 Your new post is loading...
 Your new post is loading...
Sciatica is not a “muscle” problem by itself. It is a nerve irritation pattern—often characterized by burning, aching, tingling, or sharp pain — that can radiate from the lower back into the buttocks, thigh, calf, and sometimes the foot. In many people, the sciatic nerve is irritated because nearby tissues are tight or inflamed, or because the piriformis and other deep hip muscles compress the nerve pathway. (Healthline, 2021; Dr. Alex Jimenez, n.d.). Self-massage can help by relaxing the “pressure zones” around the nerve—especially the glutes, piriformis, hamstrings, and low back tissues—so the irritated system calms down. When performed correctly, it can reduce pain and improve motion without “digging into” the nerve itself. (Harley Street Specialist Hospital, 2023; Chicago Pain Control, n.d.). The key rule: massage the muscles around the nerve, not the nerve A common mistake is pushing hard directly on the spot that hurts the most. With sciatica, that can backfire. Instead: -
Work the glute muscles and piriformis (deep buttock muscle) to reduce local compression and trigger points. (Healthline, 2021). -
Use myofascial release concepts—slow pressure and slow rolling—so tissues “let go” over time rather than resisting. (Harley Street Specialist Hospital, 2023). -
If symptoms get sharp, electric, or quickly worse, stop immediately. (Spine-health, n.d.). Pain scale guidance: “hurts good” only Keep discomfort in a safe range: This aligns with recommendations from many clinical massage educators for nerve-related pain: controlled pressure rather than aggressive force. (Chicago Pain Control, n.d.; Spine-health, n.d.). Tools that work well at home You do not need expensive equipment. The most helpful tools are simple: -
Tennis ball (or lacrosse ball if you want slightly firmer pressure later) -
Foam roller -
Two tennis balls taped together (or placed in a sock) for a safer “double-ball” low back technique -
Heat pack (before or after) The double-ball method is popular because it can engage muscles adjacent to the spine while avoiding direct pressure on the spine itself. (Massage Chair Store, n.d.; Spine-health, n.d.). Step-by-step self-massage routine for sciatica relief Heat first (optional but helpful) Use a heating pad on the glutes or lower back for 10–15 minutes to help tissues relax before you start. Heat is commonly recommended as a first-line intervention in sciatica care plans. (ChiroBoston, n.d.). Glute + piriformis trigger point release (tennis ball) Goal: Calm tight glute/piriformis trigger points that may irritate the sciatic pathway. How: -
Sit on the floor and place the ball under one buttock. -
Lean slightly toward the tight side. -
Find a tender spot and hold pressure for 20–45 seconds. -
Breathe slowly until it softens, then move 1–2 inches and repeat. Tips: -
Keep the pressure at 3/10 or less. -
If you experience numbness, burning, or shocking pain, stop and reposition. (Healthline, 2021). Healthline notes that piriformis self-massage can reduce pressure on the sciatic nerve and should be performed gently, with treatment discontinued if symptoms worsen. (Healthline, 2021). Low back muscle release (two tennis balls) Goal: Release tight low back muscles without rolling on the spine. How: -
Tape two tennis balls together or put them in a sock. -
Lie on your back with knees bent. -
Place the balls on either side of the spine (not on the spine). -
Slowly shift your body weight and pause on tight areas. Safety reminders: -
Avoid rolling directly on the spine. -
Stop immediately if pain becomes sharp or sudden. (Spine-health, n.d.; Massage Chair Store, n.d.). Myofascial release down the back of the leg (foam roller) Goal: Reduce “referred tension” through the glutes/hamstrings that can keep sciatica symptoms active. How: -
Place a foam roller under your hamstrings. -
Roll slowly from mid-thigh toward the glute area. -
Pause on tender spots for 20–30 seconds. This slow, warming style aligns with common myofascial release approaches used for sciatica-related muscle guarding. (Harley Street Specialist Hospital, 2023). Calf massage for referred pain Some people with sciatica experience significant calf tightness or deep pain. Gentle calf work can help reduce guarding and improve comfort. How: -
Use your hands or a massage tool. -
Work from the ankle toward the knee with slow strokes. -
Add small pauses on tender areas, but do not crush the tissue. Targeted lower-leg massage is commonly included in lists of sciatica massage techniques to reduce referred pain patterns. (Active Posture, 2025). What to avoid To keep self-massage helpful (not irritating), avoid these mistakes: -
Heavy pressure directly where nerve pain shoots -
Fast rolling over painful areas -
Forcing numbness or tingling to “break through” -
Long sessions that leave you sore for 24–48 hours A safe guideline: you should feel looser after the session, not flared up. If symptoms worsen, reduce pressure, shorten the session, or stop. (Spine-health, n.d.). Why integrative chiropractic care can improve long-term results Self-massage can alleviate symptoms, but it may not fully address the mechanical driver—such as joint restriction, disc irritation, or nerve root compression. That is where integrative chiropractic care often fits. Common in-clinic approaches include: -
Targeted spinal adjustments to restore joint motion and reduce irritation patterns. (Fremont Spine + Wellness, 2025). -
Myofascial release/soft tissue therapy for glutes, low back, and hip stabilizers. (Bend Total Body Chiropractic, 2025). -
Spinal decompression therapy (when appropriate) to reduce pressure on irritated nerve roots and support disc space mechanics. (Dr. Alex Jimenez, n.d.). Clinical observations from Dr. Alexander Jimenez, DC, APRN, FNP-BC Dr. Jimenez commonly highlights a practical pattern observed in clinical practice: sciatica symptoms can arise from both local muscular entrapment (e.g., piriformis syndrome) and deeper spinal drivers (e.g., disc or joint irritation). In these cases, combining soft-tissue work with an appropriate plan—often including decompression strategies and targeted care—may help reduce nerve irritation, improve function, and reduce the risk of recurrence. (Dr. Alex Jimenez, n.d.). When to stop self-massage and get checked right away Seek urgent medical evaluation if you have: -
New or worsening leg weakness -
Loss of bowel or bladder control -
Numbness in the saddle area (groin/inner thighs) -
Fever, unexplained weight loss, or severe unrelenting pain These may indicate a more serious condition requiring immediate care. Sciatica Pain Treatment in El Paso, TX: Chiropractic Care References -
A Guide to Massage for Sciatica (Massage Chair Store, n.d.). -
How to Massage Sciatica to Reduce Leg Pain Fast (Chicago Pain Control, n.d.). -
10 Massage Techniques For Sciatica Pain Relief (Harley Street Specialist Hospital, 2023). -
Self-Massage and Stretches for Piriformis Syndrome (Healthline, 2021). -
How to Use Tennis Balls for DIY Lower Back Pain Massage (Spine-health, n.d.). -
How Massage Can Ease Sciatic Pain (ChiroBoston, n.d.). -
Relief From Sciatica Pain (Fremont Spine + Wellness, 2025). -
Massage Therapy Complements Chiropractic Care for Sciatica Relief (Bend Total Body Chiropractic, 2025). -
Unlock Sciatic Relief with Targeted Massage Techniques (Active Posture, 2025). -
Piriformis Syndrome & Spinal Decompression Therapy (Jimenez, A., n.d.). -
Sciatica Pain and Symptoms Improvement (Jimenez, A., n.d.). The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and identify relevant research studies for our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We are here to help you and your family. Blessings Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN email: coach@elpasofunctionalmedicine.com
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182 Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-State Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
New York APRN License #: N25929, Verified: APRN-N25929*
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States* Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master’s in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Sciatica is a painful condition that affects the sciatic nerve, the largest nerve in the body. It often causes pain that travels from the lower back down the leg, along with numbness, tingling, or weakness. For years, treatment focused on pain medications, steroid injections, or surgery when symptoms became severe. In 2026, sciatica care has changed in important ways. New treatments now focus on targeted nerve relief, tissue healing, and personalized care plans instead of simply masking pain. Many of these advances aim to reduce the need for surgery, shorten recovery time, and lower the need for long-term medication use (BioSpace, 2025). This shift reflects a deeper understanding of how nerve pain works and how the spine, muscles, and nervous system interact. Why Sciatica Treatment Needed to Evolve Traditional sciatica care often relied on: -
Long-term pain medications -
Repeated steroid injections -
Surgical procedures like discectomy or spinal fusion While these treatments help some people, they can also lead to: -
Medication side effects -
Risk of dependency on opioids -
Long recovery times after surgery -
Ongoing nerve irritation rather than true healing Research now shows that addressing inflammation, nerve compression, movement dysfunction, and biomechanical stress together leads to better outcomes (Stanford Health Care, 2025). Advanced Diagnostic Tools in 2026 One of the biggest improvements in sciatica care is better diagnosis. In 2026, clinicians rely on more detailed imaging and functional assessments to find the exact cause of nerve pain. Key Diagnostic Advances -
High-resolution MRI scans that better show disc bulges, nerve root compression, and soft tissue inflammation -
Functional imaging to evaluate how the spine moves under load -
Improved nerve testing to distinguish sciatic pain from hip or muscle-related conditions According to clinical observations from Dr. Alexander Jimenez, many patients previously labeled with “chronic sciatica” actually have combined disc, joint, and muscle dysfunction that requires integrated care rather than surgery alone (Jimenez, 2026). Targeted Nerve Blocks and Advanced Injections By 2026, nerve blocks have become more precise and effective. How Modern Nerve Blocks Work -
Use imaging guidance to target the exact pain source -
Reduce inflammation around the nerve -
Calm overactive pain signals Unlike older steroid injections, newer nerve blocks: -
Use lower medication doses -
Focus on short-term pain interruption -
Support rehabilitation rather than replacing it These techniques are often used as a bridge to active care, such as chiropractic treatment and exercise (Apollo Spine & Pain, 2026). Spinal Cord Stimulation: Smarter and Less Invasive Spinal cord stimulation (SCS) has also improved significantly. 2026 Improvements in SCS -
Smaller implanted devices -
Better targeting of nerve pathways -
Adjustable stimulation based on daily activity These systems work by modifying pain signals before they reach the brain, helping patients with chronic nerve pain who have not responded to conservative care (Pain & Spine Specialists, 2026). Importantly, newer SCS systems are often considered before surgery, not after. Radiofrequency Ablation for Sciatic Pain Radiofrequency ablation (RFA) is gaining attention in 2026 as a minimally invasive option for persistent sciatica. Benefits of RFA RFA does not damage the entire nerve. Instead, it targets specific pain fibers, allowing normal movement while decreasing pain signals (Apollo Spine & Pain, 2026). Regenerative Therapies: Healing Instead of Masking Pain One of the most exciting advancements in sciatica treatment is the rise of regenerative medicine. Platelet-Rich Plasma (PRP) PRP uses the patient’s own blood components to: -
Reduce inflammation -
Support tissue repair -
Promote nerve healing Studies show PRP may help with disc-related sciatica by improving the health of surrounding tissues (PMC, 2025). Why Regenerative Care Matters -
Focuses on long-term healing -
Reduces reliance on repeated injections -
Supports the body’s natural repair process Market research shows regenerative sciatica treatments are expanding rapidly due to patient demand for non-surgical options (Grand View Research, 2025). Personalized Exercise Programs and Nerve Flossing Exercise is no longer “one size fits all.” In 2026, programs are custom-built based on imaging, nerve sensitivity, and movement patterns. Nerve Flossing Nerve flossing involves gentle movements that: -
Improve nerve mobility -
Reduce adhesions -
Decrease nerve tension This approach is especially helpful when guided by clinicians trained in neuromusculoskeletal care (Goodman Campbell, 2026). Other Exercise Advances When combined with chiropractic care, these programs often lead to faster recovery and fewer flare-ups. Shockwave, Laser, and Neuromodulation Therapies Several non-surgical technologies are now commonly used in the treatment of sciatica. Common Technologies in 2026 -
Shockwave therapy to stimulate healing -
Low-level laser therapy for nerve repair -
Neuromodulation devices to calm pain pathways These therapies are often used alongside manual care and rehabilitation rather than alone (Easy Reach Chiropractic, 2025). The Shift Toward Integrated, Multidisciplinary Care One of the most important changes in sciatica treatment is how care teams work together. Integrated Care Model -
Chiropractors address spinal alignment and nerve compression -
Nurse practitioners manage diagnostics, medications, and inflammation -
Exercise specialists restore movement and strength This approach treats both symptoms and underlying causes, rather than focusing only on pain relief. Clinical experience shared by Dr. Jimenez highlights that patients in integrated care models often: Chiropractic Care’s Role in 2026 Sciatica Treatment Chiropractic care remains a key non-invasive option. Chiropractic Advances Include Research continues to show chiropractic care is associated with lower opioid use in sciatica patients (UH Hospitals, 2025; ReachMD, 2025). Nurse Practitioners as Key Coordinators of Care Nurse practitioners (NPs) are playing a growing role in the treatment of sciatica. NP Contributions -
Ordering advanced imaging -
Monitoring neurological symptoms -
Managing inflammation safely -
Coordinating multidisciplinary care Studies confirm that NP-led collaborative models improve outcomes while keeping care cost-effective (JAANP, 2022; ScienceDirect, 2012). Reducing Opioid Dependence Through Modern Care A major goal of 2026 sciatica treatment is reducing opioid exposure. How New Approaches Help Integrated chiropractic and NP care has been linked to lower opioid use and fewer long-term complications (UH Hospitals, 2025). Faster Recovery and Long-Term Relief Modern sciatica treatment focuses on: Patients are no longer told to “just live with it.” Instead, care plans are designed to restore movement, reduce nerve irritation, and support overall spinal health. Looking Ahead: The Future of Sciatica Care In 2026, sciatica treatment has clearly shifted: -
From surgery to precision care -
From symptom management to nerve healing -
From isolated treatment to team-based care According to Dr. Jimenez’s clinical insights, the future lies in early diagnosis, personalized treatment, and integrated care models that respect the complexity of nerve pain rather than oversimplifying it (Jimenez, 2026). Conclusion Advancements in sciatica treatment in 2026 reflect a smarter, safer, and more patient-centered approach. With better diagnostics, minimally invasive procedures, regenerative therapies, and collaborative care models, people with sciatica now have more effective options than ever before. By addressing the true causes of nerve pain, these innovations offer hope for long-term relief without unnecessary surgery or prolonged medication use. Sciatica Explained | El Paso, Tx References BioSpace. (2025). Sciatica market outlook 2025–2035. https://www.biospace.com/press-releases/sciatica-market-size-to-reach-usd-3-4-billion-by-2035-impelled-by-advancements-in-regenerative-therapies PMC. (2025). Emerging regenerative therapies for nerve pain. https://pmc.ncbi.nlm.nih.gov/articles/PMC12138371/ Apollo Spine & Pain. (2026). Pain management breakthroughs to watch. https://www.apollospineandpain.com/pain-management-breakthroughs-watch-2026 Goodman Campbell. (2026). Most successful treatments for sciatica. https://www.goodmancampbell.com/2026/01/what-is-the-most-successful-treatment-for-sciatica/ Stanford Health Care. (2025). Advanced sciatica treatment options. https://stanfordhealthcare.org/medical-conditions/back-neck-and-spine/sciatica.html Grand View Research. (2025). Sciatica treatment market report. https://www.grandviewresearch.com/industry-analysis/sciatica-treatment-market-report UH Hospitals. (2025). Chiropractic care associated with reduced opioid use. https://news.uhhospitals.org/news-releases/articles/2025/10/new-study-shows-chiropractic-care-associated-with-reduction-in-opioid-use-disorder JAANP. (2022). Nurse practitioners in coordinated care models. https://journals.lww.com/jaanp/fulltext/2022/02000/introducing_the_american_society_for_bone_and.4.aspx Jimenez, A. (2026). Clinical insights on sciatica care. https://dralexjimenez.com/
Jimenez, A. (2026). Professional insights. https://www.linkedin.com/in/dralexjimenez/ The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and to identify relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Key Takeaways -
A head injury can set off a chain reaction—from neck muscle guarding to spinal misalignment—that irritates the sciatic nerve and causes leg pain. It can also occur alongside a spine injury after trauma. (Paiva et al., 2011; Hlwatika et al., 2022). PMC+1 -
Traumatic brain injury (TBI) ramps up inflammation and pain signaling pathways in the spinal cord, increasing the chance of ongoing low-back and sciatic pain even when imaging looks “normal.” (Liang et al., 2017; Sahbaie et al., 2019; Widerström-Noga et al., 2016). PMC+2Nature+2 -
TBI can also lead to heterotopic ossification (new bone growth) around soft tissues. Rarely, this new bone can compress the sciatic nerve, causing sciatica. (Issack et al., 2008; Panagiotopoulos et al., 2008; Cleveland Clinic, n.d.). PMC+2PMC+2 -
Integrative chiropractic care aims to realign the spine, calm the nervous system, and support recovery routines (sleep, nutrition, pacing). Some clinics suggest that improved spinal motion may help restore cerebrospinal fluid (CSF) circulation; this idea is emerging and requires further research. (Clinic sources listed; evidence caveats noted). PMC What Is Sciatica? Sciatica is a type of nerve pain that travels from the lower back through the buttocks and down the leg. It happens when the sciatic nerve or its roots in the lumbosacral spine are irritated or compressed. Symptoms include sharp or burning leg pain, tingling, numbness, or weakness (Davis, 2024). NCBI How Can a Head Injury Lead to Sciatica? 1) Brain–to–Spine Control Problems After TBI Your brain sets the tone for spinal muscles through descending motor pathways. After a head injury, those upper-motor-neuron controls can be disrupted, leading to abnormal muscle tone, spasms, and poor coordination of the deep stabilizers that protect your neck and back. That imbalance makes it easier for vertebrae to shift into stress patterns that irritate nerve roots feeding the sciatic nerve (Kandel et al., 2013). NCBI What that feels like: tight hip flexors, a tilted pelvis, and a painful pull on the lumbar segments—especially with sitting, coughing, or bending. 2) The “Neck-First” Chain Reaction Head and neck trauma often produces upper-cervical muscle guarding and joint dysfunction. The body compensates down the chain, resulting in thoracic stiffness, limited rib motion, and a pelvis that rotates or tilts on one side. Over time, this chain reaction increases pressure on the lower lumbar nerve roots, leading to sciatica symptoms. Clinical concussion resources describe how neck inflammation and proprioceptive changes can alter movement patterns and pain perception well beyond the head (Physio Pretoria; Broadview Health Centre). PMC 3) Co-Occurring Spine Injuries After Head Trauma Trauma that is strong enough to cause TBI can also injure the spine. Studies show a meaningful rate of concomitant cervical or overall spinal injuries in TBI patients; certain intracranial injury patterns (e.g., diffuse axonal injury) raise that risk (Paiva et al., 2011; Hlwatika et al., 2022; Pandrich et al., 2018). If your neck or lower back was also injured, you may develop sciatica from a disk herniation, facet injury, or foraminal narrowing after the crash or fall. PMC+2PubMed+2 4) Inflammation and Pain Signaling After TBI Even without obvious lumbar damage, TBI can sensitize pain pathways in the spinal cord. Experimental and translational studies have demonstrated that TBI can upregulate chemokine signaling (e.g., CXCR2), activate glial cells, and increase spinal inflammatory mediators, thereby amplifying pain signals from the back and legs (Liang et al., 2017; Sahbaie et al., 2019). Large clinical cohorts also link TBI with high rates of persistent pain (Widerström-Noga et al., 2016; NIDILRR/VA TBI Model Systems, 2025). This sensitization can make a minor lumbar strain feel like severe sciatica. PMC+3PMC+3Nature+3 5) Heterotopic Ossification (HO) After TBI TBI increases the chance of heterotopic ossification—abnormal bone formation in soft tissue. When HO occurs near the hip or pelvis, it can encase or compress the sciatic nerve, creating progressive sciatica months after the original injury (Issack et al., 2008; Panagiotopoulos et al., 2008; Cleveland Clinic, n.d.). Clues include a gradually stiff hip, a hard mass, or worsening nerve pain despite typical care. PMC+2PMC+2 Signs Your Sciatica May Be Linked to a Head or Neck Injury -
Sciatica began weeks to months after a concussion or head/neck trauma -
Neck stiffness, headaches, dizziness, or visual strain came first, then low-back and leg pain -
Pain flares with long sitting, screen time, or head movement -
Leg symptoms shift sides depending on posture or neck position -
Slow, progressive leg pain after hip/pelvic trauma (possible HO) Community and clinic resources also note back or leg pain flares after concussion—often tied to posture and neck mechanics (Ok Precision Chiro; Allied Performance Wellness). These are clinical perspectives rather than randomized trials, but they align with the neck-first chain-reaction idea. PubMed+1 Getting the Right Evaluation A thorough exam should screen both the head/neck and the lumbar–pelvic region: -
Neurological screen: reflexes, dermatomes, myotomes, straight-leg-raise, slump test, and upper-motor-neuron signs. -
Cervical assessment: joint motion, muscle tone, proprioception, vestibular-ocular reflexes. -
Lumbar–pelvic mechanics: sacroiliac symmetry, hip mobility, core stability, and gait. -
Imaging when indicated: red flags (severe weakness, bowel/bladder changes, progressive deficits), suspected HO, or suspected fracture/dislocation (Issack et al., 2008). PMC When to rule out HO: history of TBI with hip/pelvic trauma plus hard end-feel, palpable mass, and steadily worsening nerve pain—ask about X-ray or CT to look for extra bone (Cleveland Clinic, n.d.). Cleveland Clinic How Integrative Chiropractic Care Can Help Integrative chiropractic means blending evidence-informed spinal adjustments with soft-tissue therapy, vestibular/cervical rehab, graded activity, sleep/nutrition coaching, and care coordination with medical providers when needed. 1) Reduce Mechanical Pressure and Restore Alignment -
Gentle spinal and pelvic adjustments to improve motion and reduce joint irritation around lumbar nerve roots. -
Upper-cervical work to normalize neck mechanics that set the tone for the entire spine and pelvis. -
Hip mobility and rib-cage mechanics to unload the sciatic pathway during walking and sitting. Educational resources emphasize that sciatica relief occurs when underlying mechanical causes are addressed, not just the symptoms (Arrowhead Clinic). This reflects standard musculoskeletal reasoning, though randomized trials specific to post-TBI sciatica are limited. PMC 2) Calm the Sensitized Nervous System Post-TBI, the spinal cord may be “turned up.” Clinicians combine adjustments with graded sensory input, diaphragmatic breathing, and pacing strategies to reduce central sensitization. Experimental work supports the concept that TBI increases spinal inflammatory signaling (CXCR2) and that modulating nociceptive traffic could reduce pain (Liang et al., 2017; Sahbaie et al., 2019). PMC+1 3) Vestibular and Cervical Rehabilitation When concussion symptoms persist, incorporating vestibular, oculomotor, and proprioceptive drills can enhance balance and neck control, ultimately improving lumbar mechanics during daily tasks. Clinical resources highlight this link (Physio Pretoria; Broadview Health Centre; Allied Performance). PMC 4) Functional Strength and Mobility A plan that combines glute/hip strength, core endurance, and hamstring flexibility with walking intervals can help alleviate nerve root stress and build resilience. Start low, progress slowly, and avoid pain spikes greater than 2/10 during and after sessions. 5) Sleep, Nutrition, and Inflammation TBI recovery benefits from regular sleep, anti-inflammatory foods (such as omega-3s and colorful produce), and adequate hydration. These choices can reduce systemic inflammation that worsens nerve pain. (General TBI pain evidence: Widerström-Noga et al., 2016; NIDILRR/VA 2025). PMC+1 6) CSF Circulation: An Emerging Idea Some chiropractic clinics propose that restoring motion in the upper neck may improve cerebrospinal fluid (CSF) circulation following head/neck injury. This is a theoretical and evolving area with limited high-quality trials; if you explore this option, do so within an integrative plan that tracks objective outcomes (clinic sources provided by the user discuss this concept). PMC Step-by-Step Recovery Plan (Sample) -
Week 1–2: Settle the system -
Short walks daily, diaphragmatic breathing 5×/day -
Gentle cervical and lumbar mobility, no sustained flexed sitting -
Chiropractic assessment: begin light adjustments as indicated -
Sleep routine: same bed/wake times; limit screens before bed -
Week 3–4: Re-build motion and control -
Add vestibular/ocular drills if dizzy; cervical proprioception work -
Hip openers, glute bridges, side planks, bird-dogs (pain-guided dosing) -
Nerve mobility (sciatic sliders) if not irritable -
Week 5–8: Strength and endurance -
Progress to split squats, dead-bug variations, step-downs -
