form between the vertebrae, eventually fusing them.
- X-rays work best at mapping the disease progression than the initial diagnosis.
- An MRI provides clearer images in the early stages as smaller details are visible.
Blood Tests Blood tests can help rule out other conditions and check for signs of inflammation, providing supportive evidence along with the results of imaging tests. It typically only takes about a day or two to get the results. The doctor may order one of the following blood tests: HLA-B27 HLA-B27 test. - The HLA-B27 gene reveals a red flag that ankylosing spondylitis could be present.
- Individuals with this gene have a much higher risk of developing the condition.
- Combined with symptoms, other labs, and tests, it can help confirm a diagnosis.
ESR Erythrocyte sedimentation rate or ESR test. - An ESR test measures inflammation in the body by calculating the rate or how fast red blood cells settle to the bottom of a blood sample.
- If they settle faster than normal, the result is elevated ESR.
- That means the body is experiencing inflammation.
- ESR results may come back high, but these alone do not diagnose AS.
CRP C-reactive protein - CRP test. - A CRP test checks CRP levels, a protein associated with inflammation in the body.
- Elevated CRP levels signal inflammation or infection in the body.
- It is a useful tool for measuring disease progression after diagnosis.
- It often corresponds with changes in the spine shown on X-ray or MRI.
- Only 40-50% of individuals with ankylosing spondylitis experience an increased CRP.
ANA ANA test - Antinuclear antibodies, or ANA, go after the proteins in the cell's nucleus, telling the body its cells are the enemy.
- This activates an immune response that the body fights to eliminate.
- A study determined that ANA is found in 19% of individuals suffering from ankylosing spondylitis and is higher in women than men.
- Combined with other tests, the presence of ANA provides another clue to a diagnosis.
Gut Health - The gut microbiome plays an important role in triggering the development of ankylosing spondylitis and its treatment.
- Tests to determine the gut's health can give a doctor a complete picture of what is happening inside the body.
- Blood test diagnoses for ankylosing spondylitis and other inflammatory conditions rely heavily on piecing together different tests alongside clinical exams and imaging.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make your own healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Cardoneanu, Anca, et al. "Characteristics of the intestinal microbiome in ankylosing spondylitis." Experimental and therapeutic medicine vol. 22,1 (2021): 676. doi:10.3892/etm.2021.10108 Prohaska, E et al. "Antinukleäre Antikörper bei Spondylitis ankylosans (Morbus Bechterew)" [Antinuclear antibodies in ankylosing spondylitis (author's transl)]. Wiener klinische Wochenschrift vol. 92,24 (1980): 876-9. Sheehan, Nicholas J. "The ramifications of HLA-B27." Journal of the Royal Society of Medicine vol. 97,1 (2004): 10-4. doi:10.1177/014107680409700102 Wenker KJ, Quint JM. Ankylosing Spondylitis. [Updated 2022 Apr 9]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470173/ Xu, Yong-Yue, et al. "Role of the gut microbiome in ankylosing spondylitis: an analysis of studies in the literature." Discovery medicine vol. 22,123 (2016): 361-370.
Sports exercise headaches are exertion headaches that involve pain during or immediately after sports, exercise, or some physical activity. They come on quickly but can last a few minutes, hours, or days. Activities associated with exercise headaches include running, weightlifting, tennis, swimming, and rowing. Chiropractic, massage, decompression, and traction therapies can realign the body and relax the muscles allowing for optimal circulation and certain strategies to help prevent future episodes. Usually, there is no underlying disease or disorder, but it is recommended to talk to a healthcare provider to make sure. Sports Exercise Headaches When individuals exert their bodies intensely, they need added blood and oxygen, particularly with activities that involve tightening/tensing the abdominal muscles or increasing chest pressure. Doctors and scientists believe an exertional headache occurs when intense physical activity causes the veins and arteries to expand to circulate more blood. The expansion and increased blood circulation generate pressure in the skull that can cause pain. Alternate Triggers Exercising is not the only cause; other physical activities that can trigger an exertion headache include: - Sneezing
- Coughing
- Straining to use the bathroom
- Sexual intercourse
- Lifting or moving a heavy object
Symptoms Symptoms of a sports exercise headache include: - Neck stiffness or pain
- Pain on one or both sides of the head
- Pulsating pain discomfort
- Throbbing pain discomfort
- Shoulder tightness, discomfort, and/or pain
Sometimes individuals report the headache can feel like a migraine that could include: - Vision problems like blind spots
- Nausea
- Vomiting
- Light sensitivity
Most exercise headaches last five to 48 hours and can continue for three to six months. Diagnosis An underlying disease or disorder does not cause most exertional headaches. However, individuals experiencing severe or frequent headaches should consult their doctor or a healthcare provider. Tests will be ordered to rule out possible causes that include: If there is no underlying cause found, the medical provider can diagnose exertion headaches if there have been at least two headaches that: - Were caused by exercise or physical activity.
- Started during or after the physical activity.
- Lasted less than 48 hours.
Chiropractic Treatment According to the American Chiropractic Association, spinal adjustments are an effective headache treatment option. This includes migraines, tension headaches, or sports exercise headaches. Using the targeted approaches, chiropractic restores the body's natural alignment to improve function and alleviate stress on the nervous system. This allows the body to operate at optimal levels reducing muscle stress and muscle tension. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make your own healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References American Migraine Foundation. Secondary Headaches. (https://americanmigrainefoundation.org/resource-library/secondary-headaches/) Accessed 11/17/2021. Evans, Randolph W. "Sports and Headaches." Headache vol. 58,3 (2018): 426-437. doi:10.1111/head.13263 International Headache Society. HIS Classification ICHD-3. (https://ichd-3.org/other-primary-headache-disorders/4-2-primary-exercise-headache/) Accessed 11/17/2021. McCrory, P. "Headaches and exercise." Sports medicine (Auckland, N.Z.) vol. 30,3 (2000): 221-9. doi:10.2165/00007256-200030030-00006 National Headache Foundation. Exertional Headaches. (https://headaches.org/2007/10/25/exertional-headaches/) Accessed 11/17/2021. Ramadan, Nabih M. "Sports-related headache." Current pain and headache reports vol. 8,4 (2004): 301-5. doi:10.1007/s11916-004-0012-1 Trotta K, Hyde J. Exercise-induced headaches: prevention, management, and treatment. (https://www.uspharmacist.com/article/exerciseinduced-headaches-prevention-management-and-treatment) U.S. Pharm. 2017;42(1):33-36. Accessed 11/17/2021.
|
Can adding calisthenics resistance training to a fitness routine provide health benefits like flexibility, balance, and coordination? Calisthenics Resistance Training - Calisthenics resistance training requires no equipment, they can be done with minimal space, and are a great way to get a quick burn.
- They are a form of resistance training using your own body weight that is low-impact, which makes it accessible to individuals of all ages and fitness levels.
- They effectively help build agility, and cardiovascular health, and improve balance, coordination, and flexibility.
Benefits Muscle Strength Because calisthenics are easily adaptable to any fitness level, require minimal or no equipment, and are great for beginners and experienced exercise enthusiasts it is a fantastic full-body workout and an excellent way to build strength and muscle. Research supports that calisthenics resistance training can improve muscle strength in various ways. - One study found that eight weeks of calisthenics not only improved posture and body mass index/BMI but can impact strength, even with exercises not routinely performed. (Thomas E, et al., 2017)
- During the study, one group did calisthenics and the other maintained regular training routines.
- The researchers discovered that the group that did calisthenics increased their repetitions of exercises that were not included.
- The group who continued with their regular training routines did not improve on what they could do before the eight-week study. (Thomas E, et al., 2017)
Cardiovascular Fitness - Regular participation in calisthenic resistance training can lead to improved cardiovascular health, including increased endurance and a healthier heart.
