 Your new post is loading...
 Your new post is loading...
ADHD strengths are a source of possibility. In the right conditions, ADHD is an advantage for individuals, organizations and society.
Protecting patients while safeguarding pharmaceuticals, managing visitor access while ensuring staff safety, and maintaining compliance while operating efficiently — all these challenges demand a level of coordination that traditional security approaches simply cannot provide.
Leah Helmbrecht spent years advocating for survivors of sexual assault and domestic violence. Now, she’s sharing why she had to leave forensic nursing to protect her own mental health.
‘Nursing is about courage in the face of the unknown’
The Train More Nurses Act would help address these challenges by directing the U.S. Department of Health and Human Services (HHS), as well as the U.S. Labor Department, to conduct a review of nursing grant programs to identify opportunities to increase faculty at nursing schools nationwide, especially in underserved communities.
Many believe heart health requires hours of exercise, but research shows that just 10 minutes of movement each morning can offer surprising cardiovascular benefits.
Nurses are the backbone of the care team and key to systemic change—especially when equipped with evidence-based information.
Serotonin is a well-established modulator of various neuropsychological processes, as well as organ and endocrine functioning, and metabolism and home…
The study, published in Home Healthcare Now, also found 37% of respondents experience either verbal or emotional abuse on a daily basis.
We asked nutrition experts for their best tips on how to eat well.
Medicaid enrollees with substance use disorders have higher health costs than those without, around $1,200 compared to $550 monthly on average, KFF reported.
As the U.S. healthcare system continues to grapple with a historic nursing shortage, the proposed FY 2026 federal budget threatens to accelerate the crisis through sweeping cuts to nursing education, research, and Medicaid support—posing profound implications for workforce sustainability, patient access, and innovation. Burnout, workplace violence, and long-standing systemic challenges have already driven thousands of
HOMOEOPATHY, a natural system of medicine which is grounded in the belief that the body has an innate ability to heal itself, may be fairly new to T&T, but it
|
Discover how the UF College of Nursing dean uses her dual role to rethink nurses in leadership and empower nursing education.
Stay strong, mobile, and pain-free with 4 essential exercises everyone over 40 should do to stay fit for life
A WashU Medicine study paves the way to make an effective treatment more accessible to those 'paralyzed by life.'
According to the U.S. Bureau of Labor Statistics, an average of 194,500 job openings for registered nurses is projected each year through 2033, reflecting sustained demand for skilled nursing professionals. However, despite this growth, workforce analyses suggest a looming shortage in several states. Data from the Bureau of Health Workforce indicates the U.S. could face
A study of more than 2,100 people ages 60 to 79 found that an intensive two-year program of mental and physical activities, along with a heart-healthy diet, improved memory and thinking.
Student editor Deborah Amu asks whether the challenges newly qualified health professionals are facing will continue.
Dr. Angela Mazza examines the impacts of cortisol levels on longevity. Here's how she manages her own stress and stays in good health.
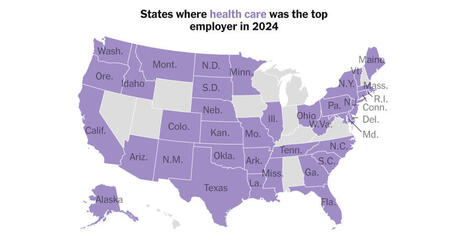
Medicine is now the nation’s largest employer, but its growth may be slowing.
In a world where health trends come and go faster than your morning smoothie blends, it’s easy to overlook the quiet powerhouses that have been working their magic for centuries. While you’ve likely heard of mainstream wellness staples like turmeric, ginger, or echinacea, there’s an entire realm of lesser-known herbs quietly transforming lives across the globe. These botanical underdogs aren’t just old wives’ tales or exotic health fads—they’re rooted in ancient traditions and backed by a growing body of modern science. From fighting fatigue to enhancing brain function, balancing hormones, calming nerves, and strengthening immunity, these hidden herbs offer powerful, natural support for the body and mind. What makes these 12 herbs so special? They’ve flown under the radar, often overshadowed by flashier ingredients, yet they hold remarkable potential for anyone looking to level up their wellness routine—without relying on synthetic supplements. Whether they come from the mountains of Asia, the fields of Africa, or the gardens of Europe, these herbs have been cherished for generations in holistic medicine systems like Ayurveda, Traditional Chinese Medicine, and folk remedies passed down through the ages. In this guide, we’re unveiling 12 of the most underrated healing herbs that deserve a front-row seat in your health arsenal. You don’t need to be an herbalist to benefit from them—many are available as teas, powders, tinctures, or capsules, ready to easily integrate into your daily life. So if you’re tired of generic advice and ready to discover truly unique plant-based remedies, you’re in the right place. Let’s dig into nature’s lesser-known medicine cabinet—you might just find the missing piece your wellness routine has been craving.
Alabama has 44 certified SANEs for the entire state. Louisiana has 42. Mississippi only has 6 — for a population of almost three million.
The following is a guest article by Joy Avery, MSN, RN - Senior Vice President, Clinical Strategy at CipherHealth Healthcare’s AI gold rush is at a crossroads. At board meetings across the country, AI has become a strategic mandate—a signpost of innovation and forward thinking. At the same time, it is also in danger of
According to a new report commissioned by the American Hospital Association, hospitals spent $18.3 billion to manage violence against both patients and staff members in 2023, in today's bite-sized hospital and health industry news from the District of Columbia, Illinois, and New York.
|




 Your new post is loading...
Your new post is loading...



























ADHD Strengths: How Brains Wired Differently Spark Innovation
ADHD minds
Please also review AIHCP's ADHD Consulting Program