Interval walking → brisk walking; monitor symptoms 24-hour response -
Return-to-work or sport plan with pacing rules -
Re-check milestones -
Sitting tolerance 30→60 min, walking 10→30 min, sleep quality, leg strength symmetry -
If regression or red flags occur, re-image or co-manage with neurology/PM&R When Surgery or Injections Are Considered -
HO compressing the sciatic nerve that fails conservative care (Panagiotopoulos et al., 2008; Issack et al., 2008). -
Large disk herniation with progressive weakness, or cauda equina red flags (StatPearls sciatica review). -
Persistent radicular pain despite comprehensive non-operative care. PMC+2PMC+2 Clinical Perspective from Dr. Alexander Jimenez, DC, APRN, FNP-BC In clinical practice, Dr. Jimenez emphasizes a whole-person approach for patients who develop sciatica after concussion or head/neck trauma. Care plans typically incorporate cervical and lumbopelvic adjustments, soft-tissue treatment, vestibular/ocular rehabilitation, and graded strength exercises, along with coaching on sleep and anti-inflammatory nutrition—often in coordination with imaging and medical partners when necessary (Jimenez, clinical web/LinkedIn profiles). These observations reflect practice patterns rather than randomized trials and should be integrated with your medical team’s recommendations. PMC Practical Tips You Can Start Today -
Neutral posture rule: If sitting for more than 20–30 minutes increases symptoms, stand and walk for 2–3 minutes. -
Head first: Treat the neck and visual/vestibular issues early to reduce downstream lumbar strain. -
Gentle nerve sliders: Only when the leg isn’t highly irritable; stop if tingling grows. -
Anti-inflammatory basics: Fish, greens, berries, olive oil; hydrate; regular sleep. -
Track trends: A simple pain/sleep/activity log helps your team tailor care. Red Flags—Get Immediate Care -
New or worsening leg weakness, foot drop, or loss of knee/ankle reflexes -
Bowel/bladder changes or saddle numbness -
Fever, unexplained weight loss, cancer history -
Hard mass and progressive hip stiffness after trauma (possible HO) (Cleveland Clinic, n.d.). Cleveland Clinic References Davis, D. (2024). Sciatica. StatPearls. National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK507908/ NCBI Fidancı, H., et al. (2021). The relationship between nerve conduction studies and neuropathic pain scale in sciatic neuropathy. Journal of Clinical Medicine Research. https://pmc.ncbi.nlm.nih.gov/articles/PMC7783856/ PMC Hlwatika, P., et al. (2022). Concurrent cranial and cervical spine injuries. SA Journal of Radiology. https://pmc.ncbi.nlm.nih.gov/articles/PMC8991192/ PMC Issack, P. S., et al. (2008). Sciatic nerve injury associated with acetabular fractures. HSS Journal. https://pmc.ncbi.nlm.nih.gov/articles/PMC2642541/ PMC Kandel, E. R., et al. (2013). The upper motor neuron syndrome. In Neuroscience (NCBI Bookshelf). https://www.ncbi.nlm.nih.gov/books/NBK10898/ NCBI Liang, D.-Y., et al. (2017). The chemokine receptor CXCR2 supports nociceptive sensitization after TBI. Journal of Neurotrauma. https://pmc.ncbi.nlm.nih.gov/articles/PMC5593214/ PMC Paiva, W. S., et al. (2011). Spinal cord injury and its association with blunt head trauma. Spinal Cord. https://pmc.ncbi.nlm.nih.gov/articles/PMC3177586/ PMC Panagiotopoulos, E. C., et al. (2008). Sciatica due to extrapelvic heterotopic ossification: A case report. International Journal of General Medicine. https://pmc.ncbi.nlm.nih.gov/articles/PMC2556682/ PMC Pandrich, M. J., et al. (2018). Prevalence of concomitant traumatic cranio-spinal injury. Journal of Clinical Neuroscience. https://pmc.ncbi.nlm.nih.gov/articles/PMC7010651/ PMC Sahbaie, P., et al. (2019). Mild Traumatic Brain Injury causes nociceptive sensitization via spinal chemokines and 5-HT3. Scientific Reports. https://www.nature.com/articles/s41598-019-55739-x Nature Widerström-Noga, E., et al. (2016). Subacute pain after TBI is associated with pain catastrophizing and fear of movement. Archives of Physical Medicine and Rehabilitation. https://pmc.ncbi.nlm.nih.gov/articles/PMC4931745/ PMC Clinical & educational resources provided by the user (contextual perspectives): Dr. Alexander Jimenez (clinical perspective links):
https://dralexjimenez.com/ | https://www.linkedin.com/in/dralexjimenez/ Video (education):
Sciatica explained (YouTube). https://www.youtube.com/watch?v=iBzwl9h5BUw General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and to identify relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Teaching is a calling—and it’s also a physically demanding job. Long hours on your feet, standing at the board, crouching to help students, carrying books and laptops, rushing between classes, and then sitting for grading and lesson planning can all strain your lower back and hips. Over time, these stresses can irritate the sciatic nerve, leading to sciatica—a pain that can radiate from the lower back into the buttock, thigh, and even the calf or foot. The good news is that targeted chiropractic care, improved ergonomics, regular movement breaks, and simple exercises can help lower your risk and aid in recovery. Integrative care—combining chiropractic with physical therapy strategies, stress management, and healthy daily habits—often gives teachers the best results (Anchor to Health Chiropractic, 2021; Boyne Ergonomics, n.d.; East Bay Chiropractic, n.d.). In El Paso, Dr. Alexander Jimenez, DC, APRN, FNP-BC, and his team use a dual-scope approach (chiropractic + nurse practitioner) to connect symptoms with root causes, guide imaging when needed, and coordinate treatment and legal documentation for work injuries, personal injuries, sports injuries, and motor vehicle accidents (MVAs) (Jimenez, n.d.). This guide explains why teachers are at risk, how to recognize sciatica, what chiropractic and integrative care can do to help, and how to set up your classroom and routine to protect your spine. What Is Sciatica? Sciatica describes irritation or compression of the sciatic nerve or its roots (usually L4–S3). You may feel: -
Sharp, burning, or shooting pain down one leg -
Numbness or tingling (paresthesia) -
Weakness with lifting the foot or standing from a chair -
Pain that worsens with prolonged sitting or standing, bending, or twisting Common drivers include disc bulging or herniation, facet irritation, tight hip musculature, or poor lumbopelvic mechanics. Postural strain and repetitive loading—both common in teaching—can make symptoms flare (Scoliosis Center of Utah, n.d.; Active Health & Wellness Center, n.d.). Why Teachers Are at Higher Risk Teaching looks simple from the outside; in reality, it’s a full-body job. Several daily demands raise sciatica risk: -
Prolonged Standing and Walking
Hall duty, labs, assemblies, and lecturing keep you upright for hours. Static standing loads the lower back and hips. Without micro-breaks, tissues fatigue and joints stiffen (East Bay Chiropractic, n.d.). -
Prolonged Sitting
Lesson planning and grading often happen at the computer. Sitting in a flexed posture for an extended period can increase disc pressure and sensitize the nerve roots (Bomberg Chiropractic, n.d.). -
Awkward Postures
Bending to help students, leaning over desks, twisting to write on boards, or crouching by low tables all add repetitive strain (Boyne Ergonomics, n.d.). -
Carrying Loads
Laptops, stacks of papers, and classroom supplies create asymmetrical loading that can irritate the low back and gluteal muscles. -
Stress and Time Pressure
Stress increases muscle tension and pain sensitivity, which can amplify sciatica symptoms (Paragon Chiropractic, n.d.). -
Mixed Movement Demands
Teachers often cycle between long-standing and long sitting—the worst of both worlds for the spine if not balanced with targeted movement and support (Anchor to Health Chiropractic, 2021). Chiropractic Care: How It Helps Teachers With Sciatica Chiropractic care focuses on joint mechanics, spinal alignment, and the nervous system. For teachers, a plan may include: -
Spinal and Pelvic Adjustments
Gentle, precise adjustments aim to restore motion in restricted segments, optimize load sharing, and reduce local inflammation, which can lower nerve irritation and referred pain (Innervate Chiropractic, n.d.; AFCadence, n.d.). -
Peripheral Joint Care
The hips, sacroiliac joints, and ankles all contribute to the stability of the lumbar spine. Correcting mechanics below (feet/ankles) and above (hips/thoracic spine) can decrease strain on the low back. -
Soft-Tissue Techniques
Myofascial therapy, trigger point work, and guided stretching can help reduce tension in the gluteal and piriformis muscles, which can mimic or exacerbate sciatica (Artisan Chiro Clinic, n.d.). -
Home Exercise and Mobility Plans
Your chiropractor can prescribe daily mobility drills, hip and core activation exercises, and nerve-friendly stretching techniques that improve stability and reduce flare-ups (Active Health & Wellness Center, n.d.; Alliance Orthopedics, n.d.). -
Ergonomic Coaching
Personalized adjustments to your desk, chair, board height, and classroom layout help maintain healthy posture during teaching and prep (Scoliosis Center of Utah, n.d.; AFCadence, n.d.). -
Prevention Strategy
Periodic “tune-ups,” posture refreshers, and load-management teaching help keep symptoms from returning (Anchor to Health Chiropractic, 2021; East Bay Chiropractic, n.d.). Teacher-specific benefit: Clinics that understand school schedules can plan short, focused visits that fit between classes and after school, while building realistic at-home routines for busy weeks (Total Health Chiropractic, n.d.; East Bay Chiropractic, n.d.). Integrative Care: Better Together While adjustments are powerful, teachers often do best with a multimodal plan: -
Physical Therapy Style Exercises
Hip hinge practice, glute activation exercises (bridges, clams), core endurance training (bird-dogs, plank variations), and graded walking can help reduce strain and support nerve mobility (Alliance Orthopedics, n.d.). A short, teacher-friendly circuit done 4–6 days a week usually works best. -
Mobility + Stretching
Carefully dosed hamstring, hip flexor, and piriformis stretching can improve comfort and reduce recurrence (Active Health & Wellness Center, n.d.). (Avoid aggressive end-range stretches during acute flares.) -
Movement Snacks
1–2 minutes every 30–45 minutes: sit-to-stand, wall angels, hip shifts, ankle rocks. These “micro-breaks” lower tissue stress from static postures (Boyne Ergonomics, n.d.). -
Stress Management
Breathing drills, brief mindfulness exercises, or short walks between classes can help reduce tension and pain sensitivity (Paragon Chiropractic, n.d.). -
Massage Therapy & Acupuncture
These modalities can decrease muscle guarding and help calm nerve-related pain—especially when combined with alignment care and exercise (Jimenez, n.d.). -
Education & Load Management
Learning safe bending, lifting, and carrying strategies for classroom tasks can prevent repetitive strain (Artisan Chiro Clinic, n.d.). The Classroom & Desk Setup: Fast Wins Board/Teaching Station Teacher Desk -
Chair: adjustable height to keep hips slightly above knees; backrest supports the natural lumbar curve. -
Desk height: forearms parallel to the floor when typing. -
Monitor: top third of screen at or slightly below eye level; screen at arm’s length. -
Keyboard/Mouse: keep elbows near sides; avoid reaching and shrugging. -
Foot support: If your feet dangle, use a footrest to maintain pelvic neutrality. Classroom Flow -
Place frequently used items within arm’s reach to reduce the need for twisting. -
Use wheeled carts for heavy loads. -
Alternate tasks: rotate standing, walking, and sitting across the period (Boyne Ergonomics, n.d.). Break Rules -
30–45 minute rule: change position—even briefly—at least every 30–45 minutes (Bomberg Chiropractic, n.d.). -
Micro-drills: 10 wall slides, 10 hip hinges, 5 controlled squats, 30-second brisk walk down the hall. -
Standing cues: Distribute weight evenly, soften your knees, and stack your ribcage over your pelvis. A 10-Minute Teacher Routine (Daily) Always adapt to your comfort and provider guidance. Stop if pain worsens. -
Cat-Camel (1 minute) – gentle spinal mobility. -
Hip Hinge Practice (1 minute) – hands on hips; hinge at hips, neutral spine. -
Glute Bridges (2 minutes) – 2 sets of 10–12. -
Bird-Dog (2 minutes) – 2 sets of 6–8 per side, slow. -
Standing Figure-4 Stretch (2 minutes) – light stretch for glutes/piriformis. -
Nerve-Friendly Hamstring Floss (1–2 minutes) – small, comfortable range (Active Health & Wellness Center, n.d.; Top 5 Core Exercises, 2020). On heavier teaching days, add 5 minutes of brisk walking at lunch or after school. How Dr. Alex Jimenez’s Dual-Scope Approach Supports Teachers (El Paso) Clinical correlation & root-cause mapping
Dr. Jimenez’s team connects your pain pattern with specific tasks (such as board writing, grading posture, and floor work) and movement findings (including hip control and trunk endurance). This helps match care to your teaching reality (Jimenez, n.d.). Dual-scope diagnosis
As a chiropractor and nurse practitioner (DC, APRN, FNP-BC), Dr. Jimenez can evaluate neuromusculoskeletal causes, screen red flags, integrate medical considerations (e.g., medication effects, comorbidities), and coordinate care plans that include conservative care and medical referrals as needed (Jimenez, n.d.). Advanced imaging when appropriate
If symptoms suggest a disc herniation, stenosis, or atypical pattern, the clinic coordinates advanced imaging (e.g., MRI) and reviews results in plain language. Imaging is used to guide, not replace, a functional exam (Jimenez, n.d.). Integrated treatment
Care plans may combine spinal adjustments, soft-tissue therapy, exercise therapy, massage, acupuncture, and ergonomic coaching. For teachers injured in MVAs or workplace incidents, the clinic also assists with legal documentation, timelines, and interprofessional communication (Jimenez, n.d.). Return-to-teach strategy
Plans are in place for school calendars, featuring short visits, home routines, and classroom-friendly movement snacks. Prevention steps are built in—so gains last. Sample 6-Week Roadmap (Teacher Edition) Weeks 0–2: Calm & Align -
Reduce painful loading (limit long static sitting/standing). -
Chiropractic adjustments to restore spinal/pelvic motion. -
Gentle mobility and core activation; posture cues in class. -
Pain-tolerant walking and short heat/ice as advised (Anchor to Health Chiropractic, 2021; Active Health & Wellness Center, n.d.). Weeks 3–4: Rebuild & Balance -
Progress core endurance (bird-dog, side bridge regressions). -
Hip strength (glute bridges, clamshells, step-ups). -
Ergonomic fine-tuning of desk/board; scheduled movement breaks. -
Soft-tissue work for gluteal and piriformis tension. Weeks 5–6: Resilience & Prevention -
Lift mechanics (hip hinge, box lift practice). -
Graded standing tolerance (alternate stances, footrests). -
“Teacher circuit” 10–15 minutes daily; weekly check-ins or tune-ups. -
Stress-reduction micro-routines between periods (Paragon Chiropractic, n.d.). Red Flags: When to Seek Immediate Care -
Progressive leg weakness or foot drop -
New bowel or bladder changes -
Fever, unexplained weight loss, or a history of cancer -
Severe night pain unrelieved by rest If these occur, seek urgent medical evaluation. Frequently Asked Questions 1) Do I have to stop teaching to get better?
Usually not. With load management, movement snacks, and an individualized plan, most teachers can keep working while they heal (East Bay Chiropractic, n.d.; Total Health Chiropractic, n.d.). 2) Will adjustments hurt?
Most adjustments are gentle and feel relieving. Your chiropractor will match techniques to your comfort and presentation (Innervate Chiropractic, n.d.). 3) Are stretches enough?
Stretches help, but the best results come from combining mobility, strength, posture coaching, and ergonomics (Active Health & Wellness Center, n.d.; Alliance Orthopedics, n.d.). 4) What if my pain keeps returning?
Recurring sciatica often reflects unaddressed daily factors—such as desk height, board placement, load carriage, or stress. A targeted prevention plan, combined with periodic tune-ups, is key (Scoliosis Center of Utah, n.d.; AFCadence, n.d.). Quick Teacher Checklist -
□ Board at shoulder-to-eye level -
□ Adjustable chair; hips slightly above knees -
□ Screen at arm’s length; top third near eye level -
□ Keyboard/mouse close; elbows by sides -
□ Movement snack every 30–45 minutes -
□ Short daily core/hip routine (10 minutes) -
□ Balanced bag or wheeled cart for supplies -
□ Stress-calming breath break 2–3×/day Putting It All Together Teachers face a perfect storm of risk factors for sciatica, including prolonged sitting, awkward postures, and time pressure. Chiropractic care can reduce nerve irritation and improve alignment. When you pair adjustments with smart ergonomics, targeted exercise, stress management, and regular movement breaks, you build a classroom routine that protects your back and your career. In El Paso, Dr. Alex Jimenez’s dual-scope clinic integrates chiropractic, nurse practitioner assessment, advanced imaging when indicated, and complementary therapies—plus the documentation support teachers may need after workplace incidents or MVAs—so you can teach with confidence and less pain (Jimenez, n.d.). Understanding Academic Low Back Pain: Impact and Chiropractic Solutions References Anchor Health Chiropractic. (2021, August 20). How chiropractic care can help teachers. Anchor Health Chiropractic. (anchortohealth.com) Bomberg Chiropractic. (n.d.). Sedentary job? Here’s how to keep your body healthy while you sit. Bomberg Chiropractic. (bombergchiropractic.com) Boyne Ergonomics. (2025, September 14). Reducing classroom risk among teachers. Boyne Ergonomics. (Boyne Ergonomics) East Bay Chiropractic (M. Marmorale, DC). (2023, December 28). Benefits of chiropractic care for teachers. East Bay Chiropractic. (East Bay Chiropractic Wellness P.C.) Scoliosis Center of Utah (K. Dean, DC). (2025, May 13). How posture and sciatica are connected: A comprehensive guide to relief. Scoliosis Center of Utah. (scoliosiscenterofutah.com) Tone and Tighten. (n.d.). Top 5 core exercises for sciatica pain relief [Video]. YouTube. (YouTube) Active Health Center. (2024, September 9). Sciatica and chiropractic care: Natural solutions for nerve pain. Active Health Center. Paragon Chiropractic and Wellness Center. (n.d.). What lifestyle changes are most effective in preventing sciatica?. Paragon Chiropractic. (Paragon Chiropractic & Wellness Center) Innervate Chiropractic. (2024, July 31). The top 10 benefits of chiropractic care for teachers: A detailed guide. Innervate Chiropractic. (Innervate Chiropractic) Abundant Life Chiropractic Health Center. (2025, August 11). Back-to-school spine health: Understanding sciatica and how to prevent it. Abundant Life Chiropractic. (Abundant Life Chiropractic Health Center) Alliance Orthopedics. (n.d.). Do I need a chiropractor or physical therapy for sciatica relief?. Alliance Orthopedics. (Alliance Orthopedics) Total Health Chiropractic. (2021, July 10). Can chiropractic care help teachers?. Total Health Chiropractic. (Total Health Chiropractic) Cadence Chiropractic. (2025). Chiropractor-recommended exercises for sciatica relief. Cadence Chiropractic. (afcadence.com) Artisan Chiropractic Clinic. (n.d.). Managing sciatica pain: Chiropractic approaches to consider. Artisan Chiropractic Clinic. (artisanchiroclinic.com) Jimenez, A. (2025, April 17). El Paso, TX doctor of chiropractic. Injury Medical & Chiropractic Center. (El Paso, TX Doctor Of Chiropractic) Jimenez, A. (2025, September 17). Chiropractic care for healing from chronic inflammation. Injury Medical & Chiropractic Center. (El Paso, TX Doctor Of Chiropractic) Jimenez, A. (2025, September 24). Chiropractic and integrative care for drivers in El Paso. Injury Medical & Chiropractic Center. (El Paso, TX Doctor Of Chiropractic) Jimenez, A. (2025, September). Safe chiropractic care in El Paso: What to expect. Injury Medical & Chiropractic Center. (El Paso, TX Doctor Of Chiropractic) General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Sports injuries and sciatica can disrupt your life. Uncover how chiropractic care can aid in your recovery and well-being. Introduction Sciatica pain can feel like an uninvited guest who overstays their welcome, zapping your energy and making every step a challenge. Imagine trying to enjoy a sunny day in El Paso, Texas, but instead, you’re wincing with every move because of a sharp, shooting pain down your leg. Whether you’re an athlete sidelined by a sports injury, a desk warrior battling the effects of a sedentary lifestyle, or someone recovering from a personal injury like a car accident, sciatica can turn your daily routine into a painful ordeal. But here’s the good news: chiropractic care, combined with non-surgical treatments, offers a beacon of hope to kick that pain to the curb. Led by experts like Dr. Alexander Jimenez, DC, APRN, FNP-BC, in El Paso, chiropractic care provides a holistic, evidence-based approach to relieve sciatica and restore your quality of life. In this comprehensive guide (we’re talking over 5,000 words of pure knowledge!), we’ll dive into the nitty-gritty of sciatica—what it is, why it happens, and how it ties into your musculoskeletal system, especially when sports injuries or personal injuries come into play. We’ll explore how chiropractic care, backed by advanced diagnostics and non-surgical treatments, can reduce sciatica pain and its overlapping symptoms. Plus, we’ll share practical tips from Dr. Jimenez’s clinical insights to help you make small changes to your routine for lasting relief. And because we know pain is no laughing matter, we’ll sprinkle in a bit of humor to keep things light—like imagining your sciatic nerve as a grumpy electrician sending out distress signals. Let’s get started and help you say goodbye to sciatica pain! What Is Sciatica and Why Does It Hurt So Much? Sciatica isn’t just a fancy term for back pain; it’s a specific condition caused by irritation or compression of the sciatic nerve, the longest nerve in your body. This nerve runs from your lower back, through your hips and buttocks, and down each leg. When it’s pinched or inflamed, it sends out signals that can feel like a bolt of lightning zapping through your leg. Symptoms vary but often include: - Sharp, shooting pain that radiates from the lower back to the foot.
- Numbness or tingling in the leg or foot, like pins and needles on steroids.
- Weakness in the leg, making it hard to move or stand.
- Burning sensation that feels like your leg is auditioning for a spicy food commercial.
Sciatica is more common than you might think, affecting over 3 million people annually in the United States (El Paso Back Clinic, 2018). It typically strikes folks between 30 and 50 years old, but anyone can fall victim if the conditions are right. The pain can range from a mild annoyance to a debilitating force that makes you want to trade your active lifestyle for a permanent spot on the couch. Causes of Sciatica: The Usual Suspects Sciatica isn’t a condition that shows up out of nowhere—it’s usually triggered by something pressing on or irritating the sciatic nerve. Here are the main culprits: - Herniated or Bulging Discs: The spinal discs act like cushions between your vertebrae, but when they bulge or herniate, they can press on the sciatic nerve roots in the lumbar spine, causing pain. Think of it like a jelly donut squishing out its filling and pinching a nerve in the process.
- Piriformis Syndrome: The piriformis muscle, a small muscle in your buttocks, can sometimes cramp or spasm, squeezing the sciatic nerve that runs beneath it. This is a common cause of “nondiscogenic” sciatica (Boyajian-O’Neill et al., 2008).
- Spinal Stenosis: This is when the spinal canal narrows, putting pressure on the nerves, including the sciatic nerve. It’s like trying to squeeze through a crowded hallway with no room to move.
- Spondylolisthesis: When a vertebra slips out of alignment, it can compress the sciatic nerve, leading to pain and discomfort.
- Sports Injuries: Athletes, especially those in high-impact sports like football, basketball, or running, can injure their lower back or pelvis, leading to sciatica. A broken pelvis, for example, can misalign the spine or pelvis, irritating the sciatic nerve (El Paso Back Clinic, n.d.-a).
- Non-Spinal Causes: Things like pregnancy, obesity, or even sitting on a thick wallet (yep, “wallet sciatica” is a real thing!) can irritate the sciatic nerve (Hicks et al., 2021).
Sports Injuries and Sciatica: A Painful Connection Sports injuries are a significant contributor to sciatica, especially for active folks in El Paso who love their outdoor adventures or competitive sports. High-impact activities can strain the musculoskeletal system, leading to issues like: - Pelvic Fractures: A broken pelvis, as noted in cases treated at El Paso Back Clinic, can disrupt the alignment of the spine and pelvis, putting pressure on the sciatic nerve (El Paso Back Clinic, n.d.-a). Imagine your pelvis as the foundation of a house—if it’s cracked, the whole structure feels off.
- Muscle Strains: Overuse or sudden movements in sports like soccer or tennis can strain the piriformis or other gluteal muscles, leading to nerve compression.
- Disc Injuries: Repetitive stress from activities like weightlifting or gymnastics can cause disc herniations, a leading cause of sciatica.
These injuries disrupt the musculoskeletal system’s balance, which includes bones, muscles, ligaments, and tendons working together to keep you moving. When one part is injured, it can throw everything out of whack, leading to nerve irritation and sciatica pain. References: - El Paso Back Clinic. (n.d.-a). Low back pain & sciatica caused by a broken pelvis. https://elpasobackclinic.com/low-back-pain-sciatica-caused-broken-pelvis/
- Boyajian-O’Neill, L. A., et al. (2008). Piriformis syndrome: A cause of nondiscogenic sciatica. Current Sports Medicine Reports, 7(5), 278–283. https://pubmed.ncbi.nlm.nih.gov/18772682/
- Hicks, B. L., et al. (2021). Extra-spinal sciatica and sciatica mimics: A scoping review. The Korean Journal of Pain, 34(3), 305–317. https://pubmed.ncbi.nlm.nih.gov/34289262/
- El Paso Back Clinic. (2018). Sciatica pain treatment in El Paso, TX, chiropractic care | Video. https://elpasobackclinic.com/sciatica-pain-treatment-el-paso-tx-chiropractor-dr-alex-jimenez/
The Musculoskeletal System: The Body’s Framework Your musculoskeletal system is like the scaffolding of a building—it provides structure, support, and the ability to move. It includes: - Bones: The framework that holds you upright.
- Muscles: The engines that power movement.
- Ligaments and Tendons: The connectors that keep everything in place.
- Joints: The hinges that allow flexibility.