- Certain calisthenic exercises, like burpees and mountain climbers, are high-intensity movements that can increase heart rate and blood circulation just from the movements.
- Gradually performing these exercises at a faster pace, research indicates could potentially experience the same cardiovascular benefits from interval or treadmill running. (Bellissimo GF, et al., 2022) - (Lavie CJ, et al., 2015)
Balance, Coordination, and Flexibility - The movements require a full range of motion that stretches and strengthens the muscles, tendons, and ligaments.
- These exercises can help decrease the risk of injury and make daily physical activities easier to perform without over-exertion.
- Incorporating calisthenics resistance training on a regular basis can help improve posture, balance, and flexibility, depending on which exercises are recommended.
- Exercises like stretches, lunges, and squats help to improve flexibility and mobility.
- Exercises like single-leg squats and one-arm push-ups can work the balance, coordination, and proprioception of the body.
Mental Health - Exercise, in general, is known to improve mood, reduce stress, and improve overall well-being.
- Calisthenic resistance training can have additional impacts on mental well-being.
- For example, the discipline and focus required to perform the movements can help concentration and mental clarity.
- One study found that calisthenics can reduce cognitive decline and may be useful for dementia prevention. (Osuka Y, et al., 2020)
- Another study found that calisthenics helped mental well-being in individuals with diseases like ankylosing spondylitis and multiple sclerosis. (Taspinar O, et al., 2015)
Types Bodyweight exercises that use an individual's own body weight as resistance are the foundation. Common examples include push-ups, squats, and lunges. An overview of some of the types of exercises. Pulling - These exercises focus on training the muscles for pulling movements, which include the back, shoulders, and arms.
- Examples include pull-ups, chin-ups, and rows.
Pushing - These exercises focus on training the muscles for pushing movements, like the chest, shoulders, and triceps.
- Examples include dips, push-ups, and handstand push-ups.
Core - Core exercises focus on training the abdominal and lower back muscles, which are responsible for maintaining stability and balance.
- Examples of core exercises include planks, sit-ups, and leg raises.
Single-Leg - Single-leg exercises focus on training one leg at a time.
- These target the muscles of the legs, hips, and core.
- Examples of single-leg exercises include single-leg squats, lunges, and step-ups.
Plyometric - Calisthenics resistance training focuses on powerful explosive movements.
- Plyometric exercises challenge the muscles to work quickly and forcefully.
- Examples include jump squats, clap push-ups, and box jumps.
Getting Started - Start by making sure calisthenics is an appropriate workout option, especially if you are a beginner or have pre-existing medical conditions.
- Once cleared to exercise start with familiar movements that can be done with the correct form.
- Pushups, bodyweight squats, planks, lunges, and other basic movements are a good place to start.
- Make sure to warm up with light and easy motions that mimic the workout movements.
- Aim to work each body part during the workout.
- Try for at least two workouts a week.
- It is recommended to split the movement patterns.
- Reps can be counted or set a timer to switch exercises every minute. This is called EMOM-style or every minute on the minute.
- Pick four to five exercises that target various areas.
- For example, sit-ups can be done for the core, lunges for the glutes and thighs, planks can be done for the shoulders and core, and jumping jacks or jumping rope for cardiovascular.
- Calisthenic resistance training is easily modifiable and can be adjusted to individual needs.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Thomas, E., Bianco, A., Mancuso, E. P., Patti, A., Tabacchi, G., Paoli, A., ... & Palma, A. (2017). The effects of a calisthenics training intervention on posture, strength, and body composition. Isokinetics and exercise science, 25(3), 215-222. Bellissimo, G. F., Ducharme, J., Mang, Z., Millender, D., Smith, J., Stork, M. J., Little, J. P., Deyhle, M. R., Gibson, A. L., de Castro Magalhaes, F., & Amorim, F. (2022). The Acute Physiological and Perceptual Responses Between Bodyweight and Treadmill Running High-Intensity Interval Exercises. Frontiers in physiology, 13, 824154. https://doi.org/10.3389/fphys.2022.824154 Osuka, Y., Kojima, N., Sasai, H., Ohara, Y., Watanabe, Y., Hirano, H., & Kim, H. (2020). Exercise Types and the Risk of Developing Cognitive Decline in Older Women: A Prospective Study. Journal of Alzheimer's disease: JAD, 77(4), 1733–1742. https://doi.org/10.3233/JAD-200867 Taspinar, O., Aydın, T., Celebi, A., Keskin, Y., Yavuz, S., Guneser, M., Camli, A., Tosun, M., Canbaz, N., & Gok, M. (2015). Psychological effects of calisthenic exercises on neuroinflammatory and rheumatic diseases. Zeitschrift fur Rheumatologie, 74(8), 722–727. https://doi.org/10.1007/s00393-015-1570-9 Lavie, C. J., Lee, D. C., Sui, X., Arena, R., O'Keefe, J. H., Church, T. S., Milani, R. V., & Blair, S. N. (2015). Effects of Running on Chronic Diseases and Cardiovascular and All-Cause Mortality. Mayo Clinic Proceedings, 90(11), 1541–1552. https://doi.org/10.1016/j.mayocp.2015.08.001
Pickleball is a growing, increasingly popular sport that can be enjoyed by individuals of every age and fitness level. It combines elements of tennis and badminton at a slightly slower pace that makes it ideal for families and provides excellent health benefits and enjoyable socializing. It is easy to learn and requires little practice. The sport is easy on the body and is a great activity for seniors because it is joint-friendly. Pickleball Individuals do not need to be athletes or belong to a certain age group to play or benefit from the sport. It requires minimal equipment and a few basic skills. Using a flat paddle and a plastic pickleball, opponents singles or doubles play a game like tennis or badminton. Playing the Game - A three-foot-long net is set up in the center of a court measuring 44 feet long by 20 feet wide.
- The court is divided between right and left service zones.
- If the receiving side misses the serving side volley, the serving side receives a point.
- The game is played to 11 points, but a player or team must win by two points.
- The ball's design keeps the pace manageable and user-friendly.
- Pickleball has other intricacies common with other racket-court sports.
- The player serves from a specific side.
- The no-volley zone, or the kitchen is seven feet from the net on both sides.
- There are rules regarding when the player must call the score, how tournaments work, and variations between singles and doubles matches.
- Most players only need a few games to pick up the basics.
Reasons To Play The sport offers a number of health benefits. Improves Mental Health - One study found individuals who played pickleball tended to have better mental health and outlook.
- Researchers followed older adults competing in pickleball competitions and tournaments.
- At the end of the study, the researchers found that a commitment to a physical hobby correlated to reduced depression levels.
Improves Cardiovascular Health - The sport is not as physically intense as say tennis, but offers significant benefits for cardiovascular health.
- One study found that individuals who played three times a week for an hour had improved cardiorespiratory fitness, lower cholesterol levels, and decreased blood pressure.
- Experts found that it is a healthy alternative to traditional exercises like walking or biking.
Improved Hand-Eye Coordination - Pickleball will improve hand-eye coordination and reflexes.
- Coordinating the feet, legs, arms, hands, and eye movements quickens responses, challenges the brain to think fast, and increases balance.
- Physical activity combined with cognitive challenges has been found to improve cognitive health and prevent mental decline in older adults.
Socialization - Pickleball requires an opponent or two for doubles matches.
- A significant benefit is that the sport provides increased socialization.
- Socializing with others, especially the elderly can help with loneliness.
- Loneliness can negatively impact physical and mental health, increasing the risk of heart disease, stroke, dementia, and depression.