When sciatica strikes, it’s often because something in this system is out of alignment or injured. For example, a herniated disc can press on nerve roots, or a tight piriformis muscle can pinch the sciatic nerve. Sports injuries, like a broken pelvis or a strained muscle, can disrupt this delicate balance, leading to pain that radiates down the leg. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Uncover the benefits of chiropractic care for better spinal health and sciatica pain management strategies with various poses. Introduction Sciatica pain can feel like an uninvited guest who overstays their welcome, radiating discomfort from your lower back down to your legs, making even simple tasks like sitting or walking feel like a Herculean effort. If you have ever experienced a sharp, shooting pain or that annoying tingling sensation, you know it is no laughing matter—though we will sprinkle in a small quantity of humor to keep things light. This blog post explores the clinical rationale behind why chiropractic care can be a game-changer for reducing sciatica pain associated with low back pain. We will explore the musculoskeletal system’s role, how sciatica impacts daily life, and why Dr. Alexander Jimenez, a distinguished chiropractor in El Paso, TX, is a go-to expert for personal injury cases. We will also weave in evidence-based insights, some yoga-inspired poses, and a touch of wit to make this journey through sciatica both informative and engaging. What Is Sciatica, and Why Does It Hurt So Much? Sciatica is not a condition but a symptom of an underlying issue affecting the sciatic nerve, the longest nerve in the human body, stretching from the lower back through the hips, past the buttocks, and down each leg. When this nerve gets irritated or compressed, it can cause pain, numbness, tingling, or weakness, typically radiating from the lower back to the leg or foot. Imagine your sciatic nerve as a superhighway for signals between your brain and legs—when there is a traffic jam (compression), chaos ensues, and your body lets you know with a vengeance. The pain can range from a mild, irritating ache to a sharp, electric-shock-like sensation. For some, it is like a cranky pirate jabbing you with a dull sword; for others, it is a constant burning that makes you want to negotiate a truce with your own body. Sciatica often stems from conditions like a herniated disc, spinal stenosis, piriformis syndrome, or even pregnancy, which can press on the nerve roots or the sciatic nerve itself (Fernandez et al., 2016). The Musculoskeletal System and the Sciatic Nerve The musculoskeletal system—your body’s framework of bones, muscles, ligaments, and tendons—plays a starring role in sciatica. The sciatic nerve exits through the spine through the lumbar and sacral regions, passing through or near muscles like the piriformis in the buttocks. When the spine is misaligned (a subluxation), a disc bulges, or a muscle tightens excessively, it can pinch and entrap the sciatic nerve, leading to pain and dysfunction. For example, a herniated disc might act like a bully, shoving the nerve against nearby structures, while a tight piriformis muscle can squeeze the nerve like an overzealous hug. This disruption affects not just the nerve but also the surrounding muscles and joints, leading to compensatory movements that can worsen pain or cause additional strain. For instance, if your lower back is out of alignment, you might limp or shift your weight, which throws off your posture and stresses other parts of your body, like a domino effect in a poorly planned game of Jenga. How Sciatica Impacts Daily Life Sciatica can turn routine activities into Olympic-level challenges. Sitting for long periods, like during a Netflix binge or a work-from-home marathon, can intensify the pain. Standing up might feel like you are auditioning for a role as a wobbly giraffe. Walking, bending, or even sneezing can trigger a flare-up, leaving you feeling like you have angered an invisible sciatic gremlin. According to a systematic review, sciatica affects 2-5% of the general population, with up to 43% prevalence in certain working groups, significantly impacting productivity and quality of life (Ropper & Zafonte, 2015). The emotional toll is no joke either. Chronic pain can lead to various emotions of frustration, anxiety, or even depression, especially when it lingers beyond the typical two-week recovery period, as seen in about 30% of cases (Ropper & Zafonte, 2015). Missing out on family outings, struggling at work, or avoiding hobbies can make you feel like sciatica is stealing your joy faster than a seagull snatching your beachside fries. References - Fernandez, M., Hartvigsen, J., Ferreira, M. L., Refshauge, K. M., Machado, A. F., Lemes, Í. R., Maher, C. G., & Ferreira, P. H. (2016). Advice to stay active or structured exercise in the management of sciatica: A systematic review and meta-analysis. Spine, 41(18), 1457-1466. https://pubmed.ncbi.nlm.nih.gov/26926164/
- Ropper, A. H., & Zafonte, R. D. (2015). Sciatica. New England Journal of Medicine, 372(13), 1240-1248. https://pubmed.ncbi.nlm.nih.gov/25806916/
Why Chiropractic Care? The Clinical Rationale Chiropractic care, particularly as practiced by experts like Dr. Alexander Jimenez, DC, APRN, FNP-BC, offers a non-invasive, evidence-based approach to managing sciatica pain. Unlike popping painkillers like candy (which only mask the problem and come with side effects), chiropractic care targets the root cause—whether it is a misaligned spine, a herniated disc, or muscle tension. Here is why it works, backed by clinical insights and a sprinkle of humor to keep you from dozing off. Restoring Spinal Alignment Chiropractic adjustments focus on correcting spinal misalignments (subluxations) that may compress the sciatic nerve or its roots. By using precise, controlled force, chiropractors like Dr. Jimenez realign the spine, reducing pressure on the nerve and restoring proper function. Think of it like untangling a knot in your earbuds—once the kink is gone, the music (or in this case, nerve signals) flows smoothly again. A 2020 study found that spinal manipulative therapy can significantly reduce chronic pain and disability in patients with chronic low back pain, which often accompanies sciatica (Rubinstein et al., 2020). Reducing Inflammation and Muscle Tension Sciatica often comes with inflammation and muscle spasms, like your body’s attempt to throw a tantrum. Chiropractic care incorporates techniques like deep-tissue massage and trigger point therapy to relax tight muscles, such as the piriformis, which can compress the sciatic nerve. Dr. Jimenez’s integrative approach also includes lifestyle and nutritional counseling to reduce systemic inflammation, helping your body calm down without resorting to a pharmacy’s worth of drugs (Jimenez, 2024). General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction: Understanding the Link Between Car Accidents and Sciatica Car accidents can cause more than just bruises or broken bones. Even a minor collision can lead to serious damage inside the body, especially in the back and spine. One of the most painful and long-lasting conditions people may experience after an accident is sciatica. Sciatica is a condition in which the sciatic nerve—the largest nerve in the body—becomes pinched or inflamed. This nerve originates from the lower back and extends down through the hips, buttocks, and legs. After a crash, the force can cause a herniated disc, spinal misalignment, or inflammation, which puts pressure on this nerve, causing sharp pain, numbness, or tingling that radiates down the leg. Research confirms that motor vehicle accidents (MVAs) are a common cause of sciatica due to the high impact they create on the spine and surrounding structures. If left untreated, sciatica can lead to long-term disability and chronic pain (Portland Urgent Care, n.d.). A team-based approach to care—combining chiropractic therapy and nurse practitioner management—can be a game changer. Chiropractors focus on restoring spinal alignment and reducing pressure on nerves, while nurse practitioners manage pain, order diagnostic tests, and coordinate care. Working together, they provide a complete and personalized recovery plan for people dealing with sciatica after a car crash. In this article, we’ll explore: -
How MVAs cause sciatica -
What symptoms to watch for -
How chiropractic and integrative medicine can help -
The role of nurse practitioners -
Why Dr. Alexander Jimenez’s dual-scope care in El Paso is uniquely effective Let’s dive into the details of this powerful healthcare partnership. Versus Texas, n.d. How Motor Vehicle Accidents Cause Sciatica A car crash may only last a few seconds, but the damage it causes can last for months—or even years. When the body is jolted during a collision, especially from behind (as in a rear-end accident), it can cause sudden movement of the spine. This often results in spinal misalignments, herniated discs, or joint inflammation, all of which can press on the sciatic nerve and trigger intense pain. Common Spinal Injuries Leading to Sciatica After a Crash: -
Herniated or Bulging Discs: The jelly-like cushions between the bones of the spine can rupture or slip out of place. This can pinch or compress the sciatic nerve. -
Spinal Misalignment: Even a slight shift in the vertebrae can cause nerve irritation or swelling around the sciatic nerve. -
Pelvic or Lower Back Trauma: Any impact to the pelvis or sacroiliac joint can put extra stress on the sciatic nerve’s pathway. After a motor vehicle accident, some injuries exhibit symptoms immediately. Others develop more slowly, especially those involving nerve compression. People may not notice sciatica until days or even weeks later, when they begin to feel tingling, burning, or shooting pain down one leg. This is why early assessment by a chiropractor or nurse practitioner is so important (Team Allied, n.d.). Symptoms of Post-Accident Sciatica -
Sharp, burning, or stabbing pain in the lower back or buttocks -
Pain radiating down the back of one leg. -
Numbness, tingling, or weakness in the leg or foot -
Increased pain with sitting, standing, or certain movements -
Limited mobility or inability to walk comfortably If any of these symptoms appear after a car accident, it’s critical to seek medical attention right away to avoid long-term damage. Chiropractic care and integrative health management can help reduce inflammation, restore mobility, and support the body's natural healing process. HM Attorneys, n.d. The Role of Chiropractic Care in Treating Sciatica Chiropractic care focuses on the musculoskeletal system, especially the spine and nervous system. When someone experiences sciatica after a car accident, chiropractors aim to relieve pressure on the sciatic nerve by correcting spinal misalignments, improving posture, and restoring natural movement. How Chiropractors Help with Sciatica: -
Spinal Adjustments
These hands-on manipulations help realign the vertebrae. When the spine is properly aligned, the pressure on the sciatic nerve can be reduced, easing pain and inflammation. -
Spinal Decompression Therapy
This non-surgical treatment gently stretches the spine to create space between vertebrae. It’s often used to relieve pressure caused by herniated or bulging discs, a common cause of sciatica after accidents (OC Spinal Care, n.d.). -
Therapeutic Exercises and Posture Correction
Chiropractors often teach stretching and strengthening exercises to reduce pressure on the lower back and improve muscle support. Correcting posture also helps prevent future flare-ups. -
Soft Tissue Therapy
Massage techniques and myofascial release help relieve muscle tension around the sciatic nerve and reduce inflammation caused by trauma. According to The Neck and Back Clinics, integrating chiropractic care after an auto accident can improve patient outcomes by accelerating recovery and helping prevent further injury. Chiropractors assess the entire body to identify imbalances, rather than just treating pain symptoms. (The Neck and Back Clinics, n.d.). Why It Matters After a Car Accident: -
Reduces pain without medication -
Restores function naturally -
Prevents long-term damage -
Improves nerve communication and body healing Chiropractic care is most effective when started early after an accident. It's also especially powerful when combined with support from a nurse practitioner and an integrative care team. Charleston Chiro Studio, n.d. The Nurse Practitioner’s Role in Sciatica Care After a Car Accident While chiropractors focus on spinal alignment and nerve function, nurse practitioners (NPs) play a crucial role in addressing the overall medical needs of patients with post-accident sciatica. Their advanced training enables them to evaluate injuries, prescribe treatments, and coordinate care with other specialists to ensure patients receive well-rounded, timely support. What Nurse Practitioners Do for MVA-Related Sciatica: -
Comprehensive Medical Evaluation
NPs take a detailed history, perform physical examinations, and assess neurological symptoms, such as weakness or numbness. They evaluate not only the back injury but also check for other trauma sustained in the crash. -
Ordering Diagnostic Imaging
To properly assess damage to the spine or discs, NPs can order X-rays, MRIs, or CT scans. These images help pinpoint nerve compression or disc herniation contributing to sciatica. -
Pain Management
Nurse practitioners can prescribe anti-inflammatories, muscle relaxants, or pain relievers. They also use non-drug techniques, such as heat, cold, or physical therapy referrals. Their approach balances relief with safety, especially for patients who want to avoid long-term medication use. -
Coordinating Specialist Referrals
If a case is complex, NPs help connect patients to orthopedic surgeons, neurologists, or physical therapists. They often act as the care manager, making sure everyone is working together on the patient’s recovery plan. -
Supporting Lifestyle and Nutrition
Nurse practitioners often recommend changes in diet, supplements, hydration, and sleep to promote nerve healing. These supportive strategies are vital for long-term improvement. As described by the Physicians Group, nurse practitioners are essential in helping auto-injury patients avoid complications by managing symptoms early, reducing the risk of chronic pain, and improving overall outcomes. (Physicians Group LLC, n.d.). Why Integrating Nurse Practitioners Improves Outcomes: -
Medical oversight of complex symptoms -
Timely diagnosis through imaging -
Safer and more personalized treatment -
Seamless coordination with chiropractic care Together, chiropractors and NPs form a comprehensive team that covers every aspect of healing, from spinal adjustments to medical diagnostics and pain control. LinkedIn: Dr. Alexander Jimenez, n.d. Dual-Scope Healing: Dr. Alexander Jimenez’s Approach to Sciatica and Injury Recovery In El Paso, Dr. Alexander Jimenez stands out as a healthcare provider who bridges the gap between chiropractic care and medical management. As a Doctor of Chiropractic (DC) and Advanced Practice Registered Nurse (APRN, FNP-BC), he provides a unique “dual-scope” approach that benefits patients recovering from motor vehicle accidents, especially those with sciatica. Dr. Jimenez’s approach doesn’t just treat the pain—it addresses the cause, manages the full picture of injury, and prepares documentation for legal claims when needed. Why Dr. Jimenez’s Dual Role Matters: -
Chiropractic Precision + Medical Oversight
He combines spinal adjustments with evidence-based medical care to treat the mechanical and neurological aspects of sciatica. His care helps relieve nerve compression while addressing inflammation and tissue damage. -
Enhanced Imaging and Diagnostics
Using advanced diagnostic tools, such as MRI and digital motion X-rays, Dr. Jimenez can pinpoint spinal injuries with precision. This is especially helpful for uncovering subtle causes of nerve pain that might otherwise be missed. -
Integrated Legal-Medical Documentation
For personal injury cases, accurate records are essential. Dr. Jimenez creates detailed evaluations, injury causation reports, and functional assessments that support patients in both their recovery and legal process. -
Nutritional and Functional Medicine Support
Recovery isn’t just about the spine. Dr. Jimenez includes personalized nutrition plans, gut health protocols, and fitness recommendations to reduce inflammation, boost energy, and strengthen recovery from the inside out. -
Collaboration with Legal Teams
He understands how to interface with attorneys handling personal injury cases. His reports meet legal standards and support the documentation needed for compensation claims related to pain and suffering, lost work time, or long-term injury. According to his clinical observations, many post-accident patients suffer from undiagnosed spinal trauma that leads to nerve entrapment and chronic conditions like sciatica. His dual-scope practice fills this gap, offering both chiropractic relief and medical guidance under one roof (Dr. Alexander Jimenez, n.d.). What Patients Can Expect: -
A full diagnostic workup -
Hands-on chiropractic adjustments -
Nurse practitioner-led care plans. -
Health coaching for long-term healing -
Coordination with legal and insurance needs Dr. Jimenez’s clinic in El Paso represents the future of integrative post-accident care—efficient, accurate, and deeply supportive for patients in pain who need answers. LinkedIn: Dr. Jimenez, n.d. The Benefits of Integrative Medicine for Sciatica After Car Accidents When it comes to recovering from sciatica caused by a motor vehicle accident, using a combination of therapies—known as integrative medicine—can provide faster, more complete healing. This approach doesn’t rely on just one type of care. Instead, it combines the best of chiropractic treatment, medical support, nutrition, physical therapy, and lifestyle coaching to treat the whole person. What Is Integrative Medicine? Integrative medicine focuses on healing the root cause of pain while also improving overall health and function. It often includes: -
Chiropractic adjustments -
Nurse practitioner medical evaluations -
Nutritional therapy -
Physical therapy and movement-based rehab -
Stress management and sleep hygiene -
Functional medicine approaches to inflammation and gut health This team-based strategy is especially helpful for sciatica, which can involve both mechanical pressure on the nerve and systemic issues, such as inflammation or muscle imbalance. Benefits of a Whole-Person Approach: -
Addresses Multiple Causes of Pain
Nerve pain can be caused by a herniated disc, inflammation, poor posture, or muscle weakness. Integrative care addresses all of these simultaneously. -
Reduces Reliance on Pain Medications
Through adjustments, nutrition, decompression, and guided movement, patients can find relief naturally, often avoiding long-term use of prescription drugs. -
Improves Recovery Speed and Function
Research indicates that combining chiropractic care with physical therapy and lifestyle coaching facilitates faster recovery, with fewer complications. (Thrive VB, n.d.). -
Promotes Long-Term Wellness
Integrative care doesn’t just treat the accident injury—it sets patients up with tools for lifelong health, such as healthy eating, proper posture, and stress reduction. -
Improves Communication Among Providers
When chiropractors, nurse practitioners, and health coaches collaborate, patients receive personalized, efficient, and well-coordinated care. Mission Village Chiropractic emphasizes that this type of care facilitates improved patient education and more effective recovery plans. Chiropractors not only treat pain but also provide coaching on lifestyle changes, posture, and exercise that can prevent future flare-ups. (Mission Village Chiropractic, n.d.). A Unified Path to Healing In El Paso and similar communities, dual-scope providers like Dr. Alexander Jimenez are leading the way in this kind of comprehensive, patient-centered care. His clinic combines chiropractic work with nurse practitioner expertise, nutritional coaching, and legal-medical documentation—all under one roof. When care is coordinated, personalized, and integrative, patients recovering from sciatica after a car accident are more likely to return to their normal lives with less pain and more confidence. Step-by-Step: What to Do If You Think You Have Sciatica After a Car Accident If you’ve been in a car accident and start feeling pain in your lower back, buttocks, or leg, it could be a sign of sciatica. Acting quickly can make a big difference in your recovery. Here’s a simple step-by-step guide to help you take the right actions. 1. Pay Attention to Your Symptoms Look for signs like: -
Sharp or burning pain in the leg -
Numbness or tingling in the foot -
Pain that worsens when sitting or bending -
Weakness in the leg or difficulty walking If these symptoms show up within days or weeks of your accident, don’t ignore them. 2. See a Dual-Scope Provider Choose a clinic that offers both chiropractic and nurse practitioner care, like Dr. Alexander Jimenez’s team in El Paso. This allows you to receive spinal assessments, imaging, and medical care all in one place. The team will: -
Perform a physical exam -
Order imaging (like MRI or X-ray) -
Begin pain management and spinal treatments -
Coordinate any additional care you might need Portland Urgent Care, n.d. 3. Start Chiropractic and Medical Treatment Early intervention is key. Chiropractors can relieve pressure on the sciatic nerve through gentle adjustments and decompression techniques. Nurse practitioners may prescribe medication or refer you for additional testing or therapies if needed. OC Spinal Care, n.d. 4. Follow Up with Lifestyle Support This may include: -
Physical therapy -
Nutritional changes -
Supplements to reduce inflammation -
Posture improvement exercises -
Stress management and sleep tips A well-rounded care plan enhances healing and helps prevent chronic sciatica from developing. (Thrive VB, n.d.) 5. Document Everything for Legal Purposes In personal injury cases, proper documentation is essential. Dr. Jimenez and providers like him supply: This can help protect your rights and ensure that you receive compensation for your injuries and care. Dr. Alexander Jimenez, n.d. Conclusion: Finding the Right Care for Sciatica After an Accident Recovering from a car accident is hard enough—dealing with sciatica makes it even harder. The pain, weakness, and limited movement caused by pressure on the sciatic nerve can interfere with your daily life, job, and overall well-being. But with the right team by your side, healing is not only possible—it’s personalized and powerful. Why Choose a Dual Chiropractic and Nurse Practitioner Approach? Sciatica is not just a bone or nerve problem—it’s a complex condition involving spinal misalignment, inflammation, muscle strain, and sometimes systemic imbalances. That’s why combining chiropractic care with nurse practitioner management creates the best outcomes. Chiropractors address the structure of the spine and relieve pressure on the nerve. Nurse practitioners address the function of the body, order tests, and manage medications or other therapies. Together, they treat the whole person—not just the symptoms. This approach works best when it’s backed by: -
Advanced diagnostics and imaging -
Hands-on spinal therapy -
Pain management and inflammation control -
Nutritional support and lifestyle coaching -
Detailed documentation for legal and insurance needs Dr. Alexander Jimenez and his team in El Paso are leaders in this kind of integrated care. With his dual-scope background as both a Doctor of Chiropractic and a Family Nurse Practitioner, Dr. Jimenez brings unmatched depth and expertise to every case, particularly in complex sciatica cases resulting from car accidents. His clinic provides: -
A one-stop shop for medical and chiropractic care -
Imaging, therapy, and nutritional services -
Legal-medical documentation support -
Personalized recovery plans that treat the root cause Whether you're experiencing pain now or suspect a hidden injury from a past accident, don’t wait. Early care leads to better outcomes, reduced pain, and a return to the things you love. References General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Can a paraspinal muscle spasm in the lower back create a chain reaction leading to hamstring spasms and potential sciatic nerve entrapment? Paraspinal Muscle Spasm Chain Reaction A paraspinal muscle spasm in the lower back can cause a cascade of events, including: (Cedars-Sinai, 2025) - Spasms in other lower back muscles
- Hamstring spasms
- Potential entrapment of the sciatic nerve
Leading to symptoms similar to sciatica: - Pain
- Sore, achy muscles
- Weak muscles
- Numbness
- Tingling along the back of the leg
Possible Mechanisms Triggering Muscle Spasms in the Lower Back - Paraspinal muscles are located along the spine and help to stabilize and support the lower back.
- When these muscles spasm, they can become tense and painful, causing a chain reaction.
- This tension can radiate down and affect other muscles in the lower back. (Noonan A. M., & Brown S. H. M., 2021)
Can Affect Lower Back Muscles and Cause Hamstring Spasms - Lower back muscles, including those like the quadratus lumborum, can be affected by paraspinal spasms. (Hospital for Special Surgery, 2024)
- The spasms can cause these muscles to tighten or spasm, potentially pulling on the hamstring muscles.
- This can lead to hamstring spasms and tightness, further contributing to pain and potential nerve irritation.
Entrapment of the Sciatic Nerve - Piriformis syndrome is a common condition where the piriformis muscle (located in the buttock) spasms and compresses the sciatic nerve. (Cedars-Sinai, 2025)
- The sciatic nerve runs from the lower back down the back of the thigh and into the leg, making it vulnerable to compression by surrounding muscles.
- If the paraspinal and hamstring spasms create enough tension on the piriformis muscle or surrounding tissues, it can lead to sciatic nerve entrapment. (Hospital for Special Surgery, 2024)
How acupuncture helps relieve sciatica Acupuncture can help relieve sciatica pain by stimulating specific points on the body, which can trigger the release of endorphins, reduce inflammation, improve blood flow, and relax tight muscles that could be compressing the sciatic nerve. By modulating the nervous system and promoting the body's natural healing processes, acupuncture can help alleviate pain and improve overall function. (Qin, Z. et al., 2015) Releases endorphins - Acupuncture stimulates the nervous system, triggering the release of endorphins, the body's natural painkillers.
Reduces inflammation - Acupuncture can help reduce inflammation in the area surrounding the sciatic nerve, which can contribute to pain and nerve irritation. (Natural Care Chiropractic, 2022)
Improves circulation - By increasing blood flow to the affected area, acupuncture can help deliver nutrients and oxygen to the sciatic nerve and surrounding tissues, promoting faster healing.
Relaxes tight muscles - Sciatica pain can be exacerbated by tight muscles compressing the nerve. Acupuncture can help relax these muscles, reducing pressure on the sciatic nerve and alleviating pain.
Regulates the nervous system - Acupuncture can help regulate the nervous system, positively impacting pain perception and overall well-being. (Qin, Z. et al., 2015)
Promotes regeneration - Some evidence suggests that acupuncture can promote sciatic nerve regeneration, potentially leading to long-term pain relief. (Natural Care Chiropractic, 2022)
Needling Types Distal needling - Acupuncture can also involve using points that are further away from the site of pain, which can also help to reduce pain and inflammation.
Local needling - Points are also selected on or near the sciatic nerve's path, which can help directly address the source of pain and inflammation. (Qin, Z. et al., 2015)
Holistic approach - Acupuncture is often viewed as a holistic approach to pain management, addressing the symptoms of sciatica and the underlying causes and imbalances in the body.
Injury Medical Chiropractic and Functional Medicine Clinic As a Family Practice Nurse Practitioner, Dr. Jimenez combines advanced medical expertise with chiropractic care to address various conditions. Our clinic integrates Functional Medicine, Acupuncture, Electro-Acupuncture, and Sports Medicine to create customized care plans that promote natural healing, mobility, and long-term wellness. By focusing on flexibility, agility, and strength, we empower patients to thrive, regardless of age or health challenges. At El Paso’s Chiropractic Rehabilitation Clinic & Integrated Medicine Center, we passionately focus on treating patients after injuries and chronic pain syndromes. We focus on improving your ability through flexibility, mobility, and agility programs tailored for all age groups and disabilities. We use in-person and virtual health coaching and comprehensive care plans to ensure every patient’s personalized care and wellness outcomes. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Cedars Sinai. (2025). Piriformis Syndrome. https://www.cedars-sinai.org/health-library/diseases-and-conditions/p/piriformis-syndrome.html#:~:text=Overview,can%20run%20through%20the%20muscle) Noonan, A. M., & Brown, S. H. M. (2021). Paraspinal muscle pathophysiology associated with low back pain and spine degenerative disorders. JOR spine, 4(3), e1171. https://doi.org/10.1002/jsp2.1171 Hospital for Special Surgery. (2024). Sciatica. https://www.hss.edu/condition-list_sciatica.asp Qin, Z., Liu, X., Wu, J., Zhai, Y., & Liu, Z. (2015). Effectiveness of Acupuncture for Treating Sciatica: A Systematic Review and Meta-Analysis. Evidence-based complementary and alternative medicine: eCAM, 2015, 425108. https://doi.org/10.1155/2015/425108 Natural Care Chiropractic, D. M. F. (2022). Acupuncture for Sciatica Pain Relief. https://www.naturalcarechiropractic.com/post/acupuncture-for-sciatica-pain-relief
For individuals experiencing lower back pain and sciatica symptoms, can using a lidocaine patch help? Lidocaine Patch Lidocaine patches are in a drug class called local anesthetics (MedlinePlus, 2025) (Food and Drug Administration, 2022). They relieve pain in small body areas by blocking the nerves from sending pain signals. The Food and Drug Administration approved lidocaine 5% or 1.8% patches for relieving postherpetic neuralgia (PHN) pain. These lidocaine patches are prescription-only (Food and Drug Administration, 2022). They are available either by prescription or over the counter and are commonly used for back pain and other areas. Over-the-counter lidocaine, 4% patches, can be used to relieve minor aches and pains, including back pain. However, further research is needed to recommend the use of lidocaine patches as an effective method of pain relief. (Department of Veterans Affairs/Department of Defense, 2022) (North American Spine Society, 2020) The Patch They are available in prescription and over-the-counter forms. Over-the-counter forms come as a 4% patch in various brands, such as (MedlinePlus, 2025) - Aspercreme
- Lidocare
- Salonpas
Prescription-only patches come in 5% or 1.8% patches and are approved to relieve long-term nerve pain from shingles in adults. Zlido is a brand name for a 1.8% lidocaine patch. Five percent lidocaine patches are available generically. (DailyMed, 2018) (Food and Drug Administration, 2021) The safety and effectiveness in children are unknown. (Food and Drug Administration, 2022) Other Lidocaine Forms As a local anesthetic, it is available in several other forms, including: - Spray
- Topical cream
- Lotion
- Liquid
- Ear drops
- Eye gel
- Injection
- It is also available as a short-term intravenous infusion for abnormal heart rhythm. (DailyMed, 2025)
Effectiveness Clinical trials have shown that the patches effectively relieve chronic low back pain. However, these studies were nonrandomized and did not include a control group to compare against the treatment group. (Santana J. A., Klass S., & Felix E. R. 2020) The results may be subject to potential biases. For this reason, further evidence is needed to support lidocaine patches' effectiveness in reducing low back pain. (North American Spine Society, 2020) High-quality randomized and controlled clinical trials are necessary to study the effectiveness. (North American Spine Society, 2020) (Santana J. A., Klass S., & Felix E. R. 2020) How to Use Safely In general, keep the following in mind (MedlinePlus, 2025) - Use according to the directions on the box and the healthcare provider's recommendations.