Getting Started Individuals need minimal gear like paddles, shoes, and balls and knowledge to get started playing. One of the easiest ways to begin is locating a court in the community. This is a great physical activity that can be competitive, but overall it is fun, easy to play, and provides great health benefits. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Casper, Jonathan M, and Jung-Hwan Jeon. “Psychological Connection to Pickleball: Assessing Motives and Participation in Older Adults.” Journal of Aging and physical activity, 1-6. 24 Oct. 2018, doi:10.1123/japa.2017-0381 Cerezuela, Juan-Leandro, et al. “Pickleball and mental health in adults: A systematic review.” Frontiers in psychology vol. 14 1137047. 21 Feb. 2023, doi:10.3389/fpsyg.2023.1137047 Ryu, Jungsu, et al. “Pickleball, Personality, and Eudaimonic Well-Being in Middle-Aged and Older Adults.” Journal of Aging and physical activity vol. 30,5 885-892. 14 Feb. 2022, doi:10.1123/japa.2021-0298 Vitale, Kenneth, and Steven Liu. “Pickleball: Review and Clinical Recommendations for this Fast-growing Sport.” Current sports medicine reports vol. 19,10 (2020): 406-413. doi:10.1249/JSR.0000000000000759 Webber, Sandra C et al. “Physical Activity Intensity of Singles and Doubles Pickleball in Older Adults.” Journal of Aging and physical activity vol. 31,3 365-370. 10 Sep. 2022, doi:10.1123/japa.2022-0194
Working out on a treadmill is a great way to get cardiovascular exercise when unable to go outside or to change things up. However, it's not just about getting on the machine and walking or running. Like anything, proper form and posture are important in preventing injuries. This allows the individual to walk smoother and faster, burn more calories, and get the full benefits. Individuals with a medical condition that impacts posture or makes it difficult to walk on a treadmill should speak to a healthcare provider for recommendations to ensure they can work out without aggravating the condition or putting themselves at risk. There is an option of working with a physical or occupational therapist to address any concerns individuals may have about using a treadmill. Treadmill Walking Exercise Errors Safety A common error is getting on a treadmill with the belt already running. This may seem unnecessary, but many accidents happen when individuals just jump on. To avoid injuries, it is recommended to follow these safety tips. - Make sure the machine is off.
- Know where the emergency stop switch is.
- Stand next to the base/running deck.
- Clip the safety key to your body to stop the treadmill if you slip or stumble.
- Start the treadmill and set it to slow speed.
- Look at the speed and carefully get onto the moving tread.
- Gradually increase the speed once comfortably on board.
Wrong Shoes A healthy step is to strike with the heel in front with the forward foot slightly off the surface. The foot then rolls from heel to toe; by the time the toe is on the ground, the individual is halfway into the next step, and the forward foot is now the rear foot and ready for the toes to push off to take the next step. - This sequence is only possible with flexible shoes.
- Wearing stiff shoes may not allow for the roll-through.
- Stiff shoes force the foot to slap down.
- The body and walking stride become a flat-footed stomp.
- Take a few minutes during a walking session to think about what the feet are doing.
- Ensure they strike with the heel, roll through the step, and the rear foot provides an adequate push-off.
- If you cannot do this in your present shoes, then it's time to look at other flexible walking/running shoes.
Holding The Handrails - The handrails provide stability, but natural walking posture or natural movement involves a healthy stride and arm motion.
- Constantly holding onto the handrails doesn't allow for this motion.
- Walking or running at a slower pace is recommended without using the handrails.
- Individuals will get a better workout at a slower pace than they would at a faster rate holding on to the rails.
- Individuals with a disability or balance issues may need the handrails and should consult a trainer or physical therapist for healthy workout recommendations.
Leaning Forward Proper walking posture means the body is upright, not leaning forward or backward. - Before stepping onto the treadmill, check and readjust your posture.
- Engage the abdominals and maintain a neutral spine.
- Give the shoulders a backward roll so they are not hunched up.
- Get on the treadmill and walk.
- Remind yourself to maintain this upright posture.
- When changing pace or incline, check your posture again.
Looking Down and Not Ahead - A healthy walking posture means the head is up and the eyes forward.
- An unhealthy walking posture can lead to neck, shoulder, and low back pain.
- Improper posture doesn't allow the body to take full, complete breaths.
- It also reinforces unhealthy sitting postures.
- Check the shoulders and do a backward roll every few minutes to ensure they aren't hunching forward.
Overstriding - Overstriding means the front heel hits the ground too far in front of the body.
- Many individuals do this to walk faster.
- An overstride can result in the foot slipping, which can cause a trip and/or a fall.
- A healthy walking stride means the front heel strikes close to the body while the back foot stays on the ground longer to provide a powerful push-off.
- This push-off provides more speed and power and works the muscles better to burn more calories.
- You may need to shorten the stride and take shorter steps when beginning.
- Then focus on feeling the back foot and getting a thorough push with each step.
- Focus on this for a few minutes each session until it becomes familiar and walking becomes faster and easier.
No Arm Movement - If the handrails are not necessary, the arms should be moving during the workout.
- Proper arm motion allows the body to go faster and burn more calories.
- The swinging motion can help shoulder and neck problems developed from unhealthy postures.
- The legs only move as fast as the arms do.
- To speed up the legs, speed up the arms.
Going Too Fast - Go only as fast as the body can go while maintaining proper walking posture and form.
- If overstriding, leaning forward, or hunching shoulders begin to present, slow down until a comfortable/maintainable speed that allows the body to walk correctly is found.
- If the workout doesn't feel like it's helping
- Individuals with a bad walking form at high speeds may consider adding running intervals.
- Running will create quick bursts of higher heart rate and change form.
Running Intervals - Warm up at a slow speed for 3 to 5 minutes.
- Increase walking speed to a fast pace that can maintain proper walking form.
- Start a jog and increase the speed to match the jogging pace.
- Jog for 1 to 3 minutes.
- Return to the fast walking pace for 3 to 5 minutes.
- Jog for 1 to 3 minutes.
- Repeat until the end of the workout.
- Finish with 3 to 5 minutes at an easy walking pace to cool down.
Challenge Yourself When the body has fully adapted to a workout, it's time to challenge the body to achieve greater fitness and stay motivated. This is where workout variation intensity, duration, frequency, and/or mode come into play. Intensity - Add intensity by increasing the incline or the speed.
Duration - Increase the time spent on the treadmill.
- If spending 30 minutes for several weeks, increase to 45 minutes for at least one weekly session.
- After a couple of weeks, increase to 60 minutes.
Frequency - Once the body is used to treadmill walking, try to incorporate a session every day or every other day.
- Walk at a brisk pace for 30 to 60 minutes, going for a total of 150 to 300 minutes per week.
Type of Exercise - Try jogging or running.
- Alternate using the exercise bike, rowing machine, or stair climber.
- Add weight training, circuit training, or anything enjoyable that gets the body moving in different ways.
Set goals and get into the habit of using the treadmill regularly to reap all the benefits. Avoid common treadmill errors, stay safe, and make the most out of walking and running workouts. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Centers for Disease Control and Prevention. Benefits of Physical Activity. Donlin, Margo C et al. "Adaptive treadmill walking encourages persistent propulsion." Gait & Posture vol. 93 (2022): 246-251. doi:10.1016/j.gaitpost.2022.02.017 Donlin, Margo C et al. "User-driven treadmill walking promotes healthy step width after stroke." Gait & Posture vol. 86 (2021): 256-259. doi:10.1016/j.gaitpost.2021.03.031 Hashiba, M. "Transient change in standing posture after linear treadmill locomotion." The Japanese Journal of Physiology vol. 48,6 (1998): 499-504. doi:10.2170/jjphysiol.48.499 Liang, Junjie et al. "The effect of anti-gravity treadmill training for knee osteoarthritis rehabilitation on joint pain, gait, and EMG: Case report." Medicine vol. 98,18 (2019): e15386. doi:10.1097/MD.0000000000015386 MacEwen, Brittany T et al. "A systematic review of standing and treadmill desks in the workplace." Preventive medicine vol. 70 (2015): 50-8. doi:10.1016/j.ypmed.2014.11.011
Healthy aging has been linked to a lifestyle consisting of proper nutrition and exercise. However, even with a healthy lifestyle, the body undergoes changes that include conditions, disease, and compromises in physical performance. Because of the effects of aging on muscle and joint tissue, cardiovascular fitness, and other physical parameters, older athletes need to take consideration, but this doesn't mean slowing down. Injury Medical Chiropractic and Functional Medicine Clinic can develop a training and treatment plan to build and maintain musculoskeletal system health, flexibility, and optimal function. Older Athletes Research has shown that the physical and mental declines that go with aging can be reduced with fitness and nutrition programs and that it is not too late to start improving fitness, no matter what age. Systemic changes that happen to an aging body include: Nervous System - Imbalances happen more easily and more often.
- Sensation changes.
Musculoskeletal System - Bone Strength Decreases.
- Muscle Strength Decreases.
- Flexibility issues occur more frequently.
Respiratory System - Decreased Vital or Breathing Capacity of Lungs - The maximum amount of air that can be exhaled after a full inhalation.
Cardiovascular System - Maximum Heart Rate slows down.
- A slower return to resting heart rate after and during physical activity and exercise.
Maintaining Endurance Common aging fitness declines include: - Changes in body composition.
- Increased body fat.
- Decreased muscle mass.
- Loss of height - can be brought on by osteoporosis.
- Diminished cardiorespiratory capacity.
- Muscle atrophy.
Research has found that when seniors start to exercise, their health improves quickly. It's estimated that the physical declines associated with aging are not necessarily inevitable but can also happen by losing fitness/deconditioning effects from reduced exercise levels, frequency, and/or intensity. Despite the losses, older athletes are often able to compete and excel in endurance activities because they tend to have higher proportions of slow twitch fibers. Memory and Fitness - Evidence suggests that seniors who exercise reduce the physical effects of aging and prevent their brain/memory from advanced degeneration.
- Physical fitness has been linked with reduced memory decline in middle-aged adults.
Training Options Training methods to maintain athletic performance. Hill Running or Interval Training - This type of training can improve fitness and condition the aerobic and anaerobic systems.
Weight Training - Weight training maintains muscle tone, fast twitch muscle fibers, and strength.
Plyometric exercises Creatine Supplements - Supplements may help improve performance during repetitive, intense exercise sessions.
Nutrition Aging causes the joints to become less flexible, resulting in a range of motion loss leading to limitations and compromised physical abilities. Proper nutrition in older athletes can protect the joints and prevent advanced degeneration. The following nutrients are recommended: - Omega-3's - nuts, seeds, and fatty fish provide anti-inflammatory effects.
- Vitamin C for collagen production.
- Sulfur amino acids - certain vegetables, meat, poultry, fish, and dairy products improve joint cartilage health.
- Bioflavonoids - all fruit and vegetables provide anti-inflammatory effects and improved circulation.
- Antioxidants - selenium and vitamin E protect against free radicals that multiply with age.
- Supplements may also be helpful but check with a doctor before beginning a program.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Gillis, Angela, and Brenda MacDonald. "Deconditioning in the hospitalized elderly." The Canadian nurse vol. 101,6 (2005): 16-20. Lexell, J. "Human aging, muscle mass, and fiber type composition." The Journal of Gerontology. Series A, Biological Sciences and medical sciences vol. 50 Spec No (1995): 11-6. doi:10.1093/gerona/50a.special_issue.11 Marriott, Catherine F S, et al. "High-Intensity Interval Training in Older Adults: a Scoping Review." Sports medicine - open vol. 7,1 49. 19 Jul. 2021, doi:10.1186/s40798-021-00344-4 Rogers, Michael E et al. "Balance training for the older athlete." International Journal of sports physical therapy vol. 8,4 (2013): 517-30. Tayrose, Gregory A et al. "The Master's Athlete: A Review of Current Exercise and Treatment Recommendations." Sports Health vol. 7,3 (2015): 270-6. doi:10.1177/1941738114548999 Townsend, Danyelle M et al. "Sulfur-containing amino acids and human disease." Biomedicine & pharmacotherapy = Biomedicine & pharmacotherapy vol. 58,1 (2004): 47-55. doi:10.1016/j.biopha.2003.11.005 Van Roie, Evelien, et al. "An age-adapted plyometric exercise program improves dynamic strength, jump performance and functional capacity in older men either similarly or more than traditional resistance training." PloS one vol. 15,8 e0237921. 25 Aug. 2020, doi:10.1371/journal.pone.0237921 Wu, Tingting, and Yanan Zhao. "Associations between functional fitness and walking speed in older adults." Geriatric nursing (New York, N.Y.) vol. 42,2 (2021): 540-543. doi:10.1016/j.gerinurse.2020.10.003
Mountain biking is a recommended sport for building muscle power and strength, endurance, and agility. Mountain biking uses bicycles designed to ride off-road and over rough terrain. The sport requires core strength, endurance, balance, and self-reliance. This is because riders are often far from civilization. Riders must learn to repair broken bike parts and fix flat tires to avoid being stranded. Mountain biking gear that riders carry includes a heavy-duty backpack with plenty of water, food, tools for repairs, and a first aid kit. Using the appropriate gear and equipment will help make the next ride safer and more comfortable. Mountain Biking Gear The first piece of equipment is a properly fitting and well-maintained mountain bike. There are all types of bicycles for every type of rider and trail. There are variations of bikes with full suspension, front suspension, disc brakes, V-brakes, different wheel sizes, and frame materials. It is recommended to consult a professional or visit a bicycle shop specializing in mountain biking to match the individual with the best bike. The right bike makes for a better ride. Brakes - Disc brakes offer more secure braking when going high speed and needing the option to stop safely and at the proper distance.
Frame Size - The bike's frame must be properly set up so the individual can easily step over and pedal at the correct height.
Suspension - Individuals that plan on taking on all kinds of terrains need the bike to absorb the shock and impact and are recommended to consider a full-suspension bike or one with a suspension fork.
Wheels - Mountain bike wheels range in size from 26 to 29 inches, and depending on the terrain and speeds, the right wheel diameter is key.
- Larger wheels accelerate slower but provide improved traction.
- Smaller wheels are lighter and easier to maneuver.
Helmet A helmet is the most important safety gear that significantly reduces the severity of head injuries; no one should ride without one. Mountain bike helmets generally have a visor to help block the sun when riding so individuals can focus on the trail and not be distracted by glare. Three styles of mountain bike helmets are available, depending on the type of activity. XC or Cross Country - Cross-country helmets provide ventilation, are open-faced, and are lightweight.
- These helmets are recommended for long rides.
Trail - A trail mountain biking helmet covers part of the face and has a visor to help protect the head from the sun and other weather elements.
- Trail helmets are recommended for mountain biking, road, and trail cycling.
Full-Face - Full-face helmets are essential for downhill trails at high speeds and on varying terrains.
- They feature an adjustable visor and chin protection for added safety.
Eye Protection - Eye protection helps keep dirt, dust, and debris out of the eyes and helps have clear vision in dark shadows and bright sunlight.
- Glasses or goggles protect the eyes if not using a full-face helmet.
- Choosing a frame with an interchangeable lens system that comes with different lenses for varying light conditions is recommended.
Hydration Pack - Wearing a hydration pack when riding provides easy access to hands-free hydration.
- This is important for anyone exercising for more than two hours and with limited access to refills on the trail.
Mountain Biking Shoes - Beginners can wear comfortable sports shoes when starting.
- Riders who begin riding more frequently will eventually want to transition to mountain biking shoes.
- Cleated bike shoes work with pedals and lock the rider's feet to the bike.
- There is a variety of cycling footwear, but all-mountain bike shoes provide thorough traction off the bike, durability, comfort, and a heavy-duty sole for optimal pedaling efficiency.
Clipless Pedals - Clipless pedals are recommended for cross-country trail riding.