- Do not use on broken or inflamed, swollen skin.
- Do not apply heat like heating pads or electric blankets over patches.
- Avoid getting water on or around the patch.
- Avoid letting a patch near your eyes to limit eye irritation.
- Fold the sticky sides of the used lidocaine patches together and safely throw them away, keeping them away from children and pets.
How to use (MedlinePlus, 2025) - Clean and dry the affected area before placing the patch.
- Apply to the affected body area as directed.
- Wash your hands after touching the patch.
- Remove the patch after what is usually recommended after eight hours.
How Quickly Does It Work? The amount of medication absorbed into the blood depends on how long the patch is placed on the body and how much is covered with the patch. In a study, healthy participants wore three lidocaine patches on their backs for 12 hours on and 12 hours off during 24 hours. Lidocaine levels were highest at 11 hours. At the end of the 24 hours, there was still some lidocaine left in the bloodstream. (Food and Drug Administration, 2022) Individuals with PHN may notice a difference in pain intensity after four hours of using the patch. (Rowbotham, M. C. et al., 1996) (Food and Drug Administration, 2022) Experts may suggest using patches for four weeks for those who experience pain after their shingles rash disappears. However, if there is still pain after these four weeks, it is recommended to see a pain specialist. (Gross, G. E. et al., 2020) Side Effects Common side effects are typically mild skin reactions where the patch is. These reactions are usually temporary and will disappear within a few minutes or hours. Examples include: (Food and Drug Administration, 2022) - Irritation
- Itchiness
- Abnormal or burning sensation
- Redness
- Swelling
- Blisters
- Bruises
- Skin bumps
- Skin color changes
- Skin peeling
Potentially serious side effects include: (Food and Drug Administration, 2022) Serious Allergic Reaction - Severe allergic reactions are rare, but it is possible.
- Symptoms include breathing problems, itchiness, and rash.
Methemoglobinemia - Methemoglobinemia is a condition that makes it hard for red blood cells to carry oxygen.
- Individuals may experience symptoms of blue-looking skin, headache, lightheadedness, shortness of breath, abnormal heart rhythm, or seizures.
Using too many lidocaine patches to cover large parts of the body or using the patches longer than 12 hours within 24 hours may cause side effects that may include heart-related effects, such as a slow heart rate and low blood pressure. Individuals may also experience the following side effects (Food and Drug Administration, 2022) - Hot or cold sensation
- Numbness
- Dizziness
- Ringing ears
- Lightheadedness
- Mood changes
- Drowsiness to unconsciousness
- Vision changes
- Seizures
- Tremors
- Vomiting
Injury Medical Chiropractic & Functional Medicine Clinic Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop an optimal health and wellness solution. We focus on what works for you to relieve pain, restore function, and prevent injury. Regarding musculoskeletal pain, specialists like chiropractors, acupuncturists, and massage therapists can help mitigate the pain through spinal adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal issues. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies that are available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References National Library of Medicine. MedlinePlus. (2025). Lidocaine transdermal patch. Retrieved from https://medlineplus.gov/druginfo/meds/a603026.html Food and Drug Administration. (2022). Lidoderm label. Retrieved from https://www.accessdata.fda.gov/spl/data/eedfe43b-1019-19a0-e053-2995a90a7696/eedfe43b-1019-19a0-e053-2995a90a7696.xml Department of Veterans Affairs/Department of Defense. (2022). VA/DoD clinical practice guideline for the diagnosis and treatment of low back pain. Retrieved from https://www.healthquality.va.gov/guidelines/Pain/lbp/VADoDLBPCPGFinal508.pdf North American Spine Society. (2020). Evidence-based clinical guidelines for multidisciplinary spine care: diagnosis and treatment of low back pain. https://www.spine.org/Portals/0/assets/downloads/ResearchClinicalCare/Guidelines/LowBackPain.pdf National Library of Medicine. DailyMed. (2018). Label: lidocaine patch. Retrieved from https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=5c66f3b9-6e04-47ab-8d94-21e89ceec154 Food and Drug Administration. (2021). Ztlido label. Retrieved from https://www.ztlido.com/wp-content/uploads/2022/12/ZTlido-LABEL.pdf National Library of Medicine. DailyMed. (2025). Lidocaine-lidocaine hydrochloride injection, solution. Retrieved from https://dailymed.nlm.nih.gov/dailymed/lookup.cfm?setid=f1b26274-a55e-4321-b96c-ce0df830f205 Santana, J. A., Klass, S., & Felix, E. R. (2020). The Efficacy, Effectiveness and Safety of 5% Transdermal Lidocaine Patch for Chronic Low Back Pain: A Narrative Review. PM & R: the journal of injury, function, and rehabilitation, 12(12), 1260–1267. https://doi.org/10.1002/pmrj.12366 Rowbotham, M. C., Davies, P. S., Verkempinck, C., & Galer, B. S. (1996). Lidocaine patch: double-blind controlled study of a new treatment method for post-herpetic neuralgia. Pain, 65(1), 39–44. https://doi.org/10.1016/0304-3959(95)00146-8 Gross, G. E., Eisert, L., Doerr, H. W., Fickenscher, H., Knuf, M., Maier, P., Maschke, M., Müller, R., Pleyer, U., Schäfer, M., Sunderkötter, C., Werner, R. N., Wutzler, P., & Nast, A. (2020). S2k guidelines for the diagnosis and treatment of herpes zoster and postherpetic neuralgia. Journal der Deutschen Dermatologischen Gesellschaft = Journal of the German Society of Dermatology: JDDG, 18(1), 55–78. https://doi.org/10.1111/ddg.14013
Cauda equina syndrome/CES is a rare condition in which the nerves in the lower back are compressed. It can include sciatica as one of its symptoms. Individuals presenting with symptoms that could be CES are advised to see a healthcare provider as soon as possible, as delaying treatment can lead to permanent damage. Cauda Equina Syndrome A cluster of nerve roots called the cauda equina, Latin for horse's tail, sends and receives messages to the legs, bladder, and other body parts. Cauda equina syndrome is a rare condition in which nerve roots in the lower spinal cord are compressed. This compresses the nerves and disrupts motor and sensory function in the bladder and lower extremities. The most common cause is a ruptured or herniated disc in the lumbar area. This usually occurs when a severe disc herniation compresses the nerve bundle at the base of the spinal cord, causing significant neurological dysfunction like bladder/bowel issues and numbness in the saddle area. If found early, it is treated with surgery within 24 to 48 hours of symptom onset. Initial Signs Symptoms can occur acutely, in hours, or gradually over weeks or months. One of the first signs and most common symptoms is urinary retention, where the bladder fills, but there is no normal sensation or urge to urinate. (American Association of Neurological Surgeons, 2024) Other symptoms include: (Gardner A., Gardner E., & Morley T. 2011) - Severe low back pain
- Sciatica
- Pain, numbness, or weakness in one or both legs
- Saddle anesthesia, which is numbness or other nerve sensations around the anus and the area that sits.
- A loss of reflexes in the extremities
- Sexual dysfunction that comes suddenly
- Loss of bowel control
- Overflow urination
There are two stages based on urinary symptoms (Fairbank J., & Mallen C. 2014) CES-Incomplete CES-I CES-Retention CES-R - Bladder control is completely lost.
Causes The most common cause is a ruptured or herniated disc in the lumbar area. Other possible causes may include: (American Association of Neurological Surgeons, 2024) Trauma or injury to the spine - that leads to fractures or dislocations (gunshots, falls, auto accidents)
Tumors or Infections - It can compress the cauda equina nerve bundle.
Spinal Stenosis - Narrowing of the spinal column can be either congenital or acquired.
Bone Spurs Tuberculosis or Pott's Paralysis Iatrogenic Side Effects - Injuries or illnesses that result from medical or surgical treatment
Spinal Lesions or Malignant Tumors - A spinal lesion refers to any abnormal growth or damage within the spine.
- It can include benign (noncancerous) and malignant (cancerous) tumors.
- A malignant tumor is a cancerous growth within the spine; essentially, a malignant tumor is a type of spinal lesion with the potential to spread to other parts of the body.
Spinal Infection, Inflammation, Hemorrhage, or Fracture Spinal Arteriovenous Malformations (AVMs) - A spinal arteriovenous malformation (AVM) is a rare condition in which the arteries and veins in the spinal cord tangle abnormally.
- This can damage the spinal cord over time.
Complications from Lumbar Surgery - Lumbar surgery can have several complications, including infections, blood clots, nerve damage, and spinal fluid leaks.
Spinal Anesthesia - Spinal anesthesia is a regional anesthesia that blocks pain and sensation in the lower body.
- It involves injecting a local anesthetic medication into the subarachnoid space surrounding the spinal cord.
- The exact cause is not fully understood, but it can involve direct nerve root injury from the needle, inflammation caused by the anesthetic, or a spinal hematoma compressing the nerve roots.
Spinal Birth Defects Diagnosis Diagnosis requires a medical history of symptoms, general health, activity level, and a physical exam to assess strength, reflexes, sensation, stability, alignment, and motion. (American Association of Neurological Surgeons, 2024) Testing includes: Blood Tests - These test for infections.
MRI - These yield three-dimensional images of the spinal cord, nerve roots, and surrounding areas.
Myelography - X-ray or computerized tomography (CT) imaging is enhanced by injecting contrast material into the cerebrospinal fluid spaces, which can show spinal cord displacement or spinal nerves.
Specialized Nerve Testing - This could be nerve conduction velocity tests and testing electrical activity in muscles or electromyography.
Treatment The extent of urinary problems can determine treatment protocols. A CES diagnosis is usually followed by emergency surgery within 24 to 48 hours to relieve compression of the nerves. Moving quickly is essential to prevent permanent complications such as nerve damage, incontinence, or leg paralysis. (American Association of Neurological Surgeons, 2024) - Depending on the cause, corticosteroids also may be prescribed to reduce swelling.
- Antibiotics may be needed if an infection is responsible for CES.
- For situations in which a tumor is the cause, surgery to remove it may be necessary, followed by chemotherapy and/or radiation.
- The outcome with CES-I during surgery is generally favorable.
- Those whose CES has deteriorated to CES-R tend to have a less favorable prognosis.
Post Surgery Therapy After surgery, CES can be challenging to deal with. If bladder function has been impaired, recovery of control can take time. - It may be necessary to use a catheter or to wear disposable underwear. (American Association of Neurological Surgeons, 2024)
- Frequent urinary infections are also a potential complication.
- Loss of bladder or bowel control can be psychologically distressing, impacting social life, work, and relationships.
- Sexual dysfunction can also occur, contributing to relationship difficulties or depression.
Therapy with a mental health professional may be recommended. When damage is permanent, it will be important to include family and friends in the adjustment to living with a chronic condition. Psychological counseling and/or a support group can be helpful. Other specialists who can help include: (American Academy of Orthopaedic Surgeons, 2024) - Occupational therapist
- Physical therapist
- Physiotherapist
- Sex therapist
- Social worker
Injury Medical Chiropractic and Functional Medicine Clinic Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to build optimal health and wellness solutions. We focus on what works for you to relieve pain, restore function, prevent injury, and mitigate issues through adjustments that help the body realign itself. The clinic can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal problems. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies that are available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References American Association of Neurological Surgeons. (2024). Cauda Equina Syndrome. https://www.aans.org/patients/conditions-treatments/cauda-equina-syndrome/ Gardner, A., Gardner, E., & Morley, T. (2011). Cauda equina syndrome: a review of the current clinical and medico-legal position. European Spine Journal: official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society, 20(5), 690–697. https://doi.org/10.1007/s00586-010-1668-3 Fairbank, J., & Mallen, C. (2014). Cauda equina syndrome: implications for primary care. The British journal of general practice: the journal of the Royal College of General Practitioners, 64(619), 67–68. https://doi.org/10.3399/bjgp14X676988 American Academy of Orthopaedic Surgeons. (2024). Cauda equina syndrome. https://orthoinfo.aaos.org/en/diseases--conditions/cauda-equina-syndrome
For individuals who injure their neck or back, the muscles may spasm or seize up, making it difficult to get through the day, exercises, physical activities, etc. Can skeletal muscle relaxers help relieve pain and reduce frequency? Back Spasms Muscle Relaxers Back muscle spasms are common back pain that feels like a sudden tightness or contraction in the back muscles. They can range from minor twinges to severe pain. Causes - Poor posture: Sitting or standing with bad posture can strain the back muscles.
- Overuse: Picking something up, bending, or lifting can cause a spasm.
- Dehydration: Not drinking enough water can cause electrolyte imbalances, leading to spasms.
- Underlying conditions: A herniated disc or degenerative disc disease can cause back spasms.
- Muscle imbalances: Weak muscles or muscles that are too tight can cause spasms.
Treatments - Home treatments: Apply heat or ice, take over-the-counter pain medication, try gentle stretching, or massage the area.
- Exercise: Improve your back's strength and flexibility with exercise or physical therapy.
- Hydration and nutrition: Drink enough water and eat foods rich in magnesium and calcium.
- Chiropractic Adjustments: These can realign the spine to the correct position and muscles to relax.
- Non-surgical Decompression: Decompression of the spine will allow more blood and nutrients to heal painful areas.
Skeletal Muscle Relaxers A healthcare provider may prescribe skeletal muscle relaxers. These medications are not available over the counter and must be prescribed by a healthcare provider. - Skeletal muscle relaxers will probably cause drowsiness.
- Individuals should not drive, operate heavy machinery, or engage in other physical activities when taking back spasm muscle relaxers.
- Skeletal muscle relaxers are not recommended for 65 or older because safer, effective alternatives exist.
- Also, women who are pregnant or breastfeeding should not take these medications.
- Discuss these issues with your healthcare provider.
Carisoprodol Carisoprodol is available generically and as Soma and Vanadom brands. It works by suppressing nerve impulses located in the brain and spinal cord. Healthcare providers prescribe this medication in combination with physical therapy for the healing release of any muscle spasm and management of musculoskeletal injuries and/or pain. (Witenko C. et al., 2014) It's not about having to continue taking the medication to feel better but more as a jump start to help with the physical therapy program. - Back muscle spasms are a perfect example of a condition that may benefit from carisoprodol in the short term.
- Carisoprodol can be habit-forming.
- Be sure to talk to a healthcare provider before suddenly going off this medication.
- Carisoprodol can cause side effects that may impair thinking or reactions.
- Avoid drinking alcohol as it may increase drowsiness and dizziness that are often caused by carisoprodol. (Zacny J. P., Paice J. A., & Coalson D. W. 2012)
- Inform your healthcare provider of any drug allergies, kidney disease, or liver disease, or if you get seizures.
Cyclobenzaprine Cyclobenzaprine is available as Amrix and in generic form. Like other muscle relaxers, cyclobenzaprine may cause dizziness or drowsiness. The sedation effects are how it works on painful, tension-filled muscles. Cyclobenzaprine is used together with physical therapy to treat skeletal muscle-related conditions and/or injuries, especially when pain or spasm is involved. When used in conjunction with physical therapy, it can help expedite recovery. - Cyclobenzaprine is chemically related to tricyclic antidepressants.
- Although it is considered a derivative of the tricyclic antidepressant class, it does not pose the same risk to liver health.
- According to the National Institutes of Health, reasons not to take this medication include having a thyroid disorder, heart block, congestive heart failure, a heart rhythm disorder, or having recently had a heart attack. (Witenko C. et al., 2014)
Metaxalone Skelaxin is the brand name for metaxalone. As with the other muscle relaxers, metaxalone is used in combination with physical therapy and rest when muscles get too tight. (Witenko C. et al., 2014) It works by suppressing nerve impulses in the brain and spinal cord. In addition to older individuals and pregnant women, metaxalone is usually not prescribed for those with kidney disease, liver disease, seizures, or blood disorders. Injury Medical Chiropractic and Functional Medicine Clinic Back spasms, muscle relaxers, and a personalized physical therapy treatment program could help individuals. Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to build optimal health and wellness solutions. We focus on what works for you to relieve pain, restore function, prevent injury, and help mitigate issues through adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal problems. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Witenko, C., Moorman-Li, R., Motycka, C., Duane, K., Hincapie-Castillo, J., Leonard, P., & Valaer, C. (2014). Considerations for the appropriate use of skeletal muscle relaxants for the management of acute low back pain. P & T: a peer-reviewed journal for formulary management, 39(6), 427–435. Zacny, J. P., Paice, J. A., & Coalson, D. W. (2012). Subjective and psychomotor effects of carisoprodol in combination with oxycodone in healthy volunteers. Drug and alcohol dependence, 120(1-3), 229–232. https://doi.org/10.1016/j.drugalcdep.2011.07.006
Sleeping with lower back pain and sciatica can be difficult and frustrating. What are ways to get more comfortable sleep? Sleeping With Lower Back Pain and Sciatica Various factors can affect sleeping with lower back pain and sciatica, including age, injury and medical history, the mattress (e.g., soft vs. firm mattress), and sleep positions. Unfortunately, there's no one-cure-all solution for this problem, and depending on the underlying cause/s, they can worsen the pain and cause sleep problems. For example, if a herniated disc places added pressure on the nerves in the lower back, twisting the spine can worsen the lower back pain, and sleeping in a fetal position can exacerbate the nerve pain. (UCF Health, N.D.) Lower-Back Pain Low-back pain can be activity-related, intermittent, or constant. (American Association of Neurological Surgeons, 2024) For some, it only occurs occasionally, such as when performing specific movements. For others, it can be excruciating, chronic, and disabling. Low-back pain is unique for everybody and can differ depending on the cause. Some low-back pain symptom descriptions include (Förster M. et al., 2013) - Aching pain deep in the back
- Shooting pain flare-ups
- Pain caused by slight pressure
- Burning
- Tingling
Sciatica Not Present For some, low-back pain may be confined to a specific area known as axial back pain. (Förster M. et al., 2013) The pain may be felt in a band along the lower back and does not radiate down the legs or anywhere else. Sciatica Present Low-back pain with sciatica pain that radiates from the lower back or hip down the leg is the most common symptom of lumbar radiculopathy (compression of spinal nerve roots). (North American Spine Society, 2020) Sciatica symptoms include:(American Academy of Orthopaedic Surgeons, 2021) - Shooting pain from the lower back down the leg
- Feeling like a bad leg cramp
- Leg weakness
- Sensory changes radiating down the leg - numbness, burning, and or tingling
Sleep Tools Consider changing the mattress to improve sleeping with lower back pain and sciatica. For the best spinal support, choose a medium to firm mattress. Pillows, wedges, and other tools can also help improve sleep. (UCF Health, N.D.) It is recommended that individuals who sleep on their backs place a small pillow under their knees to reduce pressure on their lower backs. For those who sleep on their side, placing a pillow between the knees can keep the spine in a neutral/straight position. To relieve lower back pain, consider sleeping in a reclined, angled position with the head and shoulders higher than the hips. This can be accomplished with an adjustable bed or a wedge to prop the body in a regular bed. Back Sleeping Easing back pain while sleeping involves maintaining the body in a neutral or straight position. Extending the muscles, tendons, and ligaments too far in any one direction while sleeping with lower back pain and sciatica can cause stiffness, muscle spasms, and pain. Sleeping on the back puts the spine in neutral alignment with the least stress on the neck and back. It evenly distributes body weight to avoid exerting pressure on the joints and prevent backaches. In addition, a supine position allows outstretched ligaments to shrink and recover to their normal positions. (Keck Medicine of USC, 2019) Chiropractic Assessment Chiropractic care aims to help individuals improve movement with less pain due to condition, after injury, or surgery. A chiropractic physical therapy team may be best for individuals with acute back, neck, and musculoskeletal pain and discomfort symptoms. A chiropractor can quickly assess your condition and develop a customized treatment plan to expedite pain relief and improve mobility. Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to build optimal health and wellness solutions. We focus on what works for you to relieve pain, restore function, prevent injury, and help mitigate issues through adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal problems. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References UCF Health. (N.D.). The best sleeping position for lower back pain (and the worst). https://ucfhealth.com/our-services/lifestyle-medicine/best-sleeping-position-for-lower-back-pain/ American Association of Neurological Surgeons. (2024). Low back pain. https://www.aans.org/patients/conditions-treatments/low-back-pain/ Förster, M., Mahn, F., Gockel, U., Brosz, M., Freynhagen, R., Tölle, T. R., & Baron, R. (2013). Axial low back pain: one painful area--many perceptions and mechanisms. PloS one, 8(7), e68273. https://doi.org/10.1371/journal.pone.0068273 North American Spine Society. (2020). Evidence-based clinical guidelines for multidisciplinary spine care: Diagnosis and treatment of low back pain. North American Spine Society. https://www.spine.org/Portals/0/assets/downloads/ResearchClinicalCare/Guidelines/LowBackPain.pdf American Academy of Orthopaedic Surgeons. (2021). Sciatica. https://orthoinfo.aaos.org/en/diseases--conditions/sciatica Keck Medicine of USC. (2019). The best -and worst - sleep positions for back pain. Keck Medicine of USC Blog. https://www.keckmedicine.org/blog/the-best-and-worst-sleep-positions-for-back-pain/
The iliacus muscle is a triangle-shaped muscle in the pelvic bone that flexes and rotates the thigh bone. It works with the other muscles in the hip and thigh to help bend, run, walk, sit, and maintain correct posture. Injuries and common medical conditions can affect its function, causing pain and stiffness. Can physical therapy help? The Iliacus Muscle The iliacus is one of the body's most important hip flexor muscles. The iliacus and surrounding muscles work together to produce the stability and range of motion required for bending, dancing, sitting, and walking. Anatomy The iliacus muscle is part of a complex muscle system in the hip and pelvis. Two iliacus muscles on each side of the pelvic bone enable the thigh to flex and rotate. They are innervated by the femoral nerve, which provides movement and sensation to the lower limbs. (Bordoni B. and Varacallo M. 2023) The iliacus muscle sits on the wing-shaped ilium and fits into the curved surface of the ilium, called the iliac fossa. The top of the muscle is attached to the upper wings of the ilium or iliac crest. It extends past the hip joint, which connects to the upper thigh bone/femur at the lesser trochanter protrusion. The iliacus is part of a major trio of muscles called the iliopsoas, including the major psoas and minor psoas muscles. These muscles are also attached to the upper femur but extend upward, connecting to the lumbar/lower spine at several attachment points. The iliopsoas also interact with the quadratus lumborum muscle, the deepest muscle of the lower back that starts at the iliac crest and attaches to the lumbar spine at several points. The quadratus lumborum enables flexion and elevation of the spine, while the iliopsoas enable the flexion and rotation of the hip and thigh. Functions The iliacus muscle has many functions that include: (Physiopedia, 2024) - Flexing and rotating the femur.
- Helps maintain proper body posture while standing and sitting.
- Produces hip movement that enables walking, running, and climbing stairs.
- Provides hip flexion - bringing the knee to the chest.
- Enables the forward tilt of the pelvis and side-bending.
Conditions Several conditions can affect the iliacus muscle, specifically from under and/or overuse injuries. These conditions, collectively known as Iliopsoas syndrome, are typically the result of overuse/repetitive strain or injuries. These include: - Iliopsoas tendinopathy - which affects tendons.
- Iliopsoas bursitis - which affects cushioning sacs known as bursae.
Iliopsoas syndrome can affect anyone but is common in: - Individuals and athletes who repeatedly use movements that flex the hips.
- Track-and-field athletes
- Gymnasts
- Dancers
Iliopsoas Bursitis This is the inflammation of the cushioning sac or bursa under the iliacus muscle, which helps the muscle slide over the pelvic bone. Symptoms can range from mild discomfort to pain that radiates through parts of the leg and hips. Runners, skiers, and swimmers are commonly affected, and individuals who regularly have tight hips and individuals with different forms of arthritis can also be affected. Early treatment can prevent the symptoms from worsening. Mild cases can be treated with self-care and stretching to help relieve tightness, rest, ice application, and over-the-counter nonsteroidal anti-inflammatory drugs. In severe cases, treatment options that may be recommended include: (Physiopedia, 2024) - Physical therapy
- Assistant walking devices to relieve pressure - for example, a cane.
- Corticosteroid steroid injections
- Prescription anti-inflammatory medications
Iliopsoas Tendinopathy Another condition affecting the iliacus muscles is iliopsoas tendinopathy, sometimes called snapping hip syndrome, because individuals can hear an audible snapping sound (Davenport KL. 2019). The condition is often experienced by dancers who repeatedly flex and hyperextend their hips and can result in hip and groin pain that gets worse with kicking or rotation. Treatment of iliopsoas tendinopathy can include: - Retraining muscle imbalances with strengthening and stretching exercises.
- If these fail to provide relief, corticosteroid injections may be used. A saline hydro dissection can relieve stress around the tendon by injecting fluids that cushion and release trapped tissues.
- Tendon release surgery may be recommended when all other options have failed. The surgical release involves severing the tendon to reduce pain and improve the range of motion.
Rehabilitation Core muscle strengthening is essential to the rehabilitation of iliacus muscle injuries. The iliopsoas is an integral component of the core group and can benefit from stretching and strengthening exercises (Yogateket, 2019) - Lunge stretches
- Straight leg raises
- Knee-to-chest stretches
- Standing hip flexion with resistance bands
- Certain yoga poses can also help and include variations on the bridge pose that encourage hip flexion. (Yoga International, 2024)
Injury Medical Chiropractic and Functional Medicine Clinic Iliopsoas pain is often felt at the front of the hips, thigh, mid-back, and lower back. Chiropractic care can help with iliacus muscle injuries through: Evaluation - A chiropractor can evaluate the condition and determine if the iliacus muscle is causing pain.
Treatment plan - A chiropractor can create a personalized treatment plan that may include exercise instructions, manipulation, and other therapies.
Rehabilitation - A chiropractor can create a rehabilitation program to expedite healing.
Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop an optimal health and wellness solution. We focus on what works for you to relieve pain, restore function, and prevent injury. Regarding musculoskeletal pain, specialists like chiropractors, acupuncturists, and massage therapists can help mitigate the pain through spinal adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal issues. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies that are available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Bordoni, B., & Varacallo, M. (2024). Anatomy, Bony Pelvis, and Lower Limb, Iliopsoas Muscle. In StatPearls. https://www.ncbi.nlm.nih.gov/pubmed/30285403 Physiopedia. (2024). Iliacus. https://www.physio-pedia.com/Iliacus Physiopedia. (2024). Iliopsoas bursitis. https://www.physio-pedia.com/Iliopsoas_Bursitis Davenport KL. (2019). The professional dancer’s hip. Performing Arts Medicine, 77-87. https://doi.org/https://doi.org/10.1016/B978-0-323-58182-0.00009-2 Yogateket. Lizette Pompa. (2019). Essential yoga body parts. Hip flexor/psoas and yoga. Yogateket. https://www.yogateket.com/blog/hip-flexor-psoas-and-yoga Yoga International. Amber Burke. (2024). 8 poses for iliopsoas release. https://yogainternational.com/article/view/8-poses-for-iliopsoas-release/
|
Many people think sciatica must include low back pain. But sciatica can show up in a different way—like numbness in the hamstring, calf, or foot—even when the low back feels “fine.” This can be confusing and, honestly, a little scary. Here’s the simple idea: -
Sciatica is not one disease. -
Sciatica is a pattern of symptoms caused by irritation or compression of nerve tissue that eventually feeds into the sciatic nerve. -
That irritation can happen in the low back, pelvis, hip/buttock region, or even farther down the leg, so symptoms may not always start with back pain. (Penn Medicine, n.d.; Yale Medicine, n.d.; HSS, 2024) This article explains why numbness can show up in the hamstring and foot, how to tell it apart from a hamstring strain, what “red flags” matter, and how integrative chiropractic care (with medical evaluation when needed) can help you recover safely. What Sciatica Can Feel Like When the Back Doesn’t Hurt Sciatica is often described as pain that travels from the buttocks down the leg, but it can also feel like: -
Numbness in the hamstring, calf, heel, or toes -
Tingling (“pins and needles”) -
Burning or electric sensations -
A foot that feels “asleep,” heavy, or clumsy -
Weakness (in more serious cases) (HSS, 2024; Mayo Clinic, 2025; Yale Medicine, n.d.) Some people feel mostly numbness and tingling, with very little pain. That can still be a nerve problem and deserves attention—especially if it lasts or worsens. (Mayo Clinic, 2025; Penn Medicine, n.d.) Why You Can Have Hamstring and Foot Numbness Without Low Back Pain The nerve can be irritated “upstream,” but you feel it “downstream” Nerves are like electrical cables. If the cable is irritated near the spine, you might feel symptoms farther down the line, such as the hamstring or the foot. This is why sciatica can feel like a leg problem even when the back does not hurt. (Mayo Clinic, 2025; Penn Medicine, n.d.) The irritation may be in the buttock/hip area, not the spine A well-known example is piriformis syndrome, where a deep buttock muscle can irritate or compress the sciatic nerve. This may cause leg numbness, tingling, or pain—sometimes with little or no back pain. (Total Ortho Sports Med, 2025; Jimenez, n.d.-a) Dr. Alexander Jimenez, DC, APRN, FNP-BC, often emphasizes that the biomechanics of the pelvis, sacroiliac region, and hip rotators can contribute to sciatic-type symptoms, especially when movement patterns and soft-tissue tension repeatedly stress the nerve. (Jimenez, n.d.-a) The nerve can be irritated near the hamstring itself Sometimes symptoms that feel like sciatica may relate to hamstring syndrome, where the sciatic nerve is irritated near its origin at the sit bone area. This can create buttock/back-of-thigh pain and may include tingling or numbness down the leg. (Jimenez, 2025) Spinal causes can still exist even if the back doesn’t hurt Even without back pain, symptoms can still come from spinal issues such as: -
Disc bulge or herniation -
Spinal stenosis (narrowing around nerves) -
Other causes that irritate nerve roots (HSS, 2024; Penn Medicine, n.d.) And yes, one part of the leg can hurt while another part feels numb, depending on which nerve fibers are irritated. (Mayo Clinic, 2025) Common Questions People Ask When Sciatica Feels Like Hamstring + Foot Numbness “Is this sciatica or a hamstring strain?” This is one of the most important questions because treatment choices can differ. Hamstring strain is usually a muscle/tendon injury. It often comes with a clear moment of injury (sprint, slip, deadlift, kick), plus local tenderness and pain with hamstring stretching or contraction. Sciatica-type nerve symptoms are more likely when you notice: -
Tingling, burning, or numbness -
Symptoms traveling below the knee into the foot -
Symptoms worsen with long sitting, coughing/sneezing, or certain spine/hip positions (Ducker Physio, 2025; HSS, 2024) A simple comparison: -
More like hamstring strain: localized back-of-thigh pain, pulling sensation, pain with hamstring stretch, bruising/tenderness after activity (Ducker Physio, 2025) -
More like nerve irritation: numbness/tingling, “electric” sensations, symptoms in the calf/foot, symptoms that change with posture or prolonged sitting (HSS, 2024; Mayo Clinic, 2025) “Why would my foot be numb if my hamstring is the problem?” Because numbness is usually a nerve signal issue, not a muscle issue. A strained muscle can hurt a lot, but it typically does not cause true pins-and-needles or foot numbness unless something else is affecting nerve tissue. (Ducker Physio, 2025; HSS, 2024) “Can sciatica happen with no back pain at all?” Yes. It can happen when the nerve is irritated in the buttock/hip region (piriformis-related irritation) or when nerve root symptoms are mostly in the leg. (Total Ortho Sports Med, 2025; Mayo Clinic, 2025) Why “Numbness” Matters More Than People Think Pain gets attention fast. Numbness can be quieter, but it can be a bigger warning sign—especially if it’s worsening or paired with weakness. The American Medical Association notes that numbness or weakness in the legs (and bowel/bladder changes) should be evaluated, as these may be signs of something more serious. Red Flags: When You Should Seek Care Quickly If you have hamstring/foot numbness, don’t panic—but do take these seriously. Seek urgent evaluation if you have: -
New or worsening leg weakness -
Trouble lifting the foot (foot drop) or frequent tripping -
Loss of bowel or bladder control -
Numbness in the “saddle area” (inner thighs/groin region) -
Severe symptoms that rapidly escalate Even without emergency signs, it’s smart to get checked if: -
Numbness lasts more than 1–2 weeks -
Symptoms keep returning -
Symptoms spread farther down the leg -
You can’t train, work, or sleep normally (Penn Medicine, n.d.; HSS, 2024) How Clinicians Typically Figure Out What’s Going On A good evaluation usually includes: -
A symptom history: where it starts, where it travels, what triggers it -
Neuro checks: sensation, strength, reflexes -
Motion testing: spine + hip movement -
Special tests (like nerve tension tests) -
Imaging if needed (especially if symptoms persist, worsen, or show red flags) (HSS, 2024; Penn Medicine, n.d.) A key point from the clinical literature: musculoskeletal problems can mimic radiculopathy, so careful testing is essential. Integrative Chiropractic Care for Hamstring/Foot Numbness: What It Tries To Fix When integrative chiropractic care is appropriate, the goal is not to “chase symptoms.” The goal is to address likely drivers: -
Nerve irritation (spinal or peripheral) -
Joint mechanics (lumbar spine, pelvis, SI region, hip) -
Soft tissue tension (piriformis, glutes, hamstrings) -
Movement patterns that keep re-irritating the nerve Dr. Alexander Jimenez often emphasizes that sciatic-type symptoms can be influenced by biomechanical dysfunction in the low back and pelvis, and that combining joint care with soft-tissue work and functional correction can help restore normal movement and reduce nerve stress. (Jimenez, n.d.-a) Common integrative components may include: Spinal and pelvic adjustments (when appropriate) -
Aimed at improving joint motion and reducing mechanical stress that may contribute to nerve irritation -
Often paired with exercise and education (Auburn Hills Chiropractic, n.d.; Jimenez, n.d.-b) Soft-tissue therapies These may target areas that commonly irritate the sciatic nerve pathway: -
Piriformis and deep hip rotators -
Glutes and lateral hip -
Hamstrings (especially near the upper attachment) -
Thoracolumbar fascia and related tissues (Total Ortho Sports Med, 2025; Jimenez, 2025) Corrective exercises and movement retraining This is the “keep it from coming back” part. Often includes: -
Hip mobility drills -
Glute activation and endurance work -
Core stability and trunk control -
Gradual nerve “glide” or mobility strategies (as directed) -
Return-to-sport progressions (HSS, 2024; Jimenez, n.d.-a) Co-management with medical care when needed Sciatica is commonly treated first with conservative care, and many cases improve over time. (AMA, 2024; IASP, n.d.)
But persistent numbness, weakness, or severe symptoms may need medical diagnostics and a broader plan. (Penn Medicine, n.d.; Mayo Clinic, 2025) Clinical practice guidelines often support combinations like: Practical Self-Check Tips (Not a Diagnosis) These are not perfect, but they can guide your next step. Signs it may be nerve-related: -
Numbness/tingling that travels below the knee -
Symptoms change with posture (long sitting, bending, coughing/sneezing) -
Symptoms feel electric, burning, or “deep” rather than sore/tight (HSS, 2024; Mayo Clinic, 2025) Signs it may be more muscle/tendon-related: -
Pain stays mostly in the back of the thigh -
Clear injury moment -
Pain increases with hamstring stretch or contraction -
Tenderness along the hamstring muscle belly or tendon (Ducker Physio, 2025) When in doubt, get evaluated—because the best plan depends on the true source. What Recovery Often Looks Like (A Realistic Timeline) Many sciatica cases improve over weeks to a few months, especially with a conservative plan and good movement habits. A practical, safe progression often looks like: -
Phase 1 (calm it down): reduce triggers, restore gentle motion, improve sleep positioning, light walking -
Phase 2 (restore movement): mobility + stability, targeted soft tissue work, controlled strengthening -
Phase 3 (build resilience): strength endurance, sport/work conditioning, long-term prevention habits If numbness worsens or strength declines, that’s a sign to re-evaluate the plan and consider more advanced diagnostics. (AMA, 2024; Penn Medicine, n.d.) Key Takeaways -
Sciatica can present as hamstring and foot numbness, even without back pain. (Mayo Clinic, 2025; Total Ortho Sports Med, 2025) -
Causes can include piriformis/hip-region compression, spinal nerve root irritation, or hamstring-area nerve irritation. (HSS, 2024; Jimenez, 2025; Penn Medicine, n.d.) -
Numbness and weakness matter—especially if worsening or paired with red flags. -
Integrative chiropractic care often combines manual care, soft tissue work, and corrective exercise, and may coordinate with medical evaluation when needed. (Zaina et al., 2023; Jimenez, n.d.-a) References American Medical Association. (2024, November 15). What doctors wish patients knew about sciatica. https://www.ama-assn.org/public-health/prevention-wellness/what-doctors-wish-patients-knew-about-sciatica Auburn Hills Chiropractic and Rehabilitation. (n.d.). How chiropractic adjustments can treat sciatica. https://auburnhillschiro.com/how-chiropractic-adjustments-can-treat-sciatica/ Bateman, E. A., et al. (2024). Musculoskeletal mimics of lumbosacral radiculopathy. PM&R. https://pmc.ncbi.nlm.nih.gov/articles/PMC11998970/ Ducker Physio. (2025, April 8). Tell the difference between sciatica & hamstring pain. https://www.duckerphysio.com.au/blog/difference-sciatica-and-hamstring-pain Hospital for Special Surgery. (2024, May 24). Sciatica: Simple symptoms, complex causes. https://www.hss.edu/health-library/conditions-and-treatments/list/sciatica International Association for the Study of Pain. (n.d.). Surgical or non-surgical management for sciatica. https://www.iasp-pain.org/publications/relief-news/article/management-for-sciatica/ Jimenez, A. (n.d.-a). Sciatica vs piriformis syndrome explained. https://dralexjimenez.com/sciatica-el-paso-chiropractor/sciatica-vs-piriformis-syndrome-explained/ Jimenez, A. (n.d.-b). Sciatica nerve pain treatment (El Paso, TX). https://dralexjimenez.com/sciatica-el-paso-chiropractor/ Jimenez, A. (2025). Hamstring syndrome relief and muscle recovery. https://dralexjimenez.com/hamstring-syndrome-relief-and-muscle-recovery/ Mayo Clinic. (2025, December 23). Sciatica: Symptoms and causes. https://www.mayoclinic.org/diseases-conditions/sciatica/symptoms-causes/syc-20377435 Penn Medicine. (n.d.). Sciatica. https://www.pennmedicine.org/conditions/sciatica Total Ortho Sports Med. (2025, December 5). Sciatica with no back pain: Why does my sciatica appear even when I have no back pain? https://www.totalorthosportsmed.com/sciatica-with-no-back-pain/ Yale Medicine. (n.d.). Sciatica. https://www.yalemedicine.org/conditions/sciatica Zaina, F., et al. (2023). A systematic review of clinical practice guidelines for low back pain with and without radiculopathy. Archives of Physical Medicine and Rehabilitation. https://pubmed.ncbi.nlm.nih.gov/36963709/ The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and to identify relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Sciatica pain can make even simple tasks—like getting out of bed, sitting at your desk, or driving to a clinic—feel overwhelming. When your leg burns, tingles, or feels weak, the idea of sitting in a car and waiting in a lobby may sound impossible. Telemedicine offers a different way. With a phone, tablet, or computer, you can talk with a spine specialist, nurse practitioner, or chiropractor from home. Together, you can build a plan to calm the sciatic nerve, improve your movement, and prevent the pain from worsening (UT Southwestern Medical Center, 2025; Spine Institute of Southeast Texas, n.d.). UT Southwestern Medical Center+1 This article explains, in clear language: -
What sciatica is -
How telemedicine works for back and leg pain -
How virtual visits help diagnose and manage sciatica -
The role of integrative chiropractic telemedicine -
How to prepare for a telemedicine visit -
When in-person care is still needed We’ll also include clinical observations from Dr. Alexander Jimenez, DC, APRN, FNP-BC, who uses an integrated chiropractic and nurse practitioner approach for sciatica and spine-related conditions in his practice. El Paso, TX Doctor Of Chiropractic What Is Sciatica? Sciatica is not a disease by itself. It is a group of symptoms caused by irritation or compression of the sciatic nerve. This large nerve runs from your lower back, through your hips and buttocks, and down the back of each leg. Common causes include: -
Herniated or bulging discs -
Spinal stenosis (narrowing of the spinal canal) -
Degenerative disc disease -
Muscle tightness in the lower back or gluteal region -
Joint dysfunction in the lumbar spine or sacroiliac joints (HealthCentral, n.d.; Evolve Chiropractic, n.d.) HealthCentral+1 Common symptoms: -
Sharp, burning, or electric pain running from the lower back into the buttocks and down the leg -
Tingling, numbness, or “pins and needles” in the leg or foot -
Muscle weakness, especially when lifting the foot or standing from a chair -
Pain that worsens with sitting, bending, twisting, or coughing For many people, sciatica improves over time with conservative care—such as guided exercises, posture changes, chiropractic care, and physical therapy. Telemedicine can make these treatments easier to access and follow. What Is Telemedicine for Back and Nerve Pain? Telemedicine (also called telehealth) uses secure video or phone visits instead of in-person appointments. For spine and nerve problems, this often includes: -
Video visits with orthopedic surgeons, physiatrists, nurse practitioners, chiropractors, or pain specialists -
Secure messaging for questions and updates -
Online portals for test results, medication refills, and home exercise instructions Spine centers and pain clinics across the U.S. now use telemedicine as a core part of care for back pain, sciatica, spinal stenosis, degenerative disc disease, and more (UT Southwestern Medical Center, 2025; NJ Spine & Orthopedic, n.d.; Spine Institute of Southeast Texas, n.d.). UT Southwestern Medical Center+2NJ Spine & Orthopedic+2 Why telemedicine fits sciatica so well Sciatica patients often struggle to travel. Sitting in a car, climbing stairs, or walking across a parking lot can sharply increase leg pain. Telemedicine reduces this barrier by bringing the provider to you. Helpful advantages for people with sciatica: -
Less sitting and driving when pain is severe -
Faster access to evaluation and treatment plans -
Ability to show your home workspace, chair, and bed during the visit -
Easier inclusion of family members or caregivers in the visit How a Telemedicine Visit for Sciatica Works Most telemedicine visits follow a simple, structured process. Clinics like The Spine Institute of Southeast Texas and other spine centers lay out clear steps so patients know what to expect (Spine Institute of Southeast Texas, n.d.). southeasttexasspine.com+1 Typical flow of a visit -
Scheduling the visit -
You can call the clinic or schedule online. -
You choose video or, if needed, audio-only. -
Preparing your space and technology -
Test your camera, microphone, and internet connection. -
Set up in a quiet room where you can stand, sit, and move. -
Wear comfortable clothes so you can perform basic movement tests. -
Medical history and symptom review
Your provider will ask about: -
When the pain began -
Where the pain travels—back, buttock, thigh, calf, foot -
What makes it better or worse (sitting, walking, bending) -
Any numbness, weakness, or changes in bowel or bladder control -
Guided physical exam on camera
Telemedicine providers use simple at-home tests to gather information similar to an in-person exam (UT Southwestern Medical Center, 2025). UT Southwestern Medical Center You may be asked to: -
Walk in place or on your heels and toes -
Bend forward, backward, and to the sides -
Sit and straighten your leg to see if pain shoots down the leg -
Press on certain areas to see where it is tender -
Rate your pain during each motion -
Review of imaging and tests -
If you already had an X-ray, MRI, or CT scan, the provider can review the images and reports on screen. -
If you have not had imaging, your nurse practitioner or physician can order it at a local facility when needed (Everlywell, n.d.; NJ Spine & Orthopedic, n.d.). Everlywell+1 -
Diagnosis and treatment plan
After combining your history, exam, and any imaging, the provider can typically: -
Confirm whether your pain likely comes from the sciatic nerve -
Rule out red-flag conditions that require urgent in-person evaluation -
Build a step-by-step plan for pain relief and recovery -
Follow-up and monitoring -
Telemedicine makes it easy to schedule shorter, more frequent follow-ups. -
Your provider can adjust medications, exercises, and lifestyle strategies based on your progress (Spine Institute of Southeast Texas, n.d.; Apollo Spine & Pain, 2025). southeasttexasspine.com+1 Benefits of Telemedicine for Sciatica Management Research and clinical experience show that telemedicine is not just “second best.” For many spine patients, virtual care provides equal or even better access and continuity of care (UT Southwestern Medical Center, 2025; Spine Institute of Southeast Texas, n.d.). UT Southwestern Medical Center+1 Convenience and access -
No driving or parking when sitting is painful -
Less time away from work and family -
Access to specialists, even if you live far from a spine clinic -
Easier to schedule follow-ups before pain flares out of control Support for people with limited mobility Telemedicine is especially helpful if you: -
Use a cane, walker, or wheelchair -
Have trouble sitting or standing for long periods -
Are recovering from surgery, injury, or a recent flare -
Are older or have other health conditions that make travel difficult (Spine Institute of Southeast Texas, n.d.). southeasttexasspine.com+1 Better continuity of care Continuity means you stay connected with the same care team over time. Telemedicine helps by: -
Making it easier to attend follow-up appointments -
Allowing your providers to track symptoms between visits -
Supporting recovery with regular check-ins and education (Spine Institute of Southeast Texas, n.d.). southeasttexasspine.com+1 Medication and pain-management support During virtual visits, your nurse practitioner or physician can: -
Review and adjust prescription medications -
Discuss over-the-counter pain relievers -
Consider muscle relaxers, nerve pain medications, or short courses of steroids when appropriate -
Watch for side effects and drug interactions Telemedicine pain-management models emphasize blending medication with movement, stress reduction, and treatment of the underlying cause—not just masking symptoms (Everlywell, n.d.; Apollo Spine & Pain, 2025). Everlywell+1 How Integrative Chiropractic Telemedicine Helps Sciatica Chiropractic care focuses on the alignment and mobility of the spine, pelvis, and related joints. For many people with sciatica, conditions such as joint restriction, muscle tightness, or altered posture can contribute to nerve irritation (Tigard Chiropractic Auto Injury, n.d.; Evolve Chiropractic, n.d.; HealthCentral, n.d.). tigardchiropracticautoinjury.com+2Evolve Chiropractic+2 In an integrative telemedicine model, a chiropractor works closely with a nurse practitioner or other medical provider. That collaboration is central to Dr. Alexander Jimenez’s approach, in which his dual licensure as a chiropractor and family nurse practitioner enables him to consider both musculoskeletal causes and whole-person health factors in patients with sciatica. El Paso, TX Doctor Of Chiropractic What a chiropractor can do via telemedicine Even without hands-on spinal adjustments, chiropractors can still play a major role remotely: -
Remote assessment of movement and posture -
Observing how you sit, stand, walk, and bend -
Identifying patterns that increase nerve compression -
Looking for muscle imbalances and poor ergonomics -
Guided at-home exercises -
Gentle stretches for the hamstrings, glutes, and hip flexors -
Nerve glide exercises for the sciatic nerve -
Core-strengthening movements to support the spine -
Self-management strategies -
Training you to use pillows, supports, or rolled towels to keep a neutral spine -
Teaching safe ways to get in and out of bed or a car -
Coaching you on micro-breaks, standing desks, and movement habits for office work (Tigard Chiropractic Auto Injury, n.d.). tigardchiropracticautoinjury.com -
Lifestyle and activity modifications -
Adjusting exercise routines so you stay active without overloading the nerves -
Suggesting anti-inflammatory nutrition strategies in coordination with your medical provider -
Discussing stress management, as tension often increases pain perception How the nurse practitioner and chiropractor work together In an integrative telemedicine setup—like the model used by Dr. Jimenez—the nurse practitioner can: -
Order and interpret imaging when needed -
Rule out non-musculoskeletal causes of pain -
Manage medications, including pain relievers and nerve medications -
Coordinate referrals to pain specialists or surgeons when necessary The chiropractor then: -
Focuses on mechanical and movement-based causes -
Designs a progressive program of stretches, exercises, and posture changes -
Monitors how your spine and nervous system respond over time This team approach helps address both the root mechanical cause and the overall health picture, providing patients with a more comprehensive plan for sciatica recovery. Telemedicine, Physical Therapy Principles, and At-Home Rehab Many of the same principles used in physical therapy can be delivered through telemedicine. Clinics that focus on individualized rehab plans and goal-based treatment often use virtual visits to keep patients moving forward between in-person sessions (Integrative Medical of DFW, n.d.). Integrative Medical of DFW Examples of PT-style support delivered virtually Your integrated care team may use video visits to: -
Demonstrate and observe exercises such as: -
Progress or scale exercises based on pain and strength -
Check your form to protect the spine and avoid nerve flare-ups -
Create written or video home-exercise plans you can access anytime Dr. Jimenez’s clinical observations highlight that patients recovering from sciatica often do best when they: -
Perform small amounts of movement throughout the day rather than one large workout -
Avoid long periods of sitting, especially on soft couches or low chairs -
Combine targeted exercises with ergonomic fixes and better sleep positions El Paso, TX Doctor of Chiropractic Telemedicine makes it easier to reinforce these habits week after week. Telemedicine for Office and Remote Workers with Sciatica Office professionals and remote workers often develop or worsen sciatica from: -
Long hours of sitting -
Poor desk and chair setups -
Laptop use on couches or beds -
Repetitive bending or twisting to reach equipment Chiropractic and telemedicine-based ergonomic coaching can help by: -
Reviewing the home or office workstation on camera -
Suggesting changes in chair height, monitor level, and keyboard placement -
Recommending standing-break schedules and simple stretch routines (Tigard Chiropractic Auto Injury, n.d.). tigardchiropracticautoinjury.com Telemedicine lets the provider see your actual environment and make practical, personalized suggestions—not just imagine your setup. When Telemedicine Alone Is Not Enough While telemedicine is powerful, it does not replace all in-person care. Your provider will look for “red flags” that suggest you need urgent in-person evaluation or imaging (UT Southwestern Medical Center, 2025; NJ Spine & Orthopedic, n.d.). UT Southwestern Medical Center+1 Seek immediate in-person care or emergency evaluation if you have: -