- Cycling shoes and clipless pedal systems lock the shoes into the pedals for secure and efficient pedaling and can be unclipped easily with a twist of the foot.
- Use shoes and pedals that work together.
Gloves - Mountain bike gloves provide additional padding and finger coverage.
- They absorb the shock and protect the hands from falls on rough terrain.
- The handlebar grips are padded, but additional cushion from the gloves is beneficial for long or downhill rides for extra comfort and protection.
- Full-finger gloves offer the best coverage, protection, and grip on the brake levers.
Padded Bike Shorts - Padded and protective bike shorts offer benefits for riding long distances and over rough terrain.
- These shorts provide a padded inner liner like underwear that increases comfort and reduces chafing.
- The exterior looks like a baggy pair of shorts made of tough, abrasion-resistant fabric to take the wear and tear.
Bicycle Repair Kit - A repair kit can be attached to the bike saddle and holds all the essential tools for mechanical trouble or a flat tire.
- The repair kit should include a bicycle multi-tool, an extra tube and patch kit, tire levers, a mini pump, and emergency cash.
- Riders should keep an identification card with a list of contact numbers in the seat bag in case of a serious injury or other emergencies.
First Aid Kit - Riders can lose traction on loose rock and crash on the trail.
- A first aid kit with various bandages, tape, pain relievers, and antiseptic wipes to treat cuts, scrapes, blisters, rashes, and everything in between is highly recommended.
- Also include an eye drop solution, a small pocketknife, moleskin, energy gels, and an emergency whistle.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Alena Høye, Bicycle helmets – To wear or not to wear? A meta-analysis of the effects of bicycle helmets on injuries, Accident Analysis & Prevention, Volume 117, 2018, Pages 85-97, ISSN 0001-4575, https://doi.org/10.1016/j.aap.2018.03.026. Ansari, Majid, et al. "Mountain Biking Injuries." Current sports medicine reports vol. 16,6 (2017): 404-412. doi:10.1249/JSR.0000000000000429 Clark, Gregory, et al. "Do Mountain Bikers Know When They Have Had a Concussion and, Do They Know to Stop Riding?." Clinical Journal of sports medicine: official journal of the Canadian Academy of Sports Medicine vol. 31,6 (2021): e414-e419. doi:10.1097/JSM.0000000000000819 Hall, Cougar et al. "Pedal-Assist Mountain Bikes: A Pilot Study Comparison of the Exercise Response, Perceptions, and Beliefs of Experienced Mountain Bikers." JMIR formative research vol. 3,3 e13643. 13 Aug. 2019, doi:10.2196/13643 Impellizzeri, Franco M, and Samuele M Marcora. "The physiology of mountain biking." Sports medicine (Auckland, N.Z.) vol. 37,1 (2007): 59-71. doi:10.2165/00007256-200737010-00005 Kronisch, R.L., Pfeiffer, R.P. Mountain Biking Injuries. Sports Med 32, 523–537 (2002). https://doi.org/10.2165/00007256-200232080-00004
The body adapts differently to different types of exercise. Aerobic, cardio, and endurance all refer to activities stimulating heart and breathing rates to provide the muscles with oxygenated blood. The oxygen is delivered by blood pumped from the heart through the arteries and returns to the heart through the veins. This explains all the heavy breathing during workouts. Aerobic exercise increases energy production in the muscle cells and blood delivery in the cardiovascular system. Aerobic Exercise Health The Heart All the muscles get to rest on and off when in use. The heart is a unique muscle that pumps blood through the body that never gets time off. This is why it is important to strengthen the heart. With aerobic exercise, the heart's chamber/left ventricle gets larger, producing more blood per pump to the rest of the body. This improves cardiac output for the blood pumped by the heart per minute. When the heart is stronger, pumping more blood per beat means it doesn't have to beat as rapidly. A lower resting heart rate is associated with a reduced risk of cardiovascular disease and promotes long and healthy life. Vascular Each time the heart beats, blood pumps from the left ventricle into the aorta and flows into a branching vessel network. Every artery in the body provides resistance to the circulation that the heart pushes against. The resistance provided can vary, depending on overall health and health conditions. - Aerobic exercise training reduces the workload by reducing arterial stiffness.
- Aerobic exercise increases heart rate, pushing more blood through the arteries.
- The inner wall of the arteries recognizes the increased blood flow causing the arteries to widen.
- With regular training, the arteries acclimate and become more effective at expanding with each rush of blood.
- No aerobic activity can cause the arteries to stiffen, causing circulation problems.
- Increased arterial stiffness is associated with coronary artery plaque development.
- Aerobic exercise impacts the vascular system by promoting capillary growth.
- Capillaries are microscopic vessels where oxygen diffuses from red blood cells to the muscle and other cells.
- The body stimulates a molecule called vascular endothelial growth factor to grow additional capillaries to regulate energy demand more efficiently.
- Older individuals benefit from aerobic activity similarly to young individuals.
Metabolic Along with cardiovascular benefits, aerobic exercise increases the muscles’ energy production. The energy is produced in muscle cells primarily through an oxidative energy system. Oxidative energy production takes place within cells called mitochondria. Once blood delivers oxygen to the muscle cells, it can be used to produce energy that powers the muscles. - Aerobic exercise training improves the muscle cells’ ability to burn fat by generating more mitochondria and enhancing functionality.
- Following each training session, the body burns more fat than usual.
- Aerobic training can increase resting metabolic rate, resulting in more calories burned.
- It can increase post-exercise oxygen consumption/EPOC, resulting in increased calorie burn after training in addition to calories burned during exercise.
Muscle The muscles adapt from aerobic training. Muscles are made up of various fiber types. - Aerobic exercise training primarily influences type 1 fibers, known as slow-twitch fibers.
- The name comes from the proteins responsible for their contractions.
- Relative to type 2a fibers/fast-twitch, type 1 fibers contract more slowly but have an increased capacity to contract over and over for longer.
- Aerobic training results in hypertrophy of type 1 muscle fibers by adding more slow-twitch proteins.
Strengthening the heart and making arteries more flexible directly impacts health and physical function. Aerobic exercise strengthens and trains the heart to circulate blood efficiently. Injury Medical Chiropractic and Functional Medicine Clinic can develop a personalized health plan for your needs. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Arbab-Zadeh, Armin, et al. “Cardiac remodeling in response to 1 year of intensive endurance training.” Circulation vol. 130,24 (2014): 2152-61. doi:10.1161/CIRCULATIONAHA.114.010775 Gavin, Timothy P et al. “No difference in the skeletal muscle angiogenic response to aerobic exercise training between young and aged men.” The Journal of physiology vol. 585, Pt 1 (2007): 231-9. doi:10.1113/Physiol.2007.143198 Hellsten, Ylva, and Michael Nyberg. “Cardiovascular Adaptations to Exercise Training.” Comprehensive Physiology vol. 6,1 1-32. 15 Dec. 2015, doi:10.1002/cphy.c140080 Nauman, Javaid, et al. “Temporal changes in resting heart rate and deaths from ischemic heart disease.” JAMA vol. 306,23 (2011): 2579-87. doi:10.1001/jama.2011.1826 Popel, A S. “Theory of oxygen transport to tissue.” Critical reviews in biomedical engineering vol. 17,3 (1989): 257-321. Seals, Douglas R et al. “Aerobic exercise training and vascular function with aging in healthy men and women.” The Journal of physiology vol. 597,19 (2019): 4901-4914. doi:10.1113/JP277764
Introduction Dr. Jimenez, D.C., presents how to implement exercise as part of your daily routine. Many factors and lifestyle habits tend to take over our daily lives, and in this 2-part series, we will look at how to implement exercise in a clinical setting. Part 2 will continue the presentation. We mention our patients to certified medical providers that provide available therapy treatments for individuals suffering from chronic conditions associated with Lyme disease. We encourage each patient when it is appropriate by referring them to associated medical providers based on their diagnosis or needs. We understand and accept that education is a marvelous way when asking our providers’ crucial questions at the patient’s request and acknowledgment. Dr. Alex Jimenez, D.C., uses this information as an educational service. Disclaimer How To Implement Strategies? Dr. Alex Jimenez, D.C., presents: Today we will discuss how to implement strategies using exercise as a prescription. Remember, just like we talked about how a healthy diet full of nutritious, whole foods can be used as a prescription, we want this science to make it to the patient and create outcomes because otherwise, this is just a bunch of things you know and not something that you know how to put into practice. So we’ve listened; we know that’s what you’re up to, so let’s get started. We will discuss some general aspects of implementing exercise as a prescription and some ideas we use in our practice. And then, of course, share the brilliant ideas with some of the other colleagues who also are figuring out ways to make this work in their practice. The first thing we want to share with you is when you’re approaching a patient with an exercise prescription, assuming the patient’s interested, you should ascertain first how this person is motivated. Because it always makes sense to ride their motivation wave than to come from the standpoint that this is what I want from you, and this is why you need to do it. The first thing we want to put out there is that you want to ensure that this patient has a reason to want to exercise. So it’s less about a doctor’s orders or a provider’s recommendation, and you want to partner with our patients therapeutically, which means understanding their motivation. So for most people, there are two ways we can reinforce the outcome of a positive implementation of the exercise. First, we want to optimize those factors related to one-on-one communication with our patients. And then, number two, optimize the environment in our practice for success. Okay, so we’ll go over these things in detail now. It only sometimes works if we give them a prescription and assume they want to do it. So if Joan Rivers was your patient in the past, this might have been her reason for not wanting to exercise, and you must be able to roll with it. Let’s talk about how we can do that. This works with patients, spouses, and children; it is wise to persuade people to do things and make them think it is their idea. So, with much bigger goals in mind, Nelson Mandela used the same principle. So we want you to think about who you are working with and who you are partnering with; these are some common functional medicine personas that you may come across, especially if you’re in more of a private practice, whether it’s cash or membership type of practice, you might see this persona in people. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
The body needs to be flexible to maintain a full range of motion. Stretching keeps the muscles supple, strong, and healthy; without it, the muscles shorten and become stiff and tight. Then, when the muscles are needed, they are weak and unable to extend fully. This increases the risk of joint pain, strains, injuries, and muscle damage. For example, sitting in a chair for a long time results in tight glute muscles and hamstrings, which leads to back discomfort symptoms and inhibits walking. Injury Medical Chiropractic and Functional Medicine Clinic can help individuals develop a personalized stretching program to maintain smooth mobility, flexibility, and function. Stretching Objective Benefits The body needs to be flexible to maintain mobility, balance, and independence. The benefits of regularly stretching include: - Muscles function at optimal levels.
- Maintains muscle length.
- Maintains muscle strength.
- Increased blood circulation.
- Endorphin release.
- Parasympathetic activation.
- Relieves stress.
- Natural toxin removal.
- Relieves body aches and soreness.
- Improves ability and performance in physical activities.
- Reduces the risk of injuries.
- Improves posture.
Important Areas The areas critical for mobility include: - Lower back/waistline
- Hip flexors
- Hamstrings
- Quadriceps in the front of the thigh.
- Calves
- Neck
- Shoulders
Stretch Reflex When the muscles are stretched, so are the muscle spindles. The spindle records the change in length and speed and transmits the signals through the spinal cord, which conveys the information. This triggers the stretch reflex, which tries to resist the change by causing the stretched muscle to contract. Muscle spindle function helps maintain muscle tone and protects the body from injury. One of the reasons for holding a stretch for a specific amount of time is because, as the muscle stays in a stretched position, the spindle acclimates to the new condition and reduces its resistance signaling, gradually training the stretch receptors to allow greater lengthening of the muscles. Chiropractic Stretch Training However, stretching once won't generate maximum flexibility. Tight muscles may have taken months or years to develop; therefore, it will take time to achieve flexibility and must be continually worked on to maintain it. Chiropractors and physical therapists are body movement experts and can assess individual muscle strength and develop a customized stretching program. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Bhattacharyya, Kalyan B. "The stretch reflex and the contributions of C David Marsden." Annals of Indian Academy of Neurology vol. 20,1 (2017): 1-4. doi:10.4103/0972-2327.199906 Behm, David G et al. "Acute effects of muscle stretching on physical performance, range of motion, and injury incidence in healthy active individuals: a systematic review." Applied physiology, nutrition, and metabolism = Physiologie applique, nutrition et metabolism vol. 41,1 (2016): 1-11. doi:10.1139/apnm-2015-0235 Berg, K. Stretching fundamentals. In: Prescriptive Stretching. 2nd ed. Kindle edition. Human Kinetics; 2020. da Costa, Bruno R, and Edgar Ramos Vieira. "Stretching to reduce work-related musculoskeletal disorders: a systematic review." Journal of rehabilitation medicine vol. 40,5 (2008): 321-8. doi:10.2340/16501977-0204 Page, Phil. "Current concepts in muscle stretching for exercise and rehabilitation." International journal of sports physical therapy vol. 7,1 (2012): 109-19. Witvrouw, Erik, et al. "Stretching and injury prevention: an obscure relationship." Sports medicine (Auckland, N.Z.) vol. 34,7 (2004): 443-9. doi:10.2165/00007256-200434070-00003
Introduction When exercising, it is very important to warm each muscle group to prevent injuries from occurring when working out. Stretching the arms, legs, and back can loosen up stiff muscles and increase blood flow to allow each muscle fiber to warm up and allow maximum power when each set is performed. One of the best ways to reduce muscle fatigue or stiffness before working out is to foam roll each muscle group for at least 1-2 minutes max to provide optimal functionality. Foam rolling allows the muscles to warm up before an extensive workout session. Still, it can also offer many benefits when combined with other therapies to reduce pain-like symptoms like trigger point pain from causing further injuries from reoccurring in the body. Today’s article focuses on the benefits of foam rolling, how it reduces trigger point pain, and how it is combined with chiropractic care to achieve optimal health and wellness. We refer patients to certified providers incorporating techniques and therapies for individuals dealing with trigger point pain affecting different body areas. By locating where the trigger points are coming from, many pain specialists utilize a treatment plan to reduce the effects that trigger points are causing on the body while suggesting different tools, like using a foam roller to reduce pain in the other muscle groups. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a terrific way when asking our providers intricated questions at the patient’s request and understanding. Dr. Jimenez, D.C., only utilizes this information as an educational service. Disclaimer The Benefits Of Foam Rolling Have you been dealing with pain-like symptoms in different parts of your body? Do you feel stiffness in your muscles? Or have you been feeling exhausted throughout the entire day? Many people often feel stressed, overworked, and exhausted after a long day and need to find different ways to relieve stress. Whether going to the gym to work out or yoga class, many people should warm up for about 5-10 minutes to work out each muscle group to reduce muscle fatigue and stiffness. One of the tools that people should utilize is using a foam roller. Studies reveal that foam rolling before working out can improve muscle performance and flexibility and, at the same time, alleviate muscle fatigue and soreness. Incorporating foam rolling as part of your warm-up can prevent issues like trigger point pain from causing more problems in the affected muscle group and causing more harm. Foam rolling has been known as a self-myofascial release (SMR) tool for many athletic people to relieve delay-onset muscle soreness (DOMS) and can help the recovery process for muscular performance. Studies show that when athletes have DOMS, their muscles are tender and stiff that which causes restricted movement. By foam rolling, each sore muscle group can get rolled out on a dense foam roll from the person’s body weight to apply pressure on the soft tissue. When performed correctly, the body’s range of motion will increase, and soft tissue restriction is prevented. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Back discomfort sensations and symptoms could indicate pulled-back muscles. Unless you’ve experienced the condition before, determining the cause can be difficult. A pulled-back muscle can start as a sudden, sharp sting when bending, reaching, or twisting. Or it can present gradually, worsening over a few days. It is a common injury, but if left untreated could take several weeks, and in severe cases, a few months, to heal correctly. Injury Medical Chiropractic and Functional Medicine Clinic can help diagnose the problem and develop a customized treatment plan to restore optimal function and health. Pulled Back Muscles A pulled muscle describes a strained muscle. - A strain is a muscle or tendon injury that happens when the tissue overstretches or tears.