Loss of bowel or bladder control -
Severe or quickly worsening leg weakness -
Numbness in the groin or inner thighs (“saddle anesthesia”) -
Recent major trauma, such as a fall or car accident -
Fever, chills, or unexplained weight loss along with back pain Telemedicine providers can help screen for these signs and quickly direct you to the right level of in-person care. How Dr. Alexander Jimenez Uses Telemedicine for Sciatica Dr. Alexander Jimenez, DC, APRN, FNP-BC, integrates telemedicine into his spine and injury practice to help patients with sciatica and other neuromusculoskeletal problems receive care even when they cannot easily come into the clinic. El Paso, TX Doctor Of Chiropractic Based on his dual-scope practice: -
As a nurse practitioner, he can: -
Take a full medical history -
Order and interpret imaging, such as MRI or CT, when appropriate -
Manage medications and coordinate with other specialists -
As a chiropractor, he can: -
Perform detailed movement and posture assessments over video -
Guide patients through home exercises and self-care strategies -
Educate patients on how spine mechanics and lifestyle factors affect the sciatic nerve Dr. Jimenez reports that telemedicine works especially well when: -
Patients live far from specialized spine clinics -
Pain makes it hard to travel during an acute flare -
Ongoing follow-up is needed to fine-tune exercises, medications, and lifestyle changes This integrated telemedicine model demonstrates how sciatica care can be both highly specialized and accessible, even at a distance. How to Prepare for Your Telemedicine Appointment for Sciatica Being prepared helps you get more from your virtual visit. The Spine Institute of Southeast Texas and other telemedicine programs recommend a few simple steps (Spine Institute of Southeast Texas, n.d.). southeasttexasspine.com+1 Before your visit -
Check your technology -
Test your device’s camera, microphone, and speakers or headphones. -
Make sure your battery is charged, or your device is plugged in. -
Confirm that you have a stable internet connection. -
Set up your space -
Choose a room with enough space to stand and move. -
Make sure the lighting lets your provider see your back, hips, and legs. -
Place your device so you can step back and show your whole body when needed. -
Gather key information -
A list of your current medications and supplements -
Past imaging reports (X-ray, MRI, CT), if you have them -
Notes on when your pain is worst, what triggers it, and what helps -
Dress comfortably -
Wear loose clothing so you can bend and move easily. -
Avoid long, tight skirts or very restrictive clothing. Questions to ask during the visit -
What do you think is causing my sciatica? -
Do I need imaging now, or can we start with conservative care? -
Which exercises should I do daily, and which should I avoid for now? -
How should I set up my workspace or home to reduce nerve irritation? -
When should I schedule my next telemedicine or in-person check-up? Putting It All Together: Telemedicine as a Powerful Tool for Sciatica Recovery Telemedicine has changed how spine and pain specialists, chiropractors, and nurse practitioners care for people with sciatica. It allows: -
Remote diagnosis using detailed history and guided movement tests -
Convenient follow-ups that keep your plan on track -
Medication management paired with lifestyle and exercise coaching -
Integrative chiropractic telemedicine support with posture, ergonomics, and home exercises -
Coordinated care that connects virtual visits with in-person imaging, injections, or surgery when needed (UT Southwestern Medical Center, 2025; Everlywell, n.d.; Spine Institute of Southeast Texas, n.d.). UT Southwestern Medical Center+2Everlywell+2 For many patients, especially those with limited mobility or busy schedules, telemedicine makes sciatica care more accessible, continuous, and personalized. If you are living with sciatic nerve pain, consider working with an integrated team—such as a nurse practitioner and chiropractor—who use telemedicine and in-person care together. With the right plan, you can move from flare-ups and frustration toward steadier relief, better function, and a more active life. Reclaim Your Mobility: Chiropractic Care for Sciatica Recovery References UT Southwestern Medical Center. (2025, November 19). Virtual visits, real pain relief: Telemedicine brings convenient care for back issues. Back and Spine MedBlog. https://utswmed.org/medblog/telemedicine-for-back-and-spine-issues/ UT Southwestern Medical Center Spine Institute of Southeast Texas. (n.d.). How does telemedicine work? The Spine Institute of Southeast Texas. https://www.southeasttexasspine.com/blog/how-does-telemedicine-work southeasttexasspine.com Spine Institute of Southeast Texas. (n.d.). How can telemedicine work to help treat my sciatica? The Spine Institute of Southeast Texas. https://www.southeasttexasspine.com/blog/how-can-telemedicine-work-to-help-treat-my-sciatica southeasttexasspine.com Spine Institute of Southeast Texas. (n.d.). How to prepare for your telemedicine appointment. The Spine Institute of Southeast Texas. https://www.southeasttexasspine.com/blog/how-to-prepare-for-your-telemedicine-appointment southeasttexasspine.com Spine Institute of Southeast Texas. (n.d.). 6 benefits of telemedicine. The Spine Institute of Southeast Texas. https://www.southeasttexasspine.com/blog/6-benefits-of-telemedicine southeasttexasspine.com Everlywell. (n.d.). How telemedicine pain management works. Everlywell. https://www.everlywell.com/blog/virtual-care/telemedicine-pain-management/ Everlywell NJ Spine & Orthopedic. (n.d.). What is telemedicine and can it work for back pain? NJ Spine & Orthopedic. https://www.njspineandortho.com/what-is-telemedicine-and-can-it-work-for-back-pain/ NJ Spine & Orthopedic Spine Institute of Southeast Texas. (n.d.). The many benefits of telemedicine. The Spine Institute of Southeast Texas. https://www.southeasttexasspine.com/blog/the-many-benefits-of-telemedicine southeasttexasspine.com Apollo Spine & Pain Management. (2025, May 11). How telemedicine can enhance your pain management plan. Apollo Spine & Pain Center. https://www.apollospineandpain.com/enhance-pain-management-with-telemedicine Apollo Spine and Pain Tigard Chiropractic Auto Injury. (n.d.). Sciatica solutions: How chiropractic care can help office professionals find relief. Tigard Chiropractic & Auto Injury. https://www.tigardchiropracticautoinjury.com/blog/sciatica-solutions-how-chiropractic-care-can-help-office-professionals-find-relief tigardchiropracticautoinjury.com Tigard Chiropractic Auto Injury. (n.d.). Dealing with pain from working remotely. Tigard Chiropractic & Auto Injury. https://www.tigardchiropracticautoinjury.com/blog/dealing-with-pain-from-working-remotely tigardchiropracticautoinjury.com Evolve Chiropractic. (n.d.). When sciatica strikes: How chiropractic care can provide relief. Evolve Chiropractic. https://myevolvechiropractor.com/when-sciatica-strikes-how-chiropractic-care-can-provide-relief/ Evolve Chiropractic HealthCentral. (n.d.). Chiropractor for sciatica: Causes, symptoms, & diagnosis. HealthCentral. https://www.healthcentral.com/condition/sciatica/chiropractic-treatment-sciatica HealthCentral Integrative Medical of DFW. (n.d.). Physical therapy. Integrative Medical of DFW. https://www.integrativemedical.com/physical-therapy Integrative Medical of DFW Jimenez, A. (n.d.). El Paso, TX chiropractor Dr. Alex Jimenez DC | Personal injury specialist. DrAlexJimenez.com. https://dralexjimenez.com/ El Paso, TX Doctor of Chiropractic The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for musculoskeletal injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable effort to provide supportive citations and to identify relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Sciatica can feel like a shocking zap in your back or leg, a deep ache, or a mix of numbness and weakness that makes every step harder. At its core, sciatica is a nerve problem: the sciatic nerve (or the nerve roots that form it) is being irritated, squeezed, or injured. When pressure is applied—by a herniated disc, narrowed canals, tight muscles, bone spurs, swelling, or even an external crush—the nerve’s structure and blood flow change. That physical change interferes with the nerve’s job of sending and receiving signals, which is why you feel pain, pins-and-needles, and weakness. The longer the pressure lasts, the more serious the damage can become. (Penn Medicine, 2024; Mayo Clinic, 2023). Penn Medicine+1 Quick anatomy: the sciatic nerve and its roots The sciatic nerve is the body’s largest nerve. It forms from several lower-spine nerve roots, travels through the pelvis and buttocks, then runs down the back of each thigh and splits near the knee to supply the lower leg and foot. Because it is long and passes through several tight spaces and mobile joints, it’s exposed to many “pinch points” where compression can happen—at the spine (disc herniation or stenosis), through the deep gluteal region (piriformis spasm or scar), or lower down along its branches. (Penn Medicine, 2024; iCliniq, 2024). Penn Medicine+1 What pressure does to a nerve: step-by-step When a nerve is compressed, three things show up early and drive symptoms: mechanical deformation, loss of blood flow (ischemia), and local inflammation. Together, they disturb myelin (the insulation), axons (the wires), and the tiny vessels that feed the nerve. 1) Mechanical deformation Direct pressure flattens and deforms the nerve. That physical squeeze can impair the way ions move across the nerve membrane, slowing or blocking electrical signals. In the mildest form of injury, you get a reversible conduction block (often called a neurapraxia-type picture) without overt axon loss, so symptoms can improve once pressure is removed. (NCBI Bookshelf, 2024). NCBI 2) Ischemia (reduced blood flow) Nerves have a delicate blood supply. Pressure collapses small vessels, cutting off oxygen and nutrients. With less energy, the nerve can’t maintain normal signaling, and a conduction block develops. If ischemia persists, structural injury follows. (NCBI Bookshelf, 2024; Verywell Health, 2023). NCBI+1 3) Myelin injury and demyelination Sustained compression strips or injure segments of myelin, slowing conduction. This is why you may feel intermittent tingling or shooting pain at first, then more constant numbness or weakness. If pressure keeps going, the axon itself can be damaged. (NCBI Bookshelf, 2024). NCBI 4) Axonal injury and Wallerian degeneration (with severe or prolonged pressure) With more force or more time, the axon breaks down. The distal portion degenerates (Wallerian degeneration), and weakness becomes more obvious because the muscle is no longer getting strong signals. Sensory loss also becomes clearer. Recovery takes longer because axons must regrow. (NCBI Bookshelf, 2024; ADR Spine, 2025). NCBI+1 5) Edema, inflammation, and fibrosis feed the cycle Compression increases intraneural fluid and inflammatory mediators. Swelling inside tight spaces (like fibrous tunnels) increases pressure even more, further cutting off blood flow. Over time, scar-like changes can appear around the nerve, making symptoms stubborn. (NCBI Bookshelf, 2024; PhysioWorks, n.d.). NCBI+1 Why symptoms vary (and what they mean) -
Pain often starts sharp or electric and may shoot from the lower back or buttocks down the leg, following the nerve’s path. It can worsen with coughing, sneezing, or prolonged sitting because these increase pressure or stretch on the irritated tissue. (Penn Medicine, 2024; Align Wellness Center, 2025). Penn Medicine+1 -
Numbness and tingling come from conduction block or demyelination in sensory fibers. (NCBI Bookshelf, 2024). NCBI -
Weakness signals motor fiber involvement. The pattern of weakness (e.g., trouble bending the knee or pointing the foot) hints at which root or segment is affected. (iCliniq, 2024). iCliniq -
Reflex changes and straight-leg-raise pain help clinicians confirm nerve-root irritation. (Penn Medicine, 2024). Penn Medicine When pressure is brief, symptoms may fade as swelling goes down and blood flow returns. But ongoing compression can cause chronic pain and even permanent damage, which is why early evaluation and load management matter. (Mayo Clinic, 2023; Dr. Matt Byington, n.d.). Mayo Clinic+1 The spectrum of nerve injury severity (simple view) -
Mild injury (conduction block): no lasting axon damage; symptoms can reverse after decompression and time. -
Moderate injury (axonal loss): weakness and numbness can persist; axons need to regrow; recovery may take months. -
Severe injury (complete disruption): little to no signal gets through; recovery requires significant time and sometimes surgery. These stages reflect the same underlying forces—mechanical stress, microvascular compromise, and inflammation—just at increasing intensity and duration. (NCBI Bookshelf, 2024; Mayo Clinic, 2023). NCBI+1 Special cases and compounding problems “Double-crush” patterns It’s common for a nerve to be irritated at more than one site (for example, at the spine and again in the deep gluteal region). Treating all contributing sites improves results; otherwise, symptoms can linger. (AMTA, n.d.; Southwest Wound Care, n.d.). American Massage Therapy Association+1 Compartment-like pressure In rare situations, swelling in a muscle compartment raises pressure enough to threaten nerve and muscle survival—an emergency. (PhysioWorks, n.d.). PhysioWorks! How clinicians confirm the diagnosis A careful history and exam are first. Providers look for pain patterns, neurologic changes (sensation, strength, reflexes), and provocative tests like the straight-leg raise. If needed, imaging (MRI) can show a disc herniation or stenosis, while nerve conduction studies and electromyography assess how well the nerve is working. (Penn Medicine, 2024; Dr. Matt Byington, n.d.). Penn Medicine+1 What makes pressure harmful over time? -
Duration: The longer the squeeze, the more likely demyelination and axon loss occur. (Mayo Clinic, 2023). Mayo Clinic -
Force: A strong crush can cause immediate axonal damage and lasting deficits. (Horton & Mendez, n.d.). -
Blood flow: Ischemia drives conduction block and structural injury. (Verywell Health, 2023; NCBI Bookshelf, 2024). Verywell Health+1 -
Inflammation and edema: Swelling raises pressure, making a tight tunnel even tighter. (NCBI Bookshelf, 2024). NCBI When sciatica becomes advanced Late-stage sciatica may bring severe constant pain, marked weakness, or even bladder/bowel changes, which require urgent care. Some severe cases risk permanent deficits if not addressed. (ADR Spine, 2025). adrspine.com How Integrative Chiropractic Care Helps Chiropractic integrative care brings three pillars together: spinal manipulation, soft-tissue therapy, and rehabilitation exercise, supported by education, ergonomic coaching, and coordinated referrals when necessary. The goal is to relieve pressure, calm inflammation, restore healthy motion, and rebuild strength and control, allowing the nerve to recover and making future flare-ups less likely. 1) Spinal manipulation and mobilization Gentle, targeted adjustments can improve joint mechanics in the lumbar spine and sacroiliac regions. Better alignment and motion can reduce mechanical pressure on irritated nerve roots and unload protective muscle spasm. In patients with acute radicular pain, clinicians often pair manipulation with traction, flexion-distraction, or directional preference (for example, extension-biased exercise with some disc herniations). (Physio Pretoria, n.d.; Penn Medicine, 2024). Physio Pretoria+1 Safety first: If you have progressive weakness, loss of reflexes, saddle numbness, or bladder/bowel symptoms, you need prompt medical evaluation. Chiropractors trained in integrative settings co-manage and refer in these situations. (AMTA, n.d.; OSMC, 2025). American Massage Therapy Association+1 2) Soft-tissue care around the gluteal tunnel and hip Piriformis spasm, deep gluteal adhesions, or hamstring-proximal tightness can locally irritate the sciatic nerve. Soft-tissue techniques (myofascial release, instrument-assisted work, gentle nerve-mobilization) reduce tone, improve gliding, and support circulation. If a double-crush pattern is present (spine + hip), both regions must be addressed for consistent results. (AMTA, n.d.; Southwest Wound Care, n.d.). American Massage Therapy Association+1 3) Progressive rehab to restore nerve “room,” strength, and control -
Nerve glides: careful sliders and tensioners restore mobility of the nerve relative to nearby tissues. -
Core and hip work, including gluteal and deep-core endurance, reduces the load on the lumbar segments and improves pelvic control. -
Hamstring and hip-flexor flexibility improves mechanics to reduce repeated irritation. -
Graded activity: careful step-ups in sitting time, walking, and lifting to build resilience.
Together, these reduce re-compression risk and improve daily function. (Physio Pretoria, n.d.; Align Wellness Center, 2025). Physio Pretoria+1 4) Education and load management Simple habits—avoiding long static sitting, changing positions often, hinging at the hips when lifting, and using a short, frequent walking pattern—protect the nerve while it heals. As inflammation settles and strength returns, you can resume more demanding tasks with less risk. (OSMC, 2025; AdvancedOSM, n.d.). OSMC+1 5) Imaging, testing, and referrals when needed If pain is severe, not improving, or accompanied by neurological loss, integrative teams may order MRI or electrodiagnostic testing (EMG/NCS) and coordinate with pain medicine, neurology, or surgery. (Penn Medicine, 2024; Dr. Matt Byington, n.d.). Penn Medicine+1 Dr. Alexander Jimenez, DC, APRN, FNP-BC: dual-scope, diagnostics, and complete care in El Paso At El Paso Integrative Chiropractic & Functional Medicine clinics led by Dr. Alexander Jimenez, care blends chiropractic and nurse-practitioner expertise. That dual scope supports full-spectrum evaluation of spine, hip, and lower-limb contributors to sciatica. The team emphasizes advanced imaging and diagnostics when indicated and provides comprehensive, step-by-step management plans. The clinics regularly treat injuries from work, sports, personal, and motor vehicle accidents (MVAs), and they are experienced with the medical documentation that injury cases often require. (Jimenez, n.d.). drmattbyington.com How that plays out for a sciatic nerve compression case: -
Dual-scope intake & exam -
Medical-chiropractic history and focused neuro exam (strength, reflexes, sensation). -
Straight-leg-raise and movement tests to map pain drivers. -
Triage for red flags (e.g., cauda equina features or rapidly progressive deficits). -
Targeted imaging & tests (as needed) -
Phase-based care plan -
Acute phase: unload the irritated segment (positional relief, McKenzie-style direction if appropriate, gentle mobilization), soft-tissue work to calm deep gluteal spasm, and simple nerve sliders. -
Subacute phase: add spinal manipulation as tolerated, progress hip and core endurance, restore hip hinge and gait. -
Return-to-life phase: task-specific progressions (sitting tolerance, driving, lift/transfer mechanics), sport- or job-specific drills. -
Co-management & reporting for injury cases -
For work injuries, sports trauma, personal injuries, and MVAs, the clinic coordinates with primary care, orthopedics, neurology, and legal teams. Clear visit notes, impairment summaries, and progress measures support both health outcomes and the documentation often needed in claims. (Jimenez, n.d.). drmattbyington.com Home strategies that support recovery (and what to watch for) -
Move often, in small doses. Short, frequent walks help circulation and calm nerve sensitivity. -
Position breaks. Switch between sitting, standing, and lying to avoid long static loads. -
Hip hinge and neutral spine. Use your hips for bending and lifting; keep loads close. -
Sleep setup. Try lying on your side with a pillow between your knees, or lie on your back with your knees partly elevated. -
Urgent signs: New or worsening leg weakness, foot drop, saddle numbness, or bladder/bowel changes—seek urgent care. (ADR Spine, 2025). adrspine.com Putting it together Pressure on the sciatic nerve sets off a predictable chain: mechanical squeeze → reduced blood flow → myelin injury → sometimes axonal loss. That’s why pain, tingling, and weakness can appear together—and why time under pressure matters so much. The right care plan lowers mechanical stress, restores healthy motion and muscle control, and protects the nerve while it heals. Integrative chiropractic care—combining manipulation, soft-tissue therapy, and progressive rehab—fits that mission well, especially when paired with careful screening, appropriate imaging, and referral when needed. (Penn Medicine, 2024; AMTA, n.d.; Mayo Clinic, 2023). Penn Medicine+2American Massage Therapy Association+2 From Diagnosis to Recovery: Navigating Sciatica with Chiropractic Care References Bauer, P. R., Lipson, J. C., & Pleacher, D. E. (2024). Nerve compression syndrome. In StatPearls. National Library of Medicine. https://www.ncbi.nlm.nih.gov/books/NBK230871/ NCBI Penn Medicine. (2024, December 6). Sciatica. https://www.pennmedicine.org/conditions/sciatica Penn Medicine Mayo Clinic. (2023, March 16). Pinched nerve: Symptoms & causes. https://www.mayoclinic.org/diseases-conditions/pinched-nerve/symptoms-causes/syc-20354746 Mayo Clinic American Massage Therapy Association (AMTA). (n.d.). Massage & nerve compression injuries. https://www.amtamassage.org/publications/massage-today/massage-nerve-compression-injuries/ American Massage Therapy Association Southwest Wound Care. (n.d.). Double crush syndrome: Understanding this complex nerve condition. https://southwestwoundcare.com/double-crush-syndrome-understanding-this-complex-nerve-condition/ Southwest Regional Wound Care Center Advanced Orthopaedics & Sports Medicine (AdvancedOSM). (n.d.). Peripheral nerve compression. https://www.advancedosm.com/peripheral-nerve-compression-orthopaedic-sports-medicine-specialist-cypress-houston-tx/ Advanced OSM OSMC. (2025, October 1). Is it nerve compression or something else? Common signs. https://www.osmc.com/2025/10/01/is-it-nerve-compression-or-something-else-common-signs/ OSMC Byington, M. (n.d.). Nerve compression. https://www.drmattbyington.com/nerve-compression.html drmattbyington.com iCliniq. (2024, October 18 review). Sciatic nerve injury – Causes, complications, diagnosis, and management. https://www.icliniq.com/articles/neurological-health/sciatic-nerve-injury iCliniq ADR Spine. (2025, March 3). Last stages of sciatica: Causes, symptoms, & treatment. https://www.adrspine.com/insights/last-stages-of-sciatica adrspine.com PhysioWorks. (n.d.). Compartment syndrome. https://physioworks.com.au/conditions/shin/compartment-syndrome/ PhysioWorks! Verywell Health. (2023, June 21). What is ischemia? https://www.verywellhealth.com/what-is-ischemia-p2-1745825 Verywell Health Physio Pretoria. (n.d.). Sciatic nerve pain: Sciatic nerve injury, compression, irritation. https://physiopretoria.co.za/pain/back/sciatic-nerve-pain Physio Pretoria Align Wellness Center. (2025, March 18). Sciatica nerve pain mystery: Possible suspects for your sciatica woes. https://alignwc.com/sciatica-nerve-pain-mystery-possible-suspects-for-your-sciatica-woes/ alignwc.com Horton & Mendez. (n.d.). Nerve pain after crush injury. https://hortonmendez.com/nerve-pain-after-crush-injury/ Jimenez, A. (n.d.). El Paso chiropractor & medically integrative wellness specialists. https://dralexjimenez.com/ drmattbyington.com General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
The sciatic nerve is the largest and longest nerve in the human body. It runs from the lower back through the hips, buttocks, and down each leg, carrying both motor and sensory signals. Because of its size and role, problems with the sciatic nerve can cause severe pain, weakness, and mobility challenges. Understanding how the sciatic nerve is built—and how chiropractic and integrative care can support its health—helps people make better choices for managing pain and preventing long-term problems. This article explains the structure of the sciatic nerve, its connective tissue layers, and how chiropractic adjustments, massage, physical therapy, nutrition, and integrative medicine work together to relieve pressure and restore balance. It also incorporates the clinical insights of Dr. Alexander Jimenez, DC, APRN, FNP-BC, a chiropractor and nurse practitioner in El Paso who provides dual-scope diagnosis, advanced imaging, and legal-medical care for patients recovering from injuries at work, in sports, and after motor vehicle accidents. Anatomy of the Sciatic Nerve Nerve Structure Basics Nerves are made up of bundles of fibers called axons, which are long projections of nerve cells (neurons). Axons carry signals from the brain and spinal cord to muscles and skin, allowing movement and sensation. These bundles are supported and protected by layers of connective tissue: -
Endoneurium: wraps individual axons -
Perineurium: bundles axons into groups called fascicles -
Epineurium: the outer layer that surrounds the whole nerve【training.seer.cancer.gov†source】 These layers protect the nerve from injury, reduce friction, and allow signals to move efficiently. The Cleveland Clinic explains that nerves are complex structures made of axons, connective tissue, and blood vessels that keep them alive and functioning【my.clevelandclinic.org†source】. The Sciatic Nerve’s Composition The sciatic nerve is formed by nerve roots from the lower spine (L4 to S3). These roots join together in the pelvis and travel as one thick nerve down the back of the leg【spine-health.com†source】. It is about as wide as a finger and branches out to smaller nerves in the leg and foot. Because it carries both motor and sensory fibers, damage or compression can cause pain, numbness, or weakness. ScienceDirect notes that the sciatic nerve is unique because it does not exchange fascicles with other nerves, which means its structure is consistent as it travels down the leg【sciencedirect.com/topics/immunology-and-microbiology/sciatic-nerve†source】. This makes compression or irritation especially disruptive. Common Problems With the Sciatic Nerve Sciatica Sciatica is the most well-known condition involving the sciatic nerve. It happens when the nerve is irritated or compressed, usually by a herniated disc, spinal misalignment, bone spur, or muscle tightness. Symptoms may include: -
Sharp, shooting pain in the lower back, buttock, or leg -
Numbness or tingling in the leg or foot -
Weakness in leg muscles -