- When a ligament stretches or tears, it’s called a sprain.
- Most cases can be managed and treated at home.
- But if the symptoms are not improving or make it difficult to move, see a doctor or chiropractor.
Symptoms Common signs and symptoms of a pulled-back muscle include: - Swelling
- Tenderness
- Soreness - Sore muscles that feel tight and achy usually indicate a condition that is likely to improve in a few days. More severe soreness could indicate a more significant injury.
- Spasms - A sudden convulsive spasm in the muscle can also indicate a pull. This can feel like a sudden tightening that does not release. The muscle can continue to spasm and lead to other symptoms.
- Cramping - A muscle can cramp can lead to increased tightness whenever trying to use the muscle.
- Pain - Can be characterized as a constant dullness and/or soreness in most situations or, in severe cases, sharp and shooting.
- Discomfort when moving around. If pain flares up when trying to move or use the back muscles is usually an indication that something is wrong.
- Relief during inactivity and rest. When lying down to rest or taking a temporary break, and the symptoms disappear could also be an indication of a pulled-back muscle or another injury.
Causes The most common causes are: A Strained Muscle - This causes some damage to a region of muscle tissue, usually the result of being over-used or torn from another injury.
Sprained Ligaments - Involves damage to the ligaments in a joint, usually those in the spinal vertebrae.
A Herniated Disc - This involves damage to the discs that can leak out, irritating the surrounding tissues and nerves and can cause shifting and misalignment of the spine.
These conditions are distinct, but the symptoms can be similar. Therapies It is important to consult a medical professional before treating an injury because symptoms of other injuries, such as disc problems or a broken bone, can resemble strains and sprains. Most treatments will utilize: Ice and Heat - Ice helps reduce inflammation.
- The faster ice can be applied to a pulled-back muscle, the quicker pain and swelling are reduced, and the healing process can begin.
- Apply a cold pack for 15-20 minutes as soon as the injury occurs.
- Take a 20-minute break between each cold application.
- After the first days, alternate cold therapy with heat to increase circulation.
- Try a 20-20-20 rule: 20 minutes of an ice pack followed by a 20-minute break, then 20 minutes of heat.
- Repeat as necessary, allowing 20 minutes between heat or ice therapy.
Limited Rest - Right after a muscle strain, limiting physical activity levels and avoiding movements are recommended for a short period.
- After the initial pain subsides, partial activity levels are recommended to help prevent the muscles from weakening.
Compression Stretching - Returning to activities, gentle stretching exercises can improve tissue healing by increasing blood circulation to the injured area.
- Applying heat to the area before stretching can also help.
Strength Training - Ask a doctor or chiropractor about the right strength exercises for your condition.
- Strength training will develop the muscles to prevent future injuries.
Pain Medication - Pain levels are an important indicator during the recovery process.
- Pain medications relieve symptoms but do not assist with healing and should only be used short-term to provide relief.
- If you need pain medication, consult your physician to determine the appropriate type and dosage for your situation.
Massage - Blood circulation to the injured tissues is increased with massage therapy.
Chiropractic - A chiropractor can diagnose back pain from a muscle or disc injury and develop an individualized treatment plan.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References https://www.aans.org/Patients/Neurosurgical-Conditions-and-Treatments/Low-Back-Strain-and-Sprain Allen, Laura. “Case Study: The Use of Massage Therapy to Relieve Chronic Low-Back Pain.” International journal of therapeutic massage & bodywork vol. 9,3 27-30. 9 Sep. 2016, doi:10.3822/ijtmb.v9i3.267 Kumar, Saravana et al. “The effectiveness of massage therapy for the treatment of nonspecific low back pain: a systematic review of systematic reviews.” International journal of general medicine vol. 6 733-41. 4 Sep. 2013, doi:10.2147/IJGM.S50243 https://www.merckmanuals.com/professional/injuries-poisoning/sprains-and-other-soft-tissue-injuries/overview-of-sprains-and-other-soft-tissue-injuries https://www.spine-health.com/conditions/lower-back-pain/exercises-lower-back-muscle-strain
Back pain is one of the most common reasons individuals go to a doctor, massage therapist, physiotherapist, osteopath, and chiropractor. Various health conditions, some spine-related, others not, list back pain as a symptom. Many of these conditions begin in the stomach or abdominal cavity, which leads to stomach and back pain. Stomach and back pain happening simultaneously, independently, or in combination could be caused by gut problems, back issues, or something completely different. Understanding what causes these two types of pain simultaneously can help figure out a treatment plan. Stomach Back Pain Causes Problems in the abdominal cavity and stomach issues can cause back pain and vice versa. Symptoms can also include referred pain when the pain is felt in one part of the body but is caused by pain or injury in another area. Stomach back pain causes depend on the type of condition/s that can include: Appendicitis - Inflammation in the appendix can cause sudden sharp pain in the abdomen.
- It presents mostly in the lower right area of the abdomen but can appear in or spread to other sites, especially the back.
Dysmenorrhea - The medical term for painful menstrual periods.
- Dysmenorrhea can cause pain in the abdomen and back at the same time.
- This type of pain can be:
- Primary - A condition experienced throughout life.
- Secondary - Starts later in life due to another condition.
Endometriosis - Endometriosis causes tissue to grow outside of the uterus.
- Similar to dysmenorrhea, symptoms include:
- Abdominal pain
- Referred low back pain
Fibromyalgia - This condition generates pain across the muscles and joints of the body.
- It shows up with irritable bowel syndrome -IBS.
- Fibromyalgia can simultaneously present a wide range of stomach problems and back pain.
Gallstones - Gallbladder stones or gallstones can cause blockages, inflammation, and painful swelling.
- A major symptom of gallstones is pain in the upper right of the abdomen, which can spread to the back.
Kidney Dysfunction - Kidney stones, infections, and chronic kidney disease can cause pain that's felt in the abdomen/flank and the mid and/or upper back.
Irritable bowel syndrome - IBS Inflammatory Bowel Disease - IBD - Inflammatory Bowel Disease is a family of immune-mediated, similar to autoimmune conditions with back pain as a symptom that includes:
- Crohn's disease
- Ulcerative colitis
Pancreatitis - An inflamed pancreas can cause symptoms like:
- Stomach issues.
- Pain across the abdomen and back.
Pancreatic Cancer - A common symptom of pancreatic cancer is a dull pain in the upper abdomen/belly and/or middle and/or upper back that is on and off.
- This can be because of a tumor that has formed on the tail of the pancreas or an area where it presses on the spine.
Stomach Bloating and Low Back Pain - Bloating is caused by pressure in the abdomen increasing to the point that it causes discomfort and pain.
- It can cause simultaneous stomach and back pain as the bloating adds pressure on the muscles, organs, and spine.
- One of the most common causes of bloating is trapped gas in the GI tract.
- This happens when the body cannot properly move the gas through the system.
- Bloating can also be caused by extra sensitivity to regular pressure increases.
- In these cases, the amount and movement of gas in the system are normal, but the body reacts as though something is wrong.
- Several GI tract disorders can cause similar bloating issues that include:
- Dyspepsia
- Gastritis
- Celiac diseaseDiverticular disease
- Food allergies
A chiropractic functional medicine team can work with an individual's primary physician or specialist to develop a personalized treatment plan to alleviate back pain symptoms, re-balance the body, strengthen the musculoskeletal system and restore function. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Clauw DJ. Chapter 258, Fibromyalgia, Chronic Fatigue Syndrome, and Myofascial Pain. Goldman-Cecil Medicine. Goldman L (ed.). 26th ed. Elsevier; 2020. 1774-1778. https://www.clinicalkey.com/#!/content/book/3-s2.0-B9780323532662002587 Ford AC, Talley NJ. Chapter 122, Irritable Bowel Syndrome. Feldman M (ed.). Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Elsevier: 2021. 2008-2020. https://www.clinicalkey.com/#!/content/book/3-s2.0-B9780323609623001223?scrollTo=%23hl0001104 Inadomi JM, Bhattacharya R, Hwang JH, Ko C. Chapter 7, The Patient with Gas and Bloating. Yamada’s Handbook of Gastroenterology. 4th ed. John Wiley & Sons; 2019. https://doi.org/10.1002/9781119515777.ch7 Kliegman RM, St Geme JW, Blum NJ, et al. Chapter 378, Pancreatitis. Nelson Textbook of Pediatrics. 21st ed. Elsevier; 2020. 2074-2080. https://www.clinicalkey.com/#!/content/book/3-s2.0-B9780323529501003783 Krames E, Mousad DG. Spinal Cord Stimulation Reverses Pain and Diarrheal Episodes of Irritable Bowel Syndrome: A Case Report. Neuromodulation. 2004 Mar 22;7(2):82-88. https://doi.org/10.1111/j.1094-7159.2004.04011.x Sifri CD, Madoff LC. Chapter 78, Appendicitis. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Bennett JA (ed.). Elsevier; 2020. 1059-1063. https://www.clinicalkey.com/#!/content/book/3-s2.0-B9780323482554000783 Stephen Norman Sullivan, "Functional Abdominal Bloating with Distention," International Scholarly Research Notices, vol. 2012, Article ID 721820, 5 pages, 2012. https://doi.org/10.5402/2012/721820 Wang DQH, Afdhal NH. Chapter 65, Gallstone Disease. Feldman M (ed.). Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Elsevier: 2021. 1016-1046. https://www.clinicalkey.com/#!/content/book/3-s2.0-B9780323609623000655?scrollTo=%23hl0001772 Weisman, Michael H et al. "Axial Pain and Arthritis in Diagnosed Inflammatory Bowel Disease: US National Health and Nutrition Examination Survey Data." Mayo Clinic proceedings. Innovations, quality & outcomes vol. 6,5 443-449. 16 Sep. 2022, doi:10.1016/j.mayocpiqo.2022.04.007 Whorwell PJ. Chapter 13, Abdominal Bloating. Irritable Bowel Syndrome: Diagnosis and Clinical Management. Emmanuel A, Quigley EMM (eds.). John Wiley & Sons; 2013. https://doi.org/10.1002/9781118444689.ch13 Yarze JC, Friedman LS. Chapter 12, Chronic Abdominal Pain. Feldman M (ed.). Sleisenger and Fordtran’s Gastrointestinal and Liver Disease. 11th ed. Elsevier; 2021. 158-167. https://www.clinicalkey.com/#!/content/book/3-s2.0-B9780323609623000126?scrollTo=%23hl0000408
Uneven hips can throw the back out of natural alignment and cause back stiffness, tightness, discomfort, and pain. Hips that are off-balance unhealthily affect standing, sitting, sleeping posture, walking gait, and overall movements. Biomechanics issues cause the core and spine stabilizing muscles to become weakened and fatigued from overcompensating to keep the body up and moving. Over time this can lead to chronic pain in the back, hips, knees, and feet. Chiropractic care can restore proper hip and spinal alignment and wellness. Uneven Hips Misaligned hips can be caused by work or sports injury, exercise, vehicle collision, and/or general wear and tear. When hips are out of alignment, they have shifted from their centered position. They could be rotated forward or backward, forcing the spine and the lower limbs to compensate, resulting in the spine tilting that can make the legs appear uneven. Discomfort may be one-sided low back pain near the sacroiliac joint, causing a stiff/tight back, limited motion, and/or pain symptoms. Because the spine and lower limbs have to compensate for the unevenness, the shoulders and upper back, connected to the pelvis through the spine, are also affected and result in: - Back pain.
- Hip and gluteal muscle pain.
- Uneven leg length.
- Knee, ankle, and foot issues and pain.
- Uneven shoulders.
- The shoulder blades can stick out on the side of the lower hip.
- Rib discomfort and pain.
- The rib cage could protrude out on one side. However, this could be due to advanced scoliosis.
Therapy Staying active is recommended and includes stretching and core strengthening. General stretches recommended to optimize hip equity include: Hamstring stretch - For this stretch, lie on a flat surface with your legs extended straight out.
- Bend the right leg at the knee, placing the right foot on the ground.
- Use a towel, belt, or band to grab and wrap around the left foot.
- Keep the hip/buttock on the left side planted on the floor.
- Slowly raise the left leg upward as far as possible until you feel the stretch.
- Once you feel a stretch or restriction in the hamstring, hold the position for 30 seconds.
- Repeat on the other side.
- Perform 2 to3 times.
Hip flexor stretch - Kneel on the affected leg and bend the healthy leg out in front with the foot flat on the floor.
- Back straight.
- Slowly push the hips forward until you feel the stretch in the upper thigh and hip.
- Hold the stretch for around 15 to 30 seconds.
Chiropractic Care Chiropractic treatment is a highly recommended non-surgical option for uneven hips and pelvic tilt. Depending on the severity of the misalignment, underlying issues, and body scanning images, hip alignment treatment could include: - Soft tissue therapeutic massage
- Chiropractic muscle release for tight hip flexors, quadriceps, hamstrings, and glutes.
- Decompression
- Traction
- Custom orthotics
- Bracing
- Posture training
- Activity modification
- Health Coaching
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make your own healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Kiapour, Ali et al. “Biomechanics of the Sacroiliac Joint: Anatomy, Function, Biomechanics, Sexual Dimorphism, and Causes of Pain.” International journal of spine surgery vol. 14, Suppl 1 3-13. 10 Feb. 2020, doi:10.14444/6077 Lee, Jeong-Hoon, et al. “The effect of Graston technique on the pain and range of motion in patients with chronic low back pain.” Journal of physical therapy science vol. 28,6 (2016): 1852-5. doi:10.1589/jpts.28.1852 Patel, Rikin V et al. “Pelvic Tilt and Range of Motion in Hips With Femoroacetabular Impingement Syndrome.” The Journal of the American Academy of Orthopaedic Surgeons vol. 28,10 (2020): e427-e432. doi:10.5435/JAAOS-D-19-00155 Rivière, C et al. “Spine-hip relations add understandings to the pathophysiology of femoro-acetabular impingement: A systematic review.” Orthopaedics & traumatology, surgery & research : OTSR vol. 103,4 (2017): 549-557. doi:10.1016/j.otsr.2017.03.010 Suits, William H. “Clinical Measures of Pelvic Tilt in Physical Therapy.” International journal of sports physical therapy vol. 16,5 1366-1375. 1 Oct. 2021, doi:10.26603/001c.27978
|


 Your new post is loading...
Your new post is loading...



























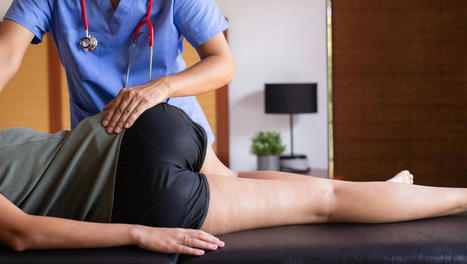





Injury Medical Chiropractic Clinic: Learning about gender and gender transitioning and how to be supportive is a great way to be an ally. For answers to any questions you may have, please call Dr. Jimenez at 915-850-0900 or 915-412-6677