Pain that worsens with sitting, coughing, or bending According to Alliance Orthopedics, sciatica can interfere with daily activities, but both chiropractic care and physical therapy are effective ways to treat it【allianceortho.com†source】. Neuropathy In some cases, nerve damage (neuropathy) affects the sciatic nerve. Neuropathy can come from diabetes, trauma, or poor circulation. It disrupts signal transmission and causes burning, tingling, or stabbing pain【emedicine.medscape.com†source】. Over time, damaged nerves can worsen without proper support. Chiropractic Care and Sciatic Nerve Relief Restoring Alignment Chiropractic adjustments focus on realigning the spine to reduce pressure on nerves. When vertebrae are misaligned, they may pinch or irritate nerve roots that form the sciatic nerve. Realignment restores space and relieves irritation. Enhanced Living Chiropractic explains that adjustments reduce nerve pressure and improve motion【enhancedlivingchiro.com†source】. Addressing the Root Cause Unlike pain medications that mask symptoms, chiropractic care works on the root cause of sciatica. Alliance Orthopedics reports that chiropractic treatments aim to restore function to the musculoskeletal system rather than simply treating pain【allianceortho.com†source】. Evidence-Based Benefits The American Association of Integrative Doctors highlights chiropractic as one of the most effective approaches for sciatica, often reducing pain and improving function without surgery【aaidoctors.com†source】. Studies also show that chiropractic care helps patients with chronic neuropathic pain by reducing inflammation and improving nervous system communication【sciencedirect.com/science/article†source】. Integrative Care for Sciatic Nerve Health Massage Therapy Massage therapy helps by relaxing tight muscles, improving circulation, and reducing inflammation around the sciatic nerve. By loosening the piriformis muscle—a small muscle near the sciatic nerve—massage may prevent irritation and relieve pain【atlaspainspecialists.com†source】. Physical Therapy Physical therapy strengthens the muscles that support the spine, improves posture, and prevents recurrence. Exercises target core muscles and hip flexibility, which reduces pressure on the nerve【allianceortho.com†source】. Acupuncture Acupuncture stimulates nerve pathways and reduces pain signals. It also encourages the body to release endorphins, natural chemicals that help with pain relief. Integrative practices show that acupuncture can complement chiropractic and physical therapy【nccih.nih.gov†source】. Nutrition and Nerve Support Nerves need nutrients to repair and function well. Vitamin B12, B-complex vitamins, and alpha-lipoic acid are especially important for nerve sheath maintenance and overall nerve health【rxwellness.net†source; asutahealth.org†source; verywellhealth.com†source】. A diet rich in leafy greens, lean proteins, and healthy fats supports healing and reduces inflammation. Dr. Alexander Jimenez’s Clinical Insights Dr. Alexander Jimenez, DC, APRN, FNP-BC, has over 30 years of experience in El Paso treating musculoskeletal and nerve conditions. His clinic focuses on dual-scope care—chiropractic adjustments combined with advanced nurse practitioner skills. This allows for comprehensive evaluation, including advanced imaging such as MRI and CT scans to assess neuromusculoskeletal injuries【dralexjimenez.com†source】. Treatment of Injuries Dr. Jimenez’s clinic treats patients with work injuries, sports trauma, and motor vehicle accidents. Sciatica is common after accidents, when sudden forces strain the lower back and hips. His approach combines: -
Chiropractic adjustments for spinal alignment -
Massage and physical therapy for soft tissue recovery -
Nutritional support for nerve healing -
Acupuncture for pain reduction -
Legal documentation for personal injury cases to ensure patients receive full care and support【linkedin.com/in/dralexjimenez†source】 Preventing Long-Term Problems Dr. Jimenez emphasizes that untreated sciatica or nerve pain can lead to chronic weakness, mobility loss, and permanent nerve damage. By addressing the root causes and supporting healing with integrative methods, patients recover faster and reduce the risk of future disability. The Role of Integrative Medicine in Pain Care The International Association for the Study of Pain defines integrative pain care as individualized, mechanism-guided, and coordinated across providers【iasp-pain.org†source】. Combining chiropractic, massage, physical therapy, nutrition, and medical care creates a more complete healing environment. Patients often report faster recovery, improved function, and better quality of life【getweave.com†source】. Conclusion The sciatic nerve is a complex bundle of axons supported by connective tissue that allows signals to move efficiently from the spine to the legs. When this nerve is irritated, conditions like sciatica cause pain and disability. Chiropractic care helps by restoring spinal alignment and relieving nerve pressure, while integrative therapies such as massage, physical therapy, acupuncture, and nutritional support create a well-rounded path to healing. With clinical expertise from providers like Dr. Alexander Jimenez in El Paso, patients benefit from advanced imaging, dual-scope diagnosis, and integrative treatment that addresses both the medical and legal sides of recovery. This whole-body approach ensures that people not only recover from nerve pain but also strengthen their health to prevent future problems. From Diagnosis to Recovery: Navigating Sciatica with Chiropractic Care | El Paso, TX References -
Alliance Orthopedics. (n.d.). Do I need a chiropractor or physical therapy for sciatica relief? Link -
Alliance Orthopedics. (n.d.). Can chiropractic care help with sciatica? Link -
American Association of Integrative Doctors. (n.d.). Chiropractic treatment for sciatica. Link -
Asuta Health. (n.d.). Natural approaches to neuropathic pain relief. Link -
Atlas Pain Specialists. (n.d.). Can a chiropractor help with nerve pain? Link -
Byju’s. (n.d.). Structure of a nerve. Link -
Cleveland Clinic. (n.d.). Nerves. Link -
Dr. Alexander Jimenez. (n.d.). Clinical insights on chiropractic and integrative care. Link -
Enhanced Living Chiropractic. (n.d.). How chiropractic care can help with sciatica. Link -
Emedicine Medscape. (n.d.). Nerve cells overview. Link -
GetWeave. (n.d.). Integrative health practices. Link -
International Association for the Study of Pain. (2023). Integrative pain care. Link -
NCCIH. (n.d.). Complementary, alternative, or integrative health. Link -
RxWellness. (n.d.). Natural therapies for nerve damage. Link -
ScienceDirect. (n.d.). Sciatic nerve anatomy. Link) -
ScienceDirect. (2021). Chronic neuropathic pain and integrative modalities. Link -
Spine-Health. (n.d.). Sciatic nerve anatomy. Link -
Verywell Health. (2024). Supplements for neuropathy. Link General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters and issues that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Find relief from sciatica, causing low back & hip pain through targeted treatments and lifestyle adjustments. Introduction Sciatica isn’t just a fancy word for leg pain—it’s a relentless, nerve-rattling condition that can make you feel like your lower body is staging a coup against your sanity. Imagine a sharp, electric jolt shooting from your lower back, through your hips, and down your leg, like a sadistic lightning bolt with a personal vendetta. For some, it’s a dull ache that lingers like an uninvited guest; for others, it’s a burning sensation that makes sitting, standing, or even existing feel like a punishment. But fear not—this blog post is your guide to understanding sciatica, its connection to low back and hip pain, and why chiropractic care, particularly from experts like Dr. Alexander Jimenez, DC, APRN, FNP-BC, in El Paso, Texas, can be your knight in shining armor. With a touch of dark humor to keep things bearable (think Wednesday Addams smirking at your suffering), we’ll dive into the sciatic nerve’s role, how it disrupts your daily life, and why chiropractic care is a game-changer. We’ll also explore Dr. Jimenez’s expertise in personal injury cases, bridging the gap between medical treatment and legal documentation. Buckle up—it’s going to be a long, informative ride. What Is Sciatica? A Nerve-Wracking Introduction Sciatica is the kind of pain that makes you wonder if you’ve been cursed by a vengeful witch. It’s not a single condition but a collection of symptoms caused by irritation or compression of the sciatic nerve, the longest and thickest nerve in your body, stretching from your lower back through your hips, buttocks, and down each leg (Jimenez, 2017). Picture it as a highway of misery, with pain, tingling, numbness, or weakness radiating along its path, usually affecting just one side of your body. It’s like your leg decided to throw a tantrum while your back eggs it on. The sciatic nerve originates from the L4 to S3 nerve roots in the lower spine, forming a thick bundle that exits the pelvis and travels down the leg (Davis et al., 2024). When something—be it a herniated disc, spinal stenosis, or a rogue muscle like the piriformis—pinches or irritates this nerve, you’re in for a world of hurt. Up to 40% of people with low back pain experience sciatica, and it’s not just a minor inconvenience; it can disable you, costing you mobility, sleep, and the ability to enjoy life without wincing (Jimenez, 2017). Let’s be real: sciatica doesn’t care if you have a big presentation or a hot date. It’ll make you hobble like a pirate with a peg leg, grimacing with every step. And if you’re thinking, “Oh, it’s just back pain,” think again. Sciatica is the VIP of pain, demanding attention and refusing to be ignored. References The Sciatic Nerve: The Culprit Behind the Chaos The sciatic nerve is like the body’s overzealous electrical wiring, connecting your lower spine to your legs and feet. It’s a massive bundle of nerve roots—L4, L5, S1, S2, and S3—that merge to form a nerve as wide as a penny (Cleveland Clinic, 2023). It runs from the lumbar spine, through the pelvis, under the piriformis muscle in your buttocks, and down the back of each thigh, branching out to your feet. It’s responsible for motor functions (like moving your legs) and sensory functions (like feeling that delightful pins-and-needles sensation when it’s angry). When this nerve gets irritated, it’s like a grumpy electrician short-circuiting your entire lower body. Compression or inflammation can come from several sources: - Herniated Discs: The gel-like center of a spinal disc bulges or ruptures, pressing on the nerve roots (Konstantinou & Dunn, 2008).
- Spinal Stenosis: The spinal canal narrows, squeezing the nerve like a cruel hug (Valat et al., 2010).
- Piriformis Syndrome: That sneaky piriformis muscle in your butt spasms or tightens, pinching the sciatic nerve (Hicks et al., 2021).
- Sacroiliitis or Pelvic Issues: Inflammation or injury in the sacroiliac joint or pelvis can mimic or cause sciatica-like pain (Jimenez, 2017).
Think of your sciatic nerve as a diva who throws a fit when her stage (your spine or hips) isn’t perfectly aligned. And when she’s upset, she’ll make sure you feel it from your lower back to your toes. References - Cleveland Clinic. (2023). Sciatica: What it is, causes, symptoms, treatment & pain relief. https://my.clevelandclinic.org/health/diseases/12792-sciatica
- Hicks, B. L., Lam, J. C., & Varacallo, M. (2021). Piriformis syndrome: A cause of nondiscogenic sciatica. Current Sports Medicine Reports, 20(2), 97–103. https://pubmed.ncbi.nlm.nih.gov/33595999/
- Jimenez, A. (2017). Sciatica from low back & hip pain. DrAlexJimenez.com. https://dralexjimenez.com/sciatica-caused-by-low-back-and-hip-pain/
- Konstantinou, K., & Dunn, K. M. (2008). Sciatica: Review of epidemiological studies and prevalence estimates. Spine, 33(22), 2464–2472. https://pubmed.ncbi.nlm.nih.gov/18923325/
- Valat, J. P., Genevay, S., Marty, M., Rozenberg, S., & Koes, B. (2010). Sciatica. Best Practice & Research Clinical Rheumatology, 24(2), 241–252. https://pubmed.ncbi.nlm.nih.gov/20227645/
How Sciatica Disrupts Your Daily Routine Sciatica doesn’t just hurt—it’s a lifestyle saboteur. Imagine trying to sit through a movie when every shift in your seat feels like a cattle prod to your backside. Or picture yourself limping through the grocery store, clutching the cart like it’s your lifeline, while your leg screams in protest. Sciatica can turn mundane tasks into Herculean challenges, affecting: - Mobility: Walking, standing, or climbing stairs becomes a painful ordeal, especially if the pain radiates below the knee (Davis et al., 2024).
- Sitting: Prolonged sitting, like at a desk or in a car, is torture because it puts extra pressure on the sciatic nerve (Jimenez, 2017).
- Sleep: Finding a comfortable position is like solving a Rubik’s Cube blindfolded, leading to restless nights and grumpy mornings.
- Work: If your job involves sitting, lifting, or twisting, sciatica can make you dread clocking in, potentially leading to missed days or disability (Jimenez, 2017).
- Mental Health: Chronic pain breeds frustration, anxiety, and even depression, as you mourn your ability to live pain-free (Ferreira et al., 2023).
Wednesday Addams would probably say, “Sciatica is the perfect reminder that life is just a series of unfortunate events, and your body is the stage.” It’s not just physical—it’s a psychological battle, too, as you wrestle with the constant discomfort and the fear that it might never end. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
The Impact of 18-Wheeler Accidents on the Human Body When an 18-wheeler collides with a car or another vehicle, the results are often catastrophic due to the truck's massive size and weight. Victims of such accidents commonly suffer from spinal trauma and musculoskeletal injuries that can severely impact daily life. The forceful impact can result in spinal fractures, disc herniations, spinal cord contusions, and nerve impingements, all of which require immediate medical attention (Wyatt Law Firm). Common Spinal Injuries After Truck Accidents 1. Herniated Discs: A herniated disc happens when the inner gel of the spinal disc leaks out and irritates nearby nerves. This is a common injury in rear-end and high-speed collisions (Complete Injury Management). 2. Spinal Fractures: The high-impact forces from an 18-wheeler crash can cause compression fractures or even burst fractures in the spine. These injuries can be life-threatening if not treated properly (CK Legal). 3. Spinal Cord Contusions and Lacerations: Contusions are bruises on the spinal cord, while lacerations refer to cuts. Both injuries can cause permanent damage and require surgical intervention (Ohio Truck Accident Help). Spinal Cord Damage: Complete vs Incomplete Injuries Spinal cord injuries (SCIs) are classified into two types: complete and incomplete. A complete injury leads to total loss of motor and sensory function below the injury site, while an incomplete injury results in partial loss of function. These outcomes vary depending on the injury’s location and severity (Mayo Clinic). In truck accidents, both types are common. Complete injuries can lead to permanent quadriplegia, while incomplete injuries might allow some mobility or sensation (TruckAccidents.com). The Development of Sciatica After a Spinal Injury Sciatica refers to pain that radiates down one or both legs due to irritation of the sciatic nerve. This often results from spinal injuries such as herniated discs or spinal stenosis—narrowing of the spinal canal that compresses nerves (Chiropractic Tucker). Additional symptoms of sciatica include numbness, tingling, and muscle weakness in the legs, making everyday activities painful or impossible (Inspired Spine). Spinal Stenosis and Nerve Compression Spinal stenosis often develops after trauma and can lead to significant nerve compression. This condition causes not only back pain but also radiating symptoms such as numbness and weakness in the lower limbs (Spine Health). After an 18-wheeler accident, untreated spinal stenosis can significantly limit a person's mobility and quality of life (UMMS). Whiplash and Soft Tissue Damage Whiplash is one of the most common musculoskeletal injuries after a truck crash. It results from the head rapidly snapping backward and then forward, damaging ligaments, tendons, and sometimes discs (Smith Law Center). Symptoms of whiplash include neck stiffness, headaches, shoulder pain, and even dizziness. Long-term complications may involve nerve damage (Ripple Chiropractic). Diagnosing and Imaging Spinal Injuries To determine the extent of spinal and musculoskeletal damage after an 18-wheeler crash, healthcare providers utilize tools such as MRI, CT scans, and X-rays. These imaging techniques help identify fractures, soft tissue damage, disc bulges, and nerve compression. Dr. Alexander Jimenez, a chiropractor and nurse practitioner in El Paso, TX, specializes in dual-scope diagnostic and treatment approaches for accident victims. His clinical practice emphasizes not only spinal alignment and soft tissue repair but also advanced imaging and legal documentation for personal injury claims (Dr. Alex Jimenez). Dr. Jimenez's Dual-Scope Injury Treatment Approach Dr. Jimenez combines chiropractic adjustments, soft tissue therapy, and functional rehabilitation with nurse practitioner responsibilities. This dual role allows him to: -
Provide full medical documentation for legal cases -
Coordinate with attorneys for personal injury claims -
Order advanced diagnostics and interpret imaging -
Administer pain management and rehabilitative plans His clinic focuses on restoring spinal function while ensuring patients are protected legally and physically (Personal Injury Doctor Group). Integrative Medicine and Chiropractic Recovery After a spinal injury from a truck accident, chiropractic care focuses on restoring spinal alignment and reducing nerve pressure. Complementary therapies may include: -
Acupuncture: Reduces inflammation and promotes circulation -
Massage therapy: Eases muscle spasms and tension -
Physical therapy: Strengthens the surrounding musculature -
Nutritional support: Promotes tissue healing Dr. Jimenez integrates these treatments to create personalized recovery plans that address pain, function, and long-term mobility (WellnessDoctorRX). Legal Support in Personal Injury Cases Victims of 18-wheeler accidents often face legal hurdles in addition to medical recovery. Dr. Jimenez’s dual credentials enable him to: -
Generate admissible legal-medical reports -
Attend depositions or provide expert testimony -
Offer consistent documentation from diagnosis to recovery This dual role significantly improves patients’ chances of receiving just compensation for spinal injuries. Conclusion: Recovery Through Holistic, Legal-Medical Care 18-wheeler accidents frequently cause complex spinal and musculoskeletal injuries, including herniated discs, spinal stenosis, whiplash, and sciatica. Accurate diagnosis and integrative care are crucial for recovery. Dr. Alexander Jimenez’s approach combines advanced imaging, chiropractic therapy, nurse practitioner interventions, and legal-medical support. This comprehensive method ensures that patients not only heal physically but also receive the legal documentation necessary to protect their rights and financial future. References Chiropractic Tucker. (n.d.). Can a car accident cause sciatica? https://www.chiropractictucker.com/can-a-car-accident-cause-sciatica/ CK Legal. (n.d.). Spinal cord injuries from trucking accidents. https://cklegal.com/spinal-cord-injuries-from-trucking-accidents/ Complete Injury Management. (n.d.). The 6 common types of spine injury from a car accident. https://www.completeinjurymanagement.com/the-6-common-types-of-spine-injury-from-a-car-accident/ DLG Trial Law. (n.d.). Spinal cord injury from truck accidents. https://dlgtriallaw.com/practice-areas/personal-injury/truck-accident/spinal-cord-injury-from-truck-accidents/ Horst Shewmaker. (n.d.). Settlement for car accident back and neck injury. https://horstshewmaker.com/settlement-car-accident-back-and-neck-injury/ Huber Thomas Law. (n.d.). Spinal cord injuries in truck accidents. https://huberthomaslaw.com/spinal-cord-injuries-truck-accidents/ Inspired Spine. (n.d.). Radiculopathy. https://inspiredspine.com/conditions-treatments/conditions/radiculopathy/ Loncar Lyon Jenkins. (n.d.). Whiplash injuries and the aftermath explained. https://loncarlyonjenkins.com/blog/whiplash-injuries-and-the-aftermath-explained/ Mayo Clinic. (n.d.). Spinal cord injury - symptoms and causes. https://www.mayoclinic.org/diseases-conditions/spinal-cord-injury/symptoms-causes/syc-20377890 MedMal Law. (2023, September). Common spine injuries from car accidents. https://www.medmal-law.com/blog/2023/september/common-spine-injuries-from-car-accidents/ Michigan Auto Law. (2023, March 8). Spine injury from car accident. https://www.michiganautolaw.com/blog/2023/03/08/spine-injury-from-car-accident/ Ohio Truck Accident Help. (n.d.). Spinal injuries. https://ohiotruckaccidenthelp.com/injuries/spinal-injuries/ Personal Injury Doctor Group. (n.d.). Auto injuries and whiplash healing process through physical therapy. https://personalinjurydoctorgroup.com/ Ripple Chiropractic. (n.d.). Car accident injury conditions. https://ripplechiropractic.com.au/conditions/car-accident-injury/ Roden Law. (n.d.). Truck accident injuries. https://rodenlaw.com/blog/truck-accident-injuries/ Seachange Chiropractic. (n.d.). Car crash injury rehab: The roles of chiropractic, rest and exercise. https://seachangechiropractic.com/car-crash-injury-rehab-the-roles-of-chiropractic-rest-and-exercise/ Smith Law Center. (n.d.). Common back injury after car accident. https://www.smithlawcenter.com/blog/common-back-injury-after-car-accident/ Spine-Health. (n.d.). What is spinal stenosis? https://www.spine-health.com/conditions/spinal-stenosis/what-spinal-stenosis TruckAccidents.com. (n.d.). Paralysis from truck accidents. https://truckaccidents.com/tennessee/practice-areas/paralysis/ UMMS. (n.d.). Overview of low back pain. https://www.umms.org/ummc/health-services/orthopedics/services/spine/patient-guides/overview-low-back-pain Victims Lawyer. (n.d.). Spinal injuries caused by car accidents. https://www.victimslawyer.com/practice-areas/car-accidents/car-accidents-injuries/spinal-injuries-caused-by-car-accidents/ Wyatt Law Firm. (n.d.). Spinal cord and paralysis injuries. https://www.wyattlawfirm.com/truck-accident/spinal-cord-paralysis-injuries/ Your PGH Lawyer. (n.d.). What is the number one injury for truck drivers? https://yourpghlawyer.com/what-is-the-number-one-injury-for-truck-drivers/ WellnessDoctorRX. (n.d.). Dr. Alexander Jimenez. https://www.linkedin.com/in/dralexjimenez/ General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicine, as well as wellness, sensitive health issues, and functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and the jurisdiction in which they are licensed to practice. We utilize functional health and wellness protocols to treat and support care for injuries or disorders affecting the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has made a reasonable attempt to provide supportive citations and identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez, DC, MSACP, CCST, IFMCP*, CIFM*, ATN* Email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Motor vehicle accidents (MVAs) are a leading cause of spinal injuries, including damage to ligaments in the lower back, which can sometimes lead to sciatica. This painful condition radiates from the lower back down the leg. In El Paso, Texas, Dr. Alexander Jimenez, a highly qualified chiropractor and board-certified family nurse practitioner, stands out as a trusted provider for victims of personal injury. With over 25 years of experience, Dr. Jimenez uses advanced imaging, diagnostic assessments, and a unique dual-scope approach to treat these injuries and support legal documentation for personal injury cases. This blog examines the clinical rationale behind ligamentous injuries resulting from motor vehicle accidents (MVAs), their connection to sciatica, and how Dr. Jimenez’s expertise benefits patients in El Paso. What Are Ligamentous Injuries in MVAs? Ligaments are tough, fibrous tissues that connect bones and provide stability to the spine. In MVAs, the sudden forces from collisions—whether rear-end, side-impact, or rollover—can stretch or tear these ligaments, particularly in the lumbar spine (lower back). A study found that flexion-distraction injuries, which often involve ligament damage, account for about 8.8% of major thoracic and lumbar spine injuries in MVAs (Occupant and Crash Characteristics). These injuries are more common in children and young adults under 30 and are often associated with two-point seatbelts or improperly used three-point seatbelts. For example, during a rear-end collision, the body is thrust forward while the head and torso lag, causing a rapid extension and flexion of the spine. This can strain ligaments, such as the anterior longitudinal ligament or posterior longitudinal ligament, leading to instability. Such injuries are particularly concerning in the lumbar spine, where they can affect nearby nerves, potentially causing symptoms like sciatica. Common Ligamentous Injuries in MVAs Injury Type Description Prevalence in MVAs Associated Factors Flexion-Distraction Ligament tears due to forward bending, often with Chance fractures 8.8% of major T&L injuries Common in young occupants, two-point seat belts Sprains Stretching of ligaments without a complete tear Common in low-severity crashes Seat belt use, minor collisions Posterior Ligamentous Disruption Damage to ligaments like the interspinous or supraspinous ligaments Often with facet dislocation High-severity crashes, neurological deficits Source: Occupant and Crash Characteristics How Ligamentous Injuries Lead to Sciatica Sciatica, also known as lumbar radiculopathy, is characterized by pain, numbness, or tingling that radiates from the lower back through the buttocks and down one or both legs. It occurs when the sciatic nerve, the largest nerve in the body, is compressed or irritated. The sciatic nerve originates from nerve roots (L4-S3) in the lumbar spine and sacrum, making it vulnerable to spinal injuries. Ligamentous injuries from MVAs can contribute to sciatica by causing spinal instability. When ligaments are damaged, the spine may move excessively, leading to misalignment or pressure on nearby structures like intervertebral discs or nerve roots. For instance, a torn ligament in the sacroiliac joint or lumbar spine can mimic sciatica symptoms by referring pain down the leg (Lumbar Instability Review). Additionally, instability may cause disc herniation, where the gel-like center of a disc bulges out and presses on the sciatic nerve roots, a common cause of sciatica (Sciatica Causes). In MVAs, the lower back often absorbs a significant amount of impact, especially in seated occupants. This can lead to combined injuries, such as ligament sprains and disc herniations, which together increase the likelihood of sciatica. For example, a study notes that herniated discs from MVAs are a primary cause of sciatica, but ligament damage can exacerbate this by destabilizing the spine (Sciatica and Car Accidents). Mechanisms Linking Ligamentous Injuries to Sciatica - Spinal Instability: Damaged ligaments, such as the posterior longitudinal ligament, allow excessive vertebral movement, which can potentially compress nerve roots.
- Disc Herniation: Instability resulting from ligament damage can lead to disc bulging, which presses on the sciatic nerve.
- Inflammation: Ligament injuries cause swelling, which may irritate nearby nerves, mimicking sciatica symptoms.
- Sacroiliac Joint Dysfunction: Injury to the sacroiliac ligaments can cause pain to radiate down the leg, resembling sciatica.
Learn more about sciatica symptoms at Sciatica Overview. Dr. Alexander Jimenez: A Trusted Provider in El Paso Dr. Alexander Jimenez, DC, APRN, FNP-BC, is a leading healthcare provider in El Paso, Texas, with a unique combination of chiropractic and medical expertise. At Injury Medical & Chiropractic Clinic, he has treated numerous MVA victims over his 25-year career, specializing in conditions such as sciatica, whiplash, and back pain. His dual licensure as a Doctor of Chiropractic and a board-certified Family Nurse Practitioner allows him to offer integrative care that addresses both the biomechanical and medical aspects of injuries. Dr. Jimenez’s practice is particularly relevant in El Paso, where MVAs are a significant cause of personal injury. His clinic focuses on restoring mobility and health through advanced therapies, including chiropractic adjustments, functional medicine, and patient-focused diet plans (Dr. Jimenez’s Staff). His reputation as a car accident specialist makes him a go-to provider for those seeking recovery and legal support after an MVA. Visit Dr. Jimenez’s Clinic for more information. Advanced Imaging and Diagnostic Assessments Accurate diagnosis is critical for treating ligamentous injuries and sciatica. Dr. Jimenez likely utilizes state-of-the-art imaging to assess MVA-related injuries, with MRI being the gold standard for detecting soft tissue damage, such as ligament tears. MRI has a sensitivity of 93% for detecting disc injuries and up to 100% for interspinous soft tissue damage, making it ideal for identifying ligamentous injuries (Trauma Imaging Strategies). Other imaging modalities include: - Plain X-rays are initially used to detect fractures or spinal deformities; however, they can miss up to 40% of cervical fractures.
- Multidetector CT (MDCT): Highly sensitive (97-100%) for bony injuries but less effective for soft tissues.
- MRI: Essential for ligamentous injuries, spinal cord lesions, and occult injuries, helping predict neurological recovery.
Dr. Jimenez’s diagnostic approach also includes physical examinations and, if necessary, electromyography (EMG) to assess nerve function. His website highlights his use of evidence-based protocols to create personalized treatment plans (Spinal Trauma Imaging). Dual-Scope Interventions: A Unique Approach Dr. Jimenez’s dual qualifications enable “dual-scope interventions,” which combine chiropractic and medical treatments. As a chiropractor, he uses spinal adjustments, mobility training, and rehabilitation to restore spinal alignment and reduce nerve pressure. As a nurse practitioner, he can order diagnostic tests, prescribe treatments, and manage overall health, addressing inflammation or other complications from MVA injuries. This integrated approach is particularly effective for sciatica caused by ligamentous injuries. For example, chiropractic adjustments can stabilize the spine, while medical interventions like anti-inflammatory medications or physical therapy protocols enhance recovery. His clinic’s use of specialized techniques, such as the “PUSHasRx System,” focuses on functional fitness and structural conditioning to support long-term healing (Dr. Jimenez’s Biography). Explore treatment options at Injury Medical Clinic. Bridging Medical Care and Legal Documentation In personal injury cases, proving that injuries resulted from a motor vehicle accident (MVA) is crucial for successful legal claims. Dr. Jimenez’s expertise makes him a vital conduit between medical care and legal documentation. His detailed assessments, supported by advanced imaging and clinical findings, provide robust evidence linking injuries like ligament damage or sciatica to the accident. This is especially important in El Paso, where personal injury cases often involve complex insurance claims or litigation. For instance, his ability to document spinal instability or nerve compression through MRI reports strengthens legal cases by clearly demonstrating causation (Back Injuries from Auto Accidents). His dual perspective ensures that patients receive medically necessary care while also meeting the documentation needs for legal proceedings. The Importance of Timely Treatment Untreated ligamentous injuries or sciatica can worsen, leading to chronic pain or disability. Dr. Jimenez emphasizes the importance of early intervention to prevent long-term complications. His clinic offers non-invasive treatments, including chiropractic care, physical therapy, and functional medicine, which are effective in managing sciatica and stabilizing the spine. For personal injury victims, timely treatment not only aids recovery but also strengthens their legal case by documenting injuries promptly. Learn about the risks of untreated injuries at Sciatica and Car Accidents. What makes Dr. Jimenez a top choice in El Paso? Dr. Jimenez’s unique qualifications and integrative approach make him an ideal choice for MVA victims in El Paso. His clinic’s focus on evidence-based care, combined with advanced diagnostics and personalized treatment plans, ensures optimal outcomes. Whether you’re dealing with sciatica, ligament damage, or other MVA-related injuries, Dr. Jimenez provides compassionate, comprehensive care tailored to your needs. If you’ve been in a car accident and are experiencing back pain or sciatica, don’t wait to seek help. Contact Injury Medical & Chiropractic Clinic Show in sidebar
Individuals dealing with pain in the buttocks and in the back of the thigh, along with numbness and tingling down to the bottom of the foot, may be experiencing hamstring syndrome, a condition caused by pressure on the sciatic nerve. What is the recommended treatment? Hamstring-Syndrome Relief The hamstrings are three muscles in the back of the thigh, extending from the pelvis or upper thigh across the back of the knee to the leg. This muscle group is important for bending the knee, straightening the hip, and stabilizing the knee. The sciatic nerve is a large nerve that runs from the lower back down the legs. It usually passes near or through these muscles, and the pelvis then runs under these muscles in the thigh. Hamstring syndrome refers to pain in the buttock and back of the thigh, often radiating down the leg, caused by compression or irritation of the sciatic nerve at the hamstring-insertion point on the ischial tuberosity, typically due to tight or scarred tissue. (Sakari Orava, 1997) Pain Location The pain is primarily felt in the buttock and back of the thigh, sometimes extending down the leg. It's characterized by pressure on the sciatic nerve, which runs through the buttock and into the back of the thigh, where it supplies the hamstring muscles. (Kaiser Permanente, 2024) Mechanism This pressure can occur due to: (Sakari Orava, 1997) (Kaiser Permanente, 2024) Fibrotic Bands - Tight, tendon-like, or scarred bands of tissue at the hamstring's insertion point/ischial tuberosity can irritate the sciatic nerve.
Compression - These bands can compress the nerve, especially when sitting or during activities that involve hip flexion and knee extension.
Traction - The sciatic nerve can also be stretched or irritated by the hamstring tendons.
Symptoms - Pain in the buttock and back of the thigh may radiate down the leg.
- Pain that is worse when sitting, stretching the hamstrings, or during activities like running. (Puranen J. & Orava S. 1988)
- Numbness or tingling in the back of the leg
Differential Diagnosis It's important to differentiate hamstring syndrome from other conditions that could be causing similar symptoms, including: - Piriformis syndrome
- Ischiogluteal bursitis
- Hamstring muscle strains
Treatment Hamstring syndrome relief may consist of the following: Conservative - Initial treatment focuses on rest, ice, stretching, and over-the-counter pain relievers.
Physical Therapy Injections - In some cases, injections with cortisone and numbing medicine may be used to reduce nerve inflammation and pain. (Lower Limb Surgery, 2024)
Surgery - In severe cases, surgery may be necessary to release the compressing bands and free the sciatic nerve. (Lower Limb Surgery, 2024)
Injury Medical Chiropractic & Functional Medicine Clinic Talk to a healthcare provider about what interventions would help the most. Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop an optimal health and wellness solution. We focus on what works for you to relieve pain, restore function, and prevent injury. Regarding musculoskeletal pain, specialists like chiropractors, acupuncturists, and massage therapists can help mitigate the pain through spinal adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal issues. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, and physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice. Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies that are available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol. To discuss the subject matter above further, please contact Dr. Alex Jimenez or us at 915-50-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Orava, Sakari. (1997). Hamstring syndrome. Operative Techniques in Sports Medicine, 5(3). https://doi.org/https://doi.org/10.1016/S1060-1872(97)80035-4. Kaiser Permanente. (2024). Hamstring Syndrome: Care Instructions. https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.hamstring-syndrome-care-instructions.abr3618 Puranen, J., & Orava, S. (1988). The hamstring syndrome. A new diagnosis of gluteal sciatic pain. The American Journal of Sports Medicine, 16(5), 517–521. https://doi.org/10.1177/036354658801600515 Zion Physical Therapy. (2023). Hamstring Tendinitis Vs. Hamstring Syndrome. https://www.zionpt.com/post/hamstring-tendinitis-vs-hamstring-syndrome Lower Limb Surgery. (2024). Hamstring Syndrome. https://www.lowerlimbsurgery.com/hamstring syndrome#:~:text=General%20Treatment%20Considerations,%E2%80%8B
Are there benefits to back cracking, risks, and how can it be done safely? Back Cracking Back cracking is intentionally applying pressure or twisting movements, producing a popping or cracking sound in the spine. Back cracking involves stretching or extending the spine. In most cases, it is considered safe when done gently as it can provide temporary relief from back pain and stiffness by: - Stretching the ligaments and muscles around the spine
- Releasing gas bubbles that may be causing pressure
- Improving joint mobility
Mechanism of Action - Cracking your back creates small gas bubbles in the synovial fluid (the lubricating fluid in the joints).
- These bubbles form when the pressure in the joints is suddenly released, causing a popping or cracking sound.
It is generally safe, but there are certain conditions under which individuals should avoid cracking their backs. Popping Sound Research has used a new type of magnetic resonance imaging (MRI), cine MRI, to study the noise source. Cine MRI produces moving images. - This study using this MRI found that the formation of bubbles makes a popping sound.
- The popping sound does not come from the popping of bubbles in the synovial fluid, as previously believed. (Kawchuk G. N. et al., 2015)
- When someone cracks their back, the force pulls the joint's bones apart, causing the pressure within the joint to drop and form a bubble, eventually dissipating. (Kawchuk G. N. et al., 2015)
Crepitus - Crepitus is the medical term for cracking or popping noise from joints.
- It is not a condition or disease but can be a symptom of one.
- Other terms include clicking or crunching.
Is It Safe To Perform Daily? Back cracking once a day is generally considered safe. But if it causes pain or swelling, then stop and contact a healthcare provider. If someone feels the need to crack their back more throughout the day, it could be a sign that they need to see a professional chiropractic healthcare provider. (AICA Orthopedics, 2022) Individuals may crack their backs to address certain conditions or to relieve various discomfort symptoms that can include: (National Center for Complementary and Integrative Health, 2025) - Headache
- Neck pain
- Lower back pain
- Sciatica
Individuals may often experience mild side effects like headache, stiffness, or pain. These side effects resolve within a day. Though back cracking can provide temporary relief for some conditions, some serious side effects like neurological problems or strokes have been reported. (National Center for Complementary and Integrative Health, 2025) Stretches and Movements When someone needs to crack their back, they can perform a spine stretch. Here are a couple of stretches and movements. (American Academy of Orthopedic Surgeons, 2022) Sitting Rotation Stretch - Sit on the floor with both legs straight.
- Cross the right foot over the left leg.
- Rotate the upper body to the right side and press against the right knee with the left elbow.
- Hold the stretch for 30 seconds and come back to the center.
- Repeat on the other side.
Knee to Chest - Lie flat on the ground.
- Lift one leg and bring the knee to the chest, pulling the knee in with your hands.
- Hold for five seconds.
- Repeat with the other leg.
Several back-cracking assistive devices, such as poles and wheels, are available. Talk to a healthcare provider to determine the right type and ensure it is safe for you and your condition or injury. Individuals Who Should Avoid Back Cracking Back cracking can cause additional stress or damage to the joints in those with back injuries or other conditions. Individuals with these conditions should avoid back cracking (AICA Orthopedics, 2022) - Numbness or tingling of the arms or legs.
- Osteoporosis
- Spinal cancer
- Spinal abnormalities
- Individuals who have a high stroke risk.
A Professional Back Adjustment A chiropractor is a healthcare provider who specializes in spine and spinal adjustments. They adjust the spine and other areas of the body to correct misalignment problems, reduce and relieve pain, and allow the body to recover independently. (National Library of Medicine. MedlinePlus, 2023) The chiropractor will take a health history to learn about previous injuries and conditions. Then, they will evaluate the patient and determine the best course of action. Although a chiropractor performs spinal adjustments, they may also incorporate other treatments, including: (National Library of Medicine. MedlinePlus, 2023) - Stretching
- Non-surgical decompression and traction
- Acupuncture
- Muscle Energy Technique (MET)
- Exercise routines
- Heat
- Ice
- Electrical stimulation
- Dietary supplements
- Nutrition and lifestyle counseling
Injury Medical Chiropractic & Functional Medicine Clinic Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to develop an optimal health and wellness solution. We focus on what works for you to relieve pain, restore function, and prevent injury. Regarding musculoskeletal pain, specialists like chiropractors, acupuncturists, and massage therapists can help mitigate the pain through spinal adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal issues. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Kawchuk, G. N., Fryer, J., Jaremko, J. L., Zeng, H., Rowe, L., & Thompson, R. (2015). Real-time visualization of joint cavitation. PloS one, 10(4), e0119470. https://doi.org/10.1371/journal.pone.0119470 AICA Orthopedics. (2022). Is cracking your back bad? https://aica.com/is-cracking-your-back-bad/ National Center for Complementary and Integrative Health. (2025). Spinal manipulation: what you need to know. Retrieved from https://www.nccih.nih.gov/health/spinal-manipulation-what-you-need-to-know American Academy of Orthopedic Surgeons. (2022). Spine conditioning program. https://orthoinfo.aaos.org/en/recovery/spine-conditioning-program/ National Library of Medicine. MedlinePlus. (2023). Chiropractic. Retrieved from https://medlineplus.gov/chiropractic.html
Can individuals dealing with sciatica incorporate nonsurgical treatments to reduce thigh pain and restore mobility in the legs and hips? The Tensor Fascia Latae Do you feel stiffness or tightness in your legs, feet, and hips? Have you experienced walking crookedly when running errands? Or have you experienced radiating pain from your gluteal region down to your feet? The hips, thighs, and legs have numerous muscles, tissues, and ligaments surrounding the skeletal bone in the body’s lower extremities. These components allow the lower half of the body to stabilize the upper body’s weight and enable the individual to be mobile throughout the day. One muscle that works together is the tensor fasciae latae (TFL) muscle. The TFL muscle is part of the proximal anterolateral thigh between the deep fibers of the iliotibial (IT) band. It works with the gluteal muscles in various hip movements and assists with the knees. (Trammell et al., 2025) This muscle is poorly misunderstood as it helps with the hips and knee joint and pelvic stability. (Iyengar et al., 2022) At the same time, it has a casual relationship with the IT band. The Iliotibial Band (ITB) The iliotibial (IT) band is part of the lower extremities as it is a tough, fibrous fascial tissue that works together with the TFL muscle and has various functional roles that are dependent on posture and allows the individual to be mobile via walking, sprinting, and running. (Hutchinson et al., 2022) However, this muscle’s main function is knee flexion. When environmental factors affect the body, it can cause irritation and inflammation to the IT band, causing knee pain. (Martinez-Velez et al., 2020) When dealing with issues within their lower extremities, they affect the IT band, TFL muscle, and the thighs. Environmental factors can also affect the lower extremities as the surrounding muscles can aggravate the nerve roots, thus leading to sciatica pain. We associate with certified medical providers who inform our patients of how sciatica can negatively impact the lower extremities, especially the thighs. While asking important questions to our associated medical providers, we advise patients to integrate various non-invasive treatments to reduce sciatica and help regain mobility back to the lower body. Dr. Alex Jimenez, D.C., envisions this information as an academic service. Disclaimer. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Stress on the lower back during pregnancy often leads to back (upper, middle, lower), sciatica, and leg pain. Can you use a massage gun while pregnant? Pregnancy Massage Gun Use Pregnant women often experience back, hip, and leg pain along with symptoms such as swelling (edema), muscle spasms, cramps, and fatigue, which interfere with daily functions and sleep. Pregnancy massage gun use is a safe and helpful form of stress and tension relief, so long as healthcare providers and safety precautions are followed and sensitive areas are avoided. Massage guns use percussion and vibration to create a form of massage that can relieve tension, stiffness, and muscle soreness, break up tissue adhesions, and reduce inflammation. Moreover, pregnancy massage can provide relaxation and pain relief for muscles and joints that are adapting to a growing, changing body. Traditional massage therapy and massage gun therapy have been shown to help reduce muscle soreness and pain. (Imtiyaz S., Veqar Z., & Shareef M. Y. 2014) The benefits of pregnancy massage gun use include: However, it is essential to discuss massage gun use with a healthcare professional and follow safety precautions when using massage guns during pregnancy. Benefits While there is no specific research on the benefits of massage guns for pregnant individuals, studies have demonstrated the general benefits of massage during pregnancy, including deep tissue massage. Therapeutic massage effectively reduces pregnancy discomforts and pain and is a safe and affordable method of pain relief. (El-Hosary EA, Abbas Soliman HF, El-Homosy SM. 2016) Researchers believe this relief helps improve the health of mother and baby in ways that include. (El-Hosary EA, Abbas Soliman HF, El-Homosy SM. 2016) (Mueller S. M., & Grunwald M. 2021) - Improves cardiovascular health
- Overall circulation improves
- Increases serotonin and dopamine levels
- Decreases chronic back pain
- Relieves muscle aches and joint pains
- Improves sleep patterns
- Increases energy
- Reduces anxiety
- Increases immune response
- Enhances sense of well-being and mood
- Reduces risk of preterm delivery
Massage Gun Safety Pregnancy massage gun use is generally safe for those who do not have preexisting conditions. (Mueller S. M., & Grunwald M. 2021) However, there are no studies on the safety of massage guns or other massage tools for pregnant individuals. It is recommended to discuss the use of massage guns with a doctor before use. When to Avoid Massage Therapies Pregnant individuals should avoid pregnancy massage of any kind if any of the following conditions are present (American Massage Therapy Association, 2018) High-risk Pregnancy - Individuals with high-risk factors, such as bleeding, pre-term contractions, and preeclampsia, should avoid using massage guns unless a doctor clears them to do so.
Preeclampsia - This condition causes a rise in blood pressure that can be serious.
- It typically develops around 20 weeks of pregnancy or later.
Deep Vein Thrombosis - DVT - Avoid using a massage gun if there is a history of deep vein thrombosis.
- Blood volume increases during pregnancy, and leg circulation can be poor.
- Certain hormones that prevent hemorrhage during delivery can cause blood to clot more easily.
- Using a massage gun on areas with potential blood clots may release the clot, leading to a life-threatening embolism. (Sutham K. et al., 2020)
- Compression socks are a better alternative for relieving leg pain and swelling, but follow the healthcare provider's recommendations.
Placenta Previa, Accrete, or Abruption - These conditions involve the placenta, which can lead to bleeding.
Gestational Diabetes - High blood sugar levels do not necessarily mean individuals cannot use a massage gun during pregnancy.
- However, speak to a doctor and monitor blood sugar before use.
How to Use Although there are no specific expert directions for the use of massage guns during pregnancy, there are guidelines to consider while using the device. This includes: - Never place the massage gun directly over bones, nerves, or joints.
- Avoid using the device around injured, swollen, or painful areas.
- Avoid using a massage gun directly on the abdomen.
Additional Tips (Hospital for Special Surgery, 2021) - Start by trying a light 10- to 15-second pass over sore or tight areas.
- Perform three to five sweeps over the location, then move on to another.
- Be careful not to keep the gun on a single area too long, as you could overwork the muscle, leading to bruising and irritation.
- The recommended time for leaving the massager in one area is two minutes.
- Stop using the massage gun if there is unusual pain, sensations, or discomfort.
Injury Medical Chiropractic and Functional Medicine Clinic Massage during pregnancy can help relieve symptoms such as anxiety, stress, pain, discomfort, tightness, and poor circulation. Regular massage can help improve sleep and can even benefit the baby. However, it is recommended to consult with a doctor about using a massage gun before trying it out. Injury Medical Chiropractic and Functional Medicine Clinic can help individuals recover and regain the benefits of quality rest through healthy sleep practices and lifestyle accommodations. We build optimal health and wellness solutions with primary healthcare providers and specialists. We focus on what works for you to relieve pain, restore function, prevent injury, and help mitigate issues through adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal problems. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies that are available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Imtiyaz, S., Veqar, Z., & Shareef, M. Y. (2014). To Compare the Effect of Vibration Therapy and Massage in Prevention of Delayed Onset Muscle Soreness (DOMS). Journal of clinical and diagnostic research: JCDR, 8(1), 133–136. https://doi.org/10.7860/JCDR/2014/7294.3971 American Massage Therapy Association. (2011). Pregnancy Massage. https://www.amtamassage.org/publications/massage-therapy-journal/massage-and-pregnancy/ El-Hosary EA, Abbas Soliman HF, El-Homosy SM. (2016). Effect of Therapeutic Massage on Relieving Pregnancy Discomforts. IOSR Journal of Nursing and Health Science., 5(4), 57-64. https://doi.org/10.9790/1959-0504025764 Mueller, S. M., & Grunwald, M. (2021). Effects, Side Effects and Contraindications of Relaxation Massage during Pregnancy: A Systematic Review of Randomized Controlled Trials. Journal of Clinical Medicine, 10(16), 3485. https://doi.org/10.3390/jcm10163485 American Massage Therapy Association. (2018). Massage and pregnancy: A powerful combination. https://www.amtamassage.org/publications/massage-therapy-journal/massage-and-pregnancy-a-powerful-combination/ Sutham, K., Na-Nan, S., Paiboonsithiwong, S., Chaksuwat, P., & Tongsong, T. (2020). Leg massage during pregnancy with unrecognized deep vein thrombosis could be life-threatening: a case report. BMC pregnancy and childbirth, 20(1), 237. https://doi.org/10.1186/s12884-020-02924-w Hospital for Special Surgery. Surgery, H. F. S. (2021). What you should know about using a massage gun. https://www.hss.edu/article_how-to-use-massage-gun.asp
Can individuals utilize chiropractic care to reduce sciatica pain and help restore mobility to their lower back and legs? Introduction Many individuals are always on the move and utilize the lower half of the body to go from one location to another. From the lower back to the feet, many individuals do repetitive movement that causes the lower back muscles to be constantly stretched. This, in turn, can lead to overlapping risk profiles that can affect the lower back and a long nerve connected to the lower back, known as the sciatic nerve. When numerous issues affect the sciatic nerve, many individuals experience pain and discomfort over time, which can develop into something chronic without treatment. Luckily, when individuals begin to think about their health and wellness, it reduces the chances of pain and discomfort from returning. Today’s article looks at the causes of sciatica and how non-surgical treatments like chiropractic care can help relieve sciatica pain and restore mobility to the lower back and legs. We discuss with certified medical providers who inform our patients how sciatica pain correlates with the lower back. While asking informed questions to our associated medical providers, we advise patients to incorporate non-surgical treatments like chiropractic care to reduce sciatica pain and help realign the body. Dr. Alex Jimenez, D.C., encompasses this information as an academic service. Disclaimer. What Causes Sciatica? Do you feel numbness or tingling sensations in your legs, making walking unbearable? Do you experience pain or discomfort in your lower back after lifting a heavy object? Or how long have you stretched your body after sitting down or standing excessively at work? Many of these scenarios are often correlated with low back pain. However, low back pain is always connected with sciatica and can impact the body. While the sciatic nerve plays a huge role in direct motor function to the hamstrings and lower extremities, sciatica is when environmental factors impact or compress the sciatic nerve, causing pain-like symptoms to the lower extremities. (Davis et al., 2024) Since the sciatic nerve is large and travels down to the feet, it allows mobility to the lower extremities. When many individuals experience low back pain, they will also experience sciatica.
Sciatica also means that pain will always be transmitted along the sciatic nerve root, leading to various impairments and socioeconomic consequences and affecting a person’s quality of life. (Siddiq et al., 2020) Many of the causes of sciatica pain can vary as they are all correlated with low back pain. Some of the various environmental factors that can cause sciatica include: - Physical inactivity
- Excessive sitting or standing
- Poor posture
- Musculoskeletal conditions
Another environmental factor that leads to the development of sciatica is disc degeneration. This can cause the nerves to be irritated due to herniation and cause asymptomatic overlapping risk profiles (Zhou et al., 2021). When people are dealing with the overlapping risk profiles of sciatica, many often seek treatment to reduce the pain and restore mobility to the lower extremities. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
|






 Your new post is loading...
Your new post is loading...







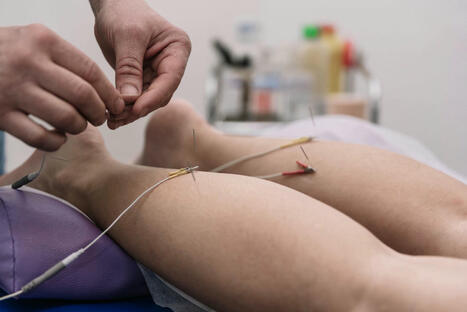

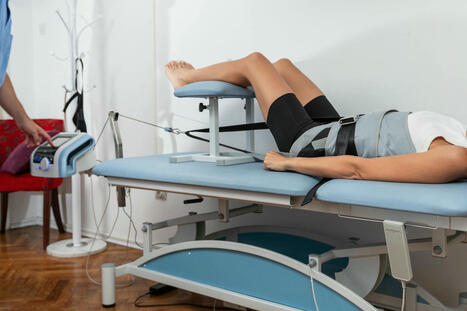


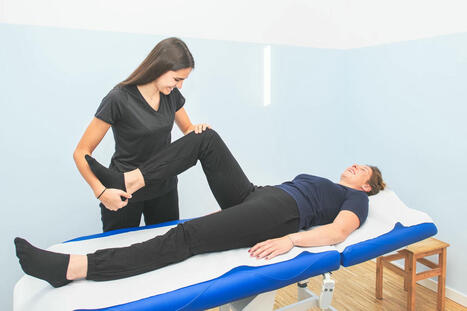








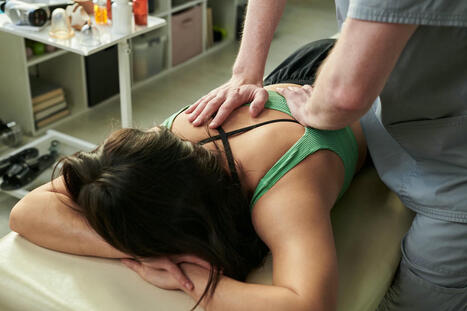








Sciatica is characterized as a collection of symptoms rather than a single condition. Pain and discomfort, along with tingling sensations, numbness and burning sensations are the most common symptoms indicating the presence of sciatica. Understanding the variety of symptoms as well as the causes for sciatica can be important in order to properly diagnose it and follow up with treatment. For more information, please feel free to ask Dr. Jimenez or contact us at (915) 850-0